NEET-PG 2018 — Microbiology
22 Previous Year Questions with Answers & Explanations
Which organism is the most common cause of acute bacterial prostatitis?
Which of the following organisms is MOST associated with histamine production in scombroid fish poisoning?
Identify the organism related to the blood smear image.
What is the Australian antigen for hepatitis B?
Cutaneous larva migrans is caused by which organism?
Which fungus is most commonly associated with orbital cellulitis in patients with diabetic ketoacidosis?
Acute Hemorrhagic Conjunctivitis is primarily caused by which type of Enterovirus?
Urea breath test is used for diagnosis of:
Whole blood is used as a sample for which of the following tests?
Sabin Feldman dye test is used for diagnosis of which of the following condition?
NEET-PG 2018 - Microbiology NEET-PG Practice Questions and MCQs
Question 1: Which organism is the most common cause of acute bacterial prostatitis?
- A. Enterococcus
- B. Streptococcus viridans
- C. Peptostreptococcus
- D. E.coli (Correct Answer)
Explanation: ***E.coli*** - **E.coli** is the most common cause of **acute bacterial prostatitis**, accounting for a significant majority of cases. - It is a **gram-negative rod** commonly found in the gastrointestinal tract and can ascend into the urinary tract and prostate. *Enterococcus* - While **Enterococcus species** can cause urinary tract infections and, less commonly, prostatitis, they are a distant second to E.coli in frequency. - They are **gram-positive cocci** and are often associated with catheter-associated infections or healthcare-acquired infections. *Streptococcus viridans* - **Streptococcus viridans** group bacteria are typically commensals of the oral cavity and are more known for causing **endocarditis** or dental infections. - They are not a common cause of acute bacterial prostatitis. *Peptostreptococcus* - **Peptostreptococcus** is a genus of **anaerobic gram-positive cocci** commonly found in the normal flora of the mouth, gastrointestinal tract, and vagina. - They are typically involved in **polymicrobial anaerobic infections** but are not a primary or common cause of acute bacterial prostatitis.
Question 2: Which of the following organisms is MOST associated with histamine production in scombroid fish poisoning?
- A. Morganella morganii (Correct Answer)
- B. P. aeruginosa
- C. Staphylococcus
- D. Salmonella
Explanation: ***Morganella morganii*** - ***Morganella morganii*** is the **MOST commonly implicated organism** in **scombroid fish poisoning** - It produces the enzyme **histidine decarboxylase**, which converts **histidine** (abundant in scombroid fish like tuna, mackerel, bonito) to **histamine** - When fish are stored at improper temperatures (>15°C), *M. morganii* proliferates and produces large amounts of **histamine** - Other histamine-producing bacteria include *Klebsiella*, *Proteus*, *Enterobacter*, and *Photobacterium* species - Symptoms mimic an **allergic reaction**: flushing, headache, palpitations, urticaria, diarrhea *Staphylococcus* - ***Staphylococcus aureus*** causes **staphylococcal food poisoning** through preformed **enterotoxins** (not histamine) - Associated with protein-rich foods left at room temperature - Causes rapid-onset nausea, vomiting, and abdominal cramps - **Not a significant cause** of scombroid fish poisoning *Salmonella* - ***Salmonella*** species cause **gastroenteritis** through direct infection and invasion of intestinal mucosa - Symptoms include **diarrhea**, **fever**, and **abdominal cramps** with longer incubation period (6-72 hours) - **Not associated** with histamine production or scombroid poisoning *P. aeruginosa* - ***Pseudomonas aeruginosa*** is an **opportunistic pathogen** causing hospital-acquired infections - Associated with wound infections, pneumonia, and UTIs in immunocompromised patients - **Not a cause** of foodborne histamine poisoning
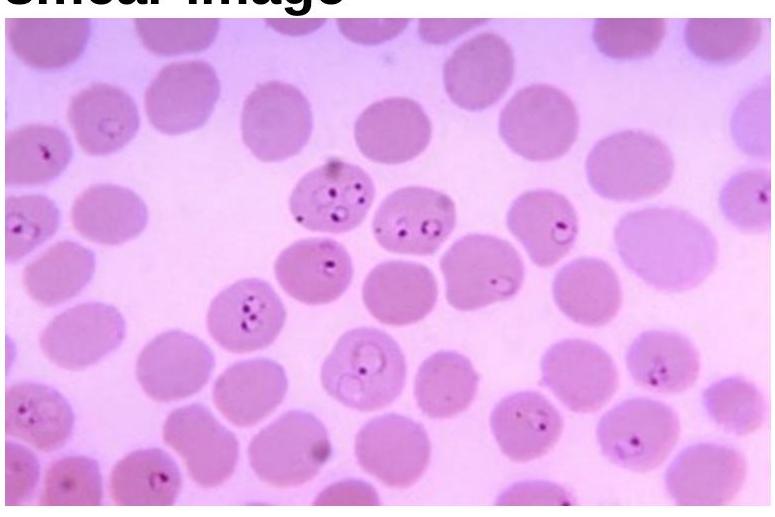
Question 3: Identify the organism related to the blood smear image.
- A. Plasmodium falciparum (Correct Answer)
- B. Salmonella Typhi
- C. Toxoplasma gondii
- D. Treponema pallidum
Explanation: ***Plasmodium falciparum*** - The image clearly displays multiple **ring-form trophozoites** within red blood cells, some of which are *appliqué* or *accolade* forms (rings on the periphery of the red blood cell) and **multiple rings per red blood cell**, which are characteristic of *P. falciparum*. - Presence of **multiple parasites per red blood cell** and various developmental stages including occasional **banana-shaped gametocytes**, though not prominent in this specific field, are key indicators of *P. falciparum* infection, differentiating it from other malarial species. - *P. falciparum* is the most dangerous malarial species and can cause **cerebral malaria** and other severe complications. *Salmonella Typhi* - This bacterium causes **typhoid fever** and is typically identified through **blood culture** or serological tests (Widal test), not by direct visualization within red blood cells on a peripheral blood smear. - *Salmonella Typhi* is an **intracellular bacterium** that primarily infects phagocytic cells (macrophages), not erythrocytes, and does not present as ring forms or other parasitic stages in blood smears. *Toxoplasma gondii* - This parasite causes **toxoplasmosis** and is typically found as **tachyzoites** or **bradyzoites** (within cysts) in tissue samples or less commonly in macrophages in disseminated disease, but not as ring forms within red blood cells on a peripheral blood smear. - Diagnosis usually involves **serological testing** for IgM/IgG antibodies or PCR, as opposed to direct visualization of unique forms in blood smears. *Treponema pallidum* - This is the spirochete responsible for **syphilis** and is too small and thin (0.1-0.2 μm diameter) to be seen with standard light microscopy on routine blood smears. - It is best identified using **dark-field microscopy** or serological tests (VDRL, RPR, TPPA, FTA-ABS) and does not infect red blood cells in the manner shown.
Question 4: What is the Australian antigen for hepatitis B?
- A. HBsAg (Correct Answer)
- B. HBeAg
- C. HBDAg
- D. HBV DNA
Explanation: ***HBsAg*** - **HBsAg** stands for **Hepatitis B surface antigen**, which was originally discovered by Baruch Blumberg in 1965 and was initially called the **Australia antigen** due to its discovery in the serum of an Australian aboriginal. - Its presence indicates an **active hepatitis B infection**, either acute or chronic. *HBeAg* - **HBeAg** (Hepatitis B e-antigen) is a marker of **viral replication** and **infectivity**. - It is distinct from HBsAg and indicates a high level of **transmissibility** of the virus. *HBDAg* - **HBDAg** is not a standard or recognized antigen for hepatitis B. - The correct antigen for hepatitis D is **HDAg** (Hepatitis D antigen), which is only found in individuals co-infected with hepatitis D virus and hepatitis B virus. *HBV DNA* - **HBV DNA** refers to the viral genetic material of the hepatitis B virus. - While its presence indicates active viral replication and is used to monitor **viral load**, it is not an antigen but rather the **viral genome** itself.
Question 5: Cutaneous larva migrans is caused by which organism?
- A. Strongyloides
- B. Toxocara canis
- C. Ancylostoma braziliense (Correct Answer)
- D. Necator americanus
Explanation: ***Ancylostoma braziliense*** - This **hookworm** species commonly found in dogs and cats is the most frequent cause of **cutaneous larva migrans** in humans. - The larvae penetrate the skin but cannot complete their life cycle in humans, instead migrating aimlessly creating **serpiginous tracks**. *Strongyloides* - **_Strongyloides stercoralis_** causes **strongyloidiasis**, which presents with a rapidly advancing (up to 10 cm/hr) migratory rash known as **larva currens**, and not the slower cutaneous larva migrans. - It differs from cutaneous larva migrans in its ability to complete its life cycle in humans, leading to **autoinfection**. *Toxocara canis* - **_Toxocara canis_** is the causative agent of **visceral larva migrans** and **ocular larva migrans**, not cutaneous larva migrans. - In visceral larva migrans, larvae migrate through internal organs, causing symptoms like **hepatomegaly** and **eosinophilia**. *Necator americanus* - This is a human hookworm that can cause **iron deficiency anemia** due to chronic blood loss in the intestines. - While its larvae can penetrate the skin, causing a transient itchy rash known as **ground itch**, they do not cause the prolonged, migratory cutaneous larva migrans.
Question 6: Which fungus is most commonly associated with orbital cellulitis in patients with diabetic ketoacidosis?
- A. Candida
- B. Mucor
- C. Rhizopus (Correct Answer)
- D. Aspergillus
Explanation: ***Rhizopus*** - *Rhizopus* is the most common cause of **mucormycosis** (also called zygomycosis), an aggressive fungal infection that frequently affects immunocompromised patients, especially those with **diabetic ketoacidosis (DKA)**. - *Rhizopus arrhizus* (formerly *R. oryzae*) accounts for approximately **70% of all mucormycosis cases**, making it the single most common causative organism. - In DKA, the acidic environment and high glucose levels favor the growth of **Mucorales fungi**, leading to rapid progression from the sinuses to the orbit and brain (rhinoorbital-cerebral mucormycosis). *Candida* - While *Candida* is a common cause of fungal infections, it typically manifests as **candidemia**, **esophagitis**, or **vulvovaginitis**, and is rarely associated with orbital cellulitis in DKA. - *Candida* infections are more likely in patients with indwelling catheters or those on broad-spectrum antibiotics, rather than specifically linked to DKA-induced orbital cellulitis. *Mucor* - The genus *Mucor* is part of the **Mucorales order** and can cause **mucormycosis** with identical clinical presentations to *Rhizopus*. - However, *Mucor* species account for only **10-20% of mucormycosis cases**, making *Rhizopus* the **most commonly** associated genus as asked in the question. - While both are clinically grouped under "mucormycosis," *Rhizopus* is the more specific and statistically correct answer when identifying the most common causative fungus. *Aspergillus* - *Aspergillus* species are common environmental fungi that can cause invasive infections, particularly in immunocompromised patients, leading to conditions like **aspergilloma** or **invasive aspergillosis**. - While *Aspergillus* can cause sinus and orbital infections, it is less commonly associated with the rapid, aggressive form of orbital cellulitis seen in DKA compared to mucormycosis caused by *Rhizopus*.
Question 7: Acute Hemorrhagic Conjunctivitis is primarily caused by which type of Enterovirus?
- A. Enterovirus type 68
- B. Enterovirus type 69
- C. Enterovirus type 70 (Correct Answer)
- D. Enterovirus type 71
Explanation: ***Enterovirus type 70*** - **Enterovirus type 70** is the most common cause of **Acute Hemorrhagic Conjunctivitis (AHC)**, particularly in epidemic outbreaks. - AHC presents with rapid onset of **ocular pain**, **redness**, **swelling**, and **subconjunctival hemorrhages**. *Enterovirus type 68* - **Enterovirus D68 (EV-D68)** is primarily known for causing **respiratory illnesses**, ranging from mild to severe, and is associated with acute flaccid myelitis. - While it can cause respiratory symptoms, it is not a primary cause of **Acute Hemorrhagic Conjunctivitis**. *Enterovirus type 69* - **Enterovirus type 69** is a rare serotype and is not typically associated with specific human diseases or large-scale outbreaks. - Unlike EV70, it is not recognized as a significant cause of **conjunctivitis**. *Enterovirus type 71* - **Enterovirus A71 (EV-A71)** is a common cause of **hand, foot, and mouth disease (HFMD)**, especially in children, and can also lead to severe neurological complications. - While it causes various infections, it is not the primary cause of **hemorrhagic conjunctivitis**.
Question 8: Urea breath test is used for diagnosis of:
- A. H. pylori (Correct Answer)
- B. E. coli
- C. Lactobacillus
- D. Campylobacter jejuni
Explanation: ***H. pylori*** - The **urea breath test** is a common and accurate non-invasive method to detect current **Helicobacter pylori** infection. - H. pylori produces the enzyme **urease**, which breaks down ingested urea into ammonia and carbon dioxide, which is then exhaled and measured. *Campylobacter jejuni* - **Campylobacter jejuni** is a common cause of **bacterial gastroenteritis** and typically diagnosed via **stool culture**. - It does not possess the **urease** enzyme, so a urea breath test would not be positive. *E.coli* - **E. coli** is a diverse group of bacteria, some strains causing gastrointestinal illness, but it is not associated with **urease production** for diagnostic purposes. - Diagnosis for diarrheagenic E. coli strains usually involves **stool culture** and specific toxin assays. *Lactobacillus* - **Lactobacillus** are beneficial bacteria commonly found in the gut and are not typically associated with pathogenic infections requiring a **urea breath test**. - They do not produce the **urease** enzyme in quantities relevant for this diagnostic test.
Question 9: Whole blood is used as a sample for which of the following tests?
- A. Genexpert
- B. Blood Culture for Bacteria
- C. Interferon Gamma Release Assay (IGRA) (Correct Answer)
- D. Serological Test for Viruses
Explanation: ***Interferon Gamma Release Assay (IGRA)*** - IGRAs, such as QuantiFERON-TB Gold, directly measure **interferon-gamma release** from T-lymphocytes stimulated by *Mycobacterium tuberculosis* antigens. - This test requires **fresh whole blood** as the living lymphocytes are essential for the immune response measured. *Blood Culture for Bacteria* - While blood is cultured, the primary goal is to **isolate and identify viable bacteria** from the bloodstream, not to detect an immune response within the whole blood itself. - Blood cultures typically involve placing blood into specific **culture media** to promote bacterial growth. *Genexpert* - The GeneXpert MTB/RIF assay is a **molecular test** used to detect *Mycobacterium tuberculosis* DNA and rifampicin resistance. - This assay is typically performed on **sputum samples** or other bodily fluids, not whole blood, to diagnose active tuberculosis. *Serological Test for Viruses* - Serological tests for viruses detect **antibodies or antigens** in the blood, which circulate in the **plasma or serum** component of blood. - These tests typically use **separated serum or plasma**, rather than whole blood, as the cellular components are not required for antibody or antigen detection.
Question 10: Sabin Feldman dye test is used for diagnosis of which of the following condition?
- A. Botulism
- B. Toxoplasmosis (Correct Answer)
- C. Sarcoidosis
- D. Yellow fever
Explanation: ***Toxoplasmosis*** The **Sabin-Feldman dye test** is a **serological assay** used to detect specific IgG antibodies against *Toxoplasma gondii*, the causative agent of toxoplasmosis. It measures the ability of antibodies in a patient's serum to prevent the cytoplasmic staining of live toxoplasma tachyzoites by methylene blue dye, indicating an **active immune response** to the parasite. This classic test has high sensitivity and specificity for detecting toxoplasma antibodies and is considered the gold standard serological test, though it has been largely replaced by ELISA and IFA in routine practice due to the requirement for live organisms. *Botulism* Botulism is diagnosed through **toxin detection** in serum, stool, or food samples using mouse bioassay, or by culturing *Clostridium botulinum* from clinical specimens. The Sabin-Feldman dye test is not relevant for the diagnosis of botulism, which is a **neuroparalytic disease** caused by botulinum neurotoxin blocking acetylcholine release at neuromuscular junctions. *Sarcoidosis* Sarcoidosis is a multisystem **granulomatous disease** diagnosed primarily by **tissue biopsy** showing non-caseating granulomas along with compatible clinical and radiological findings. Supportive tests include elevated serum ACE levels and Kveim test (historical). There is no serological test like the Sabin-Feldman dye test associated with the diagnosis of sarcoidosis, as it is not an infectious disease requiring antibody detection. *Yellow fever* Yellow fever is a **viral hemorrhagic disease** caused by a flavivirus, diagnosed by detecting viral RNA through RT-PCR or specific IgM antibodies in the acute phase of infection using ELISA or immunofluorescence. The Sabin-Feldman dye test is not used for viral infections like yellow fever, as it specifically targets **toxoplasma antibodies** and has no role in arboviral disease diagnosis.