NEET-PG 2018 — Obstetrics and Gynecology
23 Previous Year Questions with Answers & Explanations
What is the first-line maneuver for management of shoulder dystocia?
What type of uterine anomaly is shown in this X-ray HSG image?
Extramammary Paget's disease of the vulva is most commonly associated with which other cancer?
What are the effects of Progesterone-only pills?
Which of the following is not a high-risk pregnancy?
Which of the following methods is known as a fimbriectomy procedure?
What is meant by Superfecundation?
Best time to perform the quadruple test is:
Long-standing pelvic inflammatory disease (PID) may lead to which of the following complications?
Dilatation & curettage (D&C) is contraindicated in-
NEET-PG 2018 - Obstetrics and Gynecology NEET-PG Practice Questions and MCQs
Question 1: What is the first-line maneuver for management of shoulder dystocia?
- A. 90 degree rotation of posterior shoulder
- B. Emergency c-section
- C. Supra pubic pressure
- D. Sharp flexion of hip joints towards abdomen (Correct Answer)
Explanation: ***Sharp flexion of hip joints towards abdomen*** - This maneuver, known as the **McRoberts maneuver**, widens the anterior-posterior diameter of the **pelvis** and flattens the sacrum. - It increases the likelihood of dislodging the impacted fetal shoulder from behind the symphysis pubis. *Supra pubic pressure* - **Suprapubic pressure** is applied to the fetal anterior shoulder to dislodge it from the symphysis pubis and guide it under the maternal pubic bone. - This maneuver is typically performed *in conjunction with* the McRoberts maneuver, but the question specifies "sharp flexion of hip joints towards abdomen," which is McRoberts alone. *90 degree rotation of posterior shoulder* - This describes the **Woods screw maneuver**, which involves rotating the posterior shoulder to facilitate delivery. It is a secondary maneuver used if McRoberts and suprapubic pressure are insufficient. - The question asks for the primary management step, and the McRoberts maneuver (sharp flexion) is usually the first line of intervention. *Emergency c-section* - An **emergency C-section** is generally not indicated for the acute management of shoulder dystocia once the head has delivered, as it is a **delivery complication** happening during vaginal birth. - Management focuses on specific maneuvers to release the impacted shoulders through the vagina.
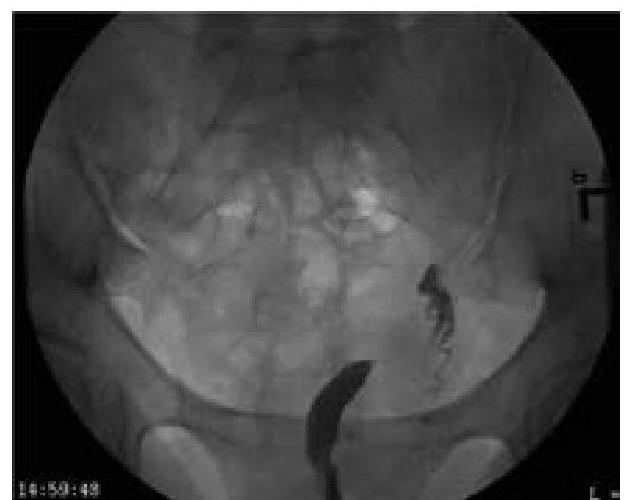
Question 2: What type of uterine anomaly is shown in this X-ray HSG image?
- A. Septate uterus
- B. Uterus didelphys
- C. Unicornuate uterus (Correct Answer)
- D. Bicornuate uterus
Explanation: ***Unicornuate uterus*** - The image shows a single, elongated uterine horn with a single fallopian tube arising from it, consistent with a **unicornuate uterus**. - This congenital anomaly results from the **failure of one Müllerian duct to develop**, leading to an abnormally shaped uterus. *Septate uterus* - A **septate uterus** would show a normal uterine fundus with an internal septum dividing the uterine cavity. - This image clearly depicts only **one rudimentary horn** and no visible septum. *Uterus didelphys* - **Uterus didelphys** involves two completely separate uteri, each with its own cervix and vagina. - The image does not show evidence of a **second, separate uterine structure**. *Bicornuate uterus* - A **bicornuate uterus** is characterized by two distinct uterine horns, which fuse at the cervix or lower uterine segment, creating a heart-shaped appearance of the fundus. - The image shows a **single, long horn** rather than two distinct horns.
Question 3: Extramammary Paget's disease of the vulva is most commonly associated with which other cancer?
- A. Vulvar cancer (Correct Answer)
- B. Vaginal cancer
- C. Cervical cancer
- D. Uterine cancer
Explanation: ***Vulvar cancer*** - **Extramammary Paget's disease (EMPD)** frequently presents in the vulvar region and is associated with an underlying **adenocarcinoma** in up to 30% of cases. - The disease involves intraepithelial adenocarcinoma cells that can spread locally and, in some instances, indicates a synchronous or metachronous **internal malignancy**, often of genitourinary or gastrointestinal origin, but primarily vulvar adenocarcinoma in this context. *Vaginal cancer* - While Paget's disease can occur in other anogenital areas, its association with **primary vaginal cancer** is much less common compared to vulvar involvement. - **Vaginal Paget's disease** is rare and usually represents secondary spread from a vulvar primary or an underlying bladder/urethral carcinoma. *Cervical cancer* - **Paget's disease** is not typically associated with **cervical cancer**. Cervical cancers are predominantly squamous cell carcinomas or adenocarcinomas arising from the transformation zone. - While cervical adenocarcinoma can present with similar cells to Paget's, it is a distinct entity and not a common association. *Uterine cancer* - **Uterine cancer**, primarily endometrial carcinoma, has no direct or common association with **Paget's disease**. - Paget's disease primarily affects the skin and can be associated with underlying gland cancers, but these are generally in proximity to the epidermal involvement rather than distant uterine sites.
Question 4: What are the effects of Progesterone-only pills?
- A. All of the options may occur (Correct Answer)
- B. May suppress ovulation
- C. Thins the lining of the uterus
- D. Thickens cervical mucus
Explanation: ***All of the options may occur*** - Progesterone-only pills (POPs) work through **multiple complementary mechanisms** that collectively provide effective contraception. - All three effects occur simultaneously and contribute to the overall contraceptive efficacy of POPs. - Understanding these mechanisms helps explain why POPs are effective despite lower hormone doses compared to combined oral contraceptives. **Mechanism 1: May suppress ovulation** - POPs can **partially suppress ovulation**, preventing the release of an egg. - Traditional POPs suppress ovulation in approximately 40-60% of cycles, while newer desogestrel-containing POPs achieve higher rates (97-99%). - This effect depends on the dose and type of progestin used in the formulation. **Mechanism 2: Thins the lining of the uterus** - Progesterone causes **endometrial atrophy**, making the uterine lining thin and unsuitable for embryo implantation. - This hostile uterine environment acts as a backup contraceptive mechanism if ovulation and fertilization occur. - Endometrial changes occur consistently with POP use. **Mechanism 3: Thickens cervical mucus** - This is the **primary and most consistent mechanism** of POPs. - Progesterone significantly **increases cervical mucus viscosity** and reduces its quantity within hours of administration. - The thickened mucus creates a physical barrier that prevents sperm penetration, motility, and viability.
Question 5: Which of the following is not a high-risk pregnancy?
- A. Age 25-30 years (Correct Answer)
- B. Diabetes mellitus
- C. Previous history of manual removal of placenta
- D. Anemia
Explanation: ***Age 25-30 years*** - An age of **25-30 years** is generally considered the optimal reproductive age range, and pregnancies within this bracket are typically classified as low-risk based on age alone. - This age range carries the lowest statistical risk for both maternal and fetal complications, assuming no other co-morbidities. *Previous history of manual removal of placenta* - A previous history of manual removal of the placenta indicates a risk factor for **recurrent placental retention** or **morbidly adherent placenta** in future pregnancies, making it a high-risk factor. - This history suggests an increased likelihood of complications such as **postpartum hemorrhage** and can influence the management of subsequent deliveries. *Anemia* - **Anemia** in pregnancy, especially severe iron deficiency anemia, is considered a high-risk factor due to increased maternal and fetal morbidity. - It can lead to complications such as **preterm delivery**, **low birth weight**, and difficulties tolerating blood loss during delivery. *Diabetes mellitus* - **Diabetes mellitus**, whether pre-existing or gestational, makes a pregnancy high-risk due to potential adverse effects on both the mother and the fetus. - Risks include **preeclampsia**, **macrosomia**, **neonatal hypoglycemia**, and **congenital anomalies**.
Question 6: Which of the following methods is known as a fimbriectomy procedure?
- A. Uchida procedure
- B. Irving procedure
- C. Madlener procedure
- D. Kroener procedure (Correct Answer)
Explanation: ***Kroener procedure*** - The **Kroener procedure** is a method of **tubal ligation** particularly known as a **fimbriectomy**, where the fimbriated end of the fallopian tube is removed. - This sterilization technique primarily involves excising the **fimbriae**, preventing **ovum capture** and subsequent fertilization. *Uchida procedure* - The **Uchida procedure** involves **injecting a sclerosing solution** under the serosa of the fallopian tube, then excising a small segment and ligating the ends. - This method aims to **bury the fimbriated end** within the broad ligament, but it is not a fimbriectomy. *Irving procedure* - The **Irving procedure** involves **tying and transecting the fallopian tube**, then burying the severed medial end into the posterior wall of the uterus. - This technique is designed to prevent **fistula formation** and recanalization but does not involve fimbriectomy. *Madlener procedure* - The **Madlener procedure** involves **crushing a section** of the fallopian tube, usually a knuckle, and then ligating it. - This method is simpler but has a **higher failure rate** compared to other sterilization techniques and does not involve removal of the fimbriae.
Question 7: What is meant by Superfecundation?
- A. Fertilization of ova and then its division
- B. Fertilization of two or more ova in one intercourse
- C. Fertilization of two or more ova in different intercourses in same menstrual cycle (Correct Answer)
- D. Fertilization of second ovum after first one is already implanted
Explanation: ***Fertilization of two or more ova in different intercourses in same menstrual cycle*** - **Superfecundation** occurs when two or more ova released during the same menstrual cycle are fertilized by sperm from **separate acts of coitus**. - This can lead to **dizygotic twins** or multiples conceived at different times within a short window, potentially from different biological fathers. *Fertilization of two or more ova in one intercourse* - This scenario describes the fertilization of multiple ova within a **single sexual encounter**, often leading to **dizygotic multiples** but not superfecundation. - Superfecundation specifically implies fertilization from **separate instances of intercourse**. *Fertilization of ova and then its division* - This describes the formation of **monozygotic (identical) twins**, where a single fertilized ovum (zygote) later splits into two or more embryos. - It is distinct from superfecundation, which involves fertilization of **multiple ova**. *Fertilization of second ovum after first one is already implanted* - This describes **superfetation**, a rare phenomenon where a new pregnancy (fertilization and conception) occurs **while already pregnant** from a previous cycle. - Superfecundation, conversely, involves **multiple conceptions within the same menstrual cycle**, not across different cycles.
Question 8: Best time to perform the quadruple test is:
- A. 8-12 weeks
- B. 11-15 weeks
- C. 15-20 weeks (Correct Answer)
- D. 18-22 weeks
Explanation: ***15-20 weeks*** - The quadruple test measures levels of four substances (**alpha-fetoprotein**, **human chorionic gonadotropin**, **unconjugated estriol**, and **inhibin A**) in the mother's blood. - This window is optimal for detecting neural tube defects and chromosomal abnormalities like **Down syndrome** and **Trisomy 18**, allowing for timely counseling and further diagnostic testing if needed. *8-12 weeks* - This period is generally too early for the quadruple test to be accurate, as the levels of the markers would not be sufficiently distinct for reliable screening. - The **combined first-trimester screening** (nuchal translucency and blood tests for PAPP-A and hCG) is typically performed during this time. *11-15 weeks* - While some components might be detectable at the later end of this range, 15-20 weeks offers a more accurate window for all four markers of the quadruple test. - **Integrated screening**, which combines first and second-trimester markers, would involve blood draws around 10-14 weeks and then 15-20 weeks. *18-22 weeks* - This period is generally considered too late for optimal results of the quadruple test, as the fetal markers might be less indicative or diagnostic interventions options might be limited. - A **detailed ultrasound** for anatomical survey is usually performed around this time.
Question 9: Long-standing pelvic inflammatory disease (PID) may lead to which of the following complications?
- A. Uterine polyposis
- B. Hydrosalpinx (Correct Answer)
- C. Endometriosis
- D. Asherman syndrome
Explanation: ***Hydrosalpinx*** - **Hydrosalpinx** is a condition where the fallopian tube is blocked and filled with serous fluid, representing the **end-stage of chronic pelvic inflammatory disease (PID)**. - Chronic inflammation from **repeated or inadequately treated PID** causes damage to the tubal epithelium, loss of fimbrial function, and **adhesions that seal the distal end of the tube**. - This leads to accumulation of sterile transudate within the obstructed tube, creating a **fluid-filled, dilated fallopian tube**. - It is a major cause of **tubal factor infertility** and increased risk of **ectopic pregnancy**. - Classic imaging finding: **sausage-shaped cystic structure** on ultrasound. *Uterine polyposis* - **Endometrial polyps** are benign growths arising from the endometrium, typically associated with **unopposed estrogen stimulation** or hormonal imbalances. - They are **not a complication of chronic PID** but rather a proliferative endometrial disorder. - Common causes include obesity, tamoxifen use, and perimenopause. *Asherman syndrome* - **Asherman syndrome** involves **intrauterine adhesions** (synechiae) causing partial or complete obliteration of the uterine cavity. - It typically results from **endometrial trauma** following procedures like **D&C (dilatation and curettage)**, particularly post-abortion or postpartum curettage. - While PID can cause adhesions, Asherman syndrome specifically refers to **intrauterine** adhesions, not a typical sequela of chronic PID, which primarily affects the **tubes and ovaries**. *Endometriosis* - **Endometriosis** is the presence of **endometrial tissue outside the uterine cavity**, most commonly on ovaries, pelvic peritoneum, and uterosacral ligaments. - It is thought to result from **retrograde menstruation** (Sampson's theory) and genetic/immune factors. - It is **not caused by PID** but is a distinct pathological entity with different etiology and pathophysiology.
Question 10: Dilatation & curettage (D&C) is contraindicated in-
- A. Pelvic inflammatory disease (PID) (Correct Answer)
- B. Endometriosis
- C. Ectopic pregnancy
- D. Abnormal uterine bleeding
Explanation: ***Pelvic inflammatory disease (PID)*** - D&C is **contraindicated** in PID due to the high risk of **spreading pre-existing infection** from the cervix or vagina into the sterile uterine cavity and beyond. - This procedure can worsen the infection, potentially leading to **sepsis**, **tubo-ovarian abscesses**, or chronic pain. *Endometriosis* - D&C is not typically contraindicated in **endometriosis**, as it is sometimes used diagnostically to rule out other causes of abnormal uterine bleeding, though it isn't a treatment for endometriosis itself. - Endometriosis involves the presence of **endometrial tissue outside the uterus**, and a D&C performed on the uterus does not directly exacerbate this condition. *Ectopic pregnancy* - D&C is not contraindicated in **ectopic pregnancy**; however, it is not the primary treatment. - A D&C may be performed if the diagnosis of ectopic pregnancy is uncertain and to rule out an **intrauterine pregnancy** or retained products of conception. *Abnormal uterine bleeding* - D&C is frequently indicated and can be both **diagnostic and therapeutic** for abnormal uterine bleeding, especially to investigate causes like polyps, fibroids, or endometrial hyperplasia. - It helps in obtaining tissue for **histopathological examination** to guide further management.