Which of these steps is followed first for the management of shoulder dystocia after McRoberts maneuver?
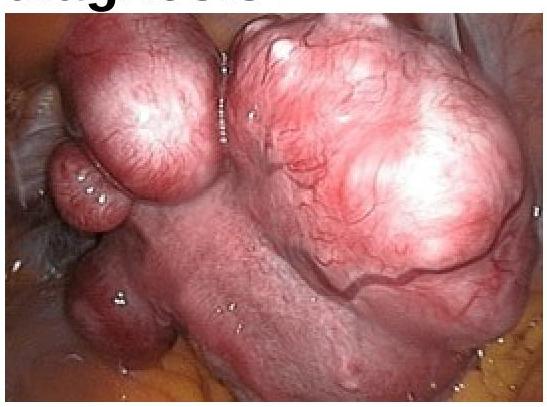
In a woman complaining of AUB following image was seen in endoscopic examination of uterus. What will be the diagnosis?
Which drug regimen is given to a pregnant woman with HIV infection?
Which of the following statements about the placenta is correct?
What is the most common symptom treated with hormone therapy (HT) in menopausal women?
Based on the provided image, which of the following is the correct diagnosis?
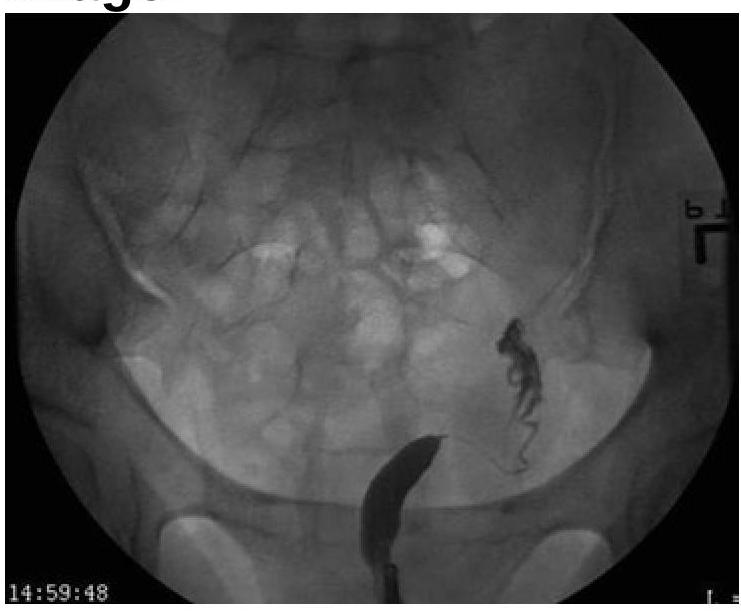
Which of the following is the most common cause of perforation of uterus in non-pregnant state?
A 16-year-old girl comes to you with primary amenorrhea; on evaluation there is absent breast development, she has a normal stature, her FSH and LH levels are found to be high and she has a karyotype of 46XX. What is the probable diagnosis?
Shoulder dystocia is managed by all of the following except:-
In Peripartum cardiomyopathy, cardiac failure occurs at:-