NEET-PG 2021 — Anatomy
8 Previous Year Questions with Answers & Explanations
Pen Test is for which nerve
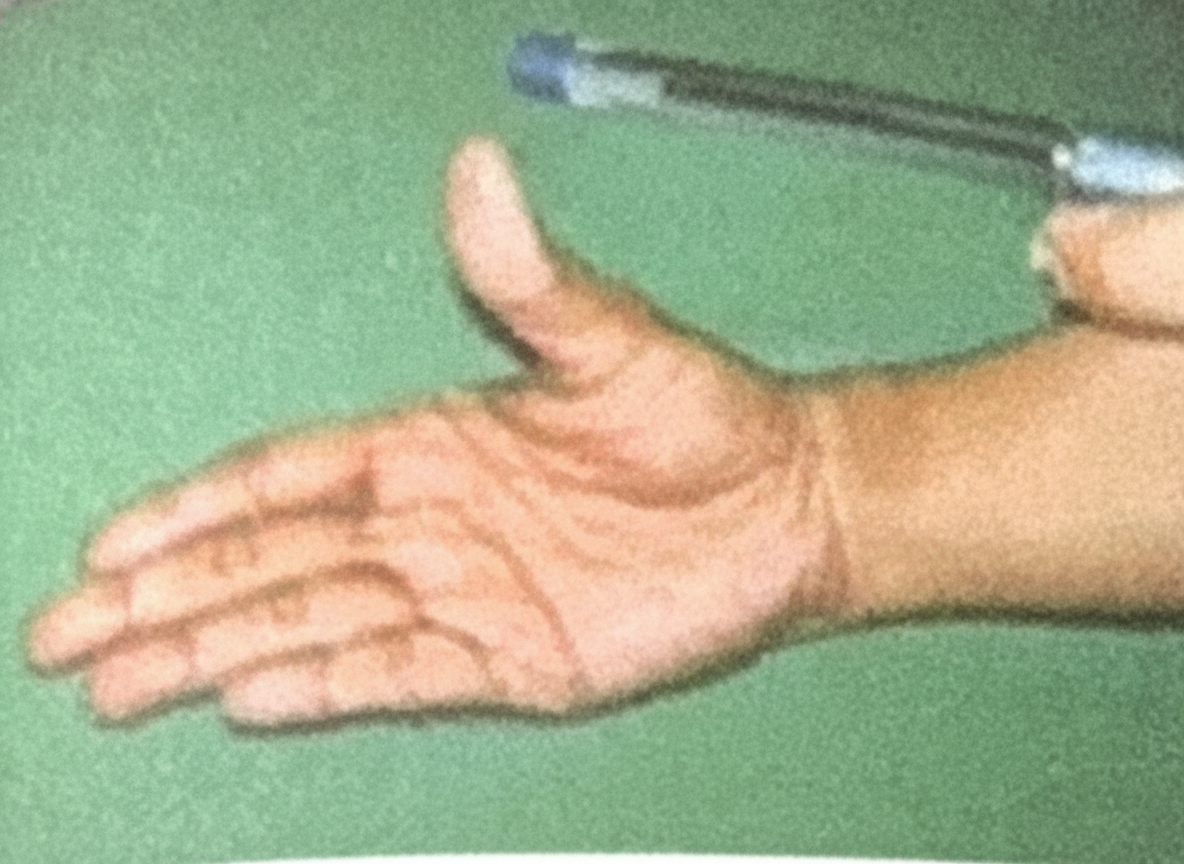
A young boy presents with multiple humerus fractures, resulting in loss of sensation over the lateral side of the forearm, along with difficulty in elbow flexion and forearm supination. What is the most likely nerve injury responsible for these symptoms?
Structure preventing vertical descent of spleen
Which nerve is responsible for gag reflex
A patient underwent a coronary artery bypass graft (CABG) using the great saphenous vein. Post-surgery, the patient experiences neuralgia on the medial aspect of the leg and foot. Which nerve is most likely injured?
A patient was admitted with skull base trauma. The doctor was testing the marked structure in the pharyngeal region. Which of the following nerves was being tested?
Which of the following statements is true regarding the structure shown in the image?
While performing a lumbar puncture on a patient presenting with fever, neck rigidity, and altered sensorium, what is the last structure to be encountered by the needle?
NEET-PG 2021 - Anatomy NEET-PG Practice Questions and MCQs
Question 1: Pen Test is for which nerve
- A. Median Nerve (Correct Answer)
- B. Radial nerve
- C. Ulnar nerve
- D. Musculocutaneous
- E. Axillary nerve
Explanation: ***Median Nerve*** - The **pen test** (or pen-holding test) assesses the ability to perform **precision grip** by pinching a pen between the thumb and index finger - This tests **thumb opposition and flexion**, which are controlled by the **thenar muscles** (abductor pollicis brevis, opponens pollicis, and flexor pollicis brevis) innervated by the median nerve - The median nerve also controls the **lateral two lumbricals** for fine finger movements essential for holding objects like a pen - **Clinical significance**: Inability to perform this test indicates median nerve injury (e.g., carpal tunnel syndrome) *Musculocutaneous* - Innervates the **anterior compartment of the arm**: biceps brachii, brachialis, and coracobrachialis - Controls **elbow flexion** and provides sensory innervation to the lateral forearm - Does not control hand muscles or precision grip functions *Radial nerve* - Innervates **extensors of the wrist, fingers, and thumb** in the posterior compartment of the forearm - Controls **wrist extension** and **finger extension** at the MCP joints - Radial nerve injury causes **wrist drop**, not impaired precision grip *Ulnar nerve* - Controls most **intrinsic hand muscles** including interossei, medial two lumbricals, and adductor pollicis - Tested by **Froment's sign** (compensatory thumb IP flexion when pinching paper due to adductor pollicis weakness) - Ulnar nerve injury affects **power grip** and finger abduction/adduction, not the precision pinch required for the pen test *Axillary nerve* - Innervates the **deltoid** and **teres minor** muscles in the shoulder - Controls **shoulder abduction** and provides sensation over the lateral upper arm - Has no role in hand function or precision grip
Question 2: A young boy presents with multiple humerus fractures, resulting in loss of sensation over the lateral side of the forearm, along with difficulty in elbow flexion and forearm supination. What is the most likely nerve injury responsible for these symptoms?
- A. Median nerve
- B. Axillary
- C. Radial nerve
- D. Musculocutaneous nerve (Correct Answer)
- E. Ulnar nerve
Explanation: ***Musculocutaneous nerve*** - The **musculocutaneous nerve** innervates the biceps brachii and brachialis muscles, responsible for **elbow flexion** and **forearm supination**, and provides sensation to the **lateral forearm** via the lateral cutaneous nerve of the forearm. - A fracture of the humerus can damage this nerve, leading to the observed **motor and sensory deficits**. *Median nerve* - The median nerve primarily controls **flexion of the wrist and fingers**, and **pronation of the forearm**, as well as sensation to the palmar aspect of the thumb, index, middle, and radial half of the ring finger. - Its injury would not typically cause difficulty with **elbow flexion** or sensory loss over the **lateral forearm**. *Axillary* - The axillary nerve primarily innervates the **deltoid** and **teres minor muscles**, important for shoulder abduction and external rotation. - An injury would lead to **weakness in shoulder abduction** and sensory loss over the lateral shoulder (regimental badge area), not the lateral forearm. *Radial nerve* - The radial nerve controls **extension of the wrist and fingers** and sensation over the posterior arm, forearm, and hand. - Injury typically results in **wrist drop** and difficulty extending the arm, not primarily elbow flexion or lateral forearm sensation. *Ulnar nerve* - The ulnar nerve innervates intrinsic hand muscles and flexor carpi ulnaris, controlling **finger abduction/adduction** and **ulnar wrist flexion**. - Sensory distribution includes the medial hand and medial 1.5 fingers, not the **lateral forearm**. - Injury causes **claw hand deformity** and sensory loss in the medial hand, not the symptoms described.
Question 3: Structure preventing vertical descent of spleen
- A. Ligamentum teres
- B. Ligamentum flavum
- C. Hepatogastric ligament
- D. Phrenocolic ligament (Correct Answer)
- E. Lienorenal ligament
Explanation: ***Phrenocolic ligament*** - The **phrenocolic ligament** is a fold of peritoneum that extends from the left colic (splenic) flexure of the colon to the diaphragm. - It forms a shelf or sling underneath the spleen, providing crucial support and preventing its **vertical descent**. *Ligamentum teres* - The **ligamentum teres hepatis** is the remnant of the obliterated umbilical vein, found in the free margin of the falciform ligament. - It connects the umbilicus to the liver and plays no role in supporting the spleen. *Ligamentum flavum* - The **ligamentum flavum** is a series of elastic ligaments connecting the laminae of adjacent vertebrae in the spinal column. - It is a component of the vertebral column and has no anatomical or functional relationship with the spleen. *Hepatogastric ligament* - The **hepatogastric ligament** is part of the lesser omentum, extending from the liver to the lesser curvature of the stomach. - Its primary function is to contain the **gastric arteries** and connect these organs, not to support the spleen. *Lienorenal ligament* - The **lienorenal ligament** (splenorenal ligament) connects the hilum of the spleen to the anterior surface of the left kidney. - While it provides **lateral support** to the spleen, it does not prevent **vertical descent** as effectively as the phrenocolic ligament.
Question 4: Which nerve is responsible for gag reflex
- A. 11th cranial nerve
- B. 6th Cranial Nerve
- C. 7th Cranial Nerve
- D. 9th Cranial Nerve (Correct Answer)
- E. 10th Cranial Nerve
Explanation: ***9th Cranial Nerve*** - The **glossopharyngeal nerve (CN IX)** is primarily responsible for the **afferent (sensory)** limb of the gag reflex, detecting touch in the posterior pharynx. - It transmits sensory information to the **brainstem**, initiating the efferent response via the vagus nerve. - CN IX is considered the nerve "responsible for" the gag reflex as it **detects and initiates** the protective response. *10th Cranial Nerve* - The **vagus nerve (CN X)** provides the **efferent (motor)** limb of the gag reflex, causing pharyngeal muscle contraction. - While essential for the motor response, CN IX is the primary sensory trigger that initiates the reflex. - Both nerves work together, but CN IX is the **detection nerve** that starts the reflex arc. *11th Cranial Nerve* - The **spinal accessory nerve (CN XI)** primarily innervates the **sternocleidomastoid** and **trapezius muscles**, controlling head and shoulder movements. - It has no direct role in the **gag reflex**. *6th Cranial Nerve* - The **abducens nerve (CN VI)** is responsible for the **lateral rectus muscle** of the eye, controlling **abduction of the eyeball**. - It does not participate in the complex **sensory or motor pathways** of the gag reflex. *7th Cranial Nerve* - The **facial nerve (CN VII)** controls **facial expressions**, taste from the anterior two-thirds of the tongue, and some glandular secretions. - While it has some role in taste and salivation, it is not the primary nerve for the **gag reflex**.
Question 5: A patient underwent a coronary artery bypass graft (CABG) using the great saphenous vein. Post-surgery, the patient experiences neuralgia on the medial aspect of the leg and foot. Which nerve is most likely injured?
- A. Common peroneal nerve
- B. Sural nerve
- C. Tibial nerve
- D. Saphenous nerve (Correct Answer)
- E. Superficial peroneal nerve
Explanation: ***Saphenous nerve*** - The **saphenous nerve** is a cutaneous branch of the femoral nerve that runs closely with the **great saphenous vein** along the medial aspect of the leg and foot. - Due to its proximity to the vein, it is highly susceptible to **injury** during the harvesting of the great saphenous vein for CABG, leading to **neuralgia** in its sensory distribution. *Common peroneal nerve* - The **common peroneal nerve** innervates the lateral and anterior compartments of the leg, affecting dorsiflexion and eversion of the foot. - Damage to this nerve typically results in **foot drop** and sensory loss over the dorsum of the foot, which is inconsistent with the patient's symptoms. *Tibial nerve* - The **tibial nerve** supplies the posterior compartment of the leg and the plantar aspect of the foot. - Injury would cause loss of plantarflexion and sensation on the sole of the foot, which is not described. *Sural nerve* - The **sural nerve** provides sensation to the posterolateral aspect of the leg and the lateral side of the foot and ankle. - While it runs near superficial veins, its sensory distribution does not match the described **medial leg and foot neuralgia**. *Superficial peroneal nerve* - The **superficial peroneal nerve** (superficial fibular nerve) provides sensation to the dorsum of the foot and anterolateral leg. - Injury would cause sensory loss over the dorsal foot, not the medial aspect of the leg and foot.
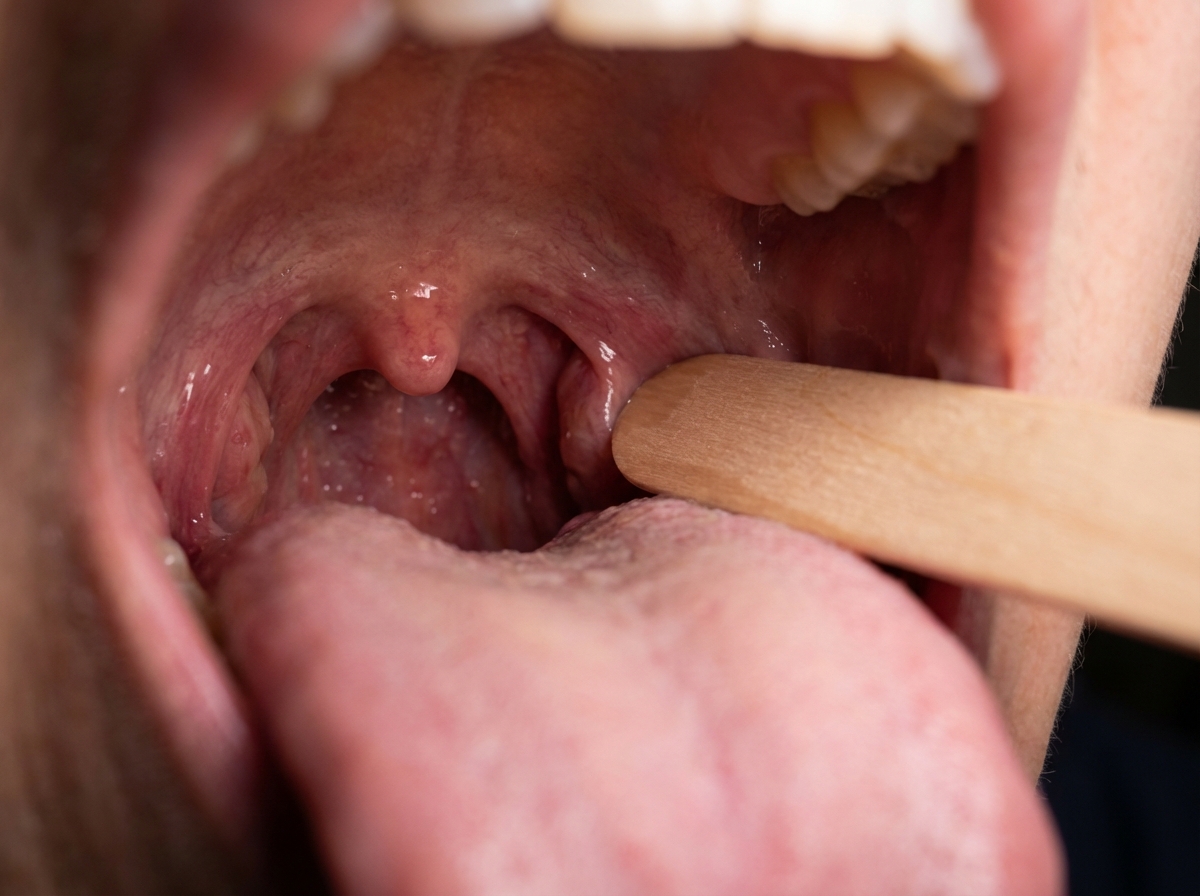
Question 6: A patient was admitted with skull base trauma. The doctor was testing the marked structure in the pharyngeal region. Which of the following nerves was being tested?
- A. Trigeminal nerve
- B. Facial nerve
- C. Glossopharyngeal nerve (Correct Answer)
- D. Vagus
- E. Hypoglossal nerve
Explanation: ***Glossopharyngeal nerve*** - The image shows a probe stimulating the posterior part of the **pharynx**, which elicits the **gag reflex**. - The afferent limb of the **gag reflex** is mediated primarily by the **glossopharyngeal nerve (CN IX)**, which detects sensation from the posterior tongue and pharynx. *Trigeminal nerve* - The **trigeminal nerve (CN V)** primarily mediates sensation from the face, teeth, and anterior two-thirds of the tongue, and motor control of the **muscles of mastication**. - It does not have a primary role in the sensation or reflex of the posterior pharyngeal wall. *Facial nerve* - The **facial nerve (CN VII)** is responsible for the **muscles of facial expression**, taste from the anterior two-thirds of the tongue, and parasympathetic innervation to several glands. - While it contributes to some aspects of swallowing, it is not the main sensory nerve for the gag reflex from the posterior pharynx. *Vagus* - The **vagus nerve (CN X)** provides the efferent limb of the gag reflex, causing pharyngeal muscle contraction. - However, the sensory input from the posterior pharynx (the afferent limb being tested by the probe) is primarily carried by the **glossopharyngeal nerve**. *Hypoglossal nerve* - The **hypoglossal nerve (CN XII)** provides motor innervation to the intrinsic and extrinsic muscles of the tongue. - While it is relevant in skull base trauma, it does not mediate sensation from the pharynx or the gag reflex being tested in the image.
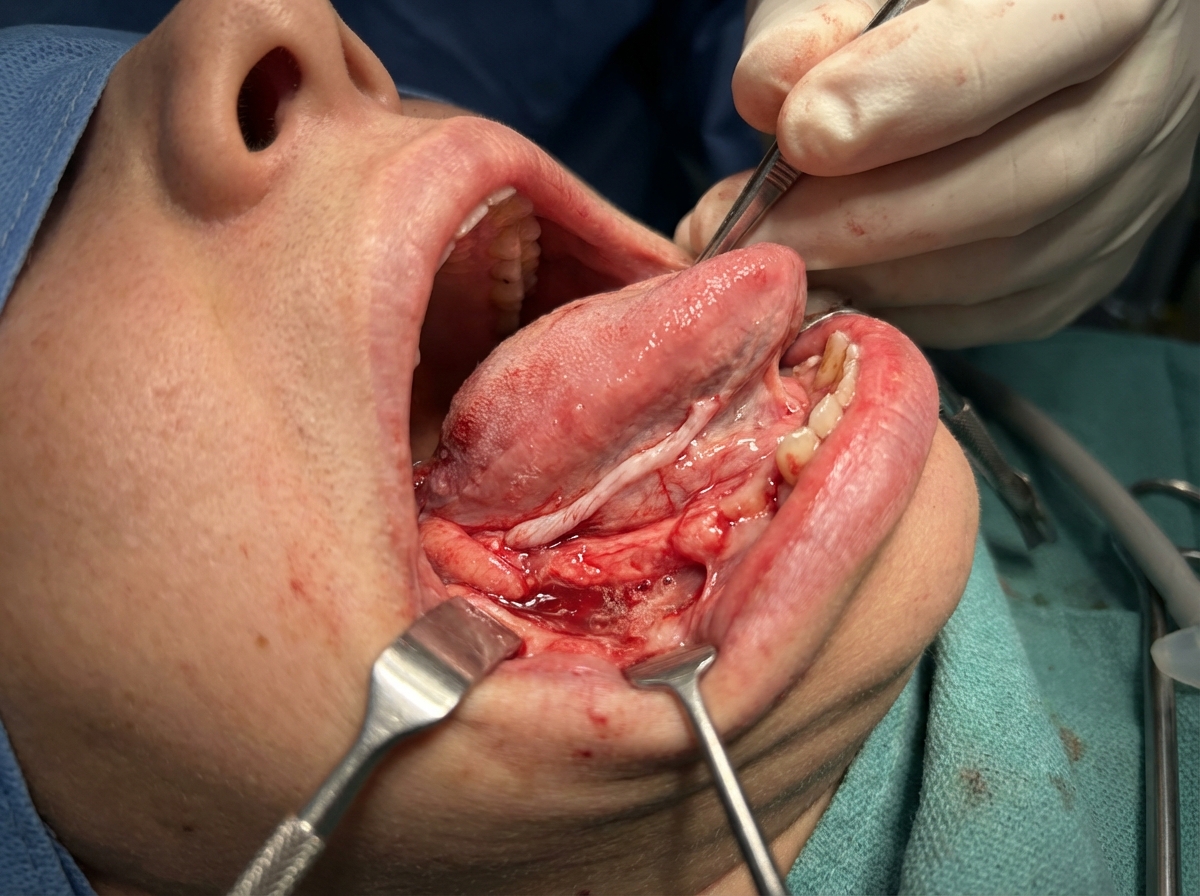
Question 7: Which of the following statements is true regarding the structure shown in the image?
- A. Hypoglossal nerve
- B. Lingual nerve (Correct Answer)
- C. Nerve to mylohyoid
- D. Inferior alveolar nerve
- E. Glossopharyngeal nerve
Explanation: ***Lingual nerve*** - The image appears to depict a **surgical field in the floor of the mouth**, likely during an excision of a lesion, where the **lingual nerve** is a key structure that needs to be identified and preserved due to its superficial position. - The lingual nerve provides **general sensation** and **taste (chorda tympani fibers)** to the anterior two-thirds of the tongue, and its injury would result in loss of these functions. *Hypoglossal nerve* - The **hypoglossal nerve** (CN XII) innervates the **intrinsic and extrinsic muscles of the tongue** (except the palatoglossus) and is deep to the submandibular duct. - While important in floor of mouth surgery, it is typically located more inferiorly and medially, deeper than the very superficial structure shown, which appears to be the lingual nerve. *Nerve to mylohyoid* - The **nerve to mylohyoid** is a branch of the inferior alveolar nerve and innervates the **mylohyoid muscle** and the **anterior belly of the digastric muscle**. - This nerve is located more inferiorly, lying on the surface of the mylohyoid muscle, and is less likely to be the prominent superficial structure highlighted in this context near the tongue root or oral mucosa. *Inferior alveolar nerve* - The **inferior alveolar nerve** is a branch of the mandibular nerve (V3) and primarily provides **sensation to the mandibular teeth** and **gingiva**; it enters the mandibular foramen. - This nerve is located deep within the mandible and jaw, not superficially within the oral cavity or floor of the mouth as depicted, making it an unlikely choice for the superficial structure shown. *Glossopharyngeal nerve* - The **glossopharyngeal nerve** (CN IX) provides **general sensation and taste** to the **posterior one-third of the tongue** and innervates the stylopharyngeus muscle. - This nerve courses deep in the pharyngeal region and does not run superficially in the anterior floor of the mouth as shown in the image, making it an incorrect choice for this superficial anterior structure.
Question 8: While performing a lumbar puncture on a patient presenting with fever, neck rigidity, and altered sensorium, what is the last structure to be encountered by the needle?
- A. Dura mater
- B. Pia mater
- C. Ligamentum flavum
- D. Arachnoid membrane (Correct Answer)
- E. Supraspinous ligament
Explanation: ***Arachnoid membrane*** - The **arachnoid membrane** is the innermost layer the needle punctures before entering the **subarachnoid space** where cerebrospinal fluid (CSF) is collected. - The needle passes through skin, subcutaneous tissue, supraspinous ligament, interspinous ligament, ligamentum flavum, epidural space, and dura mater, with arachnoid mater being the last barrier. *Dura mater* - The **dura mater** is pierced **before** the arachnoid membrane and before entering the subarachnoid space. - It is a tough, fibrous membrane forming the outermost layer of the **meninges**. *Pia mater* - The **pia mater** is in direct contact with the spinal cord and is **not punctured** during a properly performed lumbar puncture. - It is the innermost meningeal layer, adherent to the neural tissue itself. *Ligamentum flavum* - The **ligamentum flavum** is encountered **early** in the lumbar puncture procedure, prior to the epidural space and the meningeal layers. - It is a strong ligament connecting the laminae of adjacent vertebrae. *Supraspinous ligament* - The **supraspinous ligament** is one of the **first structures** encountered during lumbar puncture, after penetrating skin and subcutaneous tissue. - It connects the spinous processes of adjacent vertebrae and is pierced well before reaching the meningeal layers.