All (353)Anatomy (24)Anesthesiology (4)Biochemistry (1)Biochemistry (26)Community Medicine (12)Dental (1)Dermatology (8)ENT (1)Forensic Medicine (2)General Medicine (7)Internal Medicine (41)Microbiology (22)Obstetrics and Gynecology (23)Ophthalmology (2)Orthopaedics (1)Pathology (3)Pathology (31)Pediatrics (24)Pharmacology (27)Physiology (13)Psychiatry (3)Psychiatry (10)Radiology (30)Surgery (5)Surgery (32)
Q41
Best time to perform the quadruple test is:
Q42
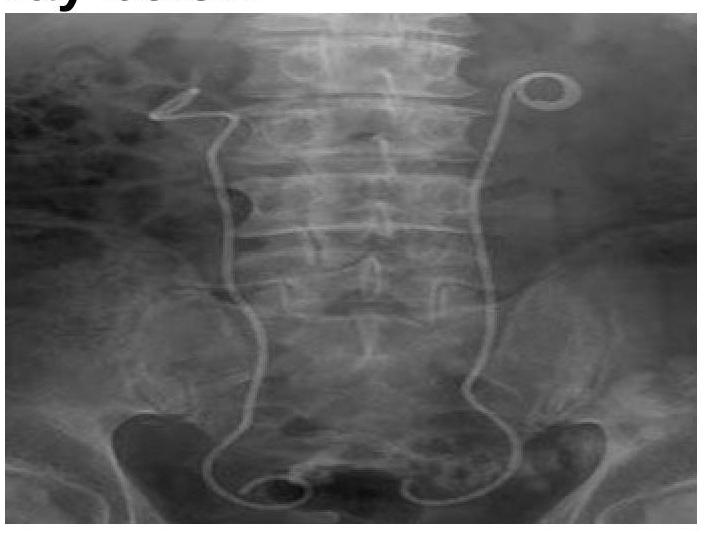
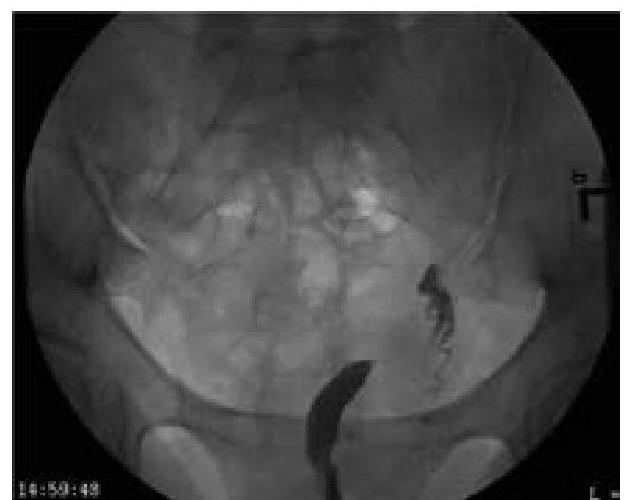
What type of uterine anomaly is shown in this X-ray HSG image?
Q43
What are the effects of Progesterone-only pills?
Q44
Which of the following is not a high-risk pregnancy?
Q45
What is meant by Superfecundation?