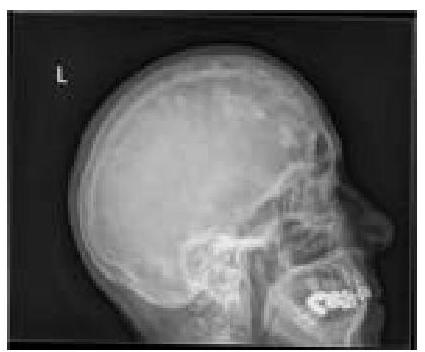
What type of lesions in the skull calvarium can be identified on this X-ray?
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Hard palate contains:
What is a potential cause of cardiogenic shock other than myocardial infarction (MI)?
Urea breath test is used for diagnosis of:
In Rheumatoid arthritis, which type of cells are prominently present ?
Anaerobes are resistant intrinsically against which of the following?
What is the current preferred term for the condition previously known as mental retardation?
What type of lesions in the skull calvarium can be identified on this X-ray?

Which of the following statements about the management of haematomas is NOT correct?
What is the most common indication for performing a tracheostomy?
Which is the best investigation for carcinoma of the head of pancreas?