A 12-year-old boy presents with weak pulses in the upper limbs, a blood pressure of 90/60 mmHg , and retinal hemorrhages. What is the most likely diagnosis?
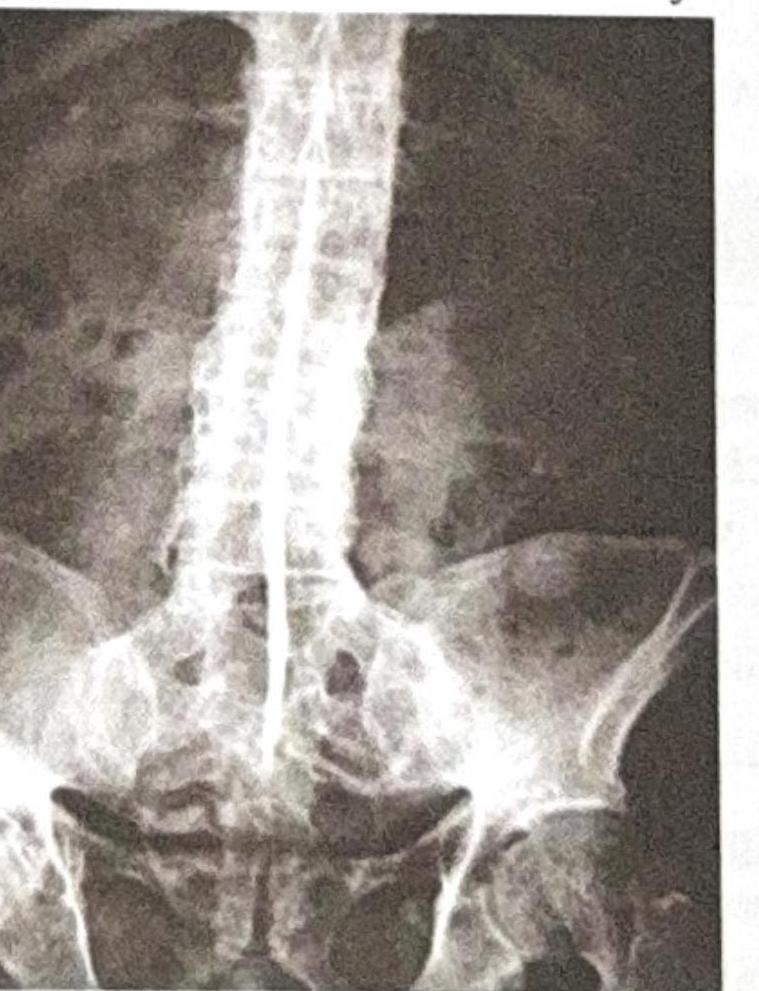
A 26-year-old male presents with backache, morning stiffness, reduced chest expansion, and reddening of the eyes. The X-ray provided is shown below. What is the most likely diagnosis?