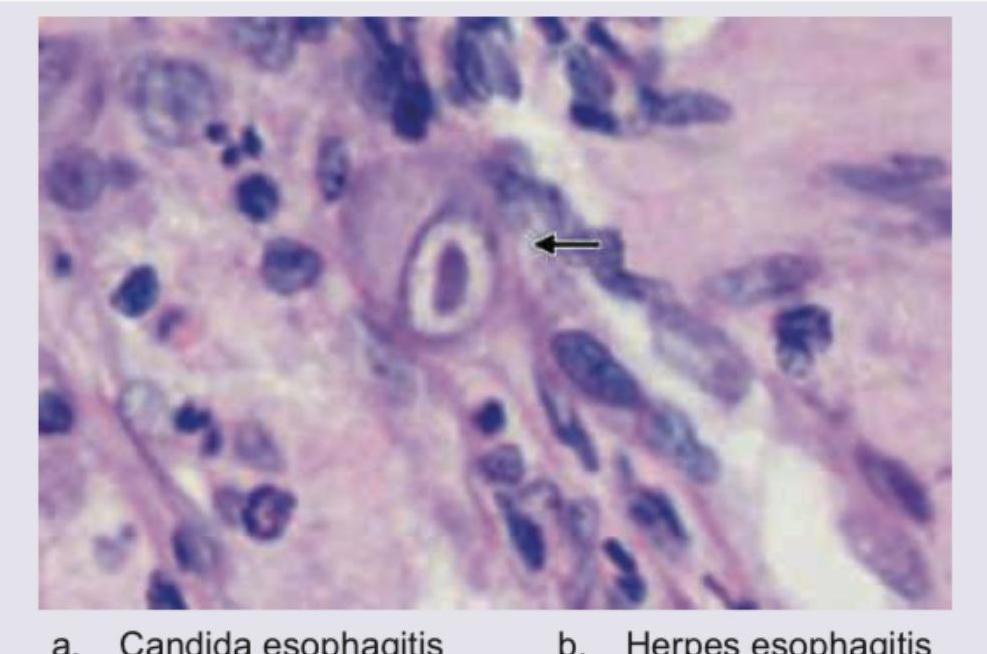
A 40-year-old immunocompromised patient presents with complaints of dysphagia. UGI endoscopy shows multiple ulcers in distal esophagus. Biopsy was performed and histopathology is shown below. Diagnosis is:
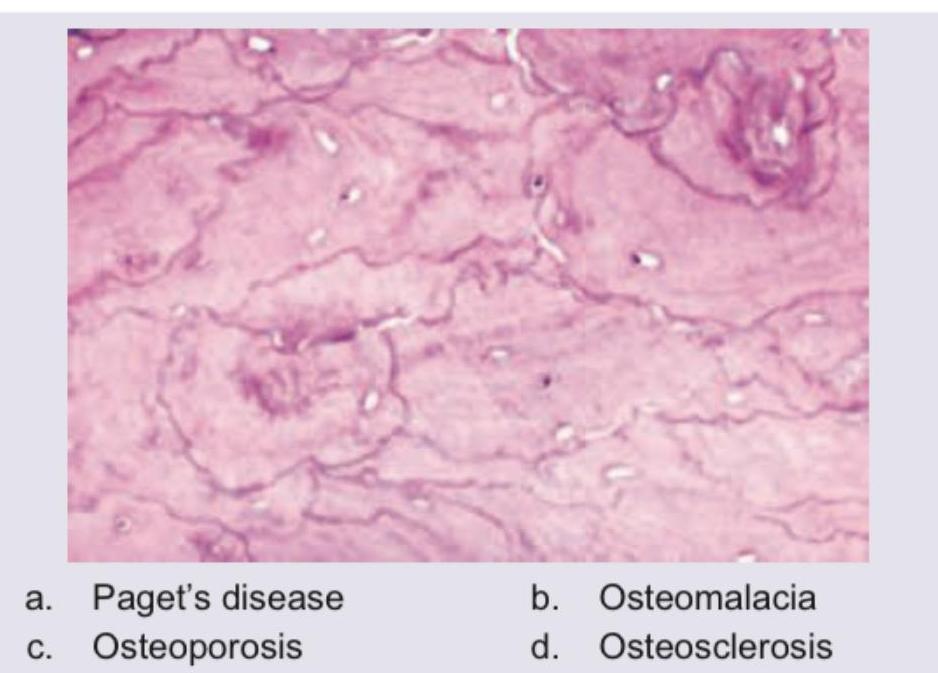
Bone biopsy specimen is shown below. Diagnosis is: