Relapsing Polychondritis - Cartilage Under Siege
- Definition: Episodic, inflammatory disease targeting cartilaginous structures (e.g., ears, nose, larynx, trachea, joints) and other proteoglycan-rich tissues like eyes or aorta.
- Epidemiology: Rare, peak onset 40-60 years, M=F.
- Pathogenesis: Autoimmune; involves cell-mediated and humoral immunity against cartilage antigens like type II collagen and matrilin-1. Strong association with HLA-DR4.
- Results in recurrent chondritis, cartilage destruction, and potential systemic complications.

- Results in recurrent chondritis, cartilage destruction, and potential systemic complications.
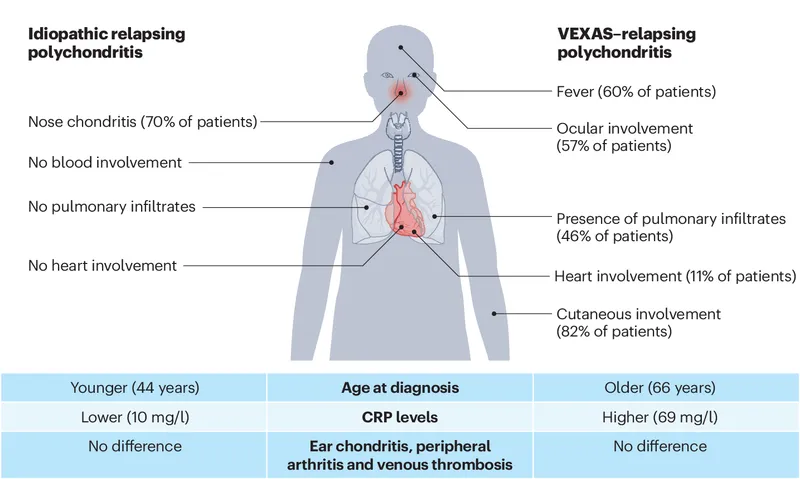
⭐ Relapsing polychondritis can be associated with other autoimmune diseases (e.g., systemic vasculitis, rheumatoid arthritis) or myelodysplastic syndrome (MDS), particularly in elderly individuals.
Relapsing Polychondritis - Ear‑Resistible Signs
📌 Mnemonic: CAN HEAR
- Cardiovascular: Aortitis (aneurysm, dissection), aortic/mitral regurgitation, pericarditis, vasculitis.
- Articular: Asymmetric, non-erosive, migratory oligo- or polyarthritis (sternoclavicular, costochondral joints common).
- Nasal Chondritis: Pain, tenderness, epistaxis, rhinorrhea. Late: saddle-nose deformity.

- Hoarseness/Respiratory Tract: Laryngotracheal-bronchial chondritis: hoarseness, cough, dyspnea, stridor. Severe: subglottic stenosis.
- Eye: Episcleritis (most common ocular), scleritis, uveitis, conjunctivitis, keratitis.
- Auricular Chondritis: Most common. Bilateral pain, swelling, erythema; lobule spared. Recurrence → 'cauliflower ear'.

- Rash/Skin (Cutaneous): Non-specific; aphthae, purpura, nodules, livedo reticularis.
- Additional Key Manifestations:
- Audiovestibular: Sensorineural hearing loss, tinnitus, vertigo.
- Systemic: Fever, malaise, weight loss.
⭐ Bilateral auricular chondritis is the most common (≈90%) and often initial manifestation.
Relapsing Polychondritis - Cartilage Detective Work
- Diagnostic Criteria: 📌 Auricular, Arthritis, Nasal, Ocular, Respiratory, Audiovestibular (AANORA)
Criteria Category Details McAdam's (Need ≥3) Bilateral auricular chondritis; Non-erosive arthritis; Nasal chondritis; Ocular inflammation; Respiratory chondritis; Audiovestibular damage Damiani & Levine's - 3+ McAdam's criteria
- 1+ McAdam's criterion + positive biopsy
- Chondritis in 2+ separate sites + response to steroids/dapsone - Biopsy (Ear/Nose/Respiratory): Chondritis, perichondritis, matrix loss (↓basophilia), fibrosis, +/- calcification. Often not needed if clinically clear.
- Labs: ↑ESR, ↑CRP (acute phase reactants), leukocytosis, anemia (chronic disease), thrombocytosis. Anti-type II collagen Abs, ANCA (some).
- Imaging: CT/MRI (airways), Echo (cardiac).
⭐ Cartilage biopsy is gold standard, but often not needed if clinical criteria met.
Relapsing Polychondritis - Cartilage Care Plan
- Goals: Symptom relief, prevent cartilage deformity, manage systemic complications.
- Treatment Algorithm:
- Mild (auricular/nasal chondritis, arthralgia): NSAIDs, colchicine, dapsone.
- Moderate/Severe (laryngotracheal, ocular, systemic vasculitis, severe chondritis): Systemic corticosteroids (Prednisone 0.5-1 mg/kg/day tapered).
- Steroid-sparing agents: MTX, AZA, MMF. Cyclophosphamide for severe/refractory disease.
- Biologics (evidence evolving): TNF-$\alpha$ inhibitors, Tocilizumab, Rituximab considered.
- Surgical options: Tracheostomy, airway stenting, valve replacement for severe complications.
- Prognosis: Variable; 5-yr survival ~70%, 10-yr ~55%. Worse with airway disease, vasculitis, older age.
⭐ Laryngotracheal involvement is a major cause of mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- Episodic inflammation of cartilaginous tissues: ears, nose, larynx, trachea, joints.
- Auricular chondritis (red, swollen ears, sparing lobules) is a classic sign.
- Laryngotracheal involvement can lead to stridor and airway collapse (life-threatening).
- Common features: saddle-nose deformity, non-erosive arthritis, ocular inflammation, audiovestibular dysfunction.
- Associated with myelodysplastic syndrome (MDS) and other autoimmune diseases.
- Diagnosis: Clinical criteria (McAdam's); biopsy confirms chondritis. Treatment: Steroids, immunosuppressants.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

