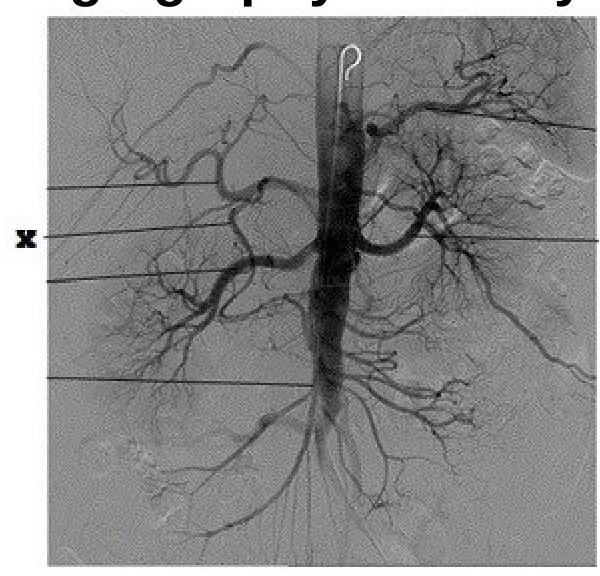
Identify the artery labeled as 'X' in the provided angiography anatomy image.
Enter your email to get your 85% OFF code and unlock the full NEET PG question bank on the app.
Identify the artery labeled as 'X' in the provided angiography anatomy image.

Modified Mallampati grading is used in assessment of -
Murphy's eye is seen in -
Galactosemia is due to deficiency of which enzyme?
Which drug regimen is given to a pregnant woman with HIV infection?
What is the most common symptom treated with hormone therapy (HT) in menopausal women?
A 1-year-old child weighing 6 kg is suffering from acute gastroenteritis with signs of sunken eyes and skin pinch returning to normal very rapidly. What will be your management?
What is mechanism of action of colchicine in acute gout?
Tadalafil should not be given with:
Where will be the placement location for Auditory Brainstem Implant?