NEET-PG 2018 — General Medicine
7 Previous Year Questions with Answers & Explanations
The following gait abnormality is seen in:
In the score shown below, alphabet P stands for?

Which nerve is thickened in this patient of Hansen disease?
This condition shown below is dependent on development of pH of urine. Which of the following subtype development is insensitive to pH of urine?
The following appearance of esophagus is seen in:
A 15-year-old boy presents with abdominal cramps and diarrhea for 8 weeks along with delayed puberty. Perianal examination reveals the following. What is the diagnosis? (NEET Pattern 2018)
The given endoscopy of the patient shows? (NEET Pattern 2018)
NEET-PG 2018 - General Medicine NEET-PG Practice Questions and MCQs
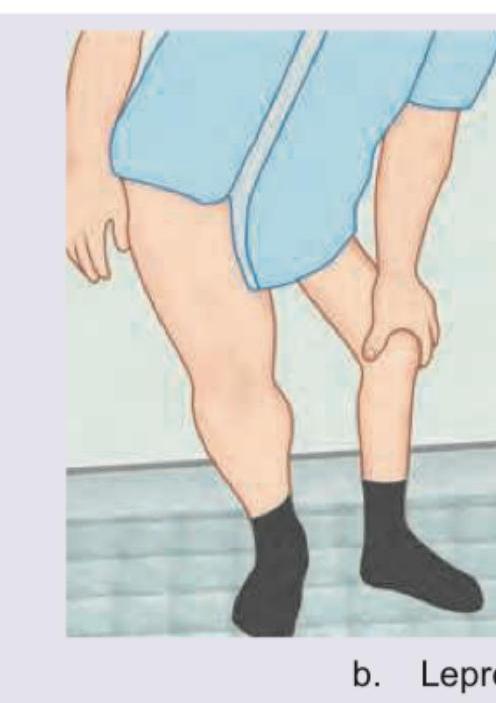
Question 1: The following gait abnormality is seen in:
- A. Avascular necrosis Hip
- B. Spastic hemiplegia
- C. Polio (Correct Answer)
- D. Leprosy
Explanation: The image shows **foot drop**, characterized by inability to dorsiflex the foot, requiring the patient to lift the leg higher during walking to clear the ground. ***Polio*** - **Polio** commonly causes **flaccid paralysis** affecting anterior horn cells, frequently resulting in foot drop due to weakness of **dorsiflexor muscles**. - This is a well-recognized complication, especially in countries like India where polio cases occurred historically, making it a clinically relevant cause. *Leprosy* - While **leprosy** can affect peripheral nerves including the **common peroneal nerve**, foot drop is a less common presentation compared to other nerve involvement patterns. - More typically seen in **advanced, untreated cases** and is relatively rare compared to other causes of foot drop. *Avascular necrosis Hip* - **Avascular necrosis (AVN) of the hip** causes **antalgic gait** due to hip pain but does not cause foot drop. - It affects the **hip joint** rather than the neural pathways controlling dorsiflexion of the foot. *Spastic hemiplegia* - **Spastic hemiplegia** results in spastic gait patterns with **circumduction**, not the flaccid foot drop pattern shown. - Characterized by **spasticity and hyperreflexia** rather than the flaccid weakness seen in foot drop.
Question 2: In the score shown below, alphabet P stands for?
- A. Pulse rate
- B. Pressure
- C. Pallor severity (Correct Answer)
- D. Physical activity
Explanation: ***Pallor severity*** - In the context of the **APGAR score**, 'P' stands for **Pallor/Appearance**, which assesses the infant's skin color. - A healthy color (pink) indicates good oxygenation, while **pallor or cyanosis** suggests poorer perfusion and is scored lower. *Pulse rate* - **Pulse rate** is represented by the first 'A' in APGAR, which stands for **Activity** (muscle tone) or sometimes **Appearance** (skin color), not 'P'. - The 'P' in the APGAR score is specifically for the assessment of the infant's **appearance or skin color**. *Pressure* - The APGAR score does not include an assessment of **pressure** as one of its five components. - The components are **Appearance, Pulse, Grimace, Activity, and Respiration**. *Physical activity* - **Physical activity** (muscle tone) is represented by the second 'A' in APGAR. - The letter 'P' in APGAR specifically refers to **pallor or appearance**.
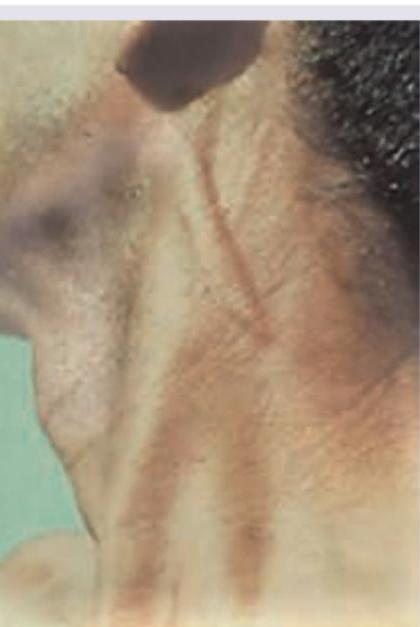
Question 3: Which nerve is thickened in this patient of Hansen disease?
- A. Greater auricular (Correct Answer)
- B. Transverse cervical nerve
- C. Greater occipital nerve
- D. Lesser occipital nerve
Explanation: ***Greater auricular nerve*** - The image shows a **thickened, cord-like structure** indicative of a hypertrophied nerve, characteristic of **Hansen's disease (leprosy)** affecting a peripheral nerve. The location points towards the greater auricular nerve. - The **greater auricular nerve** is a common site for thickening in leprosy due to its superficial course, making it susceptible to the inflammatory response caused by *Mycobacterium leprae*. *Transverse cervical nerve* - While it is a superficial cervical nerve, involvement of the **transverse cervical nerve** in leprosy is less common or prominent for palpation compared to the greater auricular nerve. - Thickening of this nerve might present with sensory changes over the anterior neck, but it is not typically as clearly palpable as the greater auricular nerve in its common course. *Greater occipital nerve* - The **greater occipital nerve** would be located more posteriorly on the scalp and neck, supplying sensation to the posterior scalp. - Its thickening would typically cause pain or sensory changes in the occipital region, which does not align with the visibly thickened nerve shown in the image. *Lesser occipital nerve* - The **lesser occipital nerve** is also located more posteriorly and superiorly in the neck, innervating the skin behind the ear. - While it can be affected in leprosy, its anatomical position and typical presentation of thickening are distinct from the prominent cord visible in the image, which is clearly positioned more anteriorly and inferiorly near the earlobe.
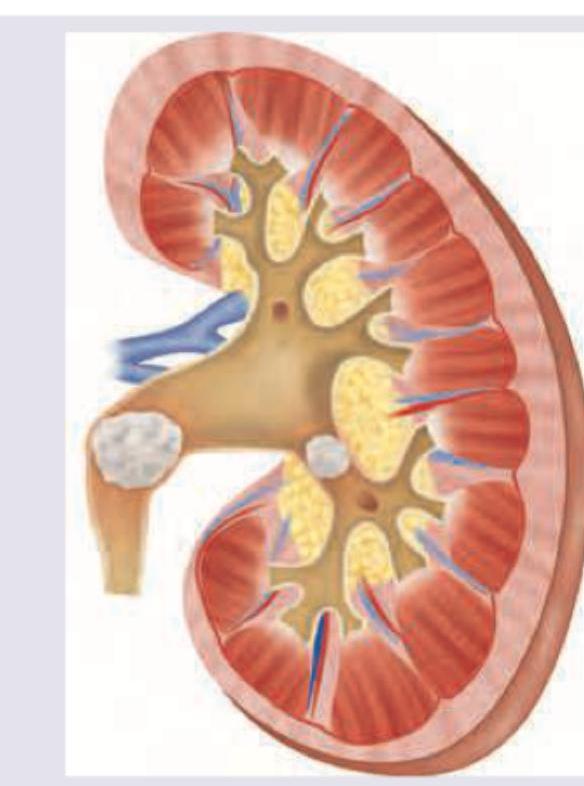
Question 4: This condition shown below is dependent on development of pH of urine. Which of the following subtype development is insensitive to pH of urine?
- A. Calcium oxalate (Correct Answer)
- B. Triple phosphate
- C. Uric acid
- D. Cystine
Explanation: ***Calcium oxalate*** - **Calcium oxalate stones** are the most common type and form **independently of urine pH**, although they can form in a wide range of pH conditions. - Precipitation of calcium oxalate is primarily influenced by concentrations of **calcium and oxalate** in urine, not pH. *Triple phosphate* - **Triple phosphate (struvite) stones** are highly sensitive to **alkaline urine** (pH > 7.0), as they typically form in the presence of urea-splitting bacteria. - These stones are often large, grow rapidly, and are associated with **urinary tract infections**. *Uric acid* - **Uric acid stones** are highly dependent on urine pH, typically forming in **acidic urine** (pH < 5.5). - Alkalinizing the urine (e.g., with potassium citrate) can help **dissolve existing uric acid stones** and prevent new formation. *Cystine* - **Cystine stones** are also pH-sensitive, forming primarily in **acidic urine**, due to the reduced solubility of cystine at lower pH levels. - Urine alkalinization is a key therapeutic strategy for managing cystine stone formation.
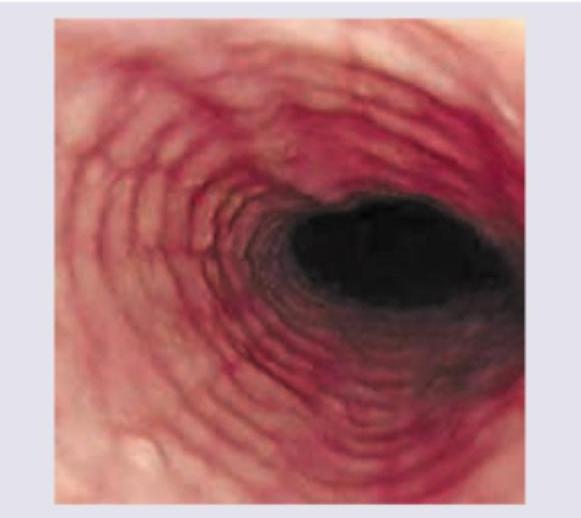
Question 5: The following appearance of esophagus is seen in:
- A. GERD
- B. Stricture
- C. Eosinophilic esophagitis (Correct Answer)
- D. Radiation esophagitis
Explanation: ***Eosinophilic esophagitis*** - The image clearly shows **trachealization** of the esophagus, characterized by **concentric rings** and **linear furrows**, which are hallmark endoscopic findings of eosinophilic esophagitis. - This condition is an **allergic inflammatory disorder** involving the esophagus, often leading to dysphagia and food impaction. *GERD* - While GERD can cause inflammation (esophagitis), it typically presents with **erosions**, **strictures**, or **Barrett's esophagus**, but not the characteristic ringed appearance seen here. - The presence of **longitudinal furrows** and a pale, corrugated appearance rather than the distinct circular rings would be less typical for classic GERD. *Stricture* - A stricture would appear as a **localized narrowing** of the esophageal lumen, which is not the predominant feature in this image. - While strictures can occur in chronic eosinophilic esophagitis, the primary morphological feature visualized is the **ringed esophagus**. *Radiation esophagitis* - This condition results from **radiation exposure** to the chest and typically presents with **mucosal edema**, **erythema**, **ulcerations**, or **fibrosis** in acute and chronic phases, respectively. - It does not commonly cause the distinctive **trachealization** or ringed appearance seen in the image.
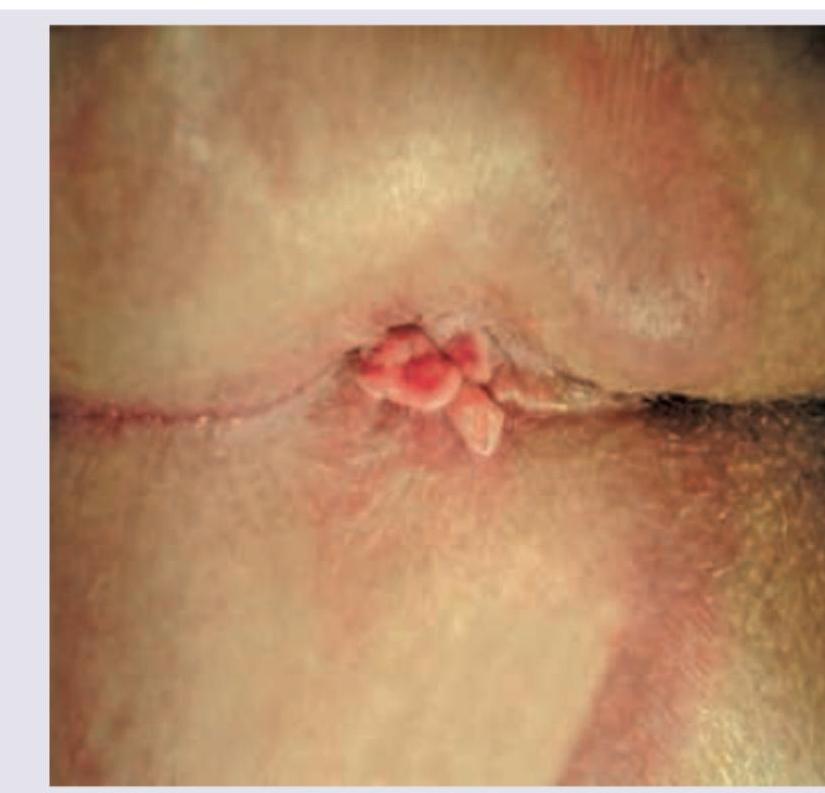
Question 6: A 15-year-old boy presents with abdominal cramps and diarrhea for 8 weeks along with delayed puberty. Perianal examination reveals the following. What is the diagnosis? (NEET Pattern 2018)
- A. Celiac disease
- B. Crohn's disease (Correct Answer)
- C. Ulcerative colitis
- D. Irritable bowel syndrome
Explanation: ***Crohn's disease*** - The combination of **chronic abdominal cramps and diarrhea**, **delayed puberty**, and the presence of **perianal lesions** (like skin tags, fissures, or abscesses, as depicted) is highly indicative of Crohn's disease. - Delayed puberty suggests **malabsorption** and chronic inflammation, which are characteristic systemic effects of Crohn's disease, particularly when it affects the small bowel. *Celiac disease* - While celiac disease can cause **abdominal cramps**, **diarrhea**, and **growth delays** (potentially leading to delayed puberty due to malabsorption), it typically does **not present with perianal lesions**. - It is an **autoimmune response to gluten**, not an inflammatory bowel disease presenting with perianal manifestations. *Ulcerative colitis* - This condition is characterized by **colonic inflammation**, causing symptoms like **bloody diarrhea** and abdominal pain. - While it can manifest with some **extraintestinal symptoms**, **perianal disease** is rare and less severe compared to Crohn's disease, and delayed puberty is less commonly associated. *Irritable bowel syndrome* - IBS is a **functional gastrointestinal disorder** without underlying structural or biochemical abnormalities, presenting with abdominal pain and altered bowel habits. - It does **not cause perianal lesions**, malabsorption, or systemic complications like delayed puberty.
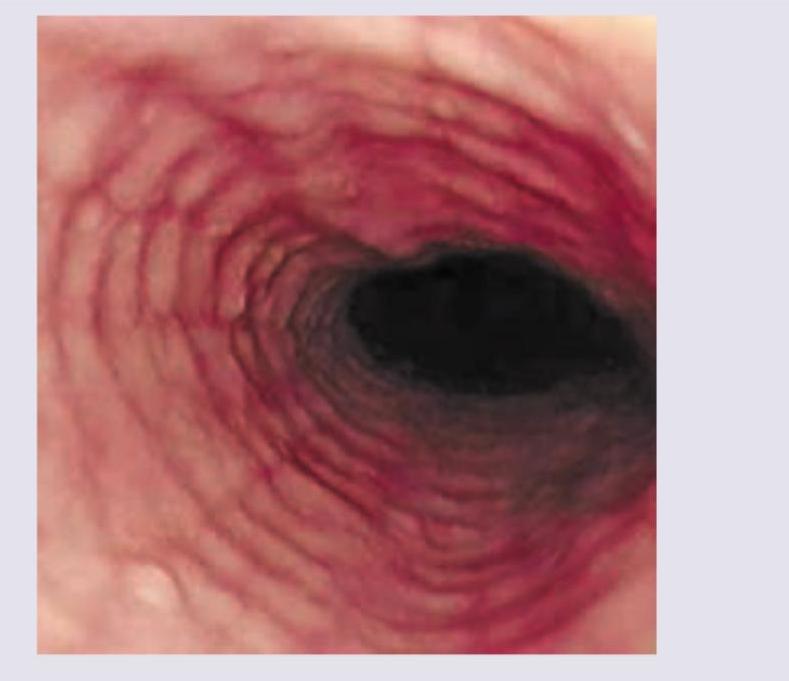
Question 7: The given endoscopy of the patient shows? (NEET Pattern 2018)
- A. Eosinophilic esophagitis (Correct Answer)
- B. Radiation esophagitis
- C. GERD
- D. Carcinoma esophagus
Explanation: **Eosinophilic esophagitis** - The endoscopic image displays prominent **concentric rings** (trachealization) and **linear furrows**, which are classic findings in eosinophilic esophagitis. - These features result from chronic inflammation and fibrosis caused by an allergic reaction leading to significant eosinophil infiltration in the esophageal wall. *Radiation esophagitis* - Endoscopic findings in radiation esophagitis typically include **erythema**, **edema**, **ulcerations**, or **strictures** in the irradiated field. - The characteristic ringed appearance seen in the image is not typical for radiation-induced injury. *GERD* - Endoscopic signs of GERD often include **erosions**, **ulcerations**, **strictures**, or **Barrett's esophagus**, usually in the distal esophagus. - While chronic GERD can cause inflammation, it typically does not produce the pronounced concentric rings and linear furrows characteristic of eosinophilic esophagitis. *Carcinoma esophagus* - Esophageal carcinoma typically presents with a **mass**, **ulceration**, **stricture**, or an **irregular, friable lesion**. - The image does not show any focal mass or destructive lesion suggestive of malignancy.