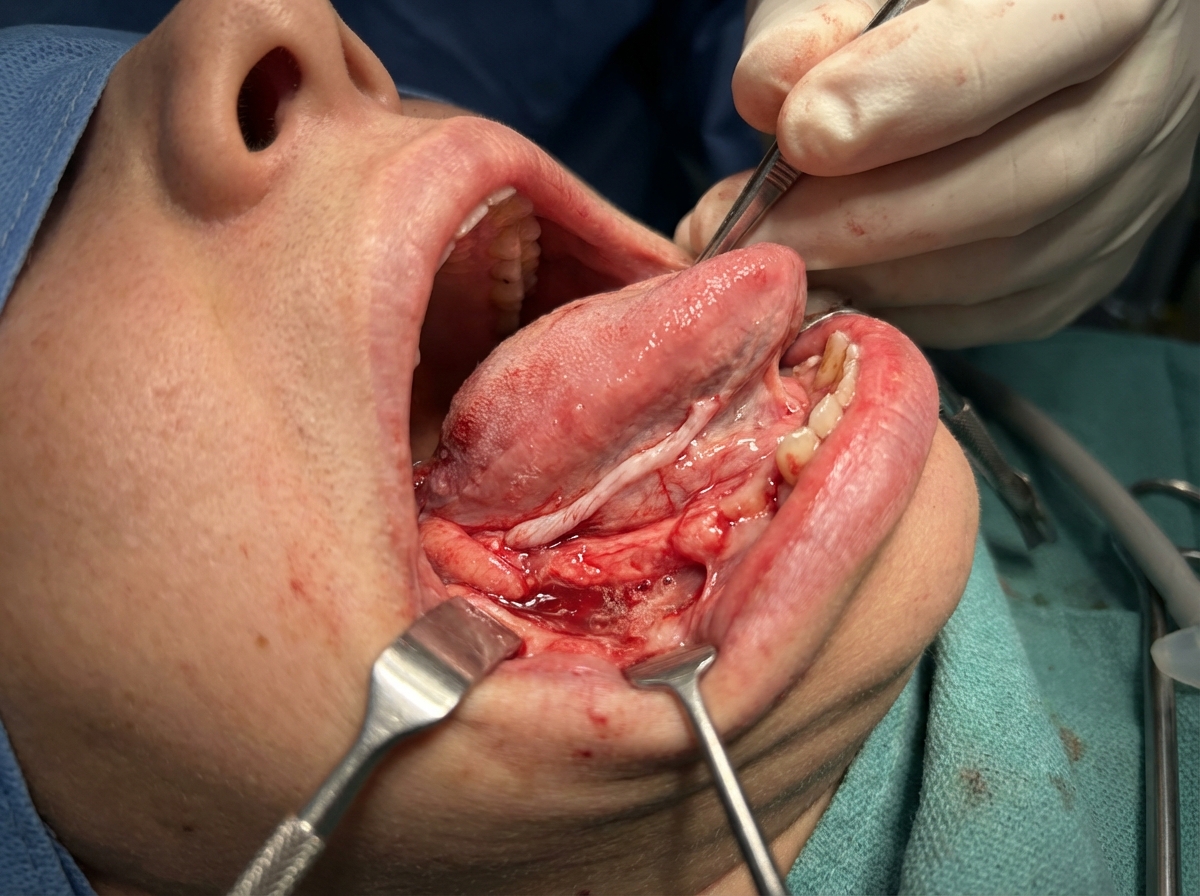
Which of the following statements is true regarding the structure shown in the image?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Which of the following statements is true regarding the structure shown in the image?

A 60-year-old male patient has an antral carcinoma spreading to the head of the pancreas with multiple small metastases to the right lobe of the liver. What is the best treatment approach?
An 85-year-old male with prostate cancer, Gleason score of 6 , and PSA <8 ng/mL. What is the best management approach?
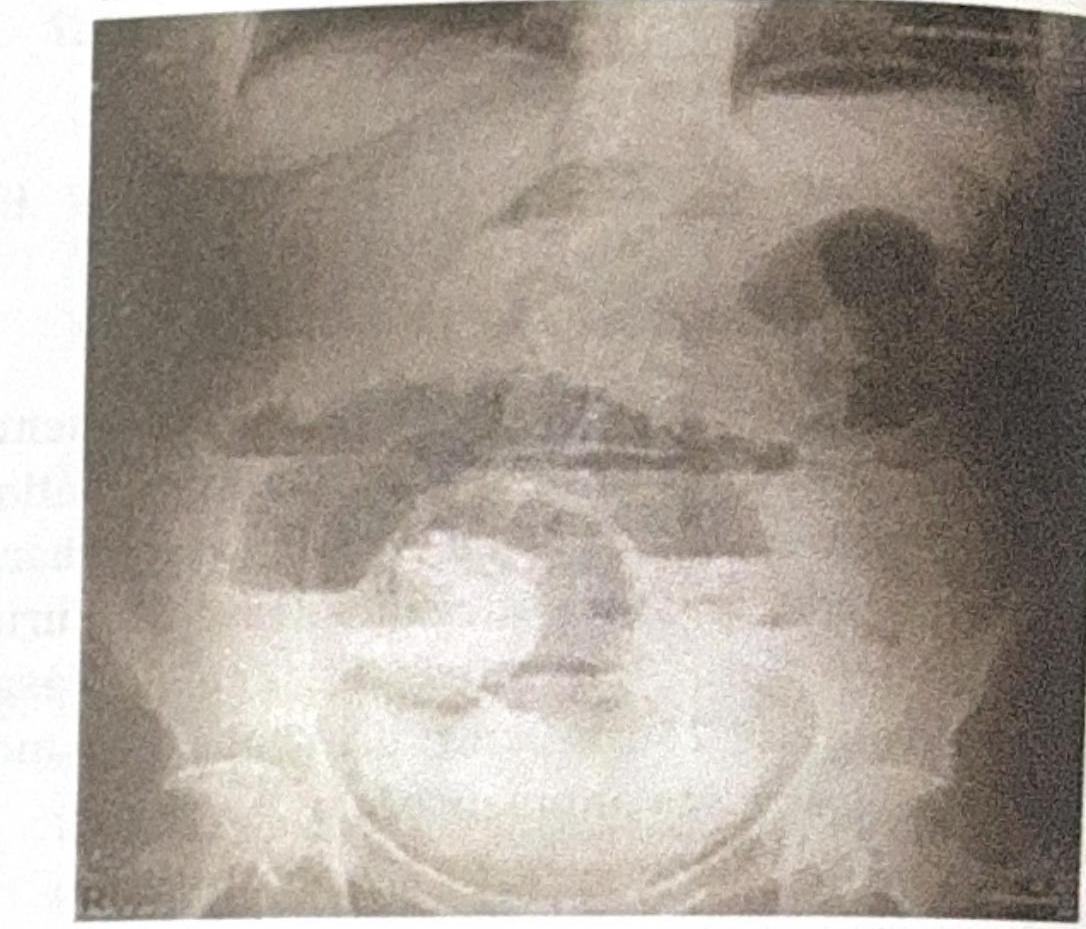
Examine the abdominal X-ray shown. What is the most likely diagnosis based on the findings?
Asymptomatic varicose veins would fall under which category of the CEAP classification system?
Which nerve is most commonly injured during submandibular gland surgery?
A patient is found to have an asymptomatic common bile duct (CBD) stone two years after cholecystectomy on routine imaging. What is the most appropriate initial management?
In which condition is gas under the diaphragm most commonly seen on imaging?
A patient with a left hypochondrium contusion presents with systolic blood pressure of 70 mm Hg and pulse rate of 110 bpm. What is the best step in management?
Mr. Ramu, a 35-year-old male, sustained a straddle injury in a motor vehicle accident and presents to the emergency department with blood at the urethral meatus. What is the next appropriate step in his management?