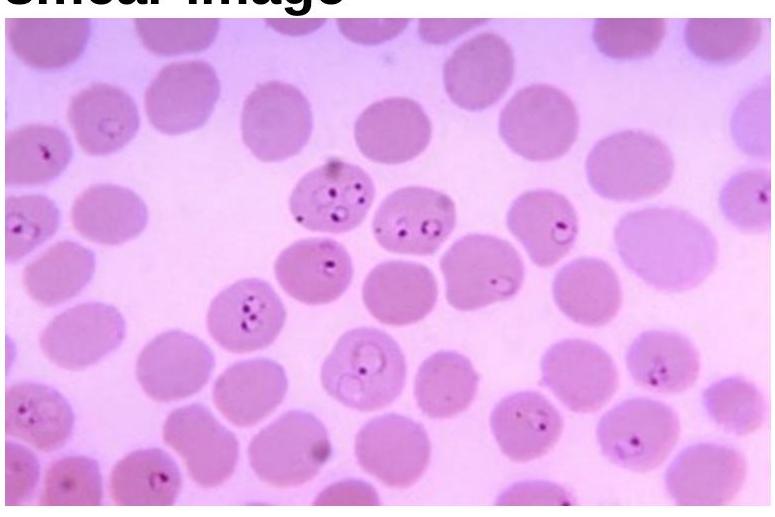
Identify the organism related to the blood smear image.
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Ureteric bud develops from:
Which of the following is an example of an X-linked disorder?
According to WHO classification, severe thinness is defined as a BMI below which value?
Identify the organism related to the blood smear image.

Which of the following is not a high-risk pregnancy?
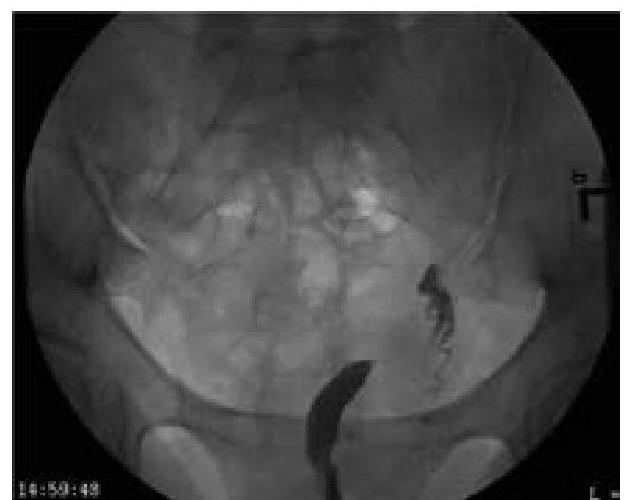
What type of uterine anomaly is shown in this X-ray HSG image?
Which of the following methods is known as a fimbriectomy procedure?
Which gene is primarily associated with Cowden syndrome?
In which type of Hodgkin's lymphoma are classical Reed-Sternberg cells most characteristically observed?
Which of the following is a key distinguishing feature of delirium compared to dementia?