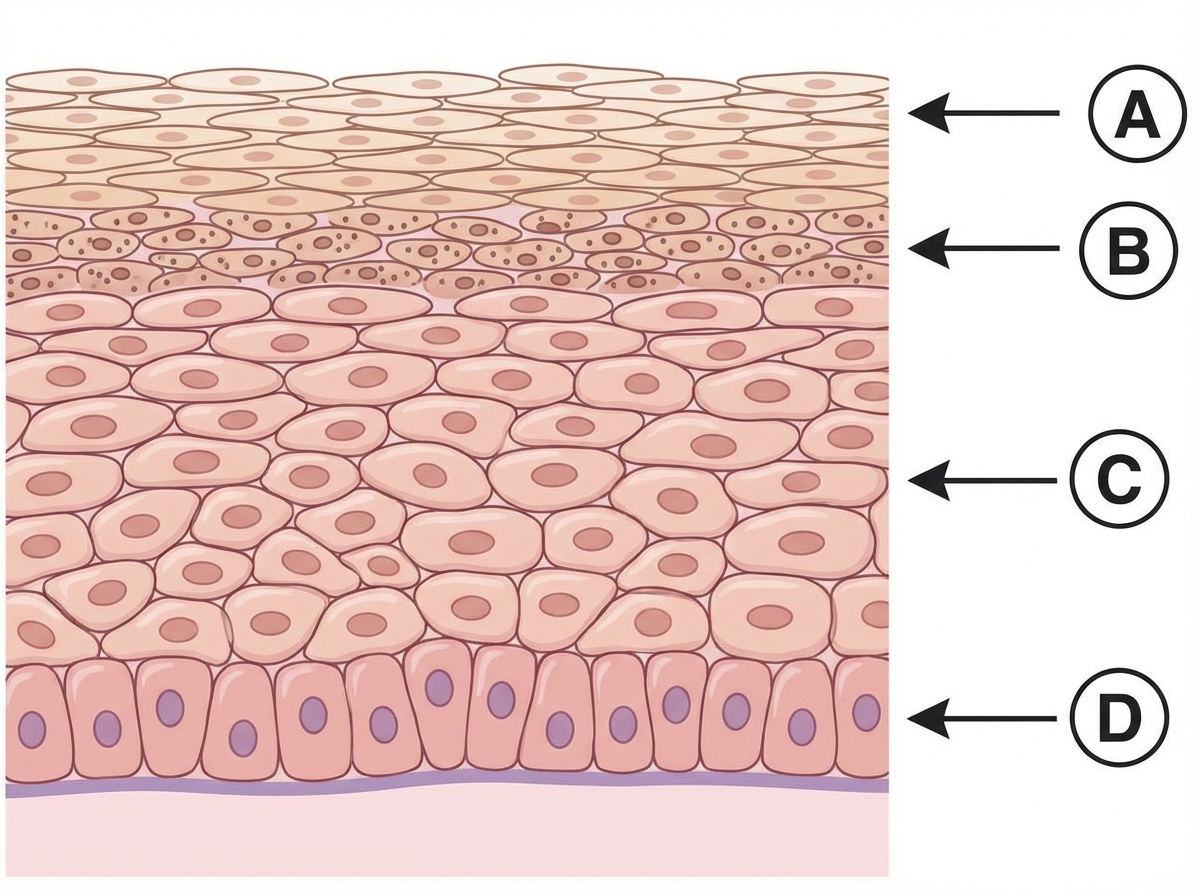
Which of the following layers contains Odland bodies?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Which of the following layers contains Odland bodies?

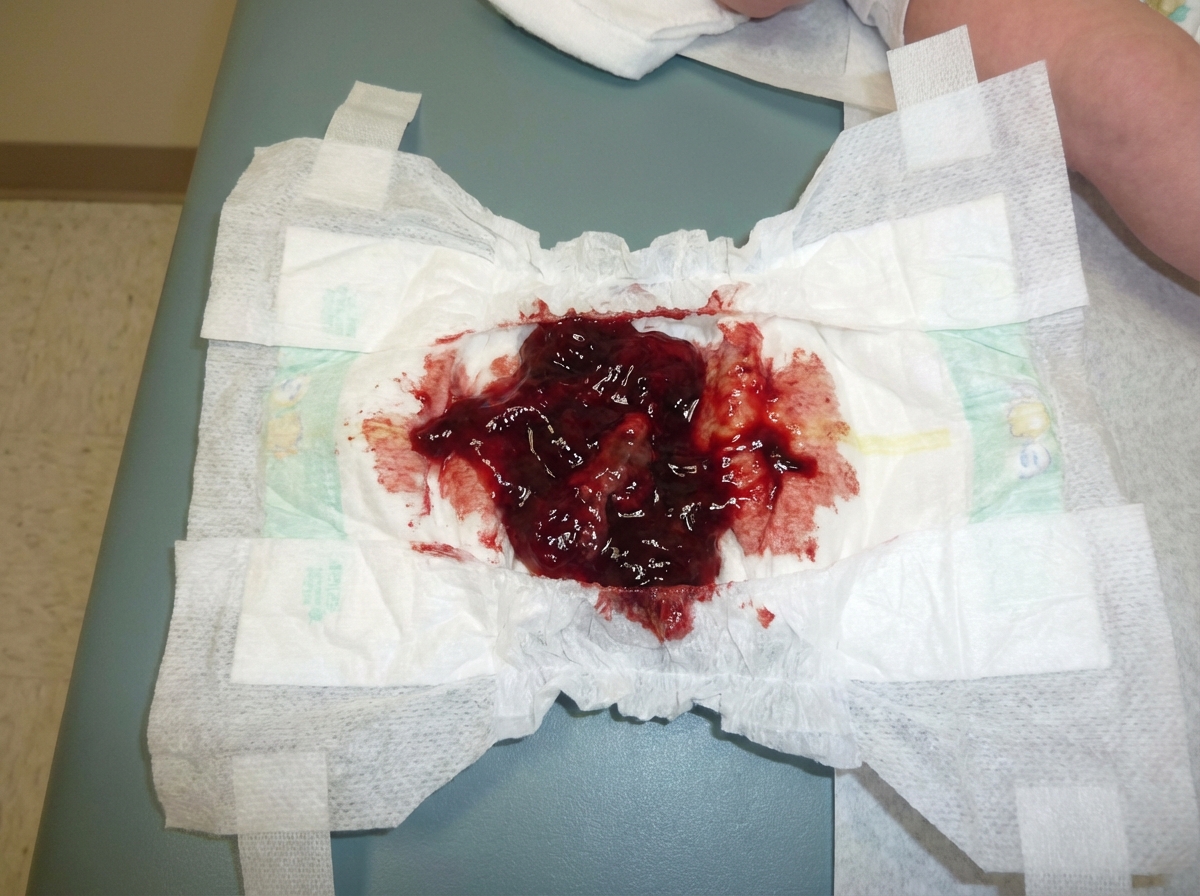
This condition shown below is dependent on development of pH of urine. Which of the following subtype development is insensitive to pH of urine?
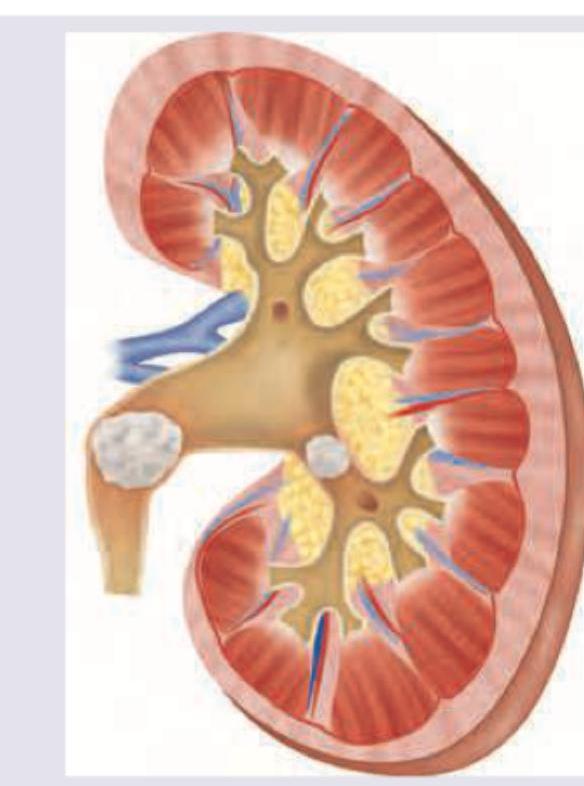
All are correct about the condition shown in the image except: (NEET Pattern 2018)
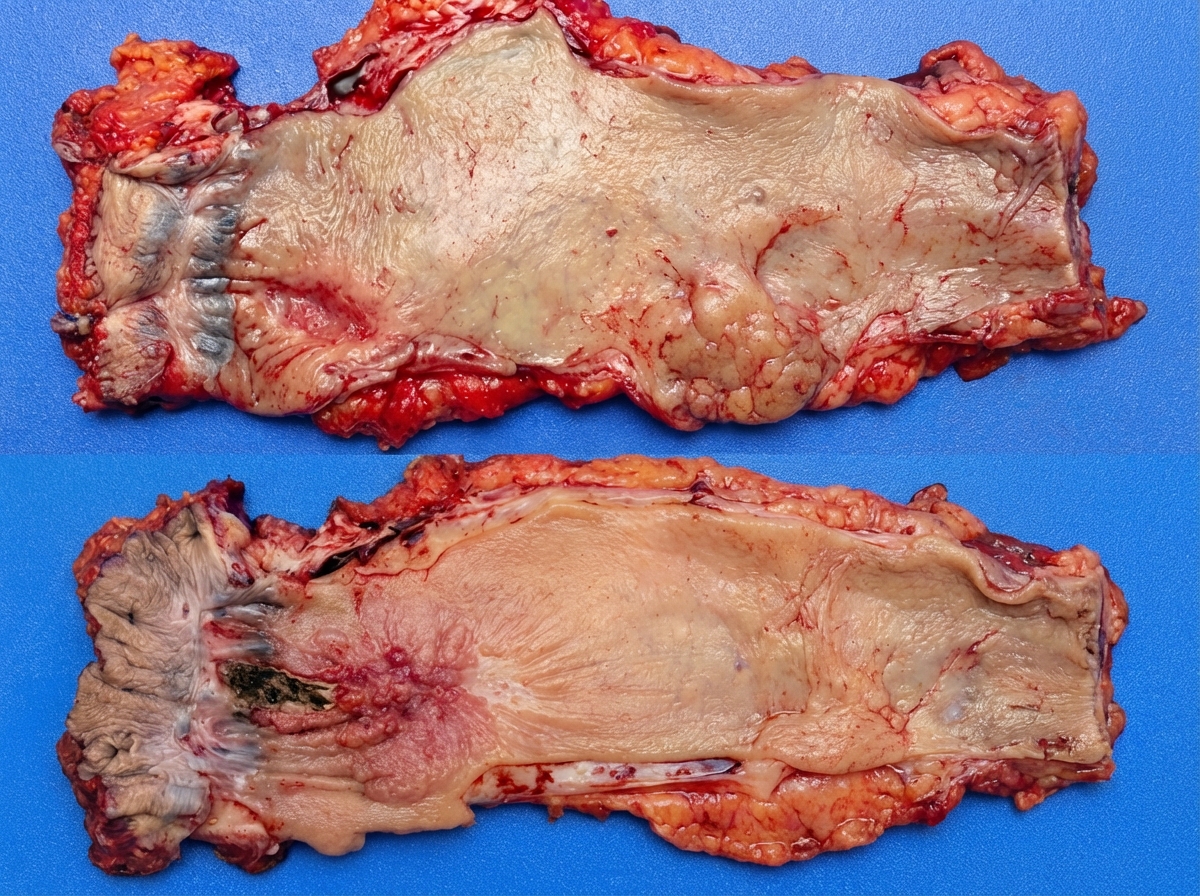
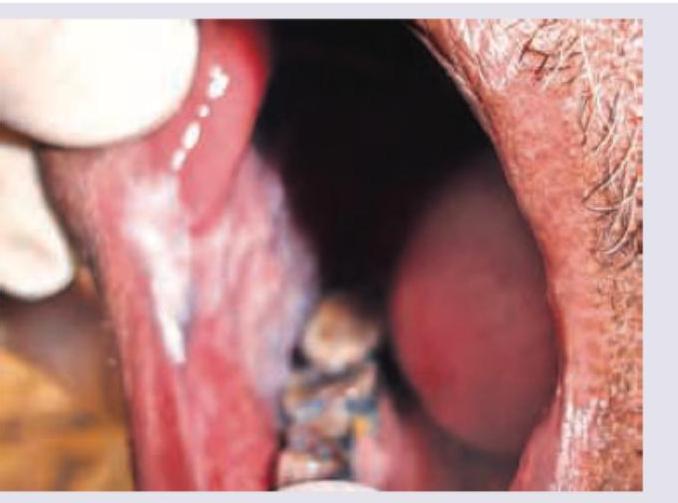
A 60-year-old man with tobacco chewing history presents with trismus and ankyloglossia. The lesion is shown below. Diagnosis is? (NEET Pattern 2018)
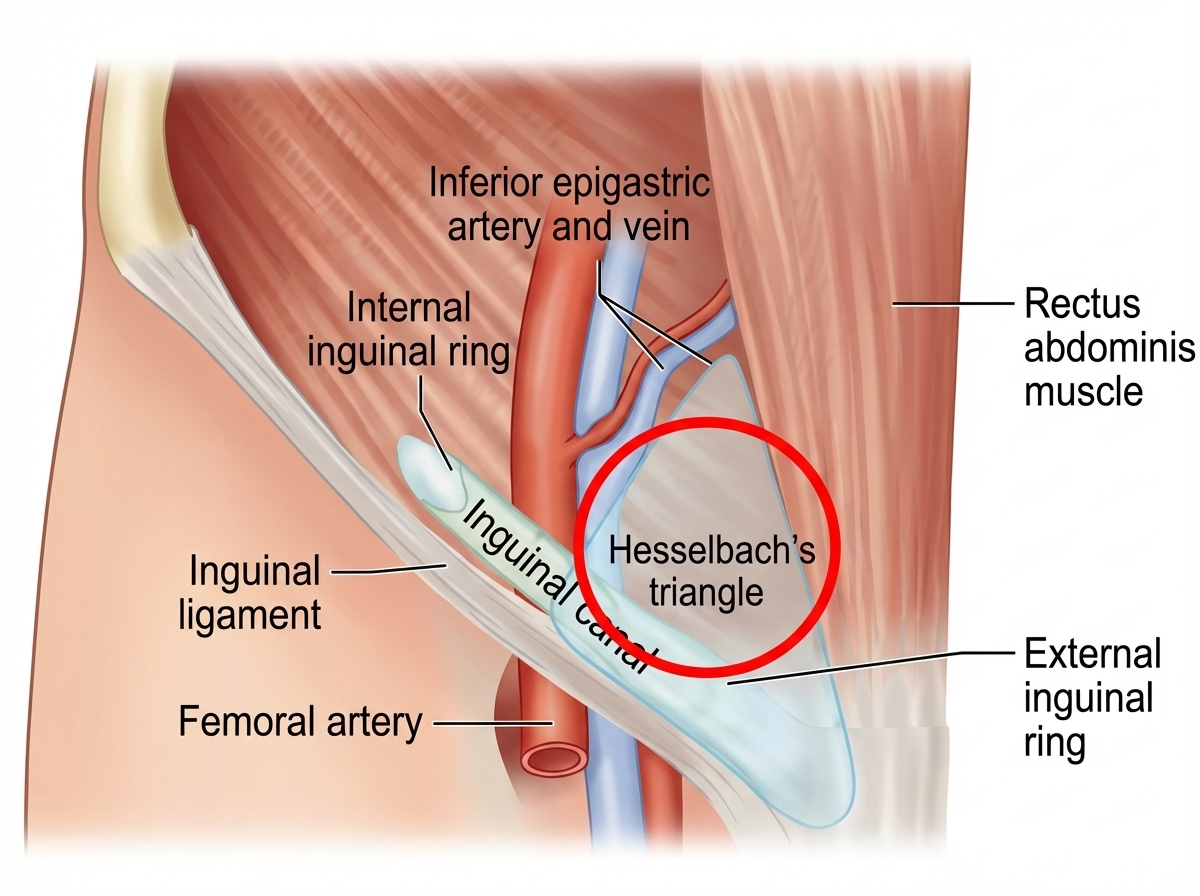
The patient has developed a hernia at the site highlighted by red circle. What is this hernia called as per NYHUS classification? (NEET Pattern 2018)
A person could not pass urine after a fall shown below. On examination vitals are stable but bladder is palpable. What is the probable diagnosis? (NEET Pattern 2018)

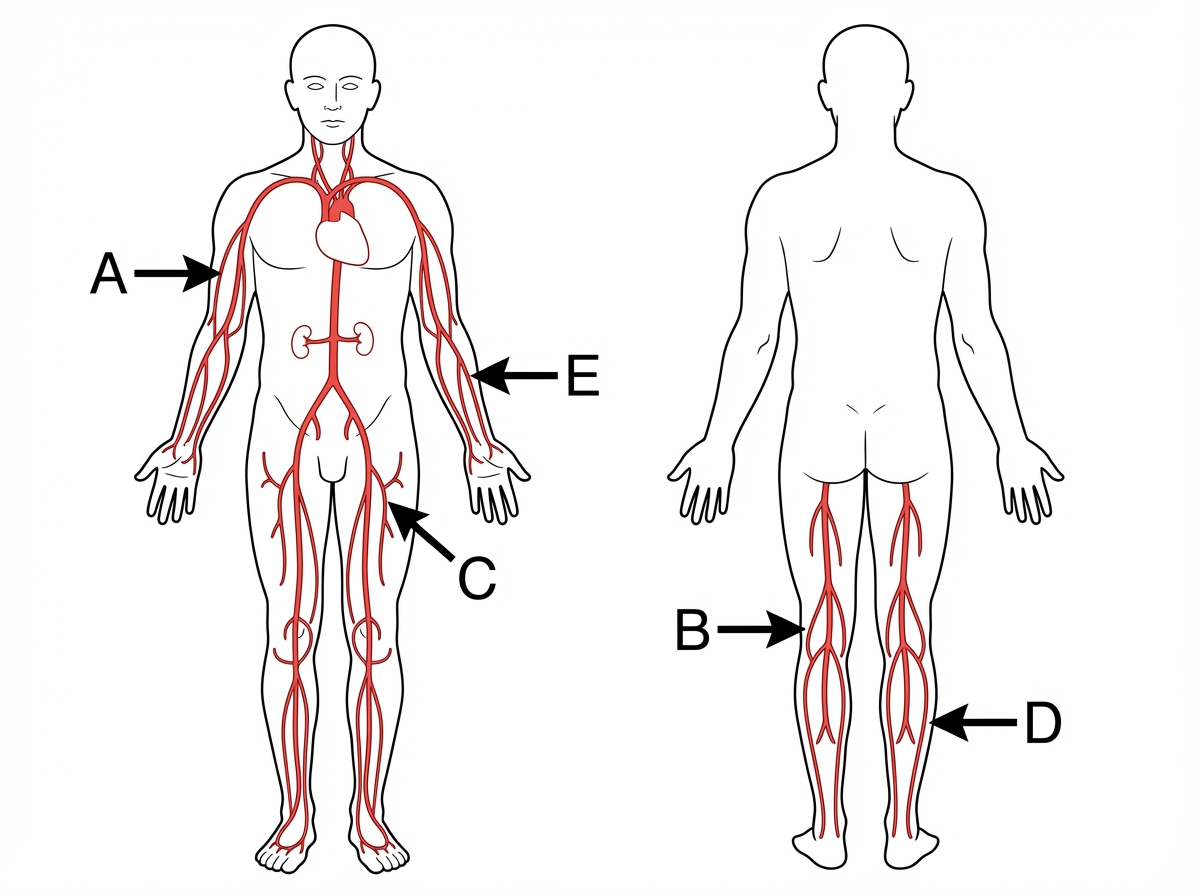
Which is the most common site of peripheral aneurysm?
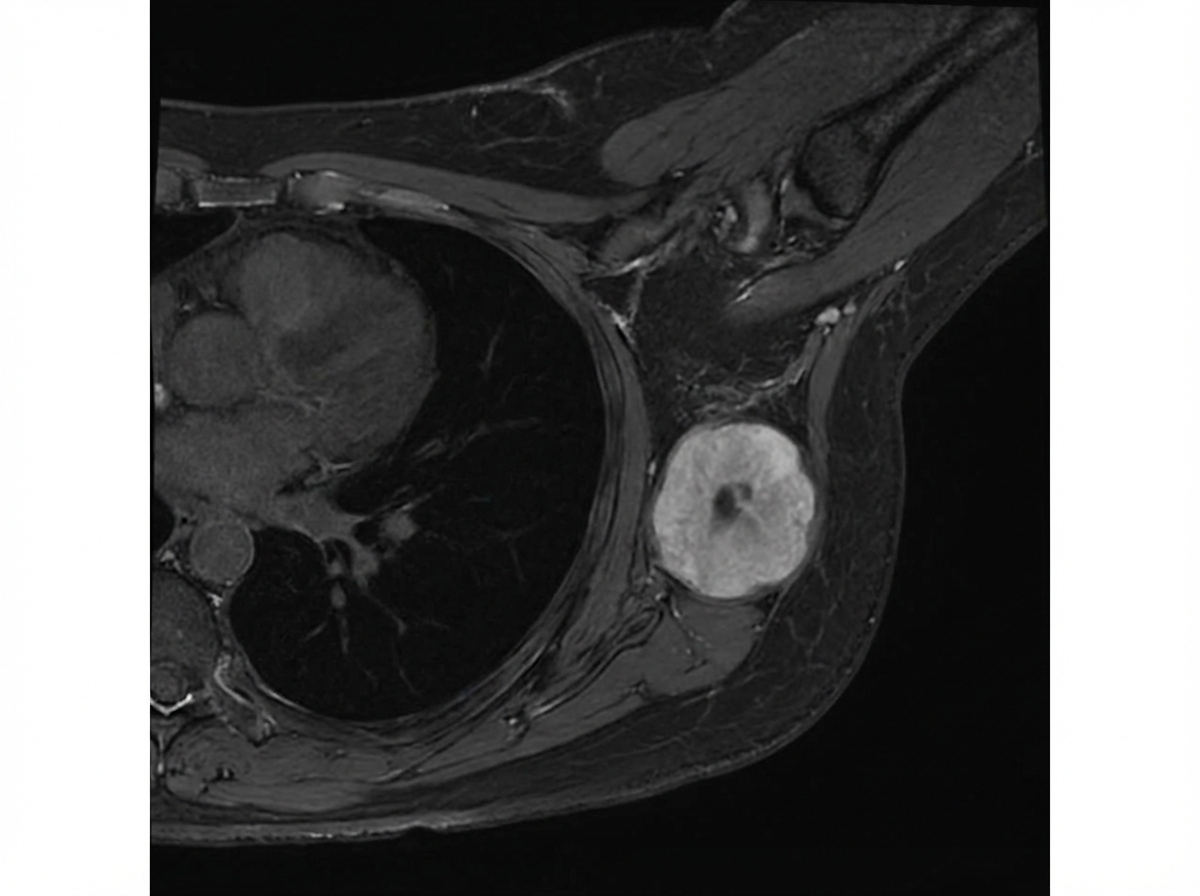
In the MRI breast shown below, 4 cm mass is present with no nodal metastasis. Which is the stage of breast cancer?
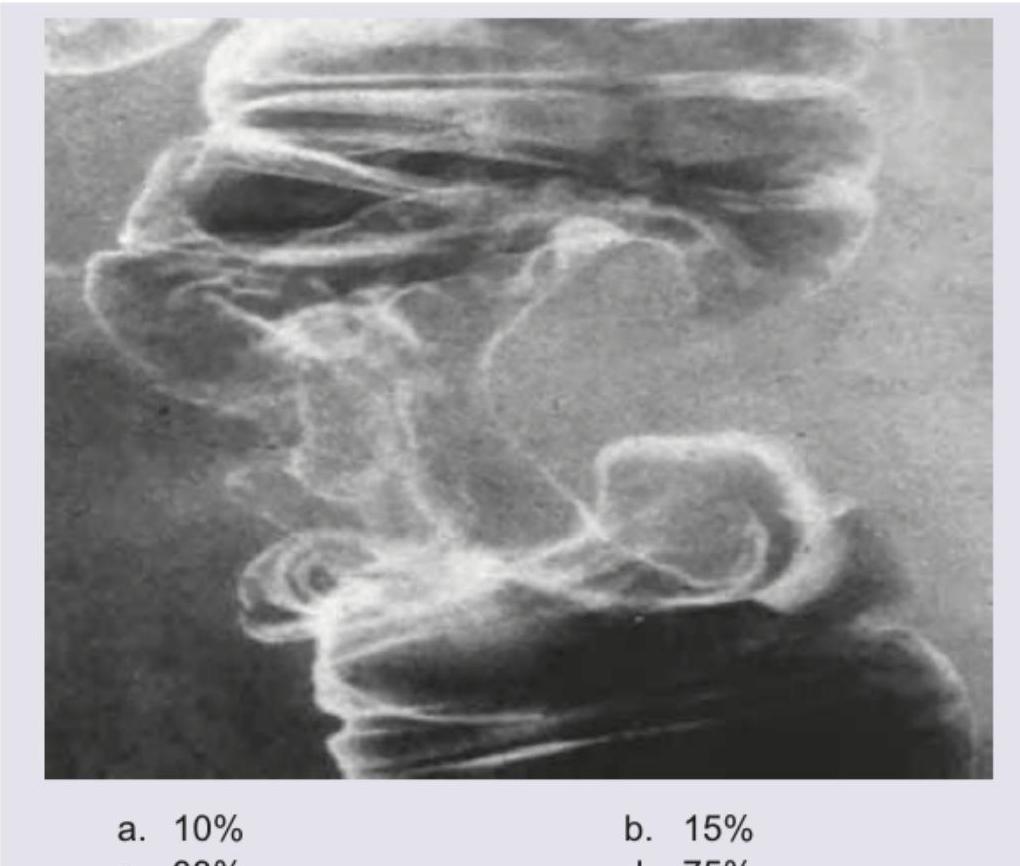
A 35-year-old patient with history of significant weight loss and medically refractory constipation underwent a barium enema shown below. In how many % of cases Metastatic liver disease is found?
A 9-month-old child presents with excessive cry and presentation shown below. On examination right iliac fossa sausage shaped lump is felt. What is the best treatment?