Which one of the following is implicated in the etiology of these adhesions around the liver?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Which one of the following is implicated in the etiology of these adhesions around the liver?

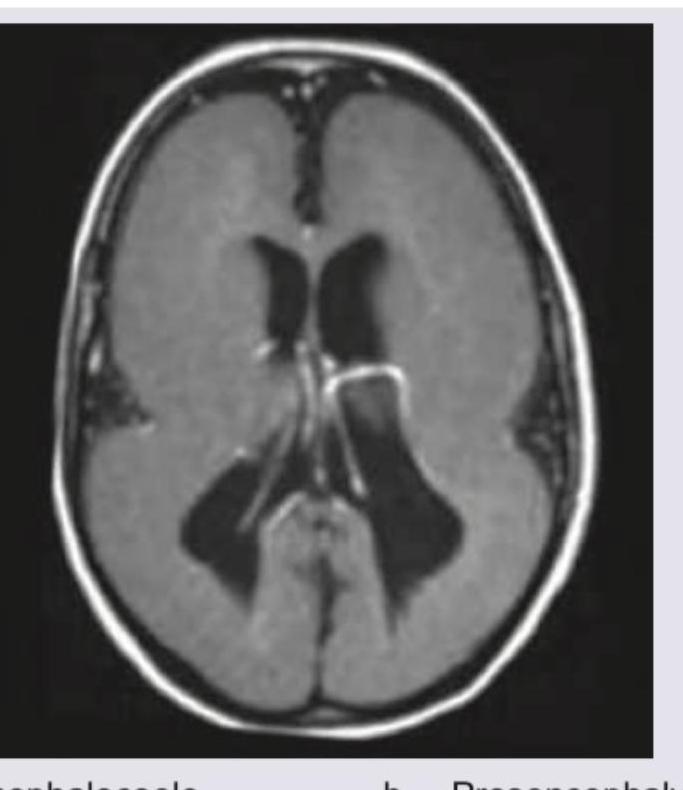
Which of the following will be the most probable diagnostic finding in the patient with X-Ray skull shown below?

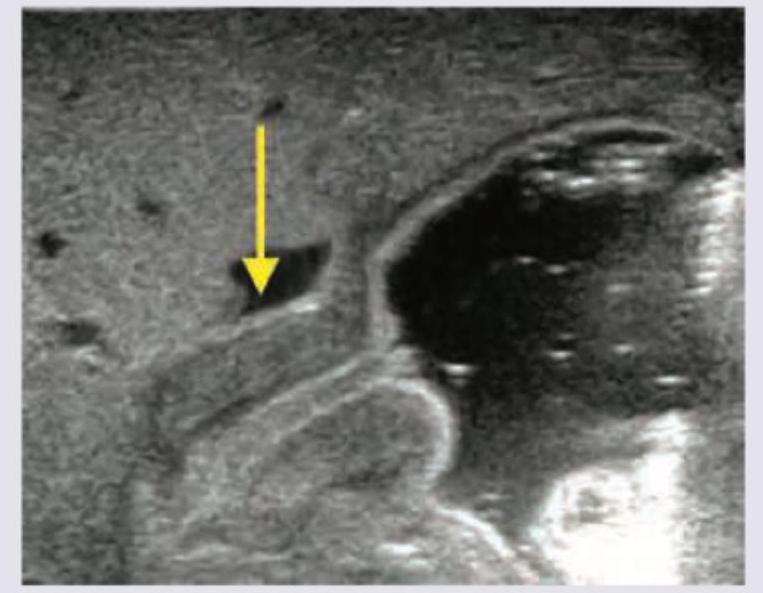
Neonate is brought at 3 weeks of age, with projectile vomiting. USG was performed and is shown below. When can the abdominal mass in this condition be best palpated?
A 1-year-old child with severe acute malnutrition develops pneumonia which is not responding to treatment. Chest X-ray picture is given. What is the likely etiology?
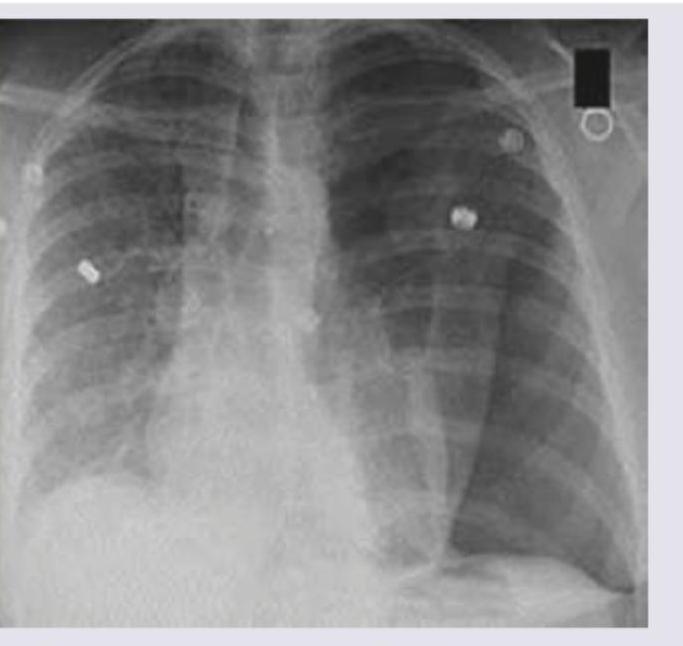
A 12-month-old child who was previously well presented with low grade fever and respiratory distress and on examination there is bilateral wheeze. There is a history of URI in elder sibling. What is the diagnosis?
Identify this condition?
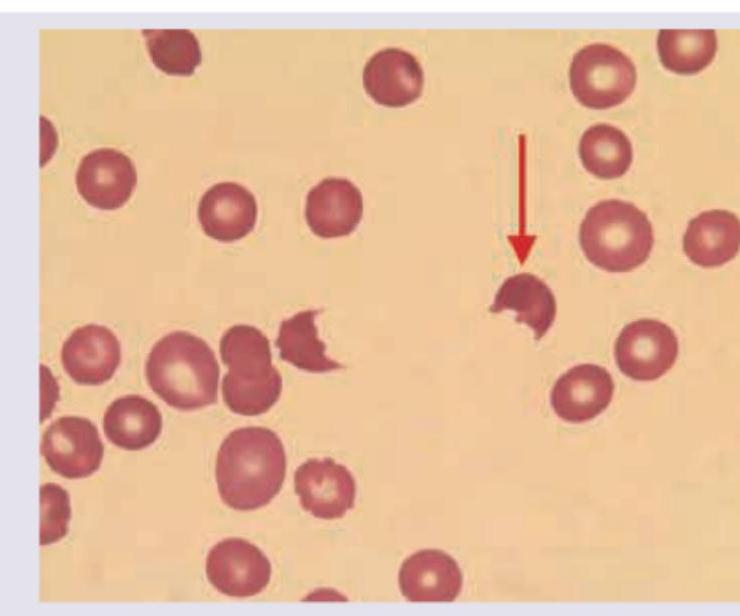
A child with history of diarrhea 1 week back presents with sudden onset pallor and oliguria. Peripheral smear findings are shown below. Which of the following is unlikely finding in this disorder?
The following Skull X-ray is seen in:

The following barium swallow study shows which of the following?
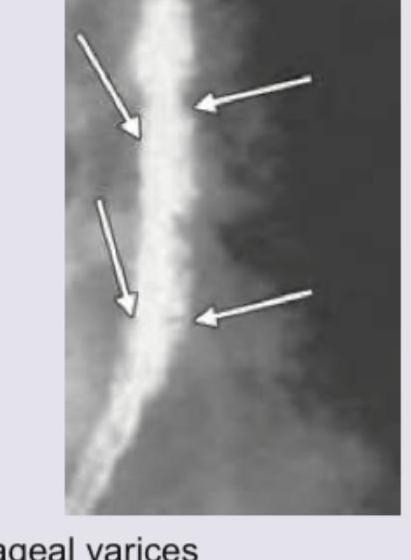
Identify the following abnormality?