NEET-PG 2018 — Internal Medicine
41 Previous Year Questions with Answers & Explanations
Cyroglobulinemia is associated with:
Calculate the GCS of a 25-year-old head injury patient who is confused, opens their eyes in response to pain, and localizes pain. What is the GCS score?
Which condition is associated with congenital adrenal hyperplasia?
Which drug is used as an adjunct to epinephrine in refractory ventricular fibrillation/ventricular tachycardia during cardiac arrest?
A boy presented with multiple non suppurative osteomyelitis with sickle cell anaemia. What will be the causative organism?
Patient presenting with cutaneous vasculitis, glomerulonephritis, peripheral neuropathy, Which investigation is to be performed next that will help you diagnose the condition?
Which of the following is a cause of hypokalemic metabolic alkalosis with hypertension?
Which is not included in AIDS related complex?
TRALI occurs within how many hours of transfusion?
Which one of the following statements about Graves' disease is FALSE?
NEET-PG 2018 - Internal Medicine NEET-PG Practice Questions and MCQs
Question 1: Cyroglobulinemia is associated with:
- A. Hepatitis A
- B. Hepatitis C (Correct Answer)
- C. Hepatitis B
- D. Hepatitis D
Explanation: ***Hepatitis C*** - **Cryoglobulinemia** is most strongly associated with chronic **Hepatitis C virus (HCV)** infection [1]. - HCV infection can lead to the formation of **cryoglobulins**, which are immunoglobulins that precipitate in the cold and can cause systemic vasculitis [1]. *Hepatitis A* - **Hepatitis A** is an acute, self-limiting viral infection that is not typically associated with chronic complications like cryoglobulinemia. - It primarily causes **acute hepatitis** and does not lead to chronic carrier states or immune complex diseases. *Hepatitis B* - While **Hepatitis B virus (HBV)** can be associated with immune complex diseases, such as **polyarteritis nodosa (PAN)** and **glomerulonephritis**, it is less commonly linked to cryoglobulinemia than HCV. - HBV-associated immune complex diseases generally involve different pathogenesis and clinical presentations than HCV-associated cryoglobulinemia. *Hepatitis D* - **Hepatitis D virus (HDV)** infection occurs only in individuals already infected with HBV. - While HDV can worsen the progression of HBV-related liver disease, it is not independently associated with cryoglobulinemia.
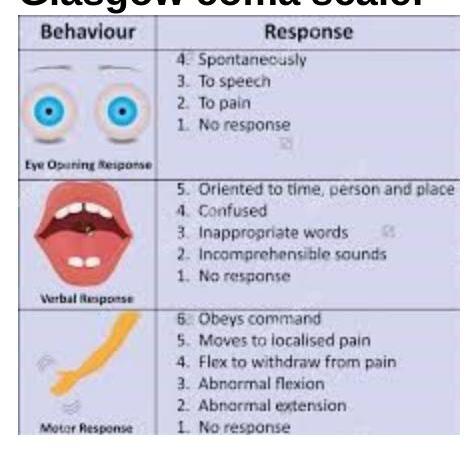
Question 2: Calculate the GCS of a 25-year-old head injury patient who is confused, opens their eyes in response to pain, and localizes pain. What is the GCS score?
- A. 6
- B. 12
- C. 11 (Correct Answer)
- D. 7
Explanation: ***11*** - **Eye-opening response**: The patient opens eyes in response to pain, which scores 2 points on the GCS. - **Verbal response**: The patient is confused, which scores 4 points on the GCS. - **Motor response**: The patient localizes pain, which scores 5 points on the GCS. - The total GCS is 2 (eyes) + 4 (verbal) + 5 (motor) = **11**. *6* - A GCS of 6 would imply much lower scores in at least two categories (e.g., eye opening to pain (2), incomprehensible sounds (2), abnormal extension (2)), indicating a more severe coma. - This option incorrectly sums the individual components given in the scenario. *12* - A GCS of 12 would suggest a higher level of consciousness than described (e.g., eyes to speech (3), confused (4), moves to localize pain (5)), or other combinations that do not match the specific patient presentation. - This option overestimates the patient's neurological status based on the given symptoms. *7* - A GCS of 7 also represents a significantly lower level of consciousness than the patient's description. For example, it could be eye opening to pain (2), incomprehensible sounds (2), and withdrawal from pain (3), which is not consistent with the patient's specific responses. - This option significantly underestimates the patient's GCS score.
Question 3: Which condition is associated with congenital adrenal hyperplasia?
- A. Male pseudohermaphroditism
- B. True pseudohermaphroditism
- C. Sequential pseudohermaphroditism
- D. Female pseudohermaphroditism (Correct Answer)
Explanation: ***Female pseudohermaphroditism*** - In **21-hydroxylase deficiency**, the most common form of CAH, virilization of a female fetus occurs due to excessive **androgen production** [2], [3]. - This leads to ambiguous genitalia in genetically female (XX) infants, presenting as **female pseudohermaphroditism** [2]. *Male pseudohermaphroditism* - This condition occurs when a **genetically male individual (XY)** has external genitalia that are undervirilized or ambiguous. - It is typically caused by inadequate **androgen synthesis** or action, such as in **androgen insensitivity syndrome**, which is not the primary presentation of CAH [2]. *True pseudohermaphroditism* - This term refers to individuals who possess both **ovarian and testicular tissue**, either in separate gonads or as ovotestes [1], [2]. - It is distinct from CAH, where gonadal tissue is uniform (either ovaries or testes), but the external genitalia are ambiguous due to hormonal imbalances [2]. *Sequential pseudohermaphroditism* - This term is not a recognized medical classification for conditions like CAH. - It does not describe a specific developmental anomaly of the reproductive system related to adrenal function.
Question 4: Which drug is used as an adjunct to epinephrine in refractory ventricular fibrillation/ventricular tachycardia during cardiac arrest?
- A. Atropine
- B. Adenosine
- C. High dose vasopressin
- D. Amiodarone infusion (Correct Answer)
Explanation: ***Amiodarone infusion*** - **Amiodarone** is a **Class III antiarrhythmic** drug commonly used in advanced cardiac life support (ACLS) protocols for refractory **ventricular fibrillation (VF)** or **pulseless ventricular tachycardia (VT)** that persists despite defibrillation and epinephrine [1]. - It works by blocking potassium channels, prolonging repolarization and the refractory period, which helps to stabilize the electrical activity of the heart. *Atropine* - **Atropine** is an anticholinergic drug primarily used to treat **symptomatic bradycardia** by increasing heart rate. - It is not indicated for the treatment of **ventricular fibrillation** or **ventricular tachycardia** during cardiac arrest. *High dose vasopressin* - **Vasopressin** was previously included in some ACLS algorithms as an alternative to epinephrine for **vasoconstrictive effects**, but recent guidelines do not support its routine use in cardiac arrest. - While it can cause **vasoconstriction**, there is no evidence that high-dose vasopressin improves outcomes in refractory VF/VT over epinephrine. *Adenosine* - **Adenosine** is an antiarrhythmic drug used to treat **supraventricular tachycardias (SVTs)** by transiently blocking the AV node. - It is not effective for **ventricular fibrillation** or **ventricular tachycardia** and can even be harmful in these rhythms.
Question 5: A boy presented with multiple non suppurative osteomyelitis with sickle cell anaemia. What will be the causative organism?
- A. Salmonella (Correct Answer)
- B. H. influenzae
- C. Enterobacter species
- D. Staphylococcus aureus
Explanation: ***Salmonella*** - **Salmonella species** are a well-known cause of **osteomyelitis** in patients with **sickle cell anemia**, due to factors like gut mucosal damage and functional asplenia. [1] - The unique pathophysiology of sickle cell disease, including areas of bone infarction and compromised reticulendothelial system function, predisposes these patients to **Salmonella infections**. [1] *Staphylococcus aureus* - While **Staphylococcus aureus** is the most common cause of osteomyelitis in the general population, it is less likely to be the causative organism in patients with **sickle cell anemia** compared to Salmonella. - Its presence usually indicates other predisposing factors like trauma or prosthetic devices. *H. influenzae* - **Haemophilus influenzae** was a common cause of osteomyelitis in children before widespread vaccination but is now rare, especially with routine immunizations. - It is not specifically associated with a higher risk in patients with **sickle cell disease** for osteomyelitis compared to other pathogens. *Enterobacter species* - **Enterobacter species** can cause osteomyelitis, particularly in immunocompromised individuals or following surgery, but they are not uniquely associated with **sickle cell anemia** as a primary cause compared to Salmonella. - Their involvement in non-suppurative osteomyelitis in this specific patient population is less common.
Question 6: Patient presenting with cutaneous vasculitis, glomerulonephritis, peripheral neuropathy, Which investigation is to be performed next that will help you diagnose the condition?
- A. ANCA (Correct Answer)
- B. RA factor
- C. Hbsag
- D. MIF
Explanation: ### ANCA - The combination of **cutaneous vasculitis**, **glomerulonephritis**, and **peripheral neuropathy** points towards a small-vessel vasculitis, for which **ANCA (anti-neutrophil cytoplasmic antibodies)** testing is crucial [1]. - ANCA is highly specific for conditions like **Granulomatosis with Polyangiitis (GPA)** and **Microscopic Polyangiitis (MPA)** [1]. ### RA factor - **Rheumatoid factor (RF)** is primarily associated with **rheumatoid arthritis**, which typically presents with symmetrical polyarthritis, not the constellation of symptoms described. - While RF can be positive in some vasculitides, it is not the most specific initial test for the given clinical presentation. ### Hbsag - **Hepatitis B surface antigen (HbsAg)** typically screens for **Hepatitis B infection**, which can cause **polyarteritis nodosa (PAN)**, a medium-vessel vasculitis. - However, the patient's symptoms (cutaneous vasculitis, glomerulonephritis) are more characteristic of **small-vessel vasculitis**, making ANCA a more direct investigation [1]. ### MIF - **MIF (Macrophage Migration Inhibitory Factor)** is a cytokine involved in inflammation, but it is not a routine diagnostic marker for vasculitis. - It is not used as a primary investigation to diagnose specific autoimmune or inflammatory conditions like vasculitis.
Question 7: Which of the following is a cause of hypokalemic metabolic alkalosis with hypertension?
- A. Liddle syndrome (Correct Answer)
- B. Bartter syndrome
- C. Gitelman syndrome
- D. Renal tubular acidosis
Explanation: ***Liddle syndrome*** - It is an **autosomal dominant** disorder characterized by a mutation in the **ENaC channel**, leading to increased sodium reabsorption and potassium excretion, thus causing **hypokalemia**, **metabolic alkalosis**, and **hypertension**. [1] - This condition mimics **primary hyperaldosteronism** but has **low plasma renin activity** and **low aldosterone levels**. [1] *Bartter syndrome* - This is a genetic disorder affecting the **Na-K-2Cl cotransporter** in the **thick ascending limb** of the loop of Henle, leading to **salt wasting** and compensatory **renin-angiotensin-aldosterone system activation**. - It presents with **hypokalemia**, **metabolic alkalosis**, but typically with **normal or low blood pressure**, not hypertension. *Gitelman syndrome* - This is an autosomal recessive disorder affecting the **thiazide-sensitive Na-Cl cotransporter** in the **distal convoluted tubule**. - It causes **hypokalemic metabolic alkalosis**, hypomagnesemia, and hypocalciuria, but patients are typically **normotensive** or **hypotensive**, distinguishing it from Liddle syndrome. *Renal tubular acidosis* - This is a group of disorders characterized by the **kidneys' inability to excrete acid** or **reabsorb bicarbonate**, leading to **metabolic acidosis**. [2] - While it can cause electrolyte abnormalities, hypokalemia is a feature of certain types (e.g., RTA type 1 and 2), but the defining feature is **metabolic acidosis**, not metabolic alkalosis, and it is not typically associated with hypertension from the primary tubular defect. [2]
Question 8: Which is not included in AIDS related complex?
- A. Recurrent genital candidiasis
- B. Generalised lymphadenopathy
- C. Chronic diarrhea
- D. Ectopic pregnancy (Correct Answer)
Explanation: ***Ectopic pregnancy*** - **Ectopic pregnancy** is a gynecological condition related to reproductive health and is **not a direct manifestation** of HIV infection or one of the opportunistic infections/conditions characteristic of AIDS-related complex. - While HIV can affect overall health during pregnancy, an ectopic pregnancy itself is a different medical issue. *Recurrent genital candidiasis* - **Recurrent genital candidiasis** can be a sign of **diminished immune function** in HIV-positive women [1]. - It is often considered an AIDS-defining condition or a common opportunistic infection seen in the progression of HIV to AIDS-related complex [1]. *Generalised lymphadenopathy* - **Generalized lymphadenopathy**, specifically **persistent generalized lymphadenopathy (PGL)**, is a common early manifestation of HIV infection [1]. - It reflects ongoing immune activation and is part of the spectrum of conditions included in AIDS-related complex [1]. *Chronic diarrhea* - **Chronic diarrhea** (lasting more than one month) is a frequent and significant symptom in individuals with HIV infection, particularly as the disease progresses [1]. - It can be caused by various opportunistic infections or directly by HIV, and is a component of AIDS-related complex or AIDS-defining illness [1].
Question 9: TRALI occurs within how many hours of transfusion?
- A. 6 hours (Correct Answer)
- B. 48 hours
- C. 72 hours
- D. 12 hours
Explanation: ***6 hours*** - **Transfusion-related acute lung injury (TRALI)** is defined as new acute lung injury occurring during or within **6 hours** after the completion of a blood transfusion [1]. - It is a severe and potentially life-threatening transfusion reaction characterized by **acute respiratory distress**, **hypoxemia**, and **bilateral pulmonary infiltrates** on chest imaging [1]. *48 hours* - While other transfusion reactions or complications may manifest within 48 hours, TRALI has a more **acute onset**, typically within the first 6 hours. - A pulmonary event occurring between 6 and 48 hours post-transfusion might be considered **delayed TRALI** or another diagnosis like **transfusion-associated circulatory overload (TACO)**, but the classic definition refers to the 6-hour window. *72 hours* - Reactions occurring 72 hours after transfusion are generally considered **delayed transfusion reactions**, which include conditions like **delayed hemolytic transfusion reactions** or **post-transfusion purpura**. - This timeframe is too long for the typical presentation of TRALI, which is characterized by rapid onset. *12 hours* - Although 12 hours falls within an acute window, the most commonly accepted and diagnostically crucial timeframe for TRALI is **within 6 hours** of transfusion. - A reaction occurring between 6 and 12 hours would still be considered suspiciously TRALI, but the strict definition emphasizes the earlier onset.
Question 10: Which one of the following statements about Graves' disease is FALSE?
- A. Common in male (Correct Answer)
- B. Referred to as toxic diffuse goiter
- C. Results in hyperthyroidism
- D. Autoimmune disorder
Explanation: ***Common in male*** - Graves' disease is significantly **more common in females** than males, with a female-to-male ratio of approximately 7:1 [1]. It is a female predominant disease [2]. - The peak incidence is between the ages of 20 and 50 years, and it is the most common cause of **hyperthyroidism** in women [1], [2]. *Results in hyperthyroidism* - Graves' disease is characterized by the production of **autoantibodies** against the TSH receptor, leading to excessive stimulation of the thyroid gland [1]. - This overstimulation results in **increased synthesis and release of thyroid hormones**, causing a state of hyperthyroidism [2]. *Autoimmune disorder* - Graves' disease is a classic example of an **organ-specific autoimmune disease** [2]. - The immune system mistakenly produces antibodies that mimic the action of TSH, leading to thyroid overactivity [1]. *Referred to as toxic diffuse goiter* - The term "toxic" refers to the **hyperthyroid state** (thyrotoxicosis), and "diffuse goiter" describes the generally uniform enlargement of the entire thyroid gland [1]. - This terminology accurately reflects the typical presentation of Graves' disease, which involves an overactive, diffusely enlarged thyroid gland [2].