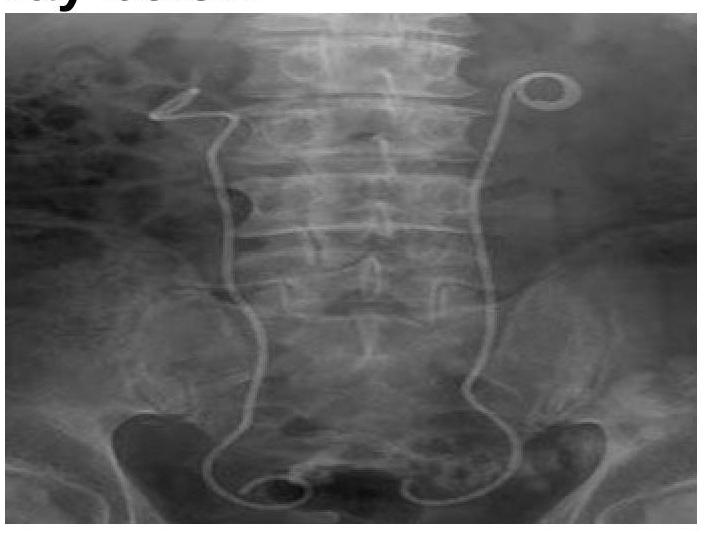
What is the structure seen in the X-ray?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Which chromosome is responsible for the production of MIF?
Which of the following is an example of an X-linked disorder?
Patient presenting with cutaneous vasculitis, glomerulonephritis, peripheral neuropathy, Which investigation is to be performed next that will help you diagnose the condition?
Which of the following organisms is MOST associated with histamine production in scombroid fish poisoning?
Which of the following methods is known as a fimbriectomy procedure?
Long-standing pelvic inflammatory disease (PID) may lead to which of the following complications?
Which gene is primarily associated with Cowden syndrome?
Anaplasia is
In hypovolemic shock there is -
What is the structure seen in the X-ray?
