Factor V mutation most commonly initially presents as:-
Which of the following conditions is most commonly associated with cryoglobulinemia?
Which of the following is seen in Rheumatoid Arthritis?
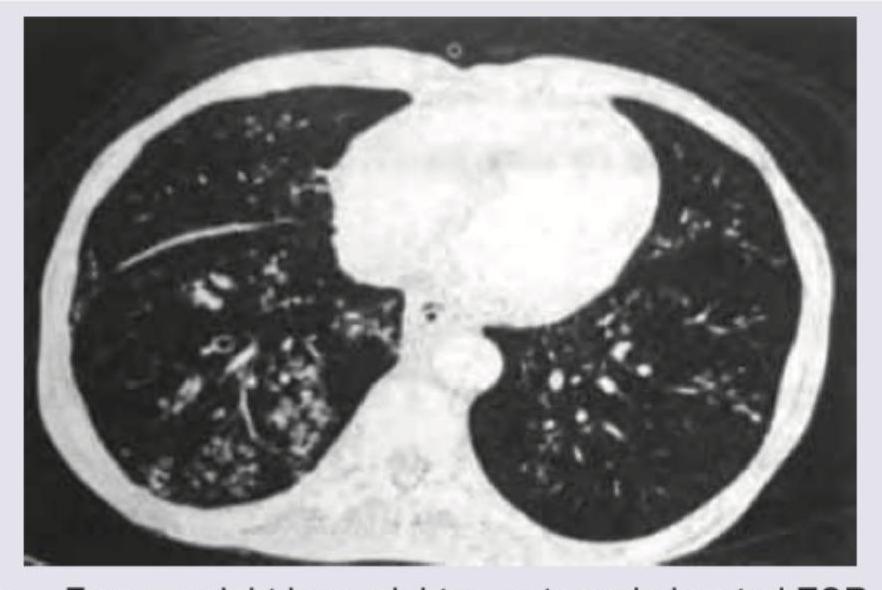
All are true about the mid brain stroke syndrome shown except:
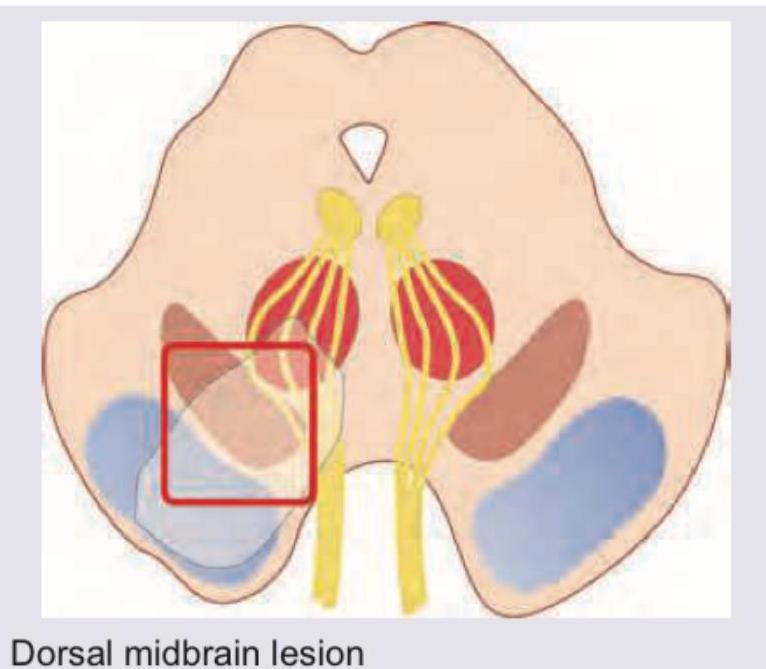
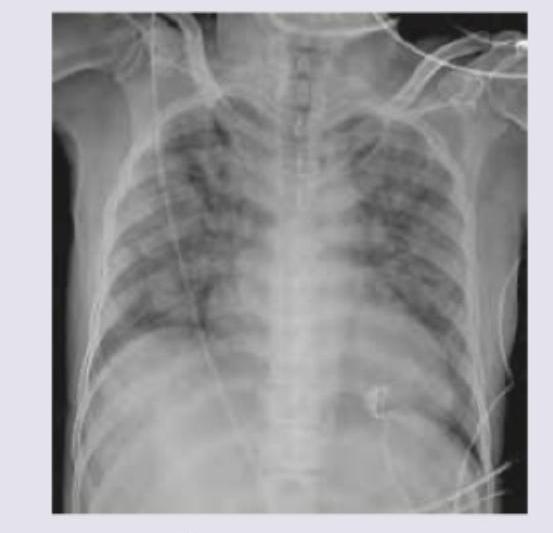
A patient in ICU was given blood transfusion. 3 hours later SpO2 is reduced to 75% with respiratory difficulty. CVP is 15 cm water and PCWP is 25 mm Hg . CXR is shown below. What is the diagnosis?
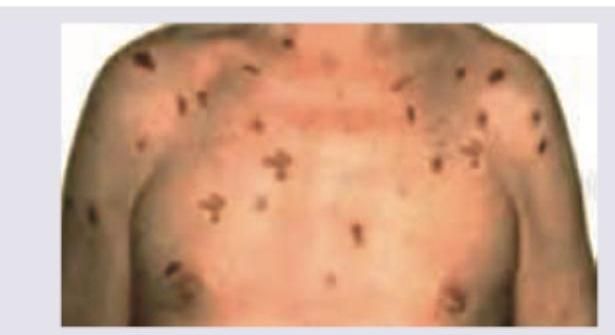
A patient undergone a Solid organ transplant is having the following lesions which are present on oral mucosa and sites shown below. Which of the following is incriminated in causing the same?
The finding shown below is used for diagnosis of CNS parasitic lesion. Which of the following best describes the condition?
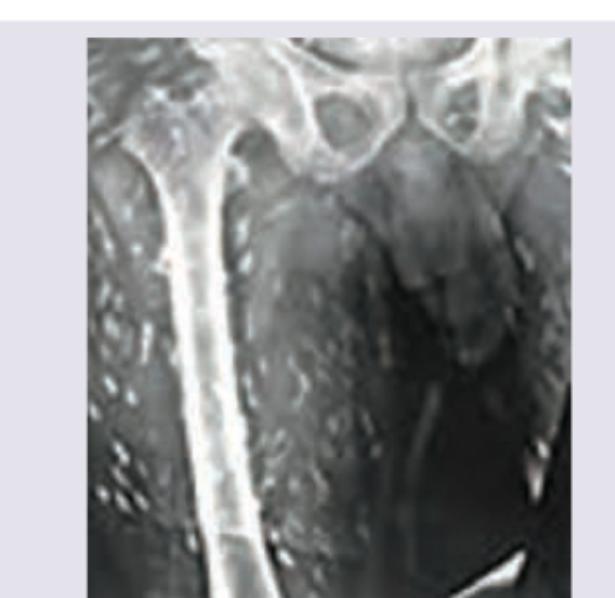
Which one of the following is implicated in the etiology of these adhesions around the liver?
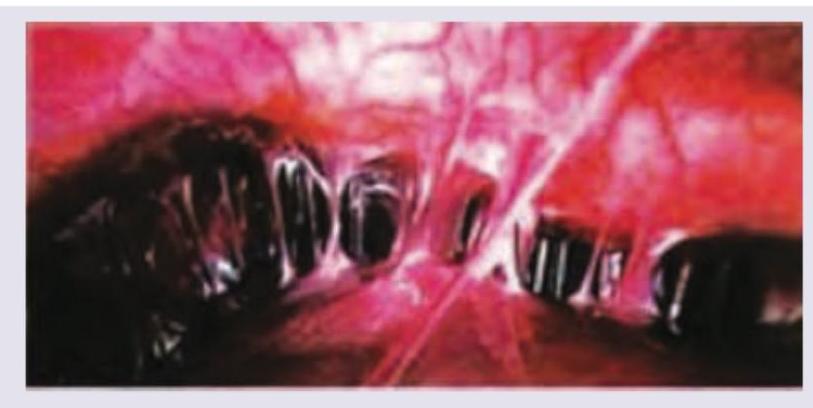
Identify the following abnormality?
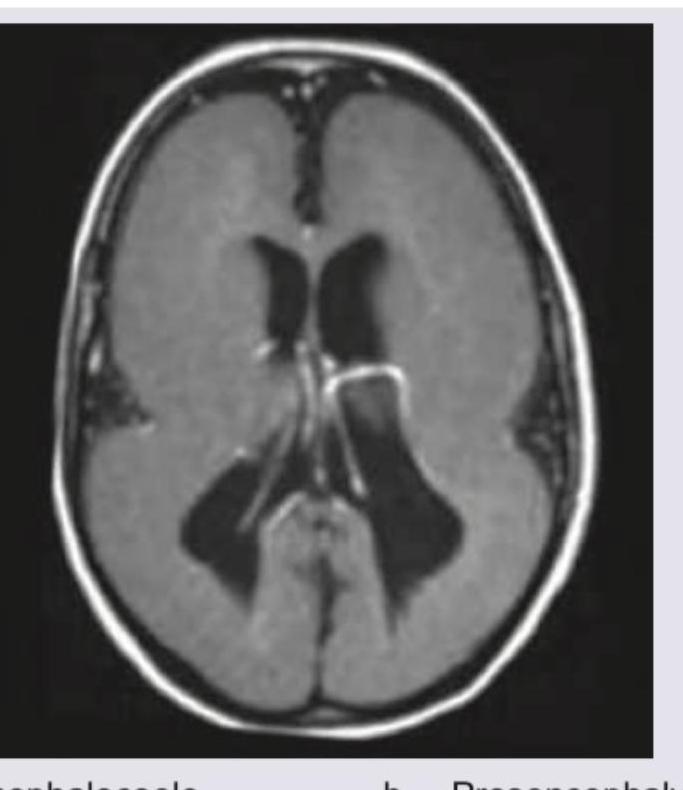
Which of the following will best describe this patient?