Name the parasite whose microfilariae have a sheath and no nuclei at the tail end.
A patient presents with a history of pastry intake causing food poisoning. What is the most likely causative agent?
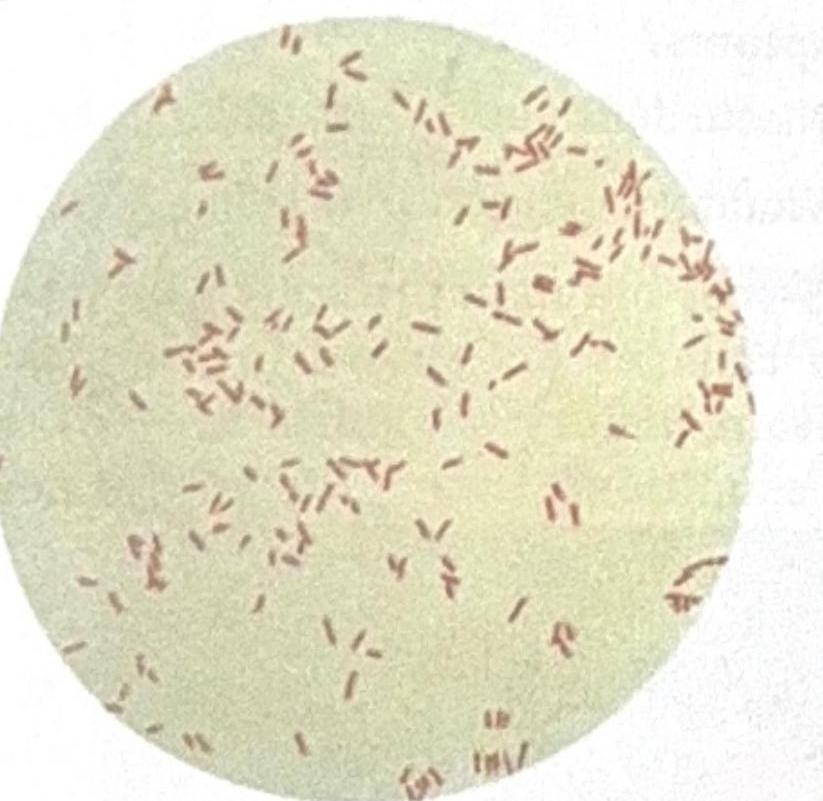
A patient presented with 70% burns, and a sample was collected from the burn site. The image shows Gram-negative rods, and the suspected organism is an obligate aerobe. What is the most likely causative microbe?