NEET-PG 2018 — Surgery
5 Previous Year Questions with Answers & Explanations
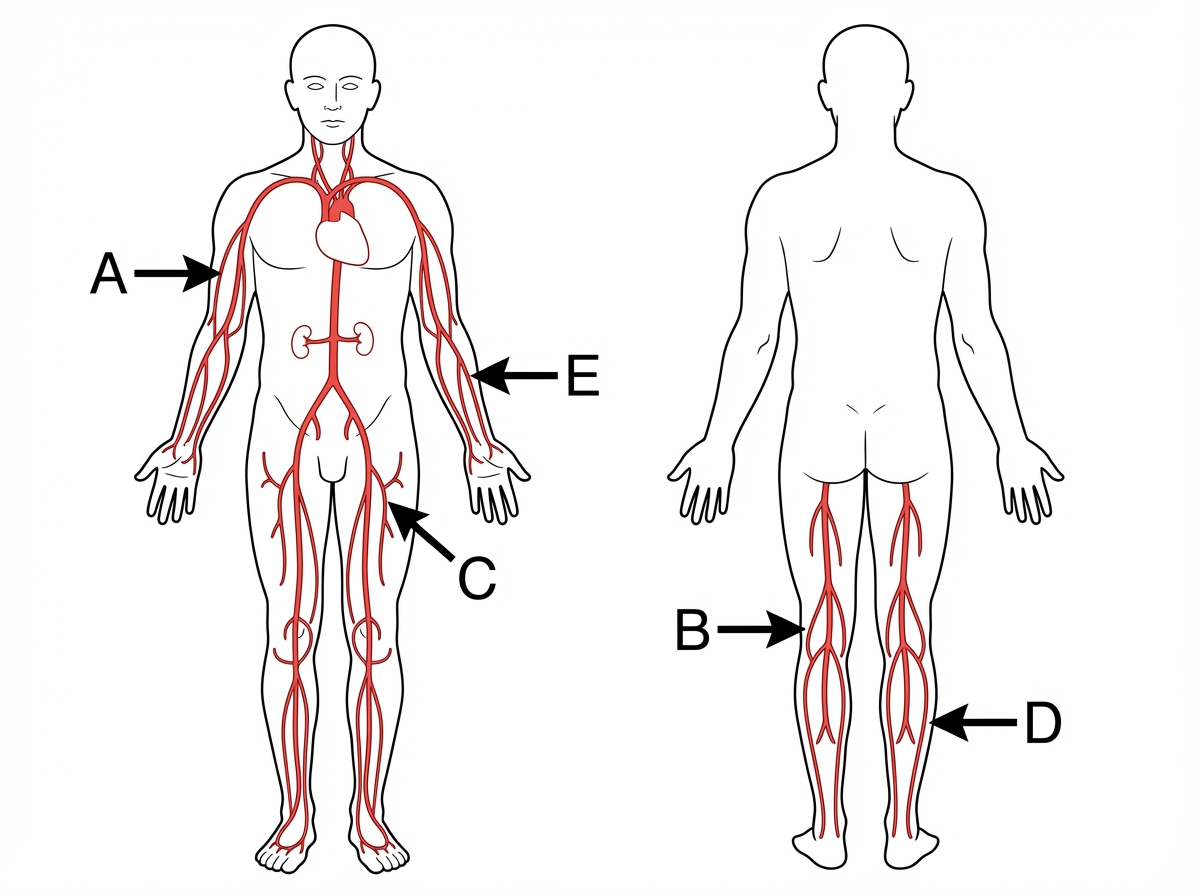
Which is the most common site of peripheral aneurysm?
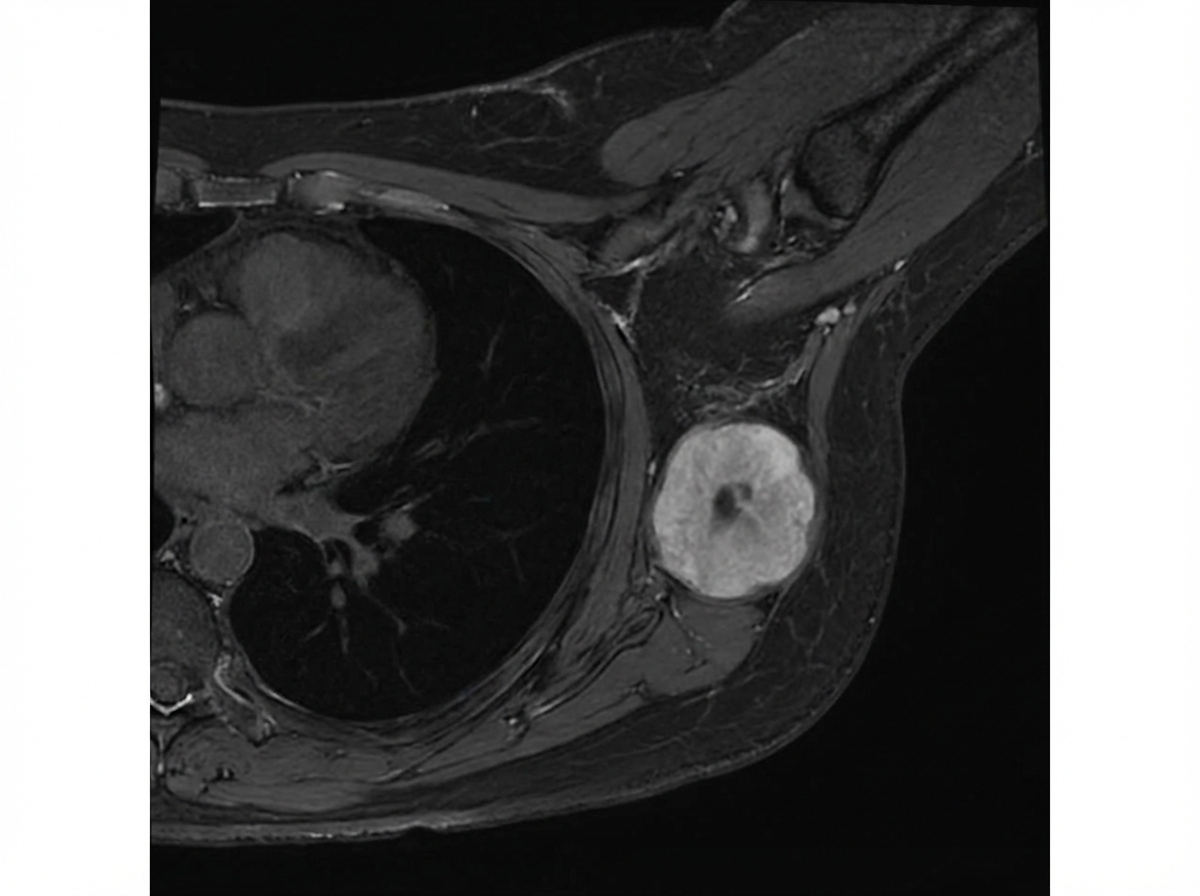
In the MRI breast shown below, 4 cm mass is present with no nodal metastasis. Which is the stage of breast cancer?
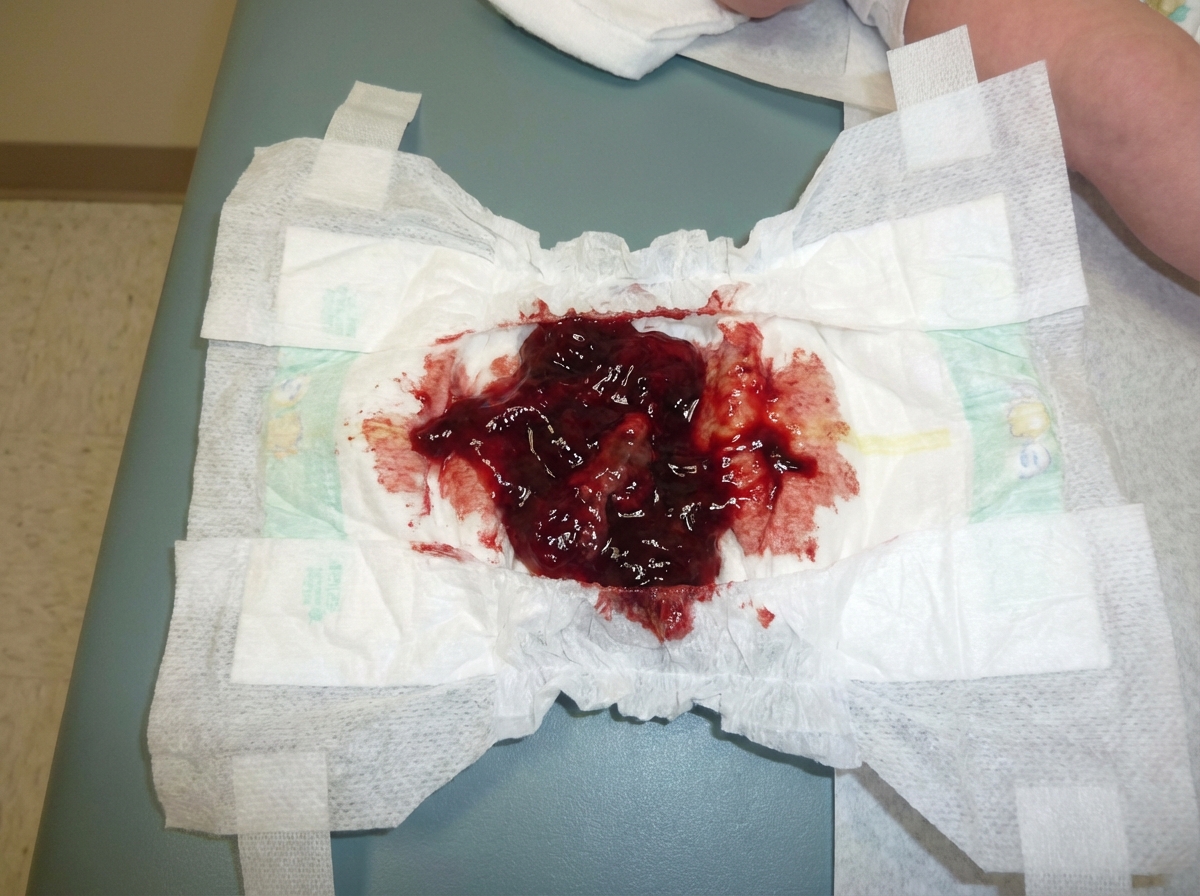
A 9-month-old child presents with excessive cry and presentation shown below. On examination right iliac fossa sausage shaped lump is felt. What is the best treatment?
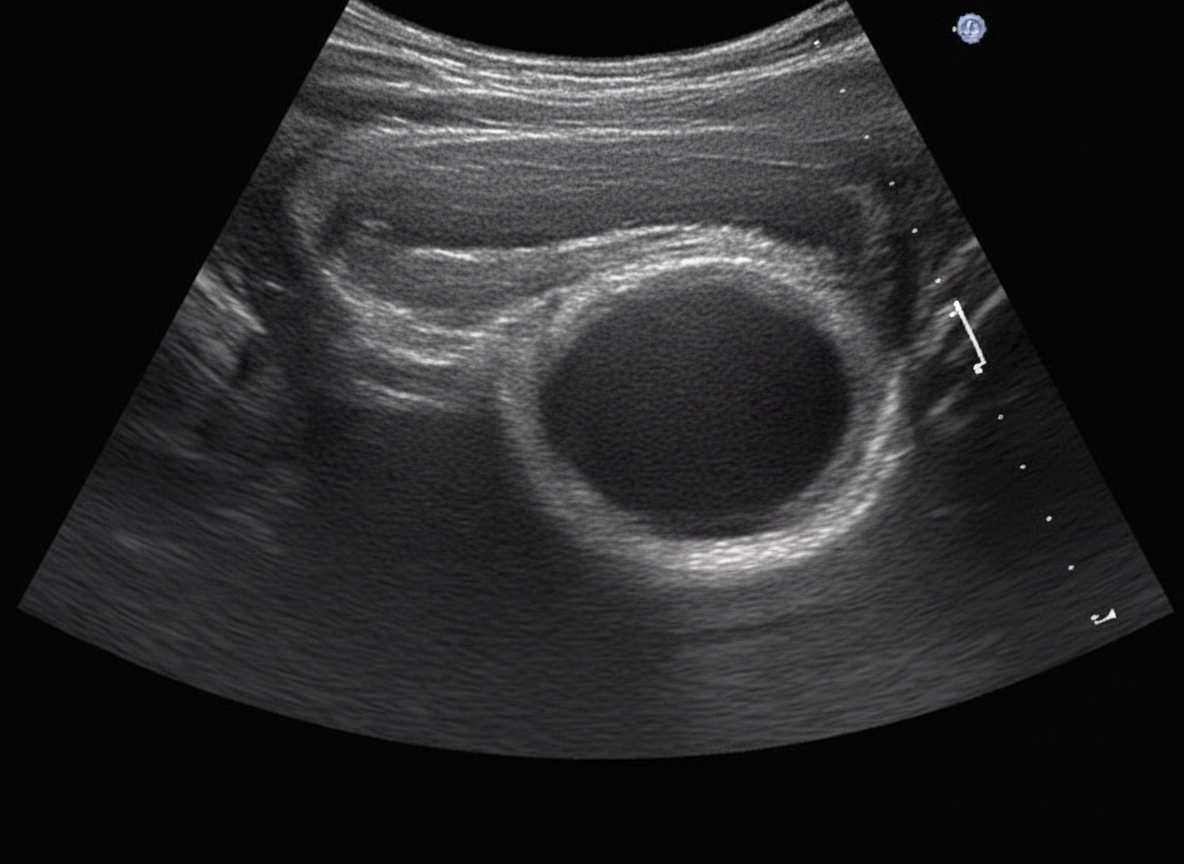
Which of the following is not an indication for surgery in the condition shown below?
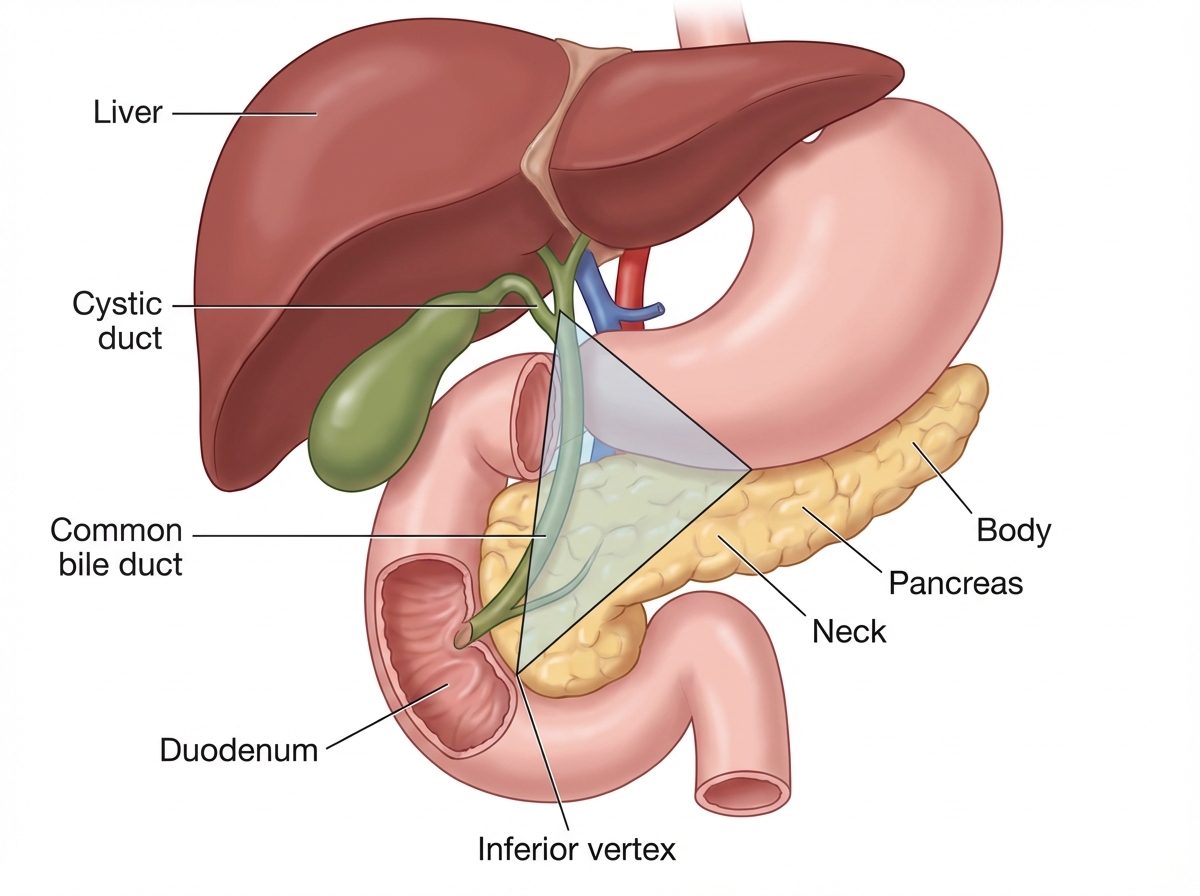
Which is correct about tumor found in the triangle location shown below?
NEET-PG 2018 - Surgery NEET-PG Practice Questions and MCQs
Question 1: Which is the most common site of peripheral aneurysm?
- A. A
- B. B (Correct Answer)
- C. C
- D. D
- E. E
Explanation: ***Option B*** - This image points to the **popliteal artery**, which is the most common site for **peripheral aneurysms**. - **Popliteal artery aneurysms** account for approximately 70% of all peripheral aneurysms and are more common in men. *Option A* - This image points to the **brachial artery** in the upper arm, which is a less common site for aneurysms. - While aneurysms can occur here, they are not as frequent as in the popliteal artery. *Option C* - This image points to the **femoral artery** in the groin region. - Although the femoral artery can be affected by aneurysms, they are less common than popliteal artery aneurysms. *Option D* - This image points to the **tibial arteries** in the lower leg. - Aneurysms in the tibial arteries are rare and typically much less common than those in the popliteal artery. *Option E* - This image points to the **radial artery** in the forearm. - Radial artery aneurysms are very rare and usually occur secondary to trauma or iatrogenic injury, not spontaneously like popliteal aneurysms.
Question 2: In the MRI breast shown below, 4 cm mass is present with no nodal metastasis. Which is the stage of breast cancer?
- A. Stage I
- B. Stage II (Correct Answer)
- C. Stage III
- D. Stage IV
- E. Stage 0
Explanation: ***Stage II*** - A tumor of **4 cm** with no nodal metastasis is classified as pT2, N0, M0. This falls under **Stage IIA** breast cancer according to the TNM staging system. - Stage II breast cancer typically includes tumors that are larger than 2 cm but not larger than 5 cm (T2N0), or smaller tumors with lymph node involvement. - The **4 cm size with N0 status** specifically defines Stage IIA. *Stage 0* - Stage 0 represents **ductal carcinoma in situ (DCIS)** or **lobular carcinoma in situ (LCIS)**, which are non-invasive breast cancers. - This case describes a **4 cm mass**, indicating an invasive tumor, not in-situ disease, ruling out Stage 0. *Stage I* - Stage I breast cancer includes tumors that are **2 cm or smaller** (T1) and have no lymph node involvement (N0). - Since the mass is **4 cm**, it exceeds the size criteria for Stage I. *Stage III* - Stage III breast cancer involves **larger tumors** (greater than 5 cm) or any tumor size with extensive lymph node involvement, or tumors invading the chest wall/skin. - While this mass is 4 cm, there is **no nodal metastasis**, which rules out Stage III. *Stage IV* - Stage IV breast cancer indicates the presence of **distant metastases** (M1), meaning the cancer has spread to other parts of the body. - The information provided clearly states **no nodal metastasis**, and no information about distant spread, therefore Stage IV is incorrect.
Question 3: A 9-month-old child presents with excessive cry and presentation shown below. On examination right iliac fossa sausage shaped lump is felt. What is the best treatment?
- A. IVF- Antibiotic- NG tube
- B. IVF- Antibiotic-Air enema (Correct Answer)
- C. IVF-Antibiotics- Barium enema
- D. IVF- Antibiotics-Warm saline enema
- E. IVF- Antibiotics- Laparotomy
Explanation: ***IVF- Antibiotic-Air enema*** - The clinical picture (9-month-old with excessive cry, **"currant jelly" stool** (image), and a **right iliac fossa sausage-shaped lump**) is classic for **intussusception**. - Initial management involves **resuscitation** (IV fluids), **antibiotics** to prevent sepsis from bowel ischemia, and then an **air enema** for both diagnosis and non-surgical reduction. - Air enema has a **success rate of 70-90%** for uncomplicated cases and is the **first-line treatment**. *IVF- Antibiotic- NG tube* - While IVF and antibiotics are appropriate initial steps for an ill child with presumed intussusception, an **NG tube** alone is insufficient for treating the intussusception itself. - An NG tube is primarily used for **gastric decompression** in cases of bowel obstruction, which may be a complication of intussusception, but it does not resolve the invagination. *IVF-Antibiotics- Barium enema* - A **barium enema** can also be used for reduction, but an **air enema** is generally preferred due to a **lower risk of peritoneal contamination** if perforation occurs and better visualization under fluoroscopy. - While it has diagnostic and therapeutic potential, air enema is often considered safer and equally effective. *IVF- Antibiotics-Warm saline enema* - This option lacks the specific pressure-based mechanism required to reduce an intussusception effectively. - A **warm saline enema** is a general type of enema, but it does not provide the controlled pressure needed for hydrostatic or pneumatic reduction of intussusception. *IVF- Antibiotics- Laparotomy* - **Laparotomy** (surgical reduction) is reserved for cases where **pneumatic reduction fails**, **signs of peritonitis** are present, or there is **suspected bowel perforation**. - Initial management should always attempt non-surgical reduction first unless contraindications exist (free air, hemodynamic instability, peritonitis).
Question 4: Which of the following is not an indication for surgery in the condition shown below?
- A. Patient's decision (Correct Answer)
- B. Size more than 5 cm
- C. Complex type
- D. Recurrence
- E. Rapid increase in size
Explanation: ***Patient's decision*** - While patient preferences are crucial in medical decision-making, simply the **patient's decision alone is not a primary medical indication for surgery** in the absence of other objective criteria for a fibroadenoma. - Surgery for **fibroadenoma** is typically guided by clinical and radiological findings, not solely by patient request. *Size more than 5 cm* - A **fibroadenoma** with a size of **more than 5 cm** is generally considered a strong indication for surgical excision. - Large fibroadenomas can cause **cosmetic distortion**, discomfort, and may be harder to distinguish from malignant lesions, especially if they show rapid growth. *Complex type* - **Complex fibroadenomas** have features such as **cysts larger than 3 mm**, sclerosing adenosis, epithelial calcifications, or papillary apocrine metaplasia. - These features are associated with a slightly **increased risk of future breast cancer** and are often considered an indication for excision to rule out malignancy and for risk reduction. *Recurrence* - If a **fibroadenoma recurs** after previous excision, particularly if it grows rapidly or shows atypical features, surgical removal is indicated. - **Recurrence** suggests a persistent or potentially more aggressive benign process that warrants further investigation and management. *Rapid increase in size* - A **rapid increase in size** of a fibroadenoma is a clear indication for surgical excision. - Rapid growth raises concern for **phyllodes tumor** or other potentially aggressive lesions and warrants histopathological examination. - Serial measurements showing significant growth over a short period (typically doubling in size over 3-6 months) indicate the need for surgical intervention.
Question 5: Which is correct about tumor found in the triangle location shown below?
- A. Associated with MEN1 (Correct Answer)
- B. Most common site is stomach
- C. Best test for diagnosis is pentagastrin test
- D. Metastasis to adjacent gut
- E. Primary treatment is medical with proton pump inhibitors
Explanation: ***Associated with MEN1*** - The triangle shown in the image represents the **Gastrinoma Triangle**, a common location for gastrin-producing tumors (gastrinomas) to occur. - Approximately 20-30% of gastrinomas are associated with **Multiple Endocrine Neoplasia type 1 (MEN1)** syndrome, which involves tumors of the parathyroid glands, pituitary gland, and pancreas. *Most common site is stomach* - The most common primary site for gastrinomas is the **duodenum** (50-70%), followed by the pancreas (20-40%). - Gastrinomas found in the stomach are rare and usually associated with MEN1, but the duodenum is the predominant site overall. *Best test for diagnosis is pentagastrin test* - The **pentagastrin stimulation test** is used to assess maximal acid output but it is not specific for diagnosing gastrinomas. - The **secretin stimulation test** is the most sensitive and specific provocative test for gastrinoma, as secretin normally inhibits gastrin release from G cells but paradoxically stimulates it in gastrinomas. *Metastasis to adjacent gut* - Gastrinomas are malignant neuroendocrine tumors that commonly **metastasize to regional lymph nodes** and the **liver**. - While they can invade locally, metastasis typically involves distant sites rather than just the adjacent gut wall. *Primary treatment is medical with proton pump inhibitors* - While **proton pump inhibitors (PPIs)** are essential for managing acid hypersecretion symptoms, they are not the primary definitive treatment. - **Surgical resection** is the primary treatment for localized, sporadic gastrinomas when feasible, offering potential cure. - PPIs serve as adjunctive medical therapy to control symptoms but do not address the underlying tumor.