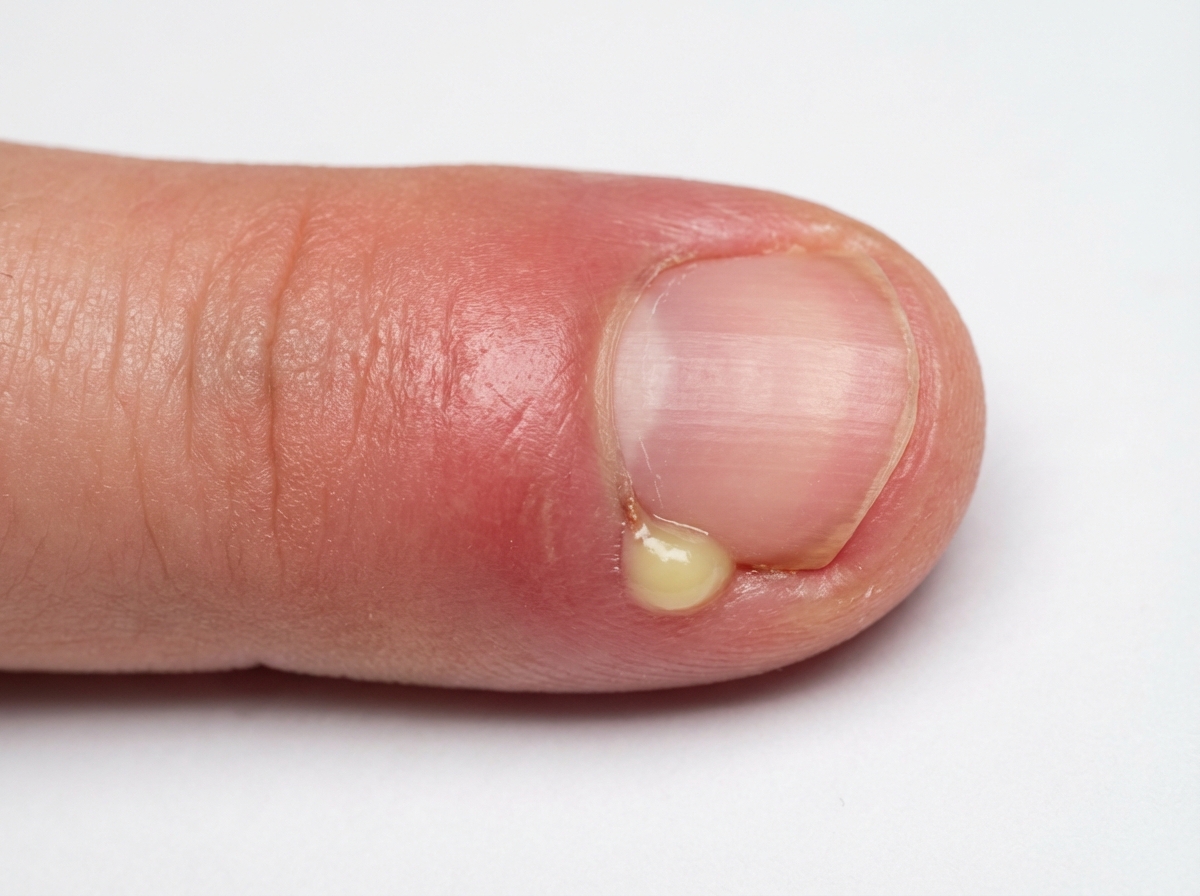
A 30-year-old woman presents with flaccid bullae on her skin that are easy to rupture. A biopsy of the lesion reveals a suprabasal split. What is the most likely diagnosis?
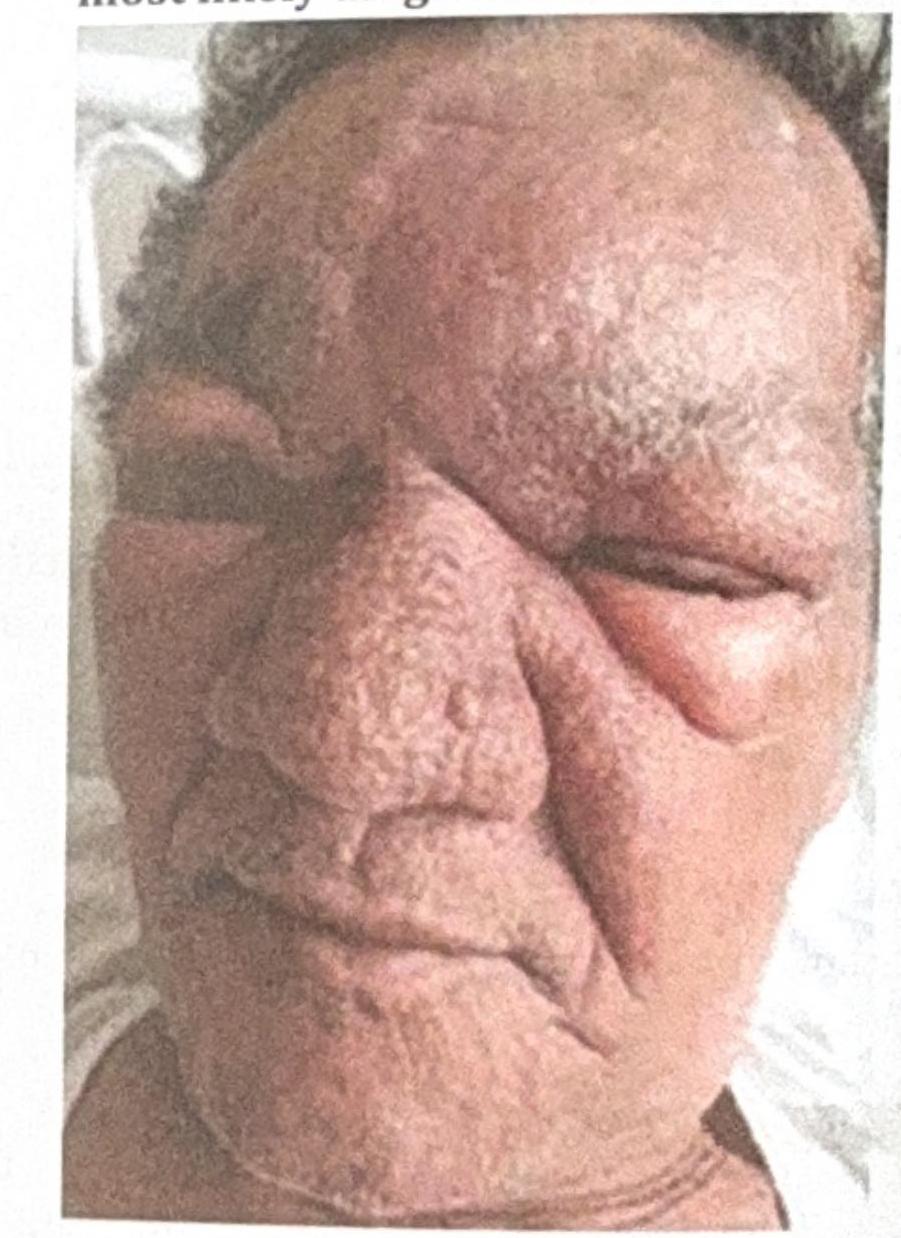
A 53 year-old male presented with erythematous, edematous plaques on his face over pre-existing hypoesthetic patches. He has been experiencing pain for the last 10 days and has been on multibacillary multidrug therapy (MBMDT) for leprosy for the past two months. What is the most likely diagnosis based on the image?
A young girl presents to the outpatient department with rough-surfaced lesions over her elbows and knees. She also complains of diminished vision at night. What is the most likely diagnosis?