Autoimmunity Basics - Tolerance Lost Saga
Autoimmunity: Immune system attack on self-tissues from lost self-tolerance.
- Self-Tolerance: Unresponsiveness to self-antigens.
- Central: Thymus (T-cells), Bone Marrow (B-cells). AIRE gene key for thymic self-Ag expression.
- Peripheral: Secondary lymphoid organs. Anergy, Tregs suppression, deletion. 📌 Tregs Actively Suppress Peripherally.
- Breakdown Mechanisms:
- Molecular Mimicry: Pathogen mimics self.
- Epitope Spreading: Response widens to new self-epitopes.
- Polyclonal B-cell Activation: Non-specific.
- Bystander Activation: Microbe-activated APCs present self-Ag.
- Sequestered Antigens: Released from privileged sites.
- Neoantigens: Altered self-antigens.
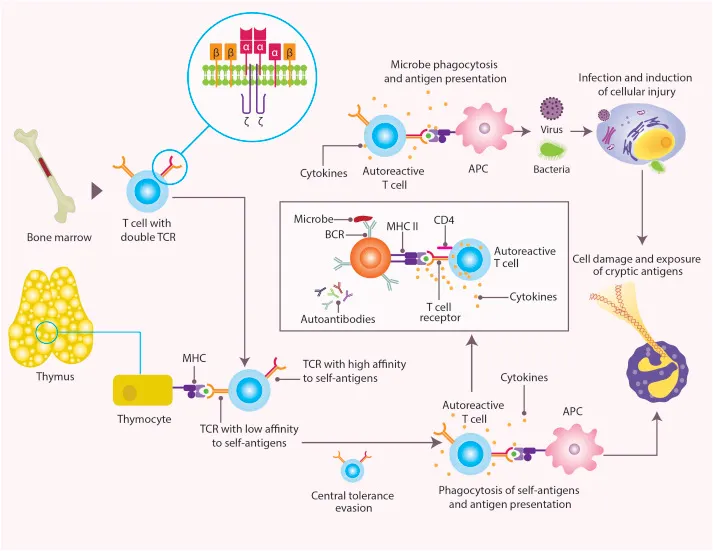
⭐ The AIRE gene is crucial for central tolerance by promoting expression of tissue-specific antigens in the thymus.
Autoimmunity Factors - The Trigger Trio
Key factors contributing to autoimmunity:
- 1. Genetic Susceptibility:
- Gene Polymorphisms: PTPN22, CTLA4, IL-2RA.
- HLA Associations:
HLA Associated Disease(s) Mnemonic 📌 HLA-B27 Ankylosing Spondylitis B27 seronegative spondyloarthropathies HLA-DR3/DR4 Type 1 DM, SLE DR3/4 are bad for pancreas & more HLA-DR4 Rheumatoid Arthritis
⭐ HLA-B27: strong link to ankylosing spondylitis (>90% patients positive).
- 2. Environmental Factors:
- Infections: Group A Strep & Rheumatic Fever (molecular mimicry).
- Drugs: Procainamide & Drug-induced Lupus (alter self-antigens).
- Others: UV radiation, smoking (tissue damage/inflammation).
- 3. Hormonal Factors:
- Estrogen: ↑ influence, may enhance autoimmunity.
- Sex Bias: ↑ prevalence in females (e.g., SLE, RA).
Organ-Specific Diseases - Targeted Trouble
| Disease | Target Organ(s) | Key Autoantibody(ies) | Key Clinical Feature(s) |
|---|---|---|---|
| Hashimoto's Thyroiditis | Thyroid Gland | Anti-TPO, Anti-Tg Abs 📌 HashiMOTo - TPO Ab | Chronic inflammation, hypothyroidism |
| Graves' Disease | Thyroid Gland | Anti-TSHR Ab (TRAb) | Diffuse goiter, hyperthyroidism, exophthalmos |
| Type 1 Diabetes Mellitus | Pancreatic β-cells | Anti-GAD65, Anti-Islet cell (ICA) | Insulin deficiency, hyperglycemia, ketoacidosis risk |
| Myasthenia Gravis | Neuromuscular Junction (NMJ) | Anti-AChR Abs | Fluctuating muscle weakness, ptosis, diplopia |
| Goodpasture's Syndrome | Lungs (alveoli) & Kidneys (GBM) | Anti-GBM Abs (Type IV collagen) | Pulmonary hemorrhage, rapidly progressive glomerulonephritis |
| Pernicious Anemia | Stomach (Parietal cells) | Anti-Intrinsic Factor, Anti-Parietal cell Abs | Vitamin B12 deficiency, megaloblastic anemia, neuropathy |
⭐ In Myasthenia Gravis, antibodies against acetylcholine receptors (AChR) lead to fluctuating muscle weakness, typically worsening with activity and improving with rest.
Systemic Diseases - Body-Wide Battle
Systemic autoimmune diseases involve immune responses against self-antigens, leading to widespread tissue damage across multiple organ systems.
| Disease | Key Autoantibody(ies) | Major Systems Affected | Hallmark Clinical Feature(s) |
|---|---|---|---|
| Systemic Lupus Erythematosus (SLE) | ANA, Anti-dsDNA, Anti-Sm | Skin, joints, kidneys, blood cells, CNS | Malar rash, photosensitivity, arthritis |
| Rheumatoid Arthritis (RA) | RF, Anti-CCP | Joints (synovium), lungs, skin, cardiovascular system | Chronic, symmetric polyarthritis; joint erosions |
| Sjögren's Syndrome | Anti-Ro/SSA, Anti-La/SSB | Exocrine glands (salivary, lacrimal), joints, lungs | Dry eyes (keratoconjunctivitis sicca), dry mouth (xerostomia) |
| Systemic Sclerosis (Scleroderma) | Anti-Scl-70 (topoisomerase I), Anti-centromere | Skin, lungs, GI tract, kidneys, heart | Skin fibrosis, Raynaud's phenomenon |
| Polymyositis/ Dermatomyositis | Anti-Jo-1, Anti-Mi-2 | Muscles, skin (DM), lungs | Proximal muscle weakness; Gottron's papules, heliotrope rash (DM) |
⭐ Anti-dsDNA and Anti-Sm antibodies are highly specific for Systemic Lupus Erythematosus (SLE).
📌 Remember SLE features with "SOAP BRAIN MD" (Serositis, Oral ulcers, Arthritis, Photosensitivity, Blood disorders, Renal involvement, ANA, Immunologic disorders, Neurologic disorder, Malar rash, Discoid rash).
High‑Yield Points - ⚡ Biggest Takeaways
- Autoimmunity is a failure of self-tolerance, leading to immune reactions against self-antigens.
- Molecular mimicry (e.g., Rheumatic fever after Strep infection) is a key pathogenic mechanism.
- Strong HLA association is common: HLA-B27 (Ankylosing Spondylitis), HLA-DR3/DR4 (Type 1 DM, RA).
- Systemic Lupus Erythematosus (SLE) is a prototypical systemic autoimmune disease with ANA and anti-dsDNA antibodies.
- Organ-specific examples include Hashimoto's thyroiditis (anti-TPO) and Myasthenia Gravis (anti-AChR).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

