All SubjectsAnatomy (24)Anesthesiology (4)Biochemistry (1)Biochemistry (26)Community Medicine (12)Dental (1)Dermatology (8)ENT (1)Forensic Medicine (2)General Medicine (7)Internal Medicine (41)Microbiology (22)Obstetrics and Gynecology (23)Ophthalmology (2)Orthopaedics (1)Pathology (3)Pathology (31)Pediatrics (24)Pharmacology (27)Physiology (13)Psychiatry (3)Psychiatry (10)Radiology (30)Surgery (5)Surgery (32)
Q11
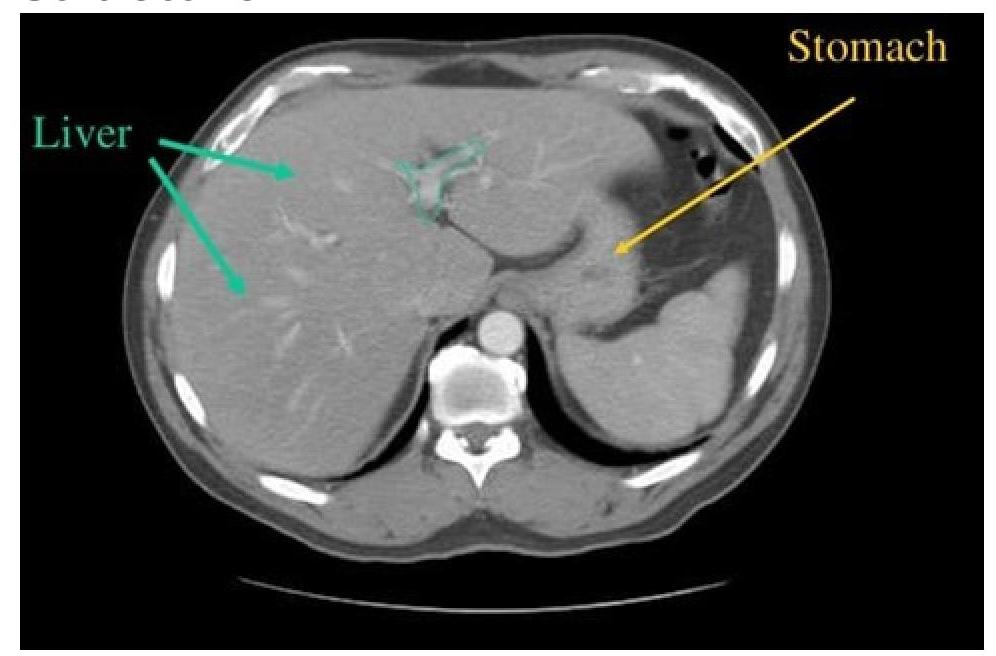
CT scan of abdomen showing a structure branching within the liver. Identify the structure.
Q12
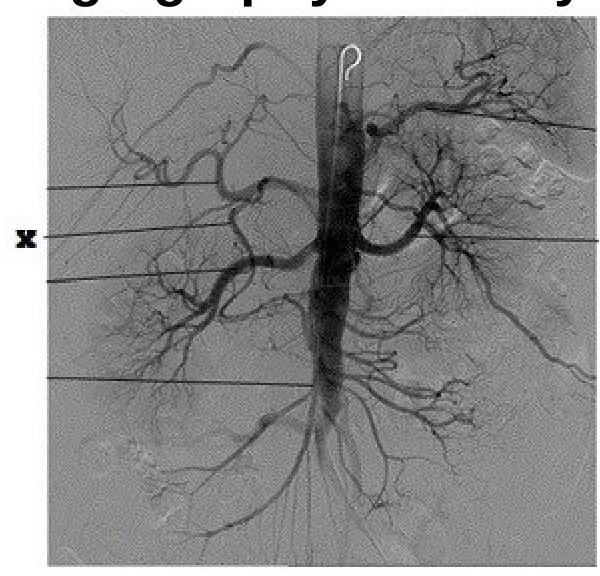
Identify the artery labeled as 'X' in the provided angiography anatomy image.
Q13
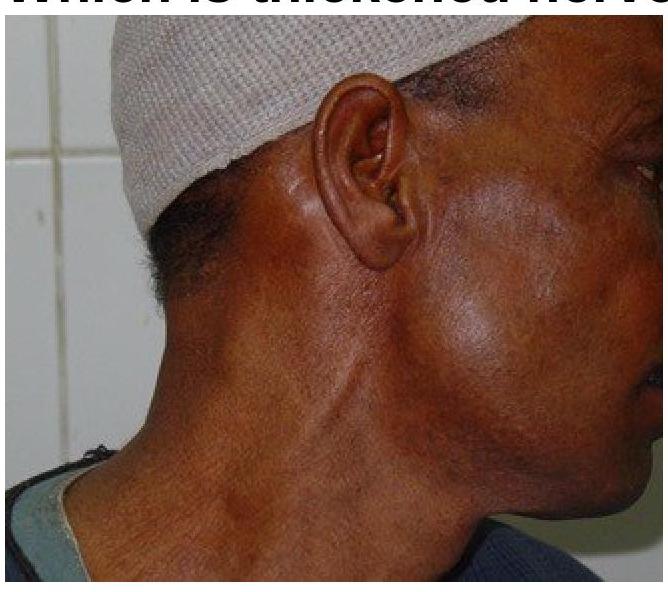
Which thickened nerve is shown in the image?
Q14
Hard palate contains:
Q15
What constitutes the Malpighian layer of skin?
Q16
What is the primary function of the deltoid muscle?
Q17
Nerves of pharyngeal arch develop from
Q18
Wallenberg syndrome involves which artery?
Q19
Nasopharyngeal chordoma arises from:-
Q20
During acute tonsillitis, referred pain from the tonsil to the middle ear occurs via which nerve?