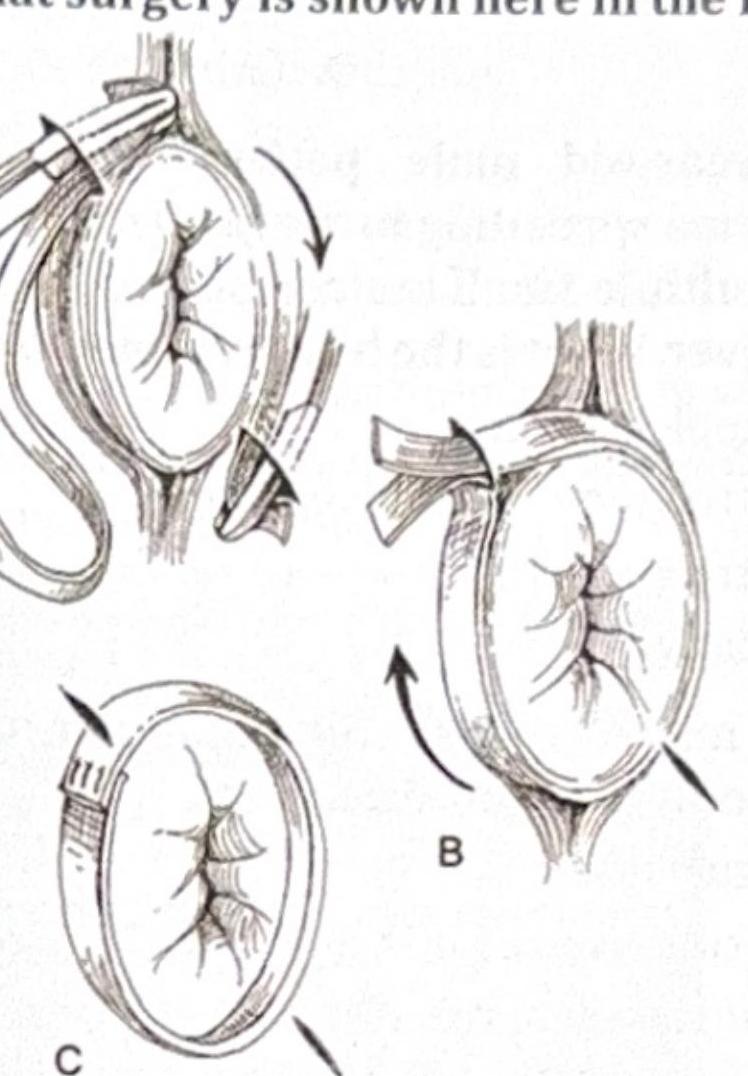
What surgery is shown here in the image?
A patient presents with upper limb swelling after undergoing a modified radical mastectomy (MRM). What is the most likely cause?
Which of the following is the most commonly performed repair for a direct inguinal hernia?
A patient presents with breathlessness and decreased air entry into the right lung following a road traffic accident (RTA) and is hypotensive. What is the next step in management?
After a total thyroidectomy, the surgeon is unable to extubate the patient, who shows cyanosis and respiratory distress. What is the most likely cause of the inability to extubate?