TRALI occurs within how many hours of transfusion?
Which one of the following statements about Graves' disease is FALSE?
In Bartter syndrome defect is seen in:
Patient presenting with cutaneous vasculitis, glomerulonephritis, peripheral neuropathy, Which investigation is to be performed next that will help you diagnose the condition?
Which is not included in AIDS related complex?
Choose the best method of diagnosis for the clinical sign represented in the image.
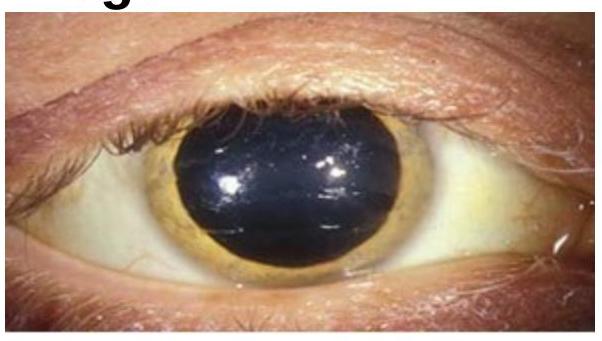
What is the earliest feature of third cranial nerve involvement in a patient with diabetes mellitus?
Which condition is associated with the ECG pattern known as pseudo P pulmonale?
What is a potential cause of cardiogenic shock other than myocardial infarction (MI)?
Which of the following is the MOST characteristic feature of ataxia telangiectasia?