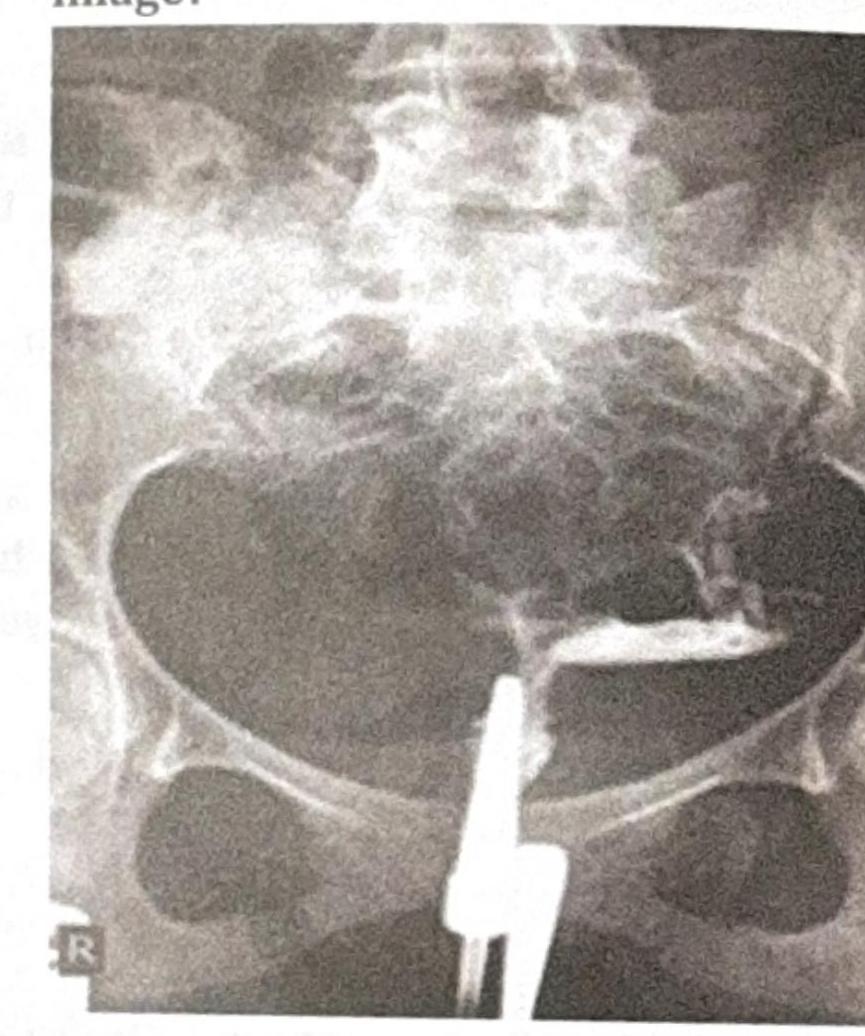
A 26-year-old male presents with backache, morning stiffness, reduced chest expansion, and reddening of the eyes. The X-ray provided is shown below. What is the most likely diagnosis?
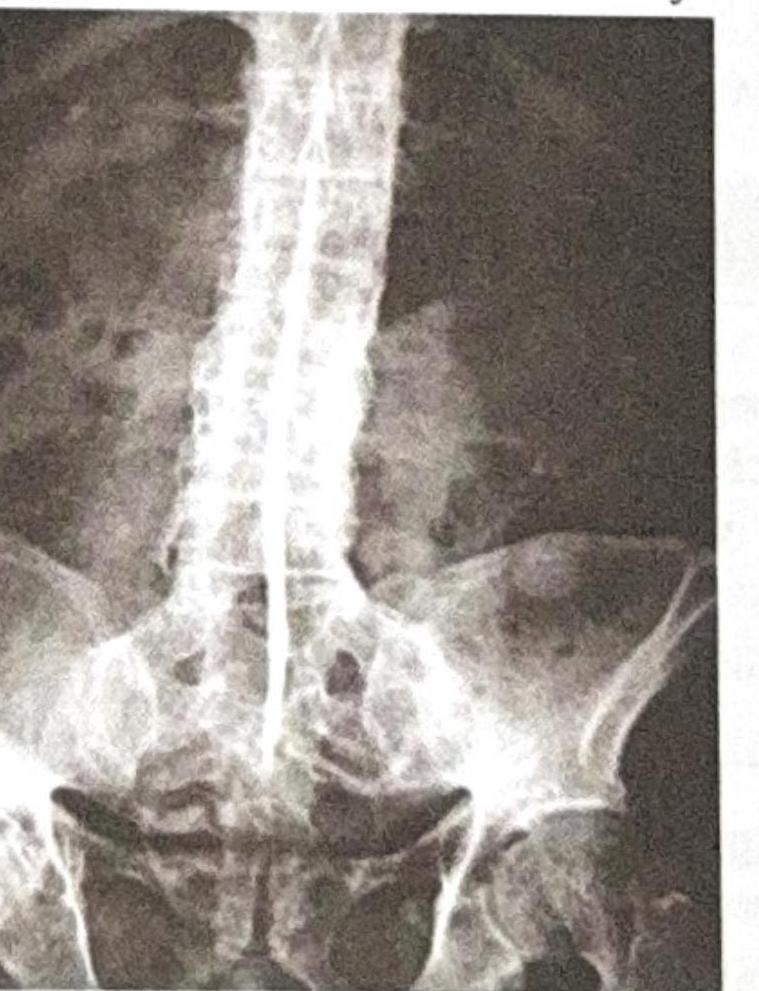
A 20-year-old patient presents with chronic low backache and early morning stiffness for the last 2 years. For the past 6 months, they have also experienced bilateral heel pain. What is the most likely diagnosis?