Rat tail appearance in contrast radiography is seen in?
Investigation of choice for screening of proximal internal carotid artery stenosis is :
HU is a measure of
Which of the following appears the same on both T1 and T2 weighted MRI sequences?
Which of the following features is used to identify the colon on an X-ray?
Investigation of choice for studying Renal Cortical mass
Step ladder pattern of gas shadow is seen in
A polytrauma patient's CT brain shows a crescent-shaped extra-axial collection with a concave inner margin. What is the most likely diagnosis?
The longest half life is that of:
NEET-PG 2012 - Radiology NEET-PG Practice Questions and MCQs
Question 21: Rat tail appearance in contrast radiography is seen in?
- A. Carcinoma esophagus
- B. Plummer-Vinson syndrome
- C. Diffuse esophageal spasms
- D. Achalasia cardia (Correct Answer)
Explanation: ***Correct: Achalasia cardia*** - The **"rat tail" or "bird's beak" sign** is the classic radiological appearance of **achalasia cardia** on barium swallow study - Shows **smooth, symmetrical, tapered narrowing** of the distal esophagus with proximal esophageal dilatation - Due to **failure of the lower esophageal sphincter (LES) to relax**, causing functional obstruction - The smooth tapering distinguishes it from irregular narrowing seen in malignancy *Incorrect: Carcinoma esophagus* - Esophageal carcinoma shows **"shouldered lesion"** or **"apple core" appearance** - Characterized by **irregular, shelf-like margins** with abrupt transition - Narrowing is **asymmetric and irregular**, not the smooth tapering of rat tail sign - May show mucosal destruction and filling defects *Incorrect: Plummer-Vinson syndrome* - Shows **postcricoid web** in the upper esophagus on barium swallow - Associated with iron deficiency anemia, glossitis, and increased risk of esophageal cancer - Presents as a thin, web-like membrane rather than distal narrowing *Incorrect: Diffuse esophageal spasms* - Shows **"corkscrew esophagus"** or **"rosary bead" appearance** on barium swallow - Multiple, **simultaneous, non-peristaltic contractions** create segmented appearance - Dynamic finding with normal segments between contractions - Represents uncoordinated muscular activity, not fixed narrowing
Question 22: Investigation of choice for screening of proximal internal carotid artery stenosis is :
- A. Doppler ultrasound (USG) (Correct Answer)
- B. CT angiography
- C. Magnetic resonance imaging (MRI)
- D. Digital subtraction angiography (DSA)
Explanation: ***Doppler ultrasound (USG)*** - **Doppler ultrasound** is the investigation of choice for screening carotid artery stenosis due to its **non-invasive nature**, widespread availability, and cost-effectiveness. It provides excellent anatomical information and hemodynamics, including **blood flow velocity** and presence of **plaque**. - It can effectively estimate the degree of **stenosis** based on flow characteristics and is safe for serial monitoring. *CT angiography* - **CT angiography** provides detailed anatomical imaging of the carotid arteries but involves **ionizing radiation** and **iodinated contrast agents**, making it less suitable for routine screening, especially in patients with renal impairment or contrast allergies. - While it offers higher resolution for certain plaque characteristics, it’s typically reserved for cases where ultrasound findings are inconclusive or for surgical planning. *Magnetic resonance imaging (MRI)* - **MRI** and **MR angiography (MRA)** can visualize carotid stenosis without ionizing radiation but are more expensive and time-consuming than ultrasound, and can be limited by artifacts from patient movement. - Patients with **claustrophobia** or **metallic implants** may not be suitable for MRI, making it less ideal for general screening. *Digital subtraction angiography (DSA)* - **Digital subtraction angiography (DSA)** is the **gold standard** for diagnosing carotid stenosis as it provides the most detailed and accurate images of the arterial lumen. However, it is an **invasive procedure** associated with risks such as stroke, arterial dissection, contrast nephropathy, and radiation exposure. - Due to its invasiveness and potential complications, DSA is typically reserved for cases with **discordant non-invasive findings** or prior to intervention rather than as a primary screening tool.
Question 23: HU is a measure of
- A. CT (Correct Answer)
- B. MRI
- C. PET
- D. USG
Explanation: ***Correct Answer: CT*** - HU stands for **Hounsfield Units**, a standardized quantitative scale used exclusively in **computed tomography (CT)** to describe the **radiodensity** of tissues based on **X-ray attenuation**. - On this scale, **water is assigned 0 HU**, air is -1000 HU, and dense bone can be +1000 HU or more. - This allows objective measurement and comparison of tissue densities across different CT scanners and examinations. *Incorrect: MRI* - **Magnetic Resonance Imaging (MRI)** does not use Hounsfield Units. - MRI signal intensity is based on the **magnetic properties of tissues** and local hydrogen proton density, not X-ray attenuation. *Incorrect: PET* - **Positron Emission Tomography (PET)** measures the metabolic activity of cells using **radioactive tracers**. - Its output is typically quantified in **Standardized Uptake Value (SUV)**, not Hounsfield Units. *Incorrect: USG* - **Ultrasound (USG)** imaging uses sound waves to create images of internal body structures. - It measures the **acoustic impedance** of tissues and displays findings in terms of echogenicity, not Hounsfield Units.
Question 24: Which of the following appears the same on both T1 and T2 weighted MRI sequences?
- A. Gall bladder
- B. Fat (Correct Answer)
- C. Kidney
- D. CSF
Explanation: ***Fat*** - On both T1 and T2 weighted MRI sequences, fat appears **bright** (high signal intensity). - This consistent bright signal makes fat a useful internal reference point for signal interpretation. *Gall bladder* - The gall bladder is filled with **bile**, which appears bright on T2-weighted images due to its high water content, but can be variable on T1. - Bile does not maintain consistently the **same signal intensity** as fat on both sequences. *Kidney* - The renal parenchyma typically has **intermediate signal intensity** on both T1 and T2, but its signal characteristics are different from the consistently bright signal of fat. - The signal can vary depending on the specific sequence parameters and hydration status, unlike fat. *CSF* - **Cerebrospinal fluid (CSF)** appears dark (low signal) on T1-weighted images and bright (high signal) on T2-weighted images due to its high water content. - This distinct signal intensity difference between T1 and T2 is contrary to the shared bright appearance of fat on both sequences.
Question 25: Which of the following features is used to identify the colon on an X-ray?
- A. Haustra (Correct Answer)
- B. Valvulae conniventes
- C. String of beads sign
- D. More number of loops
Explanation: ***Haustra (Correct Answer)*** - **Haustra** are sacculations or pouches of the colon created by the uneven contraction of the **taeniae coli** - They are THE characteristic feature that helps distinguish the large bowel from the small bowel on an X-ray - These indentations typically do **not cross the entire width** of the bowel lumen, unlike the valvulae conniventes of the small intestine - Haustra appear as incomplete septations on plain radiographs *Valvulae conniventes (Incorrect)* - **Valvulae conniventes** (also known as plicae circulares) are large, circular folds of the **small intestine** mucosa that project into the lumen - They extend **completely across the lumen** of the small bowel, making them easily distinguishable from haustra which only partially traverse the colon - This is a feature of small bowel, not colon *String of beads sign (Incorrect)* - The "**string of beads sign**" is a **pathological radiographic finding** associated with small bowel obstruction - It refers to multiple small, gas-filled loops of small bowel stacked on top of each other, often with small pockets of fluid or air trapped between the folds, resembling beads on a string - This is not a normal anatomical feature used to identify the colon *More number of loops (Incorrect)* - The number of loops is **not a primary distinguishing feature** between the large and small bowel on an X-ray - While the small intestine generally has more convolutions or loops than the colon, this is a **less reliable and specific sign** compared to the presence of haustra - Haustra remain the gold standard feature for colon identification
Question 26: Investigation of choice for studying Renal Cortical mass
- A. 99mTc DTPA
- B. 53Cr Study
- C. 99mTc DMSA (Correct Answer)
- D. 99mTc Pyrophosphate
Explanation: ***99mTc DMSA*** - **99mTc DMSA** (Technetium-99m dimercaptosuccinic acid) is the radiopharmaceutical of choice for imaging the **renal cortex** and assessing **renal cortical mass** and scarring. - It binds preferentially to the cells of the **renal tubules**, allowing for excellent visualization of cortical tissue. *99mTc DTPA* - **99mTc DTPA** (Technetium-99m Diethylenetriaminepentaacetic acid) is primarily used to assess **glomerular filtration rate (GFR)** and renal blood flow. - It is filtered by the **glomeruli** but not reabsorbed or secreted by the tubules, making it suitable for functional studies rather than morphological assessment of cortical mass. *53Cr Study* - **53Cr** (Chromium-51) is used in studies to measure **red blood cell mass**, survival, or gastrointestinal protein loss. - It has no role in the direct assessment of **renal cortical mass** or function. *99mTc Pyrophosphate* - **99mTc Pyrophosphate** is primarily used to evaluate **myocardial infarction** (hot spots) or detect bone lesions. - It is not indicated for, nor does it provide useful information about, **renal cortical mass**.
Question 27: Step ladder pattern of gas shadow is seen in
- A. Intestinal obstruction (Correct Answer)
- B. Gastric outlet obstruction
- C. Duodenal obstruction
- D. Sigmoid volvulus
Explanation: ***Intestinal obstruction*** - A **step-ladder pattern** of gas shadows is a classic radiological sign seen in **small bowel obstruction** due to dilated, fluid-filled loops of small bowel stacked on top of each other. - This pattern results from the accumulation of gas and fluid proximal to the obstruction, causing dilated bowel loops to arrange horizontally. *Gastric outlet obstruction* - This condition primarily results in a **dilated stomach** with fluid and gas, not typically a step-ladder pattern in the small bowel. - Vomiting is usually a prominent symptom, and imaging would show a large fluid-filled stomach. *Duodenal obstruction* - Causes dilatation of the stomach and duodenum, leading to a "**double-bubble sign**" (dilated stomach and proximal duodenum). - It does not typically produce the extensive, stacked small bowel loops seen in a step-ladder pattern. *Sigmoid volvulus* - Characterized by a distinctive large, dilated loop of sigmoid colon, often described as a "**coffee bean sign**" or an **inverted U-shape**. - This is a large bowel obstruction and does not typically present with a step-ladder pattern of small bowel gas.
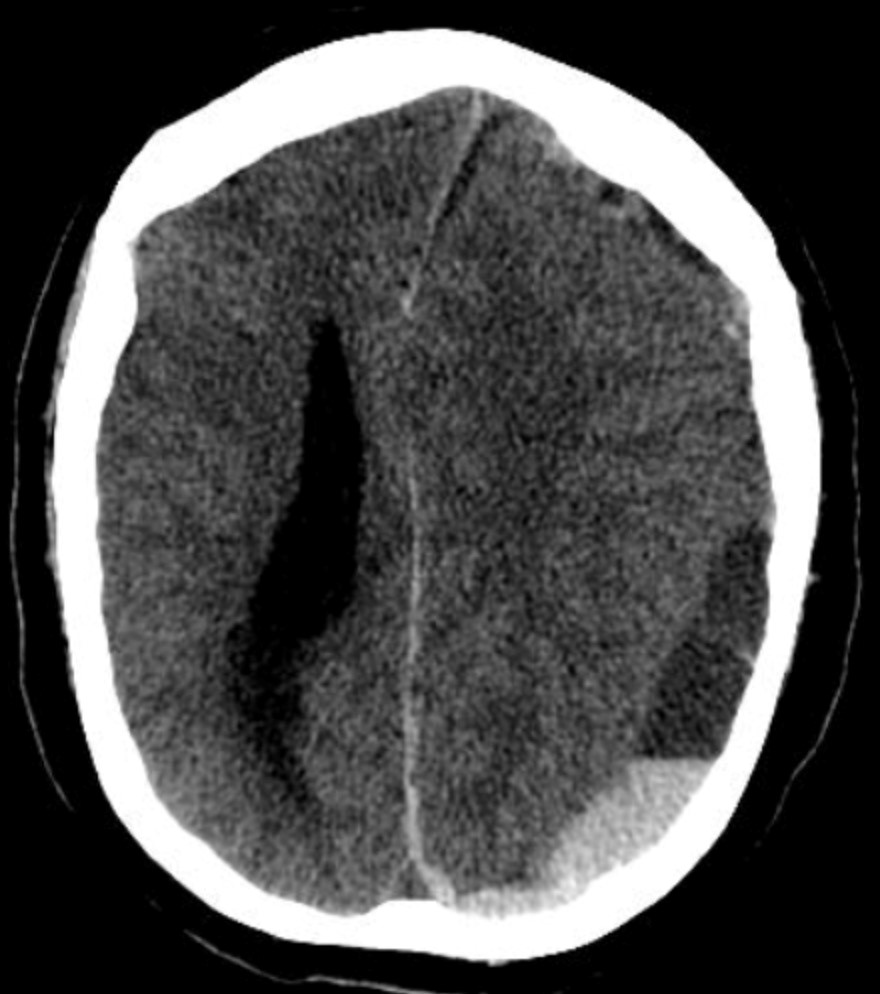
Question 28: A polytrauma patient's CT brain shows a crescent-shaped extra-axial collection with a concave inner margin. What is the most likely diagnosis?
- A. EDH
- B. SDH (Correct Answer)
- C. Contusion
- D. Diffuse axonal injury
Explanation: ***SDH*** - The image shows a **crescent-shaped collection** of hemorrhage with a concave inner margin, consistent with a **subdural hematoma** (SDH). - SDHs result from the tearing of **bridging veins** and typically conform to the brain's surface, crossing suture lines but not limited by bony sutures. *EDH* - An **epidural hematoma (EDH)** characteristically appears as a **lenticular** or **biconvex** shape on CT, not crescent-shaped. - EDHs are typically caused by arterial bleeding, often from the **middle meningeal artery**, and are limited by cranial sutures. *Contusion* - A **contusion** is brain tissue bruising that appears as **heterogeneous areas** of hemorrhage and edema within the brain parenchyma itself. - It would not manifest as a distinct extra-axial collection with a smooth, concave margin. *Diffuse axonal injury* - **Diffuse axonal injury (DAI)** involves widespread microscopic damage to axons, often at the gray-white matter junction. - It may appear as *punctate hemorrhages* or **small lesions** at these junctions on CT, but often the CT can be normal, and it would not present as a large extra-axial collection.
Question 29: The longest half life is that of:
- A. Radon
- B. Uranium (Correct Answer)
- C. Cesium
- D. Radium
Explanation: ***Uranium*** - **Uranium-238**, a common isotope, has an incredibly long half-life of approximately **4.468 billion years**, which is comparable to the age of the Earth. - This extremely long half-life is due to its slow **alpha decay**, making it a very stable radioactive element. *Radon* - **Radon-222** has a relatively short half-life of about **3.8 days**. - Its short half-life makes it a significant indoor air pollutant as it rapidly decays into other radioactive isotopes. *Cesium* - **Cesium-137**, a product of nuclear fission, has a half-life of approximately **30 years**. - While longer than radon, its half-life is much shorter compared to uranium, meaning it decays significantly faster. *Radium* - **Radium-226**, a decay product of uranium, has a half-life of approximately **1,600 years**. - Although much longer than radon and cesium, it is still orders of magnitude shorter than the half-life of uranium-238.