Introduction to DDF - Pixel Perfect ID
- Digital Dental Forensics (DDF): Application of digital imaging & software in dental identification.
- Scope:
- Human identification (mass disasters, missing persons).
- Age estimation (digital analysis of dental development).
- Bite mark analysis (digital comparison).
- Dental malpractice investigation.
- Advantages:
- Objective & reproducible results.
- Non-invasive/minimally invasive techniques.
- Efficient data storage, retrieval & sharing.
- Enhanced visualization & comparison.
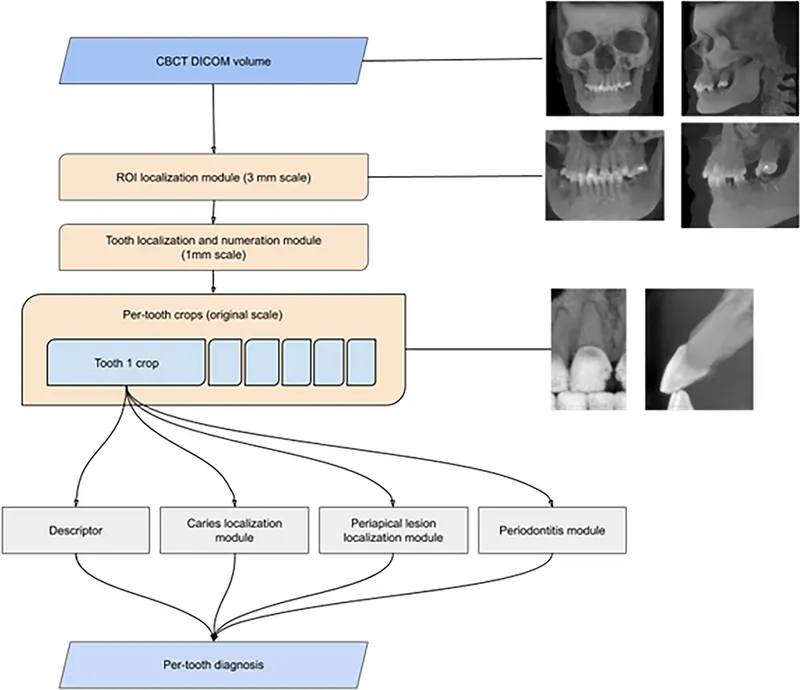
⭐ Key Advantage: DDF significantly reduces subjectivity in dental comparisons, offering quantifiable data for identification, especially with AM/PM (ante-mortem/post-mortem) radiograph comparisons using software overlays and metric analysis. This is crucial in mass casualty incidents (MCIs).
Digital Modalities & Tools - Scans, Slices & Software
- Digital Scanners:
- Intraoral Scanners (IOS): Rapid, direct 3D digital impressions.
- Cone Beam CT (CBCT): Key for 3D craniofacial imaging; relatively low radiation, high accuracy for bony structures.
- Applications: Identification, trauma analysis, age estimation support.
- Computed Tomography (CT): Superior soft tissue contrast, higher radiation dose.
- Surface Scanners (Laser/Structured Light): Non-contact 3D scanning of casts, bite marks, prostheses.
- Image Data & Slices:
- DICOM (Digital Imaging and Communications in Medicine): Universal standard format, ensuring interoperability.
- Multi-planar Reconstruction (MPR): Axial, sagittal, coronal views from volumetric data.
- 3D Volume Rendering: Visualizing complex anatomical structures.
- Software Tools:
- Image Analysis: Adobe Photoshop, ImageJ (measurements, enhancement, digital superimposition).
- CAD/CAM & 3D Analysis: Dolphin Imaging, Invivo, OsiriX (3D modeling, virtual autopsy, comparative analysis).
- Forensic Specific: PlassData, WinID3, DVI System Int. (Automated AM/PM dental record matching).
⭐ CBCT is pivotal for 3D dental reconstructions from remains, crucial for identification.
💡 DICOM viewers (e.g., OsiriX Lite, RadiAnt) are essential for initial case assessment.
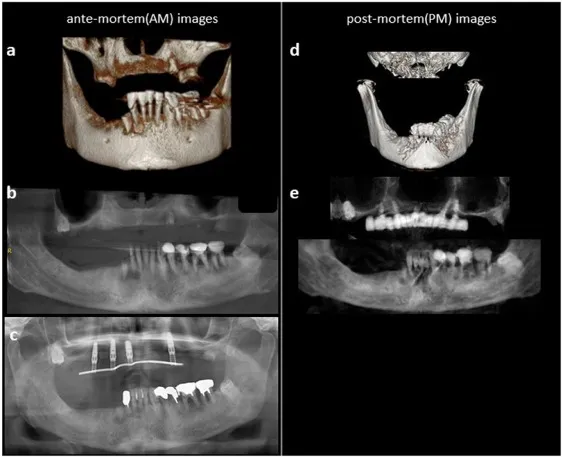
Applications in Identification - Digital Evidence Unveiled
- Comparative Dental Identification (CDI):
- Core method: Matching digital ante-mortem (AM) with post-mortem (PM) dental data.
- Key Technologies:
- Digital Radiography: Intraoral X-rays, OPGs, crucial Cone Beam CT (CBCT) for 3D views.
- Intraoral & Facial Scanners: Generate accurate 3D digital models of teeth and jaws.
- Software Assistance: For image enhancement, superimposition (e.g., Adobe Photoshop, specialized tools), feature matching, and geometric analysis.
- Disaster Victim Identification (DVI):
- Specialized software (e.g., WinID3, PlassData, CapMI).
- Streamlines rapid data entry, automated primary matching suggestions, and efficient management of multiple victims' records.
- Digital records must follow INTERPOL DVI guidelines.
- Digital Bite Mark Analysis:
- Objective documentation using 3D scanning of bite marks (on victims/objects) and suspect's dentition.
- Advanced digital overlay techniques and precise metric analysis.
- Aims for ↑objectivity, ↑reproducibility, and ↓distortion compared to traditional methods.
⭐ CBCT provides distortion-free 3D images, crucial for complex superimpositions in identification and detailed analysis of bite mark morphology, enhancing reliability.
- Age Estimation Adjuncts:
- Software-aided digital analysis of radiographs for dental development stages (e.g., Demirjian's method, Willems method).
- Calculation of pulp-to-tooth volume ratios from digital images (e.g., Kvaal's method).
- Digital Evidence & Legal Aspects:
- Critical: Secure acquisition, tamper-proof storage, and verifiable chain of custody for all digital files.
- Admissibility in court: While BSA Section 65B remains relevant for electronic records, the broader legal landscape includes the Information Technology Act, 2000 (digital signatures, cybercrimes), and evolving Supreme Court jurisprudence on digital evidence integrity, authenticity, and chain of custody requirements.

High‑Yield Points - ⚡ Biggest Takeaways
- CBCT (Cone Beam Computed Tomography) is crucial for 3D imaging in identification and age estimation.
- Intraoral scanners provide accurate digital dental models for comparison and identification.
- CAD/CAM technology aids in superimposition, facial reconstruction, and matching prosthetics.
- Digital radiography offers enhanced image quality, reduced radiation, and easier data management.
- Specialized software enables automated comparison of ante-mortem (AM) and post-mortem (PM) dental records.
- Digital analysis of tooth metrics (like pulp/tooth ratio) aids objective age determination.
- 3D imaging and digital overlays improve objectivity in bite mark analysis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

