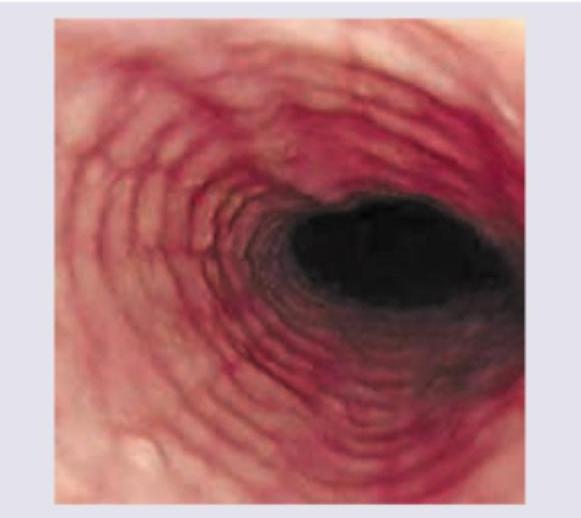
The following appearance of esophagus is seen in:
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
The following appearance of esophagus is seen in:

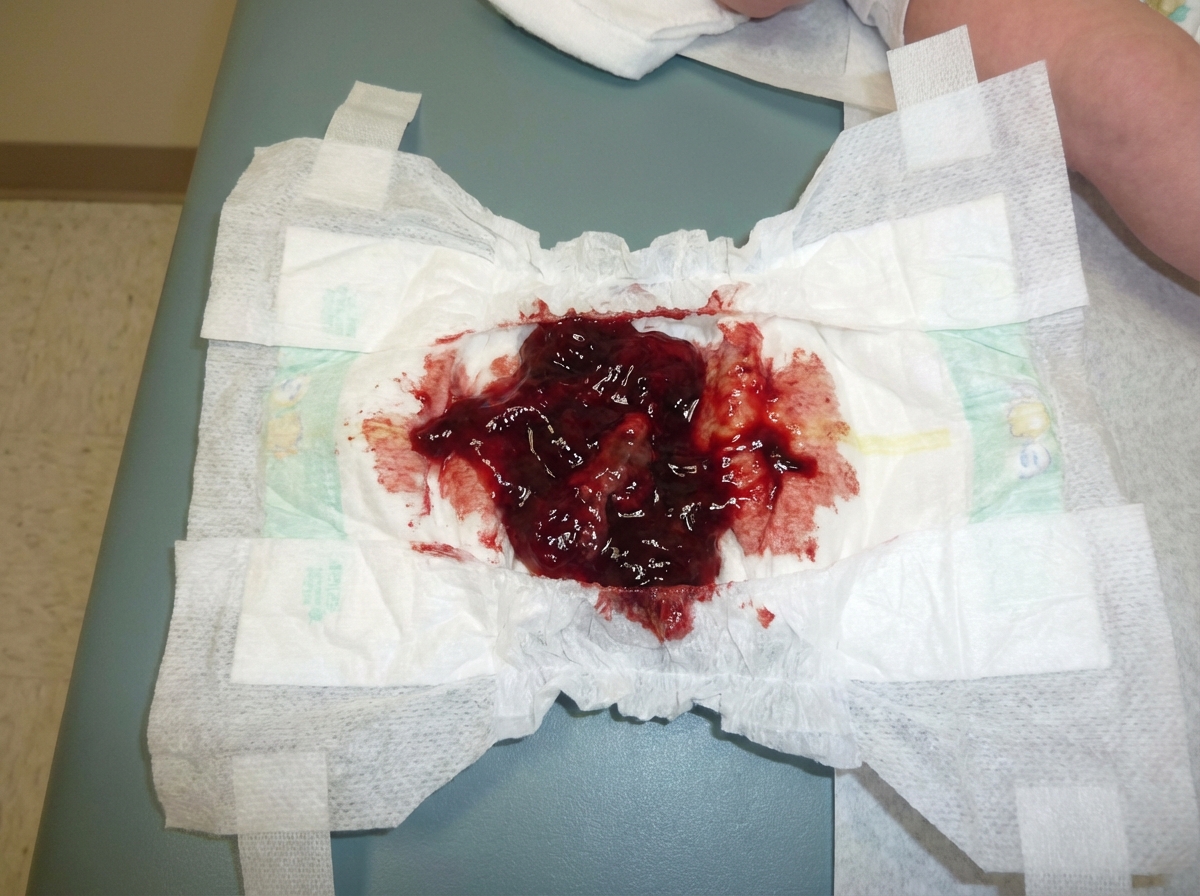
A 9-month-old child presents with excessive cry and presentation shown below. On examination right iliac fossa sausage shaped lump is felt. What is the best treatment?
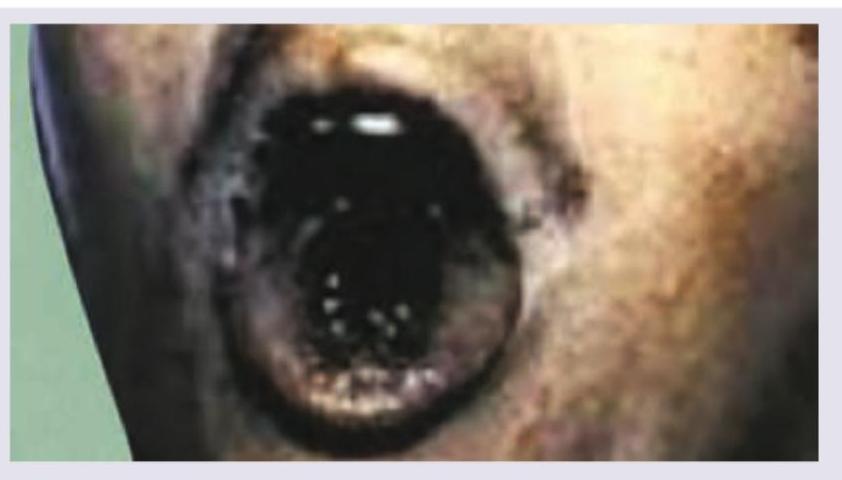
Which is the best method to secure airway and administer oxygen in case of burns shown below?
A 60-year-old male smoker presents with discoloration of urine and has brought a sample to your clinic. He denies any pain or discomfort while passing urine. No history of fever is present. IVU of the patient is shown. Which is the next best investigation to be done?
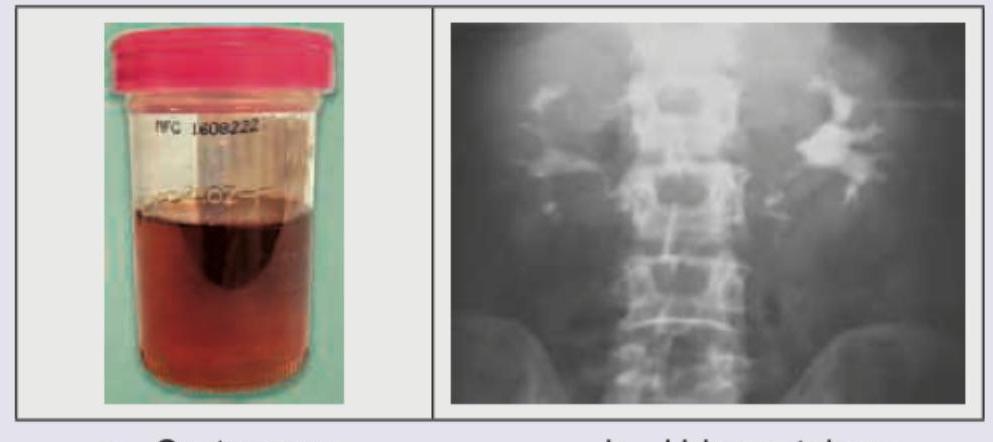
A 70-year-old man underwent the procedure shown below. 3rd day he develops seizures. What is the diagnosis?
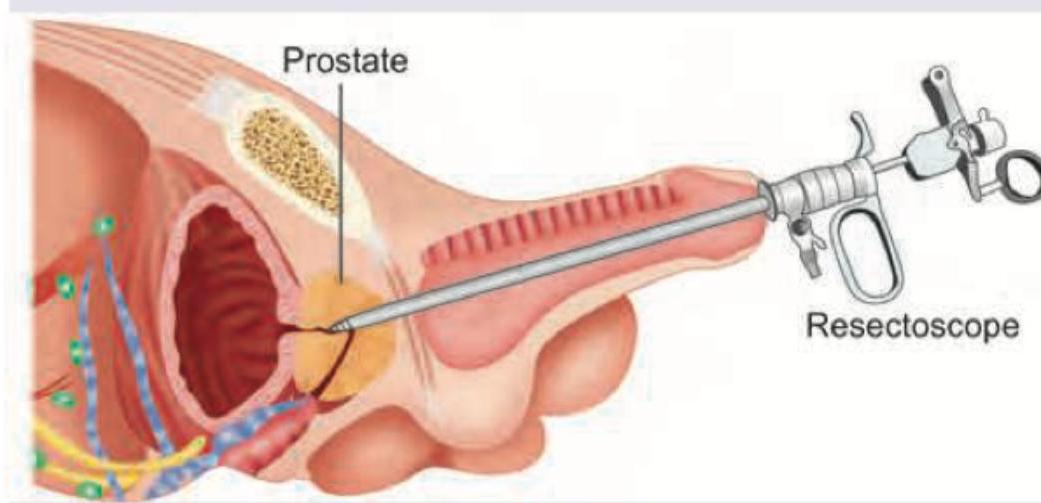
Which of the following is not an indication for surgery in the condition shown below?
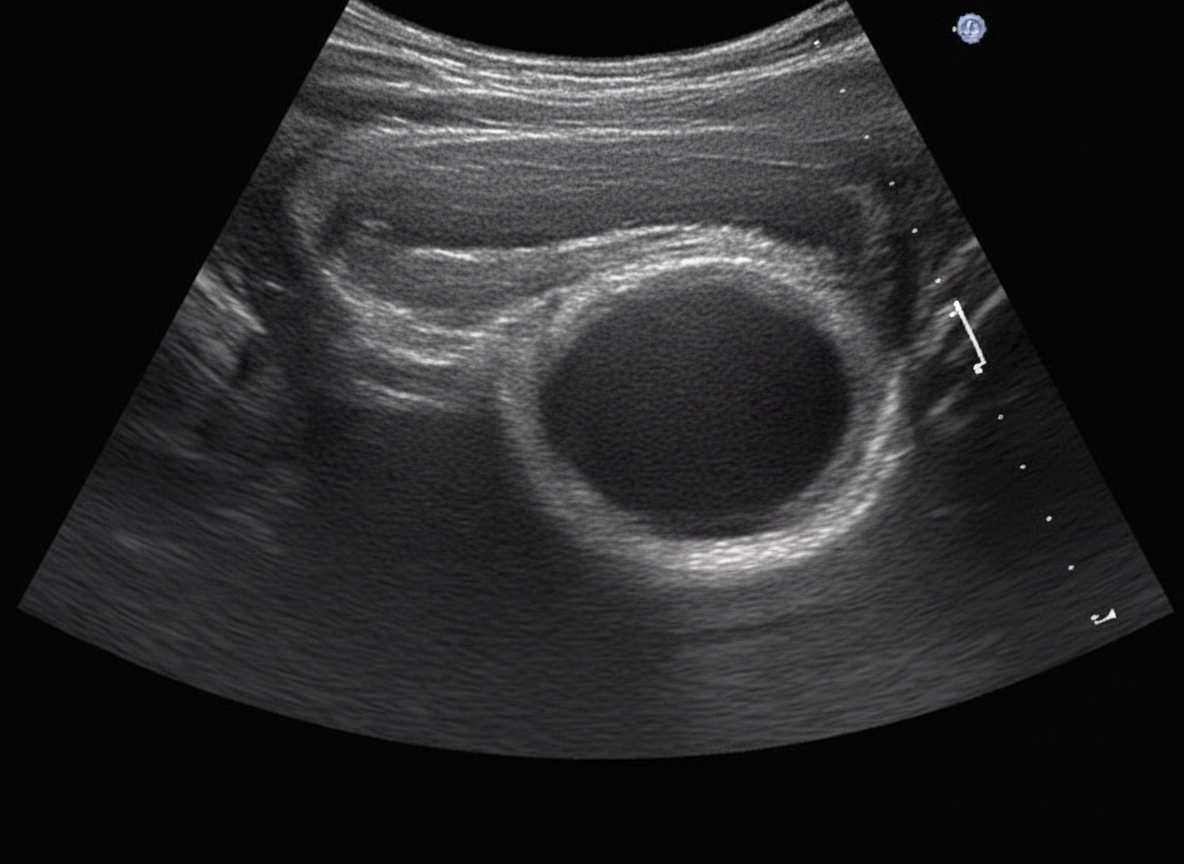
Which of the following uroflowmetry recording indicates BPH?
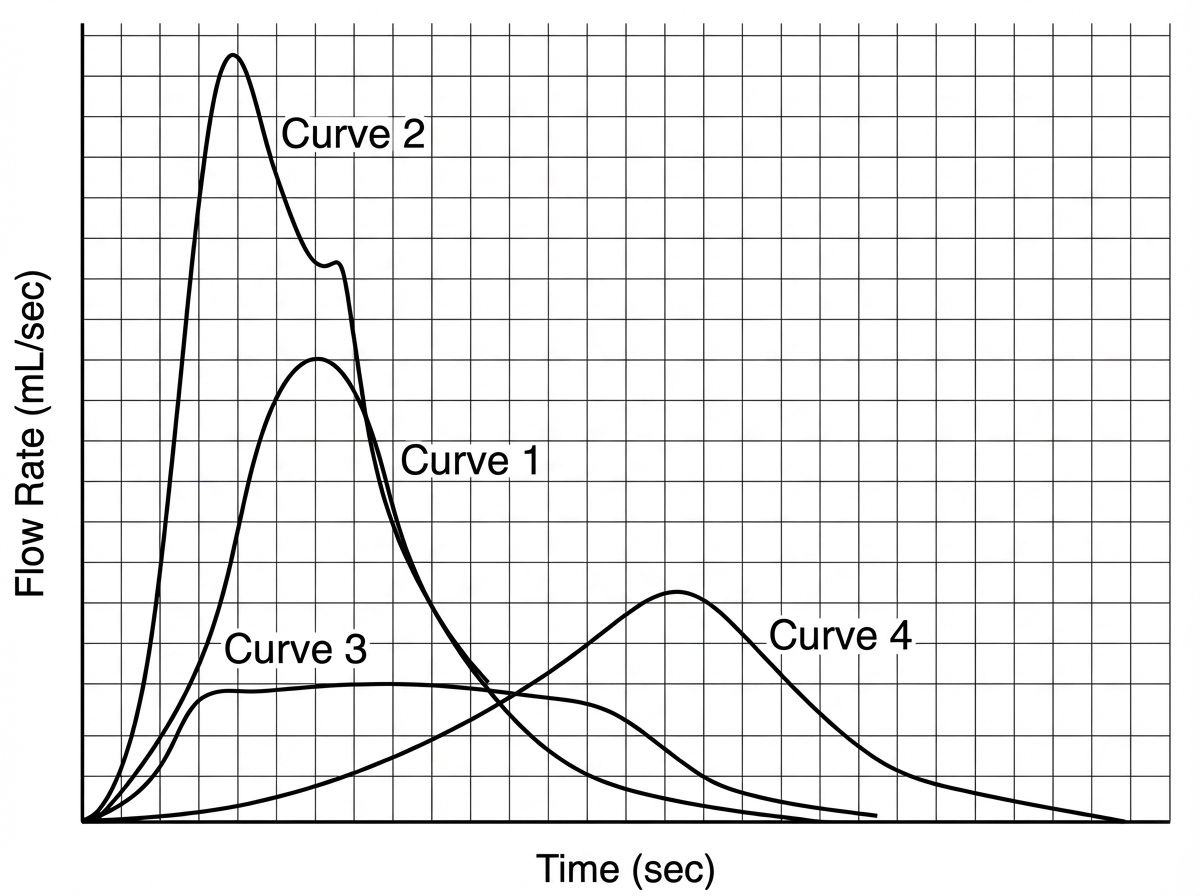
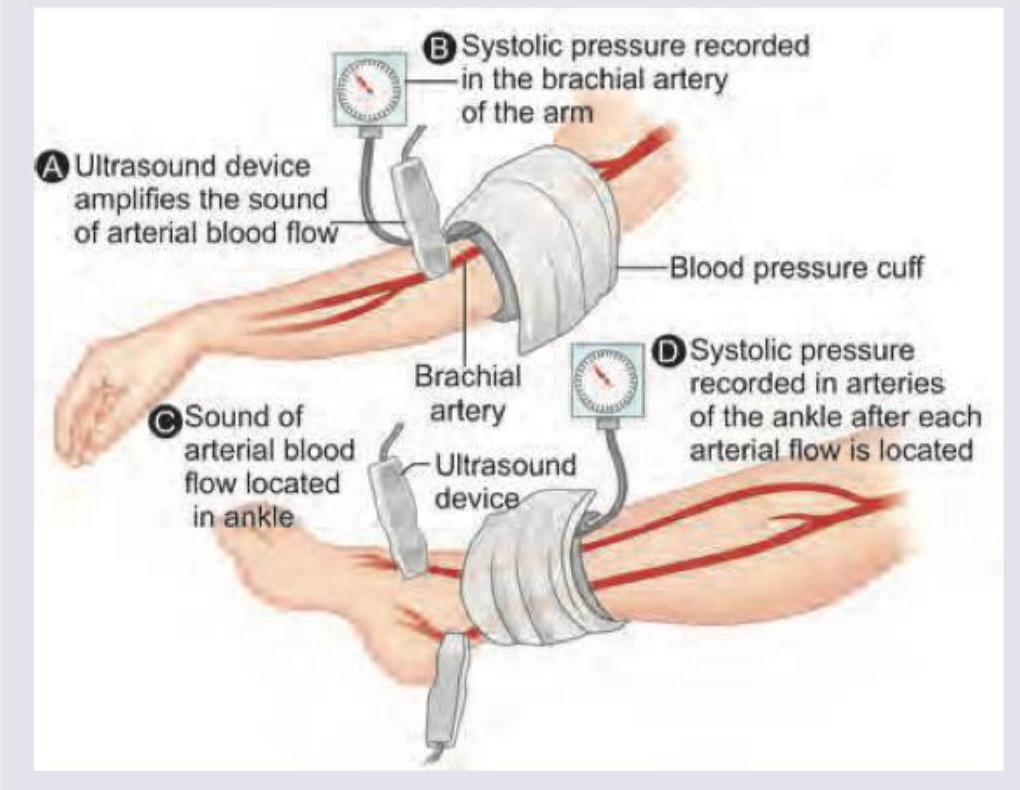
The following test was performed on the patient. Which is correct about the patient?
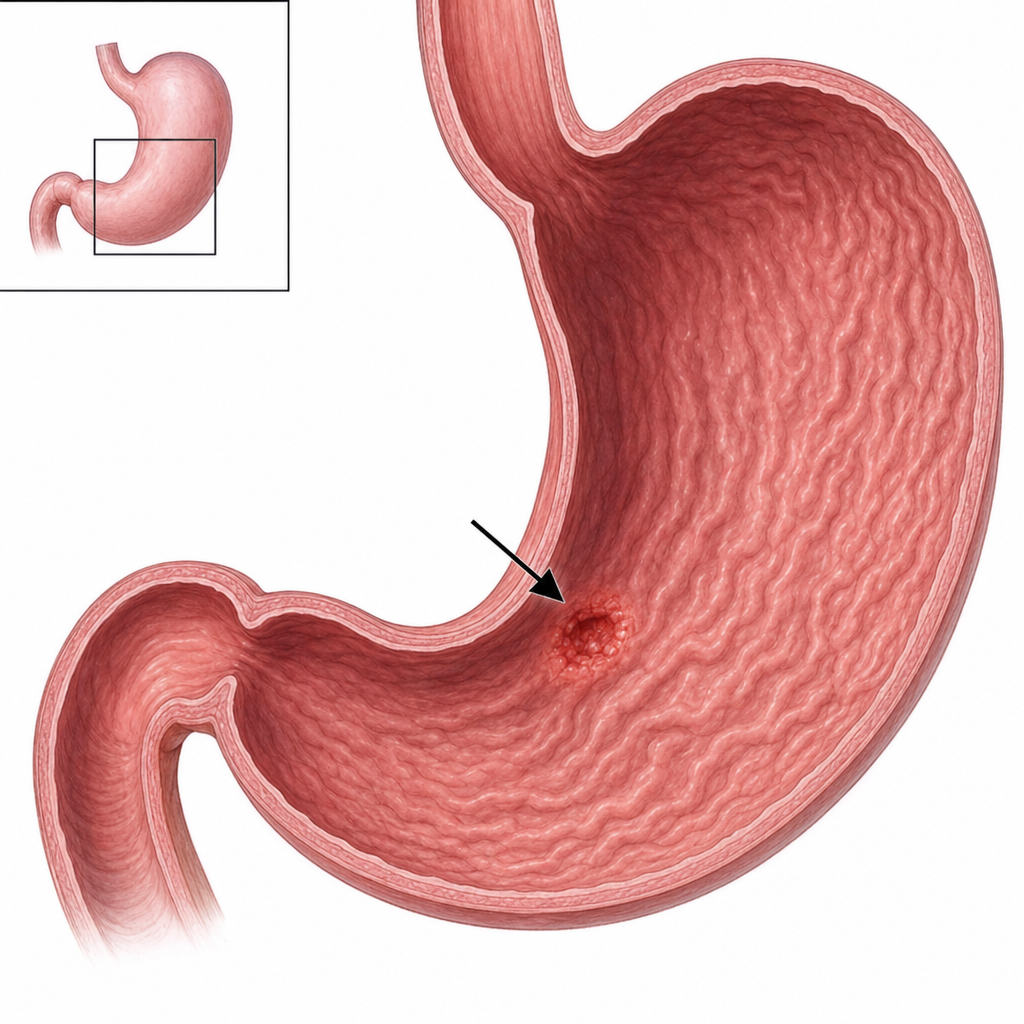
Which subtype of gastric ulcer is shown in the image?
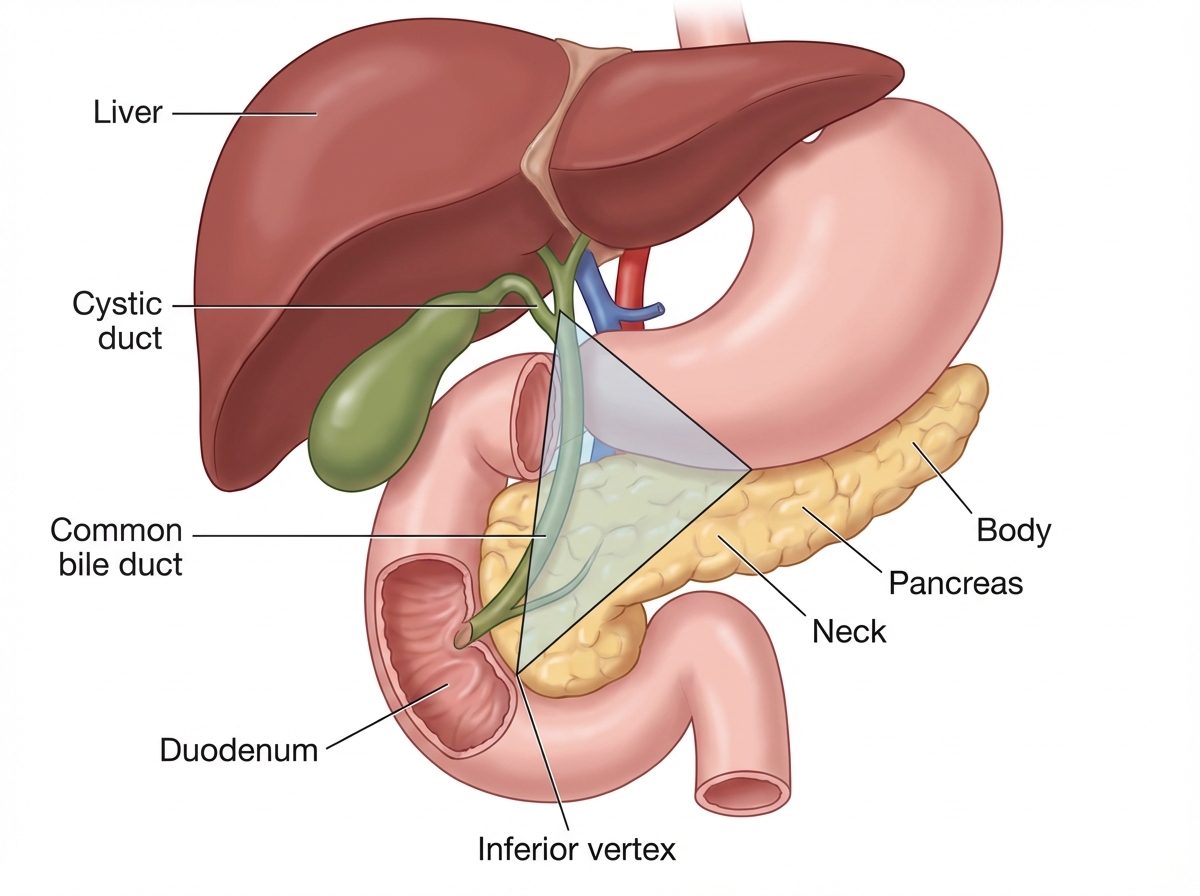
Which is correct about tumor found in the triangle location shown below?