NEET-PG 2021
176 Previous Year Questions with Answers & Explanations
Anatomy
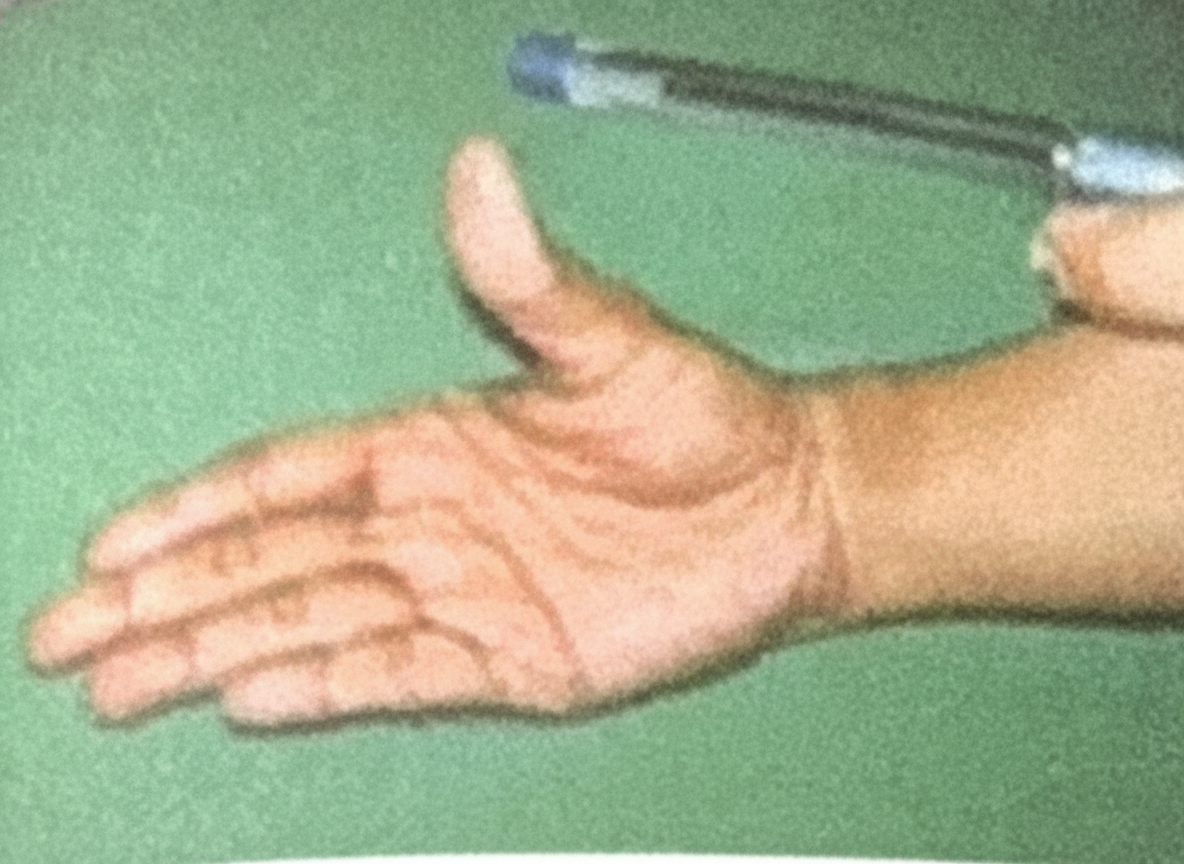
6 questionsPen Test is for which nerve
A young boy presents with multiple humerus fractures, resulting in loss of sensation over the lateral side of the forearm, along with difficulty in elbow flexion and forearm supination. What is the most likely nerve injury responsible for these symptoms?
Which blood vessel carries deoxygenated blood back to the placenta?
Structure preventing vertical descent of spleen
Which nerve is responsible for gag reflex
A patient underwent a coronary artery bypass graft (CABG) using the great saphenous vein. Post-surgery, the patient experiences neuralgia on the medial aspect of the leg and foot. Which nerve is most likely injured?
NEET-PG 2021 - Anatomy NEET-PG Practice Questions and MCQs
Question 1: Pen Test is for which nerve
- A. Median Nerve (Correct Answer)
- B. Radial nerve
- C. Ulnar nerve
- D. Musculocutaneous
- E. Axillary nerve
Explanation: ***Median Nerve*** - The **pen test** (or pen-holding test) assesses the ability to perform **precision grip** by pinching a pen between the thumb and index finger - This tests **thumb opposition and flexion**, which are controlled by the **thenar muscles** (abductor pollicis brevis, opponens pollicis, and flexor pollicis brevis) innervated by the median nerve - The median nerve also controls the **lateral two lumbricals** for fine finger movements essential for holding objects like a pen - **Clinical significance**: Inability to perform this test indicates median nerve injury (e.g., carpal tunnel syndrome) *Musculocutaneous* - Innervates the **anterior compartment of the arm**: biceps brachii, brachialis, and coracobrachialis - Controls **elbow flexion** and provides sensory innervation to the lateral forearm - Does not control hand muscles or precision grip functions *Radial nerve* - Innervates **extensors of the wrist, fingers, and thumb** in the posterior compartment of the forearm - Controls **wrist extension** and **finger extension** at the MCP joints - Radial nerve injury causes **wrist drop**, not impaired precision grip *Ulnar nerve* - Controls most **intrinsic hand muscles** including interossei, medial two lumbricals, and adductor pollicis - Tested by **Froment's sign** (compensatory thumb IP flexion when pinching paper due to adductor pollicis weakness) - Ulnar nerve injury affects **power grip** and finger abduction/adduction, not the precision pinch required for the pen test *Axillary nerve* - Innervates the **deltoid** and **teres minor** muscles in the shoulder - Controls **shoulder abduction** and provides sensation over the lateral upper arm - Has no role in hand function or precision grip
Question 2: A young boy presents with multiple humerus fractures, resulting in loss of sensation over the lateral side of the forearm, along with difficulty in elbow flexion and forearm supination. What is the most likely nerve injury responsible for these symptoms?
- A. Median nerve
- B. Axillary
- C. Radial nerve
- D. Musculocutaneous nerve (Correct Answer)
- E. Ulnar nerve
Explanation: ***Musculocutaneous nerve*** - The **musculocutaneous nerve** innervates the biceps brachii and brachialis muscles, responsible for **elbow flexion** and **forearm supination**, and provides sensation to the **lateral forearm** via the lateral cutaneous nerve of the forearm. - A fracture of the humerus can damage this nerve, leading to the observed **motor and sensory deficits**. *Median nerve* - The median nerve primarily controls **flexion of the wrist and fingers**, and **pronation of the forearm**, as well as sensation to the palmar aspect of the thumb, index, middle, and radial half of the ring finger. - Its injury would not typically cause difficulty with **elbow flexion** or sensory loss over the **lateral forearm**. *Axillary* - The axillary nerve primarily innervates the **deltoid** and **teres minor muscles**, important for shoulder abduction and external rotation. - An injury would lead to **weakness in shoulder abduction** and sensory loss over the lateral shoulder (regimental badge area), not the lateral forearm. *Radial nerve* - The radial nerve controls **extension of the wrist and fingers** and sensation over the posterior arm, forearm, and hand. - Injury typically results in **wrist drop** and difficulty extending the arm, not primarily elbow flexion or lateral forearm sensation. *Ulnar nerve* - The ulnar nerve innervates intrinsic hand muscles and flexor carpi ulnaris, controlling **finger abduction/adduction** and **ulnar wrist flexion**. - Sensory distribution includes the medial hand and medial 1.5 fingers, not the **lateral forearm**. - Injury causes **claw hand deformity** and sensory loss in the medial hand, not the symptoms described.
Question 3: Which blood vessel carries deoxygenated blood back to the placenta?
- A. Inferior vena cava
- B. Umbilical vein
- C. Umbilical artery (Correct Answer)
- D. Ductus venosus
Explanation: ***Umbilical artery*** - The **umbilical arteries** carry **deoxygenated blood** and waste products from the fetus to the placenta [2], [3]. - There are typically **two umbilical arteries** that branch off the internal iliac arteries in the fetus [2]. *Inferior vena cava* - The **inferior vena cava** carries deoxygenated blood from the lower body back to the **fetal heart**, not the placenta. - In a fetus, the inferior vena cava also carries **oxygenated blood** from the umbilical vein through the ductus venosus [1]. *Umbilical vein* - The **umbilical vein** carries **oxygenated blood** and nutrients from the placenta to the fetus [1]. - It bypasses the liver via the **ductus venosus** to deliver blood directly to the inferior vena cava [1]. *Ductus venosus* - The **ductus venosus** is a shunt that allows **oxygenated blood** from the umbilical vein to bypass the fetal liver [1]. - It connects the umbilical vein directly to the **inferior vena cava**, not to the placenta with deoxygenated blood [1].
Question 4: Structure preventing vertical descent of spleen
- A. Ligamentum teres
- B. Ligamentum flavum
- C. Hepatogastric ligament
- D. Phrenocolic ligament (Correct Answer)
- E. Lienorenal ligament
Explanation: ***Phrenocolic ligament*** - The **phrenocolic ligament** is a fold of peritoneum that extends from the left colic (splenic) flexure of the colon to the diaphragm. - It forms a shelf or sling underneath the spleen, providing crucial support and preventing its **vertical descent**. *Ligamentum teres* - The **ligamentum teres hepatis** is the remnant of the obliterated umbilical vein, found in the free margin of the falciform ligament. - It connects the umbilicus to the liver and plays no role in supporting the spleen. *Ligamentum flavum* - The **ligamentum flavum** is a series of elastic ligaments connecting the laminae of adjacent vertebrae in the spinal column. - It is a component of the vertebral column and has no anatomical or functional relationship with the spleen. *Hepatogastric ligament* - The **hepatogastric ligament** is part of the lesser omentum, extending from the liver to the lesser curvature of the stomach. - Its primary function is to contain the **gastric arteries** and connect these organs, not to support the spleen. *Lienorenal ligament* - The **lienorenal ligament** (splenorenal ligament) connects the hilum of the spleen to the anterior surface of the left kidney. - While it provides **lateral support** to the spleen, it does not prevent **vertical descent** as effectively as the phrenocolic ligament.
Question 5: Which nerve is responsible for gag reflex
- A. 11th cranial nerve
- B. 6th Cranial Nerve
- C. 7th Cranial Nerve
- D. 9th Cranial Nerve (Correct Answer)
- E. 10th Cranial Nerve
Explanation: ***9th Cranial Nerve*** - The **glossopharyngeal nerve (CN IX)** is primarily responsible for the **afferent (sensory)** limb of the gag reflex, detecting touch in the posterior pharynx. - It transmits sensory information to the **brainstem**, initiating the efferent response via the vagus nerve. - CN IX is considered the nerve "responsible for" the gag reflex as it **detects and initiates** the protective response. *10th Cranial Nerve* - The **vagus nerve (CN X)** provides the **efferent (motor)** limb of the gag reflex, causing pharyngeal muscle contraction. - While essential for the motor response, CN IX is the primary sensory trigger that initiates the reflex. - Both nerves work together, but CN IX is the **detection nerve** that starts the reflex arc. *11th Cranial Nerve* - The **spinal accessory nerve (CN XI)** primarily innervates the **sternocleidomastoid** and **trapezius muscles**, controlling head and shoulder movements. - It has no direct role in the **gag reflex**. *6th Cranial Nerve* - The **abducens nerve (CN VI)** is responsible for the **lateral rectus muscle** of the eye, controlling **abduction of the eyeball**. - It does not participate in the complex **sensory or motor pathways** of the gag reflex. *7th Cranial Nerve* - The **facial nerve (CN VII)** controls **facial expressions**, taste from the anterior two-thirds of the tongue, and some glandular secretions. - While it has some role in taste and salivation, it is not the primary nerve for the **gag reflex**.
Question 6: A patient underwent a coronary artery bypass graft (CABG) using the great saphenous vein. Post-surgery, the patient experiences neuralgia on the medial aspect of the leg and foot. Which nerve is most likely injured?
- A. Common peroneal nerve
- B. Sural nerve
- C. Tibial nerve
- D. Saphenous nerve (Correct Answer)
- E. Superficial peroneal nerve
Explanation: ***Saphenous nerve*** - The **saphenous nerve** is a cutaneous branch of the femoral nerve that runs closely with the **great saphenous vein** along the medial aspect of the leg and foot. - Due to its proximity to the vein, it is highly susceptible to **injury** during the harvesting of the great saphenous vein for CABG, leading to **neuralgia** in its sensory distribution. *Common peroneal nerve* - The **common peroneal nerve** innervates the lateral and anterior compartments of the leg, affecting dorsiflexion and eversion of the foot. - Damage to this nerve typically results in **foot drop** and sensory loss over the dorsum of the foot, which is inconsistent with the patient's symptoms. *Tibial nerve* - The **tibial nerve** supplies the posterior compartment of the leg and the plantar aspect of the foot. - Injury would cause loss of plantarflexion and sensation on the sole of the foot, which is not described. *Sural nerve* - The **sural nerve** provides sensation to the posterolateral aspect of the leg and the lateral side of the foot and ankle. - While it runs near superficial veins, its sensory distribution does not match the described **medial leg and foot neuralgia**. *Superficial peroneal nerve* - The **superficial peroneal nerve** (superficial fibular nerve) provides sensation to the dorsum of the foot and anterolateral leg. - Injury would cause sensory loss over the dorsal foot, not the medial aspect of the leg and foot.
Internal Medicine
1 questionsA patient presents with cold skin, fatigue, shortness of breath on exertion, and an enlarged liver. Upon examination, his jugular venous pressure (JVP) reveals a prominent "a" wave. What is the most likely cause of the elevated "a" wave in this patient?
NEET-PG 2021 - Internal Medicine NEET-PG Practice Questions and MCQs
Question 1: A patient presents with cold skin, fatigue, shortness of breath on exertion, and an enlarged liver. Upon examination, his jugular venous pressure (JVP) reveals a prominent "a" wave. What is the most likely cause of the elevated "a" wave in this patient?
- A. Tricuspid Stenosis (Correct Answer)
- B. Mitral Stenosis
- C. Tricuspid Regurgitation
- D. Mitral Regurgitation
- E. Pulmonary Stenosis
Explanation: ***Tricuspid Stenosis*** - A prominent "a" wave in the **JVP** indicates increased **right atrial pressure** during atrial contraction, which is characteristic of **tricuspid stenosis** due to resistance to blood flow from the right atrium to the right ventricle. - The symptoms of **cold skin**, **fatigue**, **shortness of breath on exertion**, and an **enlarged liver** are consistent with **right-sided heart failure** caused by tricuspid stenosis. - Among the valvular causes, tricuspid stenosis most directly causes a prominent "a" wave with associated right heart failure symptoms. *Mitral Stenosis* - **Mitral stenosis** primarily affects the **left atrium** and left ventricle, leading to pulmonary symptoms and, if severe, right heart failure. - It would typically cause a prominent "a" wave in the **pulmonary veins**, not directly in the JVP, although severe pulmonary hypertension could eventually lead to right ventricular overload. *Tricuspid Regurgitation* - **Tricuspid regurgitation** causes a large, prominent, and often **pulsatile "c-v" wave** in the JVP due to the reflux of blood into the right atrium during ventricular systole. - While it can cause right heart failure symptoms, it does not typically present with an isolated prominent "a" wave. *Mitral Regurgitation* - **Mitral regurgitation** primarily affects the **left side of the heart**, leading to symptoms related to left heart failure (e.g., pulmonary edema). - It does not directly cause an elevated "a" wave in the **JVP** unless there is severe, longstanding left-sided heart failure leading to secondary pulmonary hypertension and right heart failure. *Pulmonary Stenosis* - **Pulmonary stenosis** causes obstruction to right ventricular outflow, which can lead to a prominent "a" wave due to increased right atrial pressure. - However, pulmonary stenosis typically presents with a **systolic ejection murmur** at the left upper sternal border and may have signs of **RV hypertrophy** rather than the predominantly congestive symptoms seen here. - The clinical picture of hepatomegaly and signs of backward failure is more consistent with tricuspid stenosis than pulmonary stenosis.
Pharmacology
1 questionsBeta 2 receptors act via which of the following secondary messenger systems
NEET-PG 2021 - Pharmacology NEET-PG Practice Questions and MCQs
Question 1: Beta 2 receptors act via which of the following secondary messenger systems
- A. Adenylate Cyclase (Correct Answer)
- B. Phospholipase C
- C. Guanylate Cyclase
- D. Direct ion channel activation
- E. Tyrosine Kinase
Explanation: ***Adenylate Cyclase*** - **Beta-2 adrenergic receptors** are G-protein coupled receptors that primarily activate the **Gs protein**. - Activation of Gs protein leads to the stimulation of **adenylate cyclase**, which converts ATP to **cAMP**, a crucial secondary messenger for various cellular responses. *Phospholipase C* - **Phospholipase C** is typically activated by **Gq protein-coupled receptors**, such as alpha-1 adrenergic receptors or M1/M3 muscarinic receptors. - Its activation leads to the production of **IP3** and **DAG**, which then trigger intracellular calcium release and protein kinase C activation, respectively. *Guanylate Cyclase* - **Guanylate cyclase** produces **cGMP** as a secondary messenger and is primarily associated with **nitric oxide signaling** (soluble guanylate cyclase) or **natriuretic peptide receptors** (particulate guanylate cyclase). - This system is distinct from the adrenergic receptor pathways. *Direct ion channel activation* - **Direct ion channel activation** occurs in **ligand-gated ion channels**, where the binding of a neurotransmitter directly opens an ion pore without the involvement of G-proteins or secondary messengers. - Examples include nicotinic acetylcholine receptors and GABA-A receptors, which are functionally different from the G-protein coupled **beta-2 receptors**. *Tyrosine Kinase* - **Tyrosine kinase** signaling is characteristic of **receptor tyrosine kinases (RTKs)**, such as insulin receptors and growth factor receptors (e.g., EGF, PDGF receptors). - These receptors undergo autophosphorylation and initiate signaling cascades independent of G-proteins, making them distinct from **beta-2 adrenergic receptors**.
Physiology
2 questionsA child presented with dehydration and was supplemented with ORS solution for management. Which of the following transporters help in the absorption of glucose from GIT?
The body fluid compartments of a patient were measured, showing the following ion concentrations: - Sodium (Na): $10 \mathrm{mEq} / \mathrm{L}$ - Potassium (K): $140 \mathrm{mEq} / \mathrm{L}$ - Chloride (Cl): $15 \mathrm{mEq} / \mathrm{L}$ Based on these values, which fluid compartment is being described?
NEET-PG 2021 - Physiology NEET-PG Practice Questions and MCQs
Question 1: A child presented with dehydration and was supplemented with ORS solution for management. Which of the following transporters help in the absorption of glucose from GIT?
- A. GLUT 2
- B. SGLT 1 (Correct Answer)
- C. SGLT 2
- D. GLUT 1
Explanation: ***SGLT 1*** - **SGLT1 (Sodium-Glucose Co-transporter 1)** is responsible for the **active transport of glucose and galactose** from the intestinal lumen into the enterocytes, coupled with sodium. - The principle of **oral rehydration solutions (ORS)** relies on this co-transport mechanism, as glucose (or other carbohydrates like sucrose, which is broken down into glucose and fructose) facilitates the absorption of sodium and water across the intestinal wall. *GLUT 2* - **GLUT2** is primarily located on the **basolateral membrane of enterocytes** and facilitates glucose transport out of the cell into the bloodstream. It also plays a role in glucose uptake in the liver and pancreatic beta cells. - While involved in glucose handling, **GLUT2 does not absorb glucose from the intestinal lumen** into the enterocytes; rather, it transports glucose out of them. *SGLT 2* - **SGLT2 (Sodium-Glucose Co-transporter 2)** is predominantly found in the **proximal tubules of the kidneys**, where it is responsible for the reabsorption of the vast majority of filtered glucose back into the bloodstream. - It is not involved in **intestinal glucose absorption**. Selective SGLT2 inhibitors are used as antidiabetic drugs to promote glucose excretion via the kidneys. *GLUT 1* - **GLUT1 (Glucose Transporter 1)** is a ubiquitous glucose transporter found in nearly all cell types, particularly important for basal glucose uptake by tissues like the **brain** and **red blood cells**. - While essential for glucose transport in many tissues, **GLUT1 plays a negligible role in glucose absorption from the gastrointestinal tract**.
Question 2: The body fluid compartments of a patient were measured, showing the following ion concentrations: - Sodium (Na): $10 \mathrm{mEq} / \mathrm{L}$ - Potassium (K): $140 \mathrm{mEq} / \mathrm{L}$ - Chloride (Cl): $15 \mathrm{mEq} / \mathrm{L}$ Based on these values, which fluid compartment is being described?
- A. Plasma
- B. ICF (Correct Answer)
- C. Interstitial fluid
- D. ECF
Explanation: ***ICF*** - The measured ion concentrations, especially **high potassium (140 mEq/L)** and **low sodium (10 mEq/L)**, are characteristic of the **intracellular fluid (ICF)**, where potassium is the primary cation and sodium is kept low by the Na+/K+-ATPase pump. - **Chloride levels (15 mEq/L)** are also significantly lower in the ICF compared to extracellular fluids. *Plasma* - Plasma typically has **high sodium (around 140 mEq/L)** and **low potassium (around 4 mEq/L)**, which contradicts the given measurements. - Chloride levels in plasma are usually much higher, around **100-105 mEq/L**. *Interstitial fluid* - Interstitial fluid has an electrolyte composition very similar to plasma, with **high sodium** and **low potassium**, differing mainly in protein content. - This composition is not consistent with the given measurements. *ECF* - The ECF (extracellular fluid), which includes both plasma and interstitial fluid, is characterized by **high sodium** and **low potassium**. - The given ion concentrations, particularly the very **high potassium** and **low sodium**, are directly opposite to the typical ECF profile.
About NEET-PG 2021 Questions
This page contains 176 questions from the NEET-PG 2021 paper, organised across 27 subjects for focused practice. Every question comes with the correct answer and a detailed explanation to help you understand the underlying concept. Subject-wise organisation lets you target specific areas and identify which topics carried the most weight in this particular year.
Practising year-wise papers is essential for understanding how the NEET-PG exam evolves — you can spot trending topics, gauge difficulty shifts, and benchmark your readiness against a real paper. To take your preparation further, download the Oncourse app for AI-driven performance insights, spaced repetition of questions you got wrong, and a personalised study plan built around your NEET-PG goals.