All (353)Anatomy (24)Anesthesiology (4)Biochemistry (1)Biochemistry (26)Community Medicine (12)Dental (1)Dermatology (8)ENT (1)Forensic Medicine (2)General Medicine (7)Internal Medicine (41)Microbiology (22)Obstetrics and Gynecology (23)Ophthalmology (2)Orthopaedics (1)Pathology (3)Pathology (31)Pediatrics (24)Pharmacology (27)Physiology (13)Psychiatry (3)Psychiatry (10)Radiology (30)Surgery (5)Surgery (32)
Q11
Acute Hemorrhagic Conjunctivitis is primarily caused by which type of Enterovirus?
Q12
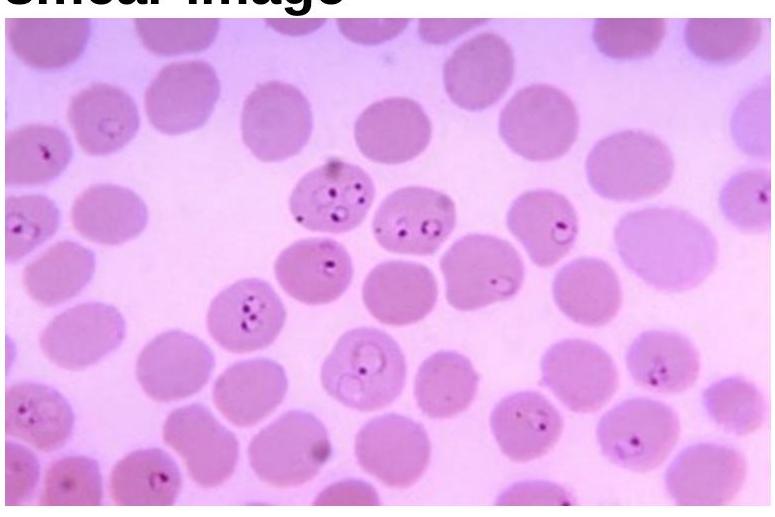
Identify the organism related to the blood smear image.