Coagulation testing is needed for:
Amphotericin B acts on:-
Drug which lacks intrinsic activity against anaerobes is:-
All are false about tigecycline, except:-
What is the mechanism of action of colchicine in acute gout?
Choice of drug for management of the parasitic infection shown below is:

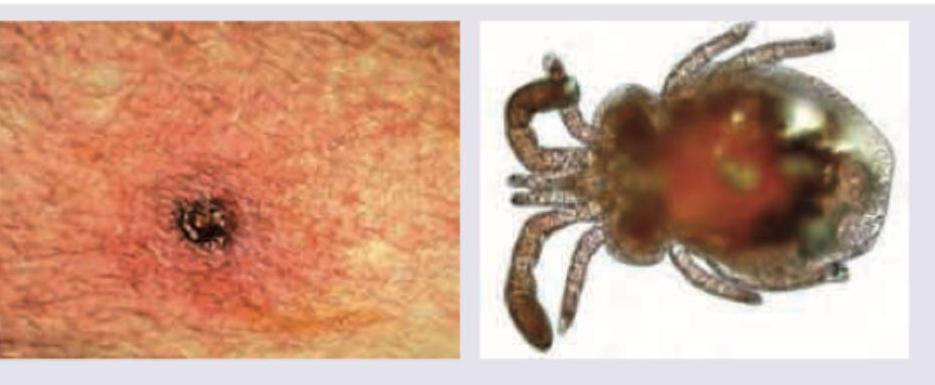
Best drug for the condition shown below is: (NEET Jan 2018)
NEET-PG 2018 - Pharmacology NEET-PG Practice Questions and MCQs
Question 21: Coagulation testing is needed for:
- A. Lepirudin (direct thrombin inhibitor) (Correct Answer)
- B. Dabigatran (oral anticoagulant)
- C. Enoxaparin (low molecular weight heparin)
- D. Fondaparinux (synthetic pentasaccharide)
Explanation: ***Lepirudin (direct thrombin inhibitor)*** - **Lepirudin**, being a direct thrombin inhibitor, necessitates **coagulation testing** (such as aPTT) to monitor its anticoagulant effect and adjust dosing, especially in patients with renal impairment. - Its narrow therapeutic window and potential for bleeding complications require careful monitoring to ensure patient safety and drug efficacy, as it lacks a specific antidote. *Dabigatran (oral anticoagulant)* - **Dabigatran** is a **direct oral anticoagulant (DOAC)** that typically does not require routine coagulation monitoring due to its predictable pharmacokinetic and pharmacodynamic profiles. - While specific tests can assess its effect in emergencies, they are not part of standard management, distinguishing it from drugs requiring regular monitoring. *Enoxaparin (low molecular weight heparin)* - **Enoxaparin**, a **low molecular weight heparin (LMWH)**, usually does not require routine coagulation monitoring in most patients due to its predictable dose-response relationship. - Monitoring with anti-Xa levels may be considered in specific populations, such as those with renal insufficiency, extremes of weight, or in pediatric and pregnant patients. *Fondaparinux (synthetic pentasaccharide)* - **Fondaparinux** is a synthetic pentasaccharide that **does not require routine coagulation monitoring** as its anticoagulant effect is highly predictable and dose-dependent. - Its action is mediated through selective inhibition of **Factor Xa**, and standard coagulation tests like aPTT or PT are not sensitive to its effects.
Question 22: Amphotericin B acts on:-
- A. Cell membrane (Correct Answer)
- B. Cytoplasm
- C. Nucleus
- D. Cell wall
Explanation: ***Cell membrane*** Amphotericin B primarily targets the **ergosterol** in the fungal **cell membrane** [1]. It binds to **ergosterol**, forming pores and disrupting the membrane's integrity, leading to leakage of cellular contents and ultimately cell death [1]. *Cytoplasm* The cytoplasm is the internal fluid of the cell where many metabolic processes occur, but it is **not the primary target** of amphotericin B's fungicidal action. While cytoplasmic contents leak out due to membrane damage, the drug does not directly act on cytoplasmic components to exert its effect. *Nucleus* The nucleus contains the genetic material of the fungal cell, but amphotericin B does **not directly interact with nuclear components** or DNA. Damage to the cell membrane is the primary mechanism, with nuclear function only indirectly affected by overall cellular disruption. *Cell wall* Fungal cell walls are composed of **chitin and glucans**, but amphotericin B **does not target these components**. Its action is distinct from drugs that inhibit cell wall synthesis, such as echinocandins.
Question 23: Drug which lacks intrinsic activity against anaerobes is:-
- A. Beta lactams
- B. Aminoglycosides (Correct Answer)
- C. Metronidazole
- D. Chloramphenicol
Explanation: ***Aminoglycosides*** - Aminoglycosides require an **oxygen-dependent transport system** to enter bacterial cells and exert their effects. - Due to the **anaerobic environment**, this transport system is inactive, rendering aminoglycosides ineffective against anaerobic bacteria. *Beta lactams* - Many beta-lactam antibiotics, especially certain **cephalosporins (e.g., cefoxitin, cefotetan)** and **carbapenems (e.g., imipenem, meropenem)**, have significant activity against anaerobes. - They inhibit **cell wall synthesis** and are a common choice for infections involving anaerobes. *Metronidazole* - **Metronidazole** is a potent and widely used antibiotic specifically effective against a broad spectrum of **anaerobic bacteria** and protozoa. - It acts by forming **cytotoxic reduced products** that disrupt bacterial DNA synthesis in anaerobic conditions. *Chloramphenicol* - **Chloramphenicol** is a broad-spectrum antibiotic that is highly effective against both aerobic and **anaerobic bacteria**. - It works by binding to the **50S ribosomal subunit**, thereby inhibiting bacterial protein synthesis.
Question 24: All are false about tigecycline, except:-
- A. 90% pseudomonas strains are sensitive
- B. It is bactericidal drug
- C. It is a broad spectrum antimicrobial (Correct Answer)
- D. Dose reduction is required in renal failure
Explanation: ***It is a broad spectrum antimicrobial*** - **Tigecycline** is known for its wide spectrum of activity, effective against a variety of gram-positive, gram-negative, and anaerobic bacteria. - It is particularly useful in treating infections caused by **multidrug-resistant (MDR)** organisms, including MRSA and VRE. *90% pseudomonas strains are sensitive* - Tigecycline generally has **poor activity** against *Pseudomonas aeruginosa*, and its use is specifically cautioned against for such infections. - **Many *Pseudomonas* strains are intrinsically resistant** to tigecycline, making it an unreliable choice for treating these infections. *It is bactericidal drug* - Tigecycline is a **bacteriostatic** antibiotic, meaning it inhibits bacterial growth rather than directly killing bacteria. - It achieves its effect by binding to the **30S ribosomal subunit**, thereby blocking protein synthesis. *Dose reduction is required in renal failure* - **Tigecycline** is primarily eliminated via **biliary and fecal excretion**, with only a small portion excreted renally. - Therefore, **dose adjustments are generally not required** in patients with renal impairment, but caution is usually advised in severe hepatic impairment.
Question 25: What is the mechanism of action of colchicine in acute gout?
- A. Renal disease involving interstitial tissues
- B. Uric acid nephrolithiasis
- C. Deficiency of enzyme Xanthine oxidase
- D. Inhibition of leukocyte migration and phagocytosis (Correct Answer)
Explanation: ***Inhibition of leukocyte migration and phagocytosis*** - Colchicine primarily exerts its anti-inflammatory effect in acute gout by **binding to tubulin**, which inhibits microtubule polymerization. - This action disrupts essential cellular functions in inflammatory cells, particularly **neutrophils**, thereby reducing their migration to inflamed sites and their ability to phagocytose uric acid crystals. *Renal disease involving interstitial tissues* - This option describes a potential complication or manifestation of gout, such as **urate nephropathy**, rather than the mechanism of action of colchicine. - Colchicine does not directly target or treat pre-existing renal interstitial tissue disease as its primary mechanism for acute gout relief. *Uric acid nephrolithiasis* - This condition involves the formation of **kidney stones from uric acid** and is a consequence of chronic hyperuricemia. - Colchicine is not used to acutely treat or prevent the formation of uric acid kidney stones; its role is in managing the inflammatory arthritis of gout. *Deficiency of enzyme Xanthine oxidase* - **Xanthine oxidase** is an enzyme involved in the production of uric acid, and its inhibition (e.g., by allopurinol or febuxostat) is a strategy to lower uric acid levels in the blood. - Colchicine does not affect xanthine oxidase activity; it works downstream by modulating the inflammatory response to uric acid crystals.
Question 26: Choice of drug for management of the parasitic infection shown below is:
- A. Albendazole
- B. Praziquantel
- C. Niclosamide
- D. Triclabendazole (Correct Answer)
Explanation: ***Triclabendazole*** - The image displays an adult **Fasciola hepatica** (liver fluke), characterized by its **leaf-like shape** and the prominent **anterior cone** terminating in an oral sucker. - **Triclabendazole** is the drug of choice for treating **fascioliasis**, as it effectively kills both immature and mature forms of Fasciola hepatica. *Albendazole* - **Albendazole** is primarily used to treat a wide range of **intestinal nematode infections** (e.g., Ascaris, hookworm, whipworm) and some **cestode infections** (e.g., neurocysticercosis, echinococcosis). - It has **limited efficacy** against trematodes like Fasciola hepatica. *Praziquantel* - **Praziquantel** is a broad-spectrum antihelminthic drug effective against most **trematodes (flukes)**, including schistosomes and other liver flukes (e.g., Clonorchis, Opisthorchis), and **cestodes (tapeworms)**. - However, it is **ineffective against Fasciola hepatica**, making it unsuitable for this specific infection. *Niclosamide* - **Niclosamide** is an oral anthelmintic primarily used to treat **tapeworm infections (cestodiasis)**, including Taenia species and Hymenolepis nana. - It is **not effective against trematodes** like Fasciola hepatica.
Question 27: Best drug for the condition shown below is: (NEET Jan 2018)
- A. Ivermectin
- B. Doxycycline (Correct Answer)
- C. Sulphonamides
- D. Penicillin
Explanation: ***Correct: Doxycycline*** - The image shows a **tick embedded in the skin** with surrounding erythema, indicative of a **tick bite** and potential **Lyme disease** or other tick-borne infections. - **Doxycycline** is the **drug of choice** for early Lyme disease (caused by *Borrelia burgdorferi*) and many other common tick-borne illnesses like Rickettsial infections (e.g., Rocky Mountain Spotted Fever) and Anaplasmosis. *Incorrect: Ivermectin* - **Ivermectin** is primarily used to treat **parasitic worm infections** like onchocerciasis, strongyloidiasis, and scabies. - It is **not effective** against bacterial infections transmitted by ticks. *Incorrect: Sulphonamides* - **Sulphonamides** are a class of **antibiotics** effective against various bacterial infections, but they are generally **not the first-line treatment** for tick-borne diseases. - For tick-borne illnesses, **doxycycline** typically has broader and more effective coverage. *Incorrect: Penicillin* - **Penicillin** is an **antibiotic** primarily effective against a range of gram-positive and some gram-negative bacteria, and spirochetes like *Treponema pallidum*. - While it has some activity against *Borrelia burgdorferi* (Lyme disease), **doxycycline is preferred** for early-stage Lyme disease and is specifically active against other common tick-borne pathogens where penicillin is not.