NEET-PG 2018
353 Previous Year Questions with Answers & Explanations
Biochemistry
1 questionsWhich of the following statements regarding phenylketonuria (PKU) is false?
NEET-PG 2018 - Biochemistry NEET-PG Practice Questions and MCQs
Question 1: Which of the following statements regarding phenylketonuria (PKU) is false?
- A. Blood phenyl alanine level >20 mg/dl causes severe disease
- B. Neurological symptoms are due to deficiency of phenylalanine hydroxylase. (Correct Answer)
- C. Method of choice for screening is blood phenylalanine by Guthrie's test.
- D. PKU is caused by a deficiency of phenylalanine hydroxylase.
Explanation: ***Neurological symptoms are due to deficiency of phenylalanine hydroxylase.*** - This statement is **FALSE** - it confuses the cause with the mechanism. - Neurological symptoms in PKU are caused by the **accumulation of phenylalanine and its toxic metabolites** (such as phenylpyruvate, phenyllactate, and phenylacetate) in the brain, not directly by the enzyme deficiency itself. - The deficiency of **phenylalanine hydroxylase** is the underlying cause, but the **toxic buildup** is what damages the developing brain, leading to intellectual disability, seizures, and behavioral problems. *Blood phenyl alanine level >20 mg/dl causes severe disease* - This statement is **TRUE**. - Blood phenylalanine levels **>20 mg/dL** are diagnostic of **classical PKU**, which causes severe disease if untreated. - Normal phenylalanine levels are 1-2 mg/dL; levels >20 mg/dL require strict dietary management to prevent neurological damage. *Method of choice for screening is blood phenylalanine by Guthrie's test.* - This statement is **TRUE** in the traditional context taught for medical exams. - The **Guthrie bacterial inhibition assay** measures blood phenylalanine from a heel prick and has been the standard newborn screening method for decades. - While modern laboratories increasingly use **tandem mass spectrometry (MS/MS)**, the Guthrie test remains a validated and widely taught screening method. *PKU is caused by a deficiency of phenylalanine hydroxylase.* - This statement is **TRUE**. - **Phenylketonuria (PKU)** is an autosomal recessive disorder caused by mutations in the **PAH gene**, leading to deficiency of the enzyme **phenylalanine hydroxylase**. - This enzyme normally converts phenylalanine to tyrosine; its absence leads to phenylalanine accumulation.
Community Medicine
1 questionsWhat is the ratio of incidence of a disease among the exposed to the incidence among non-exposed?
NEET-PG 2018 - Community Medicine NEET-PG Practice Questions and MCQs
Question 1: What is the ratio of incidence of a disease among the exposed to the incidence among non-exposed?
- A. Odds ratio
- B. Relative risk (Correct Answer)
- C. Absolute risk
- D. Attributable risk
Explanation: ***Relative risk*** - **Relative risk** (RR) directly compares the **incidence of disease** in an exposed group to the incidence in an unexposed group. - It is used in **cohort studies** and **randomized controlled trials** to quantify the strength of an association between an exposure and an outcome. *Odds ratio* - The **odds ratio** (OR) is a measure of association between an exposure and an outcome in **case-control studies**. - It compares the odds of exposure among cases to the odds of exposure among controls, not directly comparing incidence rates. *Absolute risk* - **Absolute risk** is the **incidence of a disease** in a population, without comparison to another group. - It represents the probability of developing a disease over a specified period. *Attributable risk* - **Attributable risk** (AR) quantifies the amount of disease that can be **attributed to a specific exposure**. - It is the difference in incidence rates between exposed and unexposed groups, not a ratio.
Dental
1 questionsWhat is the first permanent tooth to erupt?
NEET-PG 2018 - Dental NEET-PG Practice Questions and MCQs
Question 1: What is the first permanent tooth to erupt?
- A. First premolar
- B. Second premolar
- C. First molar (Correct Answer)
- D. Second molar
Explanation: ***First molar*** - The **first molars** are typically the first permanent teeth to erupt, usually around **6 years of age**. - They erupt distal to the primary second molars and are not preceded by primary teeth, making them crucial for establishing the **occlusion**. *First premolar* - **First premolars** typically erupt later, between **10 and 11 years of age**, replacing the primary first molars. - Their eruption is part of the **exchange of primary teeth** for permanent successors. *Second premolar* - The **second premolars** erupt even later, usually between **11 and 12 years of age**, replacing the primary second molars. - They are also involved in the **replacement of primary teeth**, not the initial permanent eruption. *Second molar* - **Second molars** erupt much later than the first molars, typically between **11 and 13 years of age**, distal to the first molars. - They are part of the **later stages of permanent dentition development**.
Dermatology
1 questionsWhich of the following are risk factors for cutaneous lymphoma?
NEET-PG 2018 - Dermatology NEET-PG Practice Questions and MCQs
Question 1: Which of the following are risk factors for cutaneous lymphoma?
- A. Weakened immune system
- B. Age
- C. Gender
- D. All of the options (Correct Answer)
Explanation: ***All of the options*** - **All listed factors**, including age, gender, and a weakened immune system, are recognized risk factors for the development of cutaneous lymphoma. - The risk of cutaneous lymphoma generally **increases with age**, shows a slightly higher incidence in **males**, and is significantly elevated in individuals with **compromised immune systems**. *Age* - While age is a risk factor, it is only one component among several that contribute to the overall risk of developing cutaneous lymphoma. - The incidence of most lymphomas, including cutaneous forms, typically **increases with advancing age**, but other factors also play a critical role. *Gender* - Like age, gender is a recognized risk factor, with a slightly **higher incidence in males** compared to females. - However, gender alone does not fully explain the risk, as environmental and other host-related factors also contribute. *Weakened immune system* - A weakened immune system is a significant risk factor, as it impairs the body's ability to control abnormal cell growth, including cancerous lymphocytes. - However, it is not the sole risk factor; individuals with healthy immune systems can also develop cutaneous lymphoma due to other contributing factors.
Internal Medicine
2 questionsCyroglobulinemia is associated with:
Calculate the GCS of a 25-year-old head injury patient who is confused, opens their eyes in response to pain, and localizes pain. What is the GCS score?
NEET-PG 2018 - Internal Medicine NEET-PG Practice Questions and MCQs
Question 1: Cyroglobulinemia is associated with:
- A. Hepatitis A
- B. Hepatitis C (Correct Answer)
- C. Hepatitis B
- D. Hepatitis D
Explanation: ***Hepatitis C*** - **Cryoglobulinemia** is most strongly associated with chronic **Hepatitis C virus (HCV)** infection [1]. - HCV infection can lead to the formation of **cryoglobulins**, which are immunoglobulins that precipitate in the cold and can cause systemic vasculitis [1]. *Hepatitis A* - **Hepatitis A** is an acute, self-limiting viral infection that is not typically associated with chronic complications like cryoglobulinemia. - It primarily causes **acute hepatitis** and does not lead to chronic carrier states or immune complex diseases. *Hepatitis B* - While **Hepatitis B virus (HBV)** can be associated with immune complex diseases, such as **polyarteritis nodosa (PAN)** and **glomerulonephritis**, it is less commonly linked to cryoglobulinemia than HCV. - HBV-associated immune complex diseases generally involve different pathogenesis and clinical presentations than HCV-associated cryoglobulinemia. *Hepatitis D* - **Hepatitis D virus (HDV)** infection occurs only in individuals already infected with HBV. - While HDV can worsen the progression of HBV-related liver disease, it is not independently associated with cryoglobulinemia.
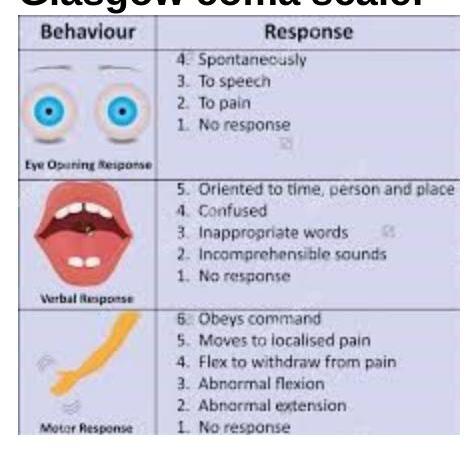
Question 2: Calculate the GCS of a 25-year-old head injury patient who is confused, opens their eyes in response to pain, and localizes pain. What is the GCS score?
- A. 6
- B. 12
- C. 11 (Correct Answer)
- D. 7
Explanation: ***11*** - **Eye-opening response**: The patient opens eyes in response to pain, which scores 2 points on the GCS. - **Verbal response**: The patient is confused, which scores 4 points on the GCS. - **Motor response**: The patient localizes pain, which scores 5 points on the GCS. - The total GCS is 2 (eyes) + 4 (verbal) + 5 (motor) = **11**. *6* - A GCS of 6 would imply much lower scores in at least two categories (e.g., eye opening to pain (2), incomprehensible sounds (2), abnormal extension (2)), indicating a more severe coma. - This option incorrectly sums the individual components given in the scenario. *12* - A GCS of 12 would suggest a higher level of consciousness than described (e.g., eyes to speech (3), confused (4), moves to localize pain (5)), or other combinations that do not match the specific patient presentation. - This option overestimates the patient's neurological status based on the given symptoms. *7* - A GCS of 7 also represents a significantly lower level of consciousness than the patient's description. For example, it could be eye opening to pain (2), incomprehensible sounds (2), and withdrawal from pain (3), which is not consistent with the patient's specific responses. - This option significantly underestimates the patient's GCS score.
Obstetrics and Gynecology
1 questionsWhat is the first-line maneuver for management of shoulder dystocia?
NEET-PG 2018 - Obstetrics and Gynecology NEET-PG Practice Questions and MCQs
Question 1: What is the first-line maneuver for management of shoulder dystocia?
- A. 90 degree rotation of posterior shoulder
- B. Emergency c-section
- C. Supra pubic pressure
- D. Sharp flexion of hip joints towards abdomen (Correct Answer)
Explanation: ***Sharp flexion of hip joints towards abdomen*** - This maneuver, known as the **McRoberts maneuver**, widens the anterior-posterior diameter of the **pelvis** and flattens the sacrum. - It increases the likelihood of dislodging the impacted fetal shoulder from behind the symphysis pubis. *Supra pubic pressure* - **Suprapubic pressure** is applied to the fetal anterior shoulder to dislodge it from the symphysis pubis and guide it under the maternal pubic bone. - This maneuver is typically performed *in conjunction with* the McRoberts maneuver, but the question specifies "sharp flexion of hip joints towards abdomen," which is McRoberts alone. *90 degree rotation of posterior shoulder* - This describes the **Woods screw maneuver**, which involves rotating the posterior shoulder to facilitate delivery. It is a secondary maneuver used if McRoberts and suprapubic pressure are insufficient. - The question asks for the primary management step, and the McRoberts maneuver (sharp flexion) is usually the first line of intervention. *Emergency c-section* - An **emergency C-section** is generally not indicated for the acute management of shoulder dystocia once the head has delivered, as it is a **delivery complication** happening during vaginal birth. - Management focuses on specific maneuvers to release the impacted shoulders through the vagina.
Psychiatry
1 questionsWhat is Prosopagnosia?
NEET-PG 2018 - Psychiatry NEET-PG Practice Questions and MCQs
Question 1: What is Prosopagnosia?
- A. Impairment of consciousness
- B. Being unaware of one's problems
- C. Failure to identify objects
- D. Difficulty in identifying known faces (Correct Answer)
Explanation: ***Difficulty in identifying known faces*** - **Prosopagnosia**, also known as **face blindness**, is a neurological disorder characterized by an inability to recognize familiar faces. - Individuals with prosopagnosia may have trouble recognizing even close family members or their own reflection, despite having intact vision and general intellectual function. - This is a specific type of agnosia limited to face recognition. *Impairment of consciousness* - Impairment of consciousness refers to a reduced state of awareness or responsiveness, often seen in conditions like coma or delirium. - This is a broad neurological state and does not specifically describe the inability to recognize faces. *Being unaware of one's problems* - This symptom is known as **anosognosia**, which is a lack of insight into one's own neurological deficits or illness. - Anosognosia is a problem of self-awareness, not specifically face recognition. *Failure to identify objects* - The inability to identify objects is a form of **agnosia**, specifically **associative visual agnosia** if the person can see the object but not recognize it. - While prosopagnosia is a type of agnosia, it is highly specific to faces, whereas object agnosia refers to a broader failure in object recognition.
Surgery
2 questionsWhich of the following is category 3 in the Maastricht classification of donation after cardiac death?
Which of the following factors is NOT a component of the Van Nuys prognostic index?
NEET-PG 2018 - Surgery NEET-PG Practice Questions and MCQs
Question 1: Which of the following is category 3 in the Maastricht classification of donation after cardiac death?
- A. Awaiting cardiac arrest (Correct Answer)
- B. Patient found deceased upon arrival
- C. Attempts at resuscitation after cardiac arrest
- D. Cardiac arrest following brain death declaration
Explanation: ***Awaiting cardiac arrest*** - This category denotes patients who are anticipated to have a **cardiac arrest** and are considered for organ donation after the cessation of circulatory function. - These individuals are typically in an **intensive care setting**, where withdrawal of life support is planned, leading to eventual cardiac death. *Patient found deceased upon arrival* - This describes individuals who have suffered **unwitnessed cardiac arrest** and are pronounced dead upon the arrival of medical personnel. - Organ viability for donation is often compromised due to the **unknown downtime** and lack of controlled conditions. *Attempts at resuscitation after cardiac arrest* - This category includes patients for whom **resuscitation efforts** were initiated following cardiac arrest but were ultimately unsuccessful. - Organ donation in this context requires assessment of the impact of resuscitation on **organ perfusion** and viability. *Cardiac arrest following brain death declaration* - This scenario describes donation after **neurological determination of death** (brain death), not cardiac death. - In brain death, the heart may still be beating with full circulatory support, and organ procurement occurs while **circulation is maintained**.
Question 2: Which of the following factors is NOT a component of the Van Nuys prognostic index?
- A. Age
- B. Tumor size
- C. Estrogen receptor (ER) status (Correct Answer)
- D. Margin width
Explanation: ***Estrogen receptor (ER) status*** - The **Van Nuys prognostic index** (VNPI) for **ductal carcinoma in situ (DCIS)** assesses factors related to local recurrence risk after breast-conserving therapy. - The VNPI includes: **tumor size, margin width, pathologic classification (nuclear grade and necrosis), and age**. - While ER status is an important prognostic factor in **invasive breast cancer**, it is **not included** in the VNPI scoring system for DCIS. *Age* - **Age** is a key component of the VNPI, with younger patients having higher risk of local recurrence. - Patients **under 40 years** receive score 3, **40-60 years** receive score 2, and **over 60 years** receive score 1. *Tumor size* - The **size of the DCIS lesion** is a critical component of the VNPI. - Lesions **≥41 mm** receive score 3, **16-40 mm** receive score 2, and **≤15 mm** receive score 1. *Margin width* - **Surgical margin width** is an essential component of the VNPI. - Margins **<1 mm** receive score 3, **1-9 mm** receive score 2, and **≥10 mm** receive score 1.
About NEET-PG 2018 Questions
This page contains 353 questions from the NEET-PG 2018 paper, organised across 25 subjects for focused practice. Every question comes with the correct answer and a detailed explanation to help you understand the underlying concept. Subject-wise organisation lets you target specific areas and identify which topics carried the most weight in this particular year.
Practising year-wise papers is essential for understanding how the NEET-PG exam evolves — you can spot trending topics, gauge difficulty shifts, and benchmark your readiness against a real paper. To take your preparation further, download the Oncourse app for AI-driven performance insights, spaced repetition of questions you got wrong, and a personalised study plan built around your NEET-PG goals.