Preop Prep - Setting Bones Straight
- Assessment (ABCDE First!):
- Critical AMPLE history (Allergies, Meds, PMH, Last Meal, Events).
- Full exam; document limb neurovascular status.
- Investigations:
- Labs: CBC, Coags (PT/INR, aPTT), Group & X-match.
- Imaging: X-rays, CT (complex #/polytrauma). FAST scan.
- Stabilization:
- Resuscitate: 2 large bore IVs, fluids/blood. Target SBP >90 mmHg, MAP >65 mmHg.
- Hemorrhage control: Pressure, splints, pelvic binder if needed.
- Pain: Multimodal analgesia. Consider early regional blocks.
- Prophylaxis: DVT, Tetanus. Prevent hypothermia. NPO status confirmation.
⭐ For open fractures, administer prophylactic antibiotics (e.g., Cefazolin 1-2g IV) ideally within 1 hour of injury to reduce infection risk.
Intraop Anesthesia - Navigating the Nerves
- Regional Anesthesia (RA) Preferred:
- Benefits: Superior analgesia, ↓blood loss/DVT/PE, ↓opioids, faster rehab.
- Neuraxial: Spinal (rapid), Epidural (catheter for prolonged pain relief).
- PNBs (Ultrasound-Guided): Standard for safety & efficacy.
- Upper Limb: Interscalene, Supraclavicular, Axillary.
- Lower Limb: Femoral, Sciatic, Popliteal, PENG, Adductor Canal.
- General Anesthesia (GA):
- Indications: RA C/I, patient refusal, airway control, prolonged/complex surgery. RSI common.
- Key Nerve Safety:
- Tourniquet: Pain >45-60 min (Max 2 hrs). Monitor for neuropraxia.
- Positioning: Meticulous padding; avoid nerve stretch/compression.
- 📌 LAST: Constant vigilance. Have 20% lipid emulsion ready.
⭐ USG for PNBs: Crucial for ↑success, ↓risk (intraneural/vascular injury).
Key Injury Anesthesia - Fracture Focus Fiesta
-
Core Principles:
-
- ATLS: Airway, Breathing, Circulation.
-
- DCR for hemodynamically unstable.
-
- Early multimodal pain relief (regional blocks).
-
- VTE prophylaxis.
-
-
Key Fractures & Anesthesia:
-
- Pelvic:
-
- Massive hemorrhage risk (MTP).
-
- Associated visceral/vascular injuries.
-
-
- Femur (Shaft):
-
- Blood loss (1-1.5L). High FES risk.
-
- 📌 FES Triad: Respiratory distress, Neurologic signs, Petechial rash.
-
- Early fixation improves outcomes.
-
- Long Bones (General):
-
- Tourniquet: Max ~2 hrs; monitor pain, hemodynamics.
-
- Compartment syndrome: high suspicion, urgent fasciotomy.
-
- Crush Injury:
-
- Risks: Hyperkalemia ($K^+$↑), rhabdomyolysis, AKI.
-
- Manage: IV fluids, mannitol, $NaHCO_3$.
-
⭐ > For suspected major pelvic fractures, apply pelvic binder at greater trochanters; avoid log-rolling if unstable (prevents clot dislodgement).
Postop & Problems - Healing Hurdles Help
- Pain: Multimodal (opioids, NSAIDs, regional blocks/PNBs). Aim: early mobilization, prevent CRPS.
- VTE (DVT/PE): High risk. Prophylaxis: LMWH/DOACs, mechanical. Risk-stratify duration.
- Infection (SSI/Osteomyelitis): Asepsis, prophylactic antibiotics. Rx: Debridement, targeted antibiotics.
- Compartment Syndrome: Vigilance! Fasciotomy if pressure > 30 mmHg or ΔP (Diastolic BP - Compartment Pressure) < 20-30 mmHg.
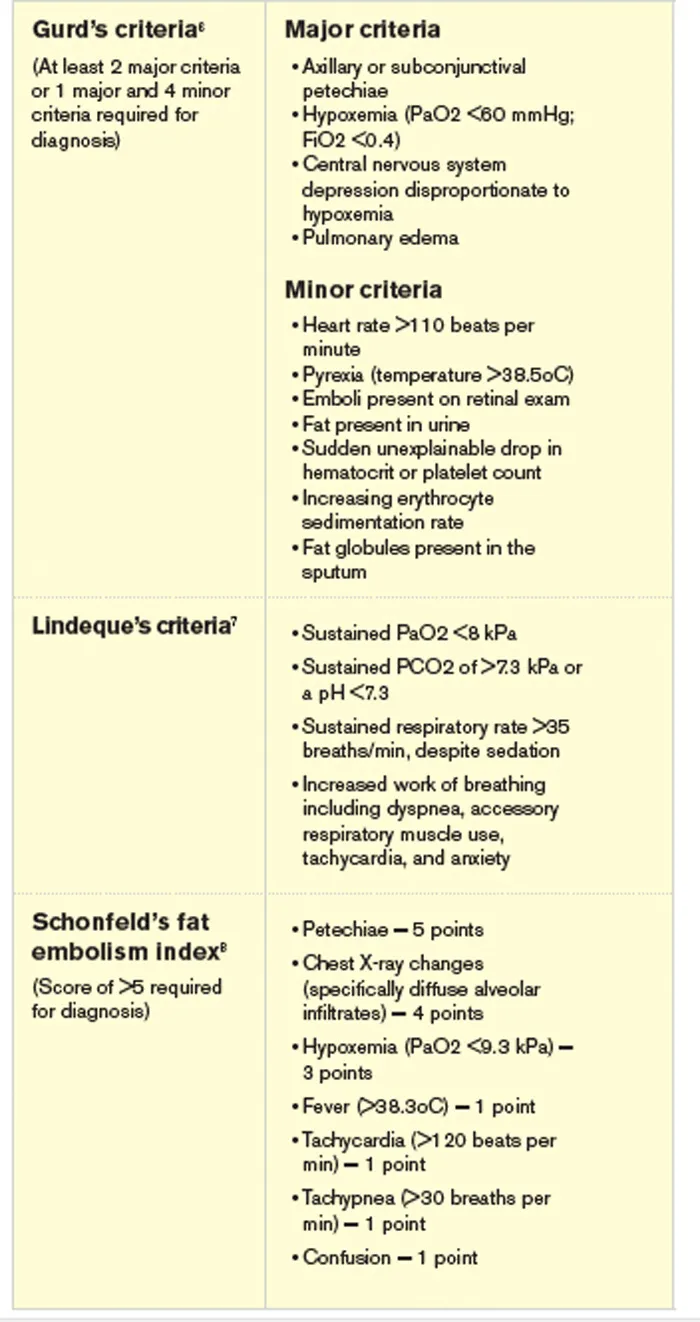
- Fat Embolism Syndrome (FES): Long bone/pelvic #. Gurd's criteria. Supportive. Early fixation ↓ risk.
- Healing Hurdles (Non-union): Address infection, stability, vascularity, smoking.
⭐ For open fractures, antibiotic administration within 1 hour of injury is critical to reduce infection rates, ideally as soon as possible after injury assessment is complete and IV access obtained (Gustilo-Anderson classification influences choice).
High‑Yield Points - ⚡ Biggest Takeaways
- Fat Embolism Syndrome (FES): High risk with long bone/pelvic fractures; watch for hypoxemia, neurological changes, petechial rash.
- Regional Anesthesia: Preferred for pain control & ↓ thromboembolic events if no contraindications (e.g., coagulopathy).
- Damage Control Orthopedics (DCO): Early temporary stabilization in polytrauma, definitive fixation later.
- Tourniquet Management: Max 2 hours inflation; risk of nerve injury, ischemia-reperfusion.
- Tranexamic Acid (TXA): Crucial for ↓ blood loss in major trauma, especially pelvic fractures.
- Hypothermia Prevention: Actively warm to avoid worsening coagulopathy & acidosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more


