Asphyxial Deaths

On this page
🗺️ The Asphyxial Landscape: Death's Oxygen Crisis
Asphyxia represents a final common pathway where oxygen delivery fails catastrophically, triggering a predictable cascade from consciousness to cardiac arrest within 3-5 minutes. Understanding asphyxial deaths requires mastering not just the mechanism of oxygen deprivation, but the specific anatomical signatures each method inscribes on tissues. The forensic pathologist must distinguish between 12 major categories, each with distinct patterns of injury, postmortem findings, and medicolegal implications.
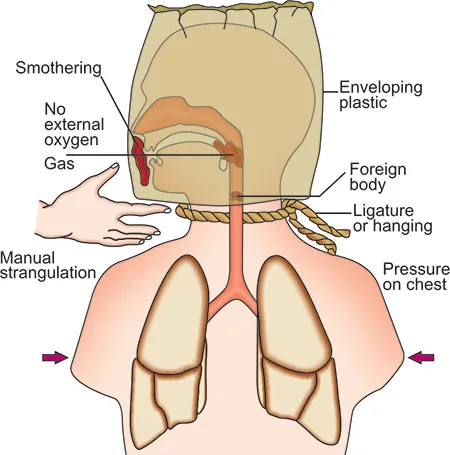
The Oxygen Deprivation Spectrum
Asphyxia disrupts oxygen delivery through four fundamental mechanisms, each producing characteristic clinical and postmortem findings:
- Anoxic Asphyxia - Environmental oxygen depletion
- Confined spaces with O₂ <16% (normal 21%)
- Carbon monoxide displacing oxygen (COHb >50% lethal)
- Cyanide blocking cytochrome oxidase (2-3 mg/kg fatal)
- Hydrogen sulfide paralyzing respiratory centers (>500 ppm rapidly fatal)
- Hypoxic Asphyxia - Airway obstruction preventing oxygen entry
- Smothering with complete airway occlusion
- Choking with foreign body (most common: food bolus 65% of cases)
- Drowning with fluid-filled airways
- Suffocation in plastic bags or enclosed spaces
- Stagnant Asphyxia - Circulatory failure despite adequate oxygen
- Hanging with vascular neck compression
- Strangulation (ligature 80% homicidal, manual 90% homicidal)
- Traumatic asphyxia with thoracic compression >500 kg force
- Positional asphyxia restricting chest expansion
- Histotoxic Asphyxia - Cellular inability to utilize oxygen
- Cyanide poisoning (blood cyanide >3 mcg/mL fatal)
- Hydrogen sulfide toxicity
- Methemoglobinemia (>70% MetHb lethal)
📌 Remember: CHOPS for asphyxia mechanisms - Chemical (toxins), Hypoxic (airway), Obstructive (circulation), Positional (mechanics), Stagnant (blood flow). Each letter represents a distinct pathophysiological route to oxygen deprivation, guiding your differential diagnosis from scene investigation through autopsy.
Classic Asphyxial Signature: The Tardieu Spots Story
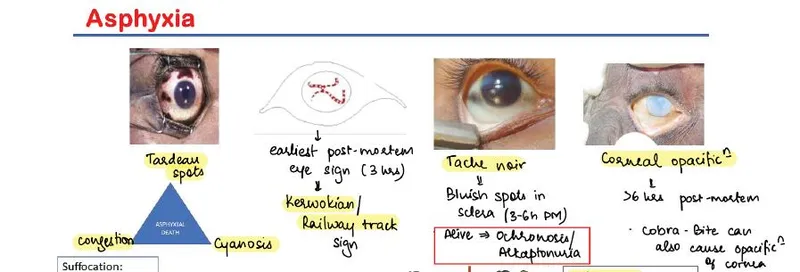
The classical signs of asphyxia represent acute vascular responses to hypoxia and elevated venous pressure, though their presence varies significantly by mechanism:
-
Petechial Hemorrhages (Tardieu Spots)
- Conjunctival petechiae: Present in 60-80% of strangulation cases
- Facial petechiae: More common in ligature (70%) than manual strangulation (40%)
- Visceral petechiae: Thymus (85% in infants), epicardium (60%), lungs (75%)
- Mechanism: Capillary rupture from venous back-pressure >50 mmHg
- Absent in rapid deaths (<30 seconds) and drowning (<20% of cases)
-
Cyanosis and Congestion
- Facial plethora with dark purple discoloration
- Neck vein engorgement (JVP elevated >15 cm H₂O)
- Tongue protrusion and cyanosis in hanging (40% of cases)
- Ears and lips dusky blue (arterial O₂ saturation <75%)
-
Fluidity of Blood
- Postmortem blood remains fluid in >90% of asphyxial deaths
- Mechanism: Hypoxia prevents fibrinogen conversion
- Contrast with clotted blood in cardiac deaths (70% show clots)
- Forensic value: Allows postmortem chemistry and toxicology
⭐ Clinical Pearl: The "asphyxial triad" (petechiae + cyanosis + fluid blood) appears in only 35-40% of confirmed asphyxial deaths. Its absence never excludes asphyxia, but its presence strongly suggests prolonged venous obstruction with survival >45-60 seconds before death. Rapid asphyxiation (drowning, chemical) rarely produces classical signs.
The Medicolegal Classification Matrix
| Asphyxia Type | Typical Manner | Key Autopsy Finding | Scene Evidence | Survival Time | Petechiae Frequency |
|---|---|---|---|---|---|
| Hanging | Suicide 85% | Oblique ligature mark | Suspension point | 5-15 min | 60-70% |
| Ligature Strangulation | Homicide 80% | Horizontal ligature mark | Struggle signs | 4-7 min | 70-80% |
| Manual Strangulation | Homicide 90% | Fingernail abrasions | Defense injuries | 3-5 min | 40-50% |
| Smothering | Homicide 60% | Minimal external signs | Pillow/cloth fibers | 2-4 min | 20-30% |
| Drowning | Accident 70% | Foam in airways | Wet clothing | 3-8 min | <20% |
| Choking | Accident 95% | Foreign body in airway | Food/object nearby | 1-3 min | <10% |
💡 Master This: Manner of death determination in asphyxia depends on the constellation of scene findings, injury patterns, and victim history-never a single autopsy finding. Hanging with feet touching ground ("partial hanging") accounts for 30% of suicidal hangings. Ligature strangulation requires sustained force for 10-15 seconds to produce unconsciousness, making accidental death virtually impossible in adults.
The Timeline of Asphyxial Death
Understanding the temporal progression from oxygen deprivation to irreversible brain death guides both clinical resuscitation and forensic interpretation:
⭐ Clinical Pearl: The "5-minute rule" defines the critical window for neurologically intact survival after complete oxygen deprivation. Brain injury begins at 3 minutes (hippocampal CA1 neurons most vulnerable), becomes irreversible at 5 minutes in normothermia, extends to 15-20 minutes in hypothermia (<30°C). This explains why cold-water drowning victims tolerate longer submersion times with better outcomes.
Connect the foundational understanding of asphyxial mechanisms through the cellular and biochemical chaos detailed in , where the molecular cascade from hypoxia to cell death reveals why different asphyxial methods produce varying survival times and injury patterns.
🗺️ The Asphyxial Landscape: Death's Oxygen Crisis
📚 Suffocation Secrets: When Air Cannot Reach
Suffocation encompasses any mechanism preventing atmospheric oxygen from reaching the alveoli, excluding neck compression. This category includes smothering, choking, traumatic asphyxia, positional asphyxia, and environmental oxygen depletion-each writing distinct signatures despite the shared final pathway. Master suffocation patterns, and you distinguish intentional homicide from tragic accident in 65% of pediatric asphyxial deaths and 40% of custody-related deaths.

Smothering: The Silent Killer
Smothering involves external occlusion of nose and mouth, producing minimal external evidence despite violent struggle. This discrepancy between force required and visible injury makes smothering diagnosis particularly challenging:
-
External Findings (Often Subtle)
- Perioral abrasions or contusions: Present in only 35-40% of cases
- Fingernail crescents on cheeks or neck: 25-30% of cases
- Lip frenulum tears: Rare (<5%), more common in infants
- Nasal bone fractures: <10% unless extreme force used
- Key forensic challenge: 60-70% of smothering victims show NO external injury
-
Internal Findings (More Reliable)
- Petechiae in conjunctivae: 60-75% of cases with survival >90 seconds
- Intramuscular neck hemorrhages: 40% from struggling against restraint
- Pulmonary congestion and edema: Universal (>95%)
- Visceral petechiae (heart, thymus, lungs): 70-80% in prolonged smothering
- Foreign material in airways: Fibers from pillow/cloth in 30%
📌 Remember: PILLOW for smothering evidence - Petechiae (conjunctival), Internal hemorrhages (neck muscles), Lip injuries (frenulum), Lung edema (congestion), Oral abrasions (perioral), Witness statements (scene reconstruction). The absence of external injury never excludes smothering; internal findings and scene investigation provide the diagnosis.
Choking: The Café Coronary
Choking from airway foreign bodies produces the "café coronary"-sudden collapse during eating mimicking cardiac arrest. This accounts for approximately 5,000 deaths annually in the United States, with 65% involving food boluses:
-
High-Risk Victim Profile
- Elderly with poor dentition: 40% of adult choking deaths
- Alcohol intoxication: Present in 35-45% of adult cases
- Neurological impairment: Parkinson disease, stroke in 25%
- Children <5 years: 60% of pediatric choking deaths
- Mental disability: Overrepresented in 20% of cases
-
Common Foreign Bodies by Age
- Adults: Meat bolus (50%), bread/rice (15%), bones (10%)
- Children 1-3 years: Grapes, hot dogs, nuts (70% combined)
- Infants <1 year: Small toys, coins, balloons (65%)
- Elderly: Poorly chewed meat, dentures (55%)
-
Autopsy Findings
- Foreign body in larynx/trachea: Location determines survival time
- Laryngeal obstruction: Death in 1-2 minutes
- Tracheal obstruction: Death in 2-4 minutes
- Bronchial obstruction: May survive >10 minutes with partial airway
- Petechiae: Rare (<10%) due to rapid death
- Abrasions in pharynx: From retrieval attempts in 40%
⭐ Clinical Pearl: The "Heimlich scar" refers to xiphoid process fracture or upper abdominal bruising in 15-20% of successful abdominal thrust maneuvers. Its presence confirms choking event but doesn't indicate cause of death if resuscitation failed. Conversely, absence doesn't exclude choking-many victims die before intervention attempted.
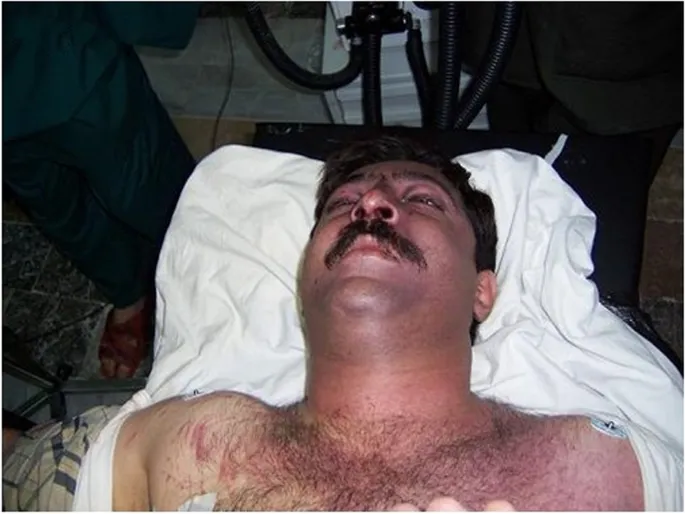
Traumatic Asphyxia: The Crush Syndrome
Traumatic asphyxia results from sudden severe thoracoabdominal compression, forcing blood from right heart into valveless head and neck veins, producing pathognomonic findings:
-
Classic Presentation: The Perthes Sign
- Intense facial cyanosis with sharp demarcation at clavicles
- Petechiae covering face, neck, upper chest: "Mask of ecchymoses"
- Subconjunctival hemorrhages: Universal (100%) when conscious during compression
- Epistaxis and hemoptysis: Common (60-70%)
- Neurological deficits: Temporary blindness in 40%, seizures in 25%
-
Mechanism Requirements
- Compressive force: >500 kg applied to thorax
- Glottis closure: Victim must be conscious initially (reflex glottic closure)
- Rapid compression: <2 seconds produces maximal vascular effects
- Duration: >2-3 minutes required for fatal outcome
- Examples: Crowd crush (30%), vehicle vs pedestrian (25%), industrial accidents (20%)
-
Internal Findings
- Rib fractures: Present in 85%, multiple bilateral fractures
- Pulmonary contusions: >90% show hemorrhagic consolidation
- Cardiac contusions: 40% with troponin elevation
- Hepatic lacerations: 60% from compression against spine
- Survival possible if compression released within 3-4 minutes
💡 Master This: Traumatic asphyxia victims who survive initial compression often develop ARDS within 24-48 hours (incidence 40-50%) and may show persistent neurological deficits from cerebral venous infarction. The dramatic facial appearance (cyanosis, petechiae) typically resolves within 7-10 days, but retinal hemorrhages may cause permanent vision loss in 10-15% of survivors.
Positional Asphyxia: The Restraint Tragedy
Positional asphyxia occurs when body position prevents adequate chest expansion or diaphragmatic movement, most commonly in restraint situations:
-
High-Risk Positions
- Prone maximal restraint: Hands cuffed behind back, pressure on upper back
- Hog-tie position: Ankles bound to wrists behind back (Fatal in >5 minutes)
- "Hobble" restraint: Ankles bound, forced into squad car (Risk increases 400%)
- Inverted suspension: Head-down position (autoerotic accidents, entrapment)
- Seated compression: Obese individuals in confined spaces
-
Contributing Risk Factors
- Obesity: BMI >40 increases risk 800%
- Stimulant intoxication: Cocaine/methamphetamine in 60% of custody deaths
- Struggle/exertion: Increases O₂ demand 500%, depletes reserves
- Multiple restrainers: Weight on back/chest in 80% of fatal cases
- Excited delirium: Present in 70% of restraint-related deaths
-
Autopsy Findings (Characteristically Minimal)
- No specific pathognomonic findings (diagnosis of exclusion)
- Petechiae: Rare (<15%) due to absence of venous obstruction
- Visceral congestion: Non-specific, present in 70%
- Toxicology: Stimulants detected in 60%, alcohol in 40%
- Restraint marks: Wrist/ankle ligature marks in 90%
⭐ Clinical Pearl: Positional asphyxia deaths typically occur 5-15 minutes after restraint application, often after struggling ceases. The "quiet period" before death represents exhaustion and respiratory failure, NOT cooperation. Survival requires position change within 10 minutes in high-risk individuals. Never transport restrained subjects prone-lateral position maintains airway and allows chest expansion.
Explore the specific vulnerabilities and diagnostic challenges of young victims through , where developmental anatomy and non-verbal victims create unique investigative challenges requiring specialized forensic approaches.
📚 Suffocation Secrets: When Air Cannot Reach
🔬 Hanging & Strangulation: The Neck Compression Quartet
Neck compression deaths divide into four mechanistically distinct categories: hanging, ligature strangulation, manual strangulation, and mugging strangulation-each producing characteristic injury patterns that reveal manner of death in >85% of cases. Understanding the biomechanics of neck compression transforms subtle ligature marks and internal hemorrhages into definitive evidence distinguishing suicide from homicide.
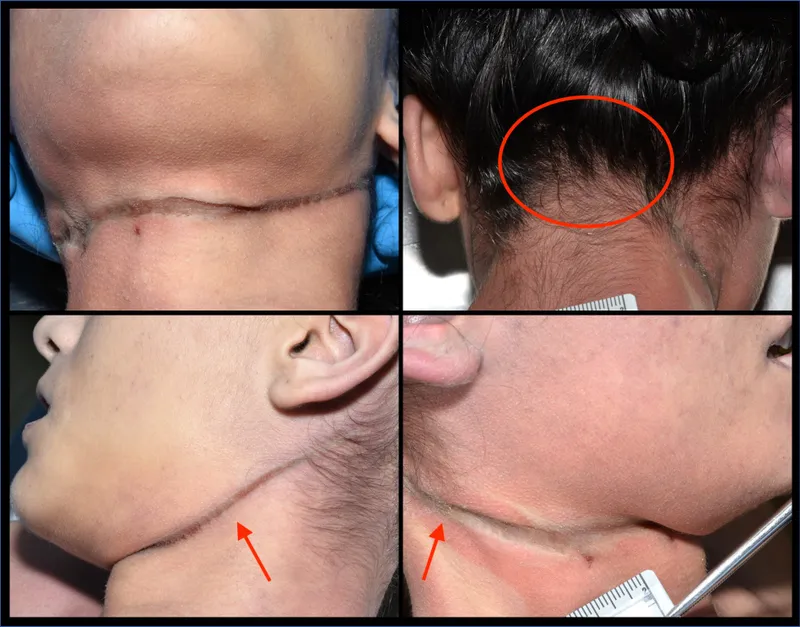
Hanging: The Suspension Story
Hanging involves neck compression from body weight suspended by ligature, producing death through multiple mechanisms operating simultaneously. The forensic pathologist must distinguish typical (knot location matters) from atypical hanging, and complete from partial suspension:
-
Suspension Biomechanics
- Complete suspension: Body entirely suspended (Only 30% of suicidal hangings)
- Partial suspension: Part of body supported (70% of cases, may involve kneeling/sitting)
- Required force: Only 2-3 kg pressure occludes jugular veins
- 15 kg occludes carotid arteries (achieved with partial suspension)
- >30 kg occludes vertebral arteries and compresses trachea
- Consciousness lost: 10-15 seconds from carotid occlusion
- Death time: 5-15 minutes depending on mechanism dominance
-
The Ligature Mark Signature
- Oblique orientation: Rises toward suspension point (Pathognomonic for hanging)
- Incomplete: Gap at suspension point in 60% of cases
- Above thyroid cartilage: Typically at hyoid bone level or higher
- Depth variation: Deepest opposite suspension point, shallow near knot
- Parchment-like: Dry, yellow-brown appearance from antemortem pressure
- Width matches ligature: Narrow rope (<1 cm) vs broad ligature (>3 cm)
📌 Remember: LIGATURE distinguishes hanging from strangulation marks - Location (high, above thyroid), Incomplete (gap present), Gradient (depth variation), Angle (oblique upward), Texture (parchment-like), Uniform (single mark), Rope width (matches ligature), Elevation (rises to suspension point). Horizontal marks below thyroid suggest homicidal ligature strangulation, not hanging.
- Internal Neck Findings in Hanging
- Hyoid bone fracture: 25-35% of cases (Increases with age >40 years)
- Thyroid cartilage fracture: 15-20%, superior horns most common
- Carotid intimal tears: Rare (<5%), indicates extreme force
- Strap muscle hemorrhage: 40-60%, suggests antemortem hanging
- Spinal injuries: C2-C3 subluxation in judicial hanging, rare in suicidal
⭐ Clinical Pearl: The "Sydney Furrow" describes the classic oblique hanging mark, but 20-25% of confirmed hangings show no visible ligature mark due to soft/broad ligatures (bedsheets, clothing) or very brief suspension. Internal neck dissection revealing muscle hemorrhage confirms antemortem hanging even without external marks. Conversely, ligature marks can form postmortem if body remains suspended >2-3 hours.
Ligature Strangulation: The Homicidal Hallmark
Ligature strangulation involves neck compression by constricting band tightened by force other than body weight, representing homicide in 80% of cases:
-
Ligature Mark Characteristics
- Horizontal orientation: Encircles neck at thyroid cartilage level
- Complete: Typically 360° circumference (no gap)
- Below hyoid: Usually at mid-thyroid level, lower than hanging
- Uniform depth: Consistent pressure around entire circumference
- Multiple marks: Present in 40% from repeated applications or slippage
- Knot location: Posterior in 65% (attacker behind victim)
-
Mechanism and Force Requirements
- Sustained pressure: Requires 4-5 kg force maintained >10-15 seconds
- Consciousness: Lost after 10-15 seconds of carotid occlusion
- Struggle phase: 20-40 seconds of convulsive movements
- Respiratory arrest: 1-2 minutes after application
- Cardiac arrest: 3-5 minutes total strangulation time
- Impossible to self-inflict: Loss of consciousness prevents sustained pressure
-
Associated Injuries (Homicidal Indicators)
- Defense wounds: Present in 70% (hands, forearms)
- Facial injuries: Blunt trauma in 60% from struggle/assault
- Fingernail marks: On neck in 40% from victim's attempts to remove ligature
- Genital trauma: Sexual assault in 35% of female victims
- Binding marks: Wrists/ankles bound in 45% of cases
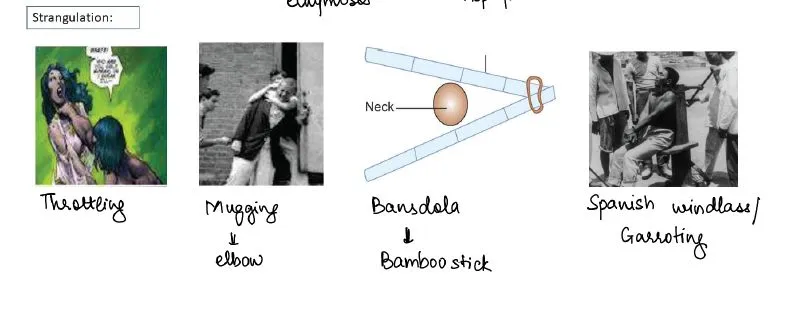
Manual Strangulation: The Intimate Violence
Manual (throttling) strangulation involves neck compression by hands/forearms, representing homicide in >90% of cases and often indicating intimate partner violence:
-
External Neck Findings
- Fingernail abrasions: Crescentic marks in 60-80% of cases
- Fingertip bruises: Circular contusions 1-2 cm diameter
- Pattern: Thumb marks anterior, finger marks posterior (face-to-face)
- Bilateral asymmetry: Dominant hand produces deeper injuries
- Perioral petechiae: Present in 40% from venous obstruction
- Conjunctival petechiae: 70-80%, bilateral and profuse
-
Internal Neck Injuries (More Severe Than Hanging)
- Hyoid fracture: 50-75% (significantly higher than hanging)
- Thyroid cartilage fracture: 40-50%, bilateral superior horns
- Strap muscle hemorrhage: >90%, extensive bilateral
- Laryngeal hemorrhage: 60%, vocal cord petechiae
- Carotid sheath hemorrhage: 30%, indicates extreme force
💡 Master This: Manual strangulation requires sustained compression for 4-5 minutes to cause death, making accidental death virtually impossible in adults. The extensive internal injuries (hyoid fracture, muscle hemorrhage) develop from repeated compression/release cycles during struggle. Delayed death (hours to days later) occurs in 10-15% due to laryngeal edema or carotid thrombosis-always hospitalize assault victims for 24-48 hour observation.
- Victim-Perpetrator Dynamics
- Intimate partner violence: >70% of female victims
- Face-to-face position: 85% of cases (frontal approach)
- Conscious time: 20-30 seconds before loss of consciousness
- Survival possible: If released before 2-3 minutes of compression
- Repeat attempts: Evidence of prior strangulation in 50% of intimate partner homicides
⭐ Clinical Pearl: The "choking game" or "pass-out challenge" involves adolescent self-strangulation for euphoria, accounting for 250-1,000 deaths annually. These deaths mimic suicidal hanging but occur in seated/standing positions with ligature around neck and no suspension point. Scene investigation reveals videos, social media references, and prior attempts in 40%. Distinguish from autoerotic asphyxia by absence of sexual paraphernalia.
| Feature | Hanging | Ligature Strangulation | Manual Strangulation | Mugging Strangulation |
|---|---|---|---|---|
| Manner | Suicide 85% | Homicide 80% | Homicide 90% | Homicide 95% |
| Mark Location | High (hyoid level) | Mid (thyroid level) | Variable/absent | Low (cricoid level) |
| Mark Pattern | Oblique, incomplete | Horizontal, complete | Fingernail crescents | Horizontal, arm width |
| Hyoid Fracture | 25-35% | 30-40% | 50-75% | 15-25% |
| Petechiae | 60-70% | 70-80% | 70-80% | 50-60% |
| Time to Death | 5-15 min | 3-5 min | 4-6 min | 2-4 min |
The distinct patterns of neck compression deaths connect through shared pathophysiology detailed in , where understanding the cellular consequences of hypoxia explains why different compression mechanisms produce varying survival times and injury severity.
🔬 Hanging & Strangulation: The Neck Compression Quartet
🏥 Drowning: The Aquatic Asphyxia
Drowning represents death from liquid aspiration into airways, causing asphyxia through alveolar flooding and surfactant washout. This mechanism produces >320,000 deaths globally each year, with 90% occurring in freshwater and 70% classified as accidental. Master drowning pathophysiology and autopsy findings, and you distinguish true drowning from bodies disposed in water postmortem-a critical determination affecting 35% of drowning investigations.
Drowning Definitions: The Utstein Clarity
The 2002 World Congress on Drowning standardized terminology, eliminating confusing classifications (wet/dry, primary/secondary) that plagued forensic interpretation:
-
Drowning: Process of respiratory impairment from submersion/immersion in liquid
- Fatal drowning: Death within 24 hours of drowning event
- Non-fatal drowning: Survival beyond 24 hours (previously "near-drowning")
- Submersion: Entire body including airway underwater
- Immersion: Face/airway in liquid, body not necessarily submerged
-
Eliminated Terms (No Longer Used)
- "Wet drowning": All drowning involves liquid aspiration (85-90% of cases)
- "Dry drowning": Laryngospasm without aspiration (10-15%, still true drowning)
- "Secondary drowning": Delayed death now termed "complications of non-fatal drowning"
- "Near-drowning": Replaced by "non-fatal drowning" for clarity
📌 Remember: DROWN for drowning pathophysiology sequence - Dive reflex (initial breath-hold), Respiratory distress (struggle phase), Open airway (involuntary inspiration), Water aspiration (alveolar flooding), Neurological injury (hypoxic brain damage). This 3-8 minute sequence explains why immediate rescue within 5 minutes offers 50% survival chance, dropping to <10% after 10 minutes submersion.
The Drowning Sequence: From Panic to Unconsciousness
Understanding the temporal progression from submersion to death guides resuscitation efforts and forensic timeline reconstruction:
-
Phase 1: Voluntary Breath-Hold (0-60 seconds)
- Initial panic and struggle to surface
- Dive reflex in cold water: Bradycardia, peripheral vasoconstriction
- Trained swimmers: Breath-hold >90 seconds possible
- Children: Shorter tolerance <30 seconds typical
-
Phase 2: Involuntary Inspiration (1-2 minutes)
- CO₂ buildup overrides voluntary control
- First gasp aspirates water into airways
- Wet drowning (85-90%): Continued aspiration of fluid
- Dry drowning (10-15%): Laryngospasm prevents aspiration
-
Phase 3: Loss of Consciousness (2-4 minutes)
- Hypoxia produces unconsciousness
- Laryngospasm relaxes (in dry drowning)
- Passive aspiration continues
- Convulsions common (60% of witnessed drownings)
-
Phase 4: Cardiac Arrest (3-8 minutes)
- Severe hypoxia triggers dysrhythmias
- Ventricular fibrillation in 50%
- Asystole in remaining 50%
- Brain death begins at 5 minutes (normothermia)
⭐ Clinical Pearl: The "cold water drowning exception" allows neurologically intact survival after submersion >20-30 minutes when water temperature <10°C. Hypothermia reduces cerebral metabolic rate by 50% per 10°C drop, extending viable resuscitation window. The youngest documented survivor: 66 minutes submersion at 5°C (age 2 years). Never pronounce cold-water drowning victim dead until rewarmed to >32°C.
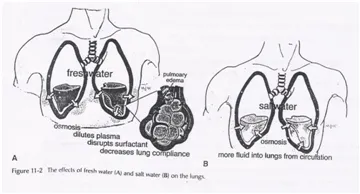
Freshwater vs Seawater: The Physiological Divide
The tonicity difference between aspirated fluid and plasma produces distinct pathophysiological cascades, though forensic distinction proves difficult:
-
Freshwater Drowning (Hypotonic Aspiration)
- Rapid alveolar absorption: 3 mL/kg/min into circulation
- Hemodilution: Plasma osmolality drops 15-20 mOsm/kg
- Hemolysis: Occurs with aspiration >11 mL/kg (rarely achieved)
- Hyperkalemia: K⁺ rises 1-2 mEq/L from hemolysis
- Surfactant washout: Causes ARDS in survivors (40%)
- Ventricular fibrillation: More common than seawater (60% vs 40%)
-
Seawater Drowning (Hypertonic Aspiration)
- Osmotic fluid shift: Plasma → alveoli (pulmonary edema)
- Hemoconcentration: Hematocrit increases 10-15%
- Hypernatremia: Na⁺ rises 10-15 mEq/L (rarely >160 mEq/L)
- Hypermagnesemia: Mg²⁺ increases 2-3 mEq/L
- Surfactant destruction: Severe V/Q mismatch
- Asystole: More common than freshwater (60% vs 40%)
💡 Master This: The "drowning volume paradox" reveals that electrolyte changes require aspiration of >22 mL/kg (1.5 L in 70 kg adult), but most drowning victims aspirate only 2-4 mL/kg. Death results from surfactant dysfunction and V/Q mismatch, not electrolyte abnormalities. Postmortem serum analysis cannot reliably distinguish freshwater from seawater drowning because volumes aspirated prove insufficient for diagnostic changes.
Autopsy Findings: Reading the Drowned Body
Drowning produces characteristic but non-specific findings; diagnosis requires correlation with scene investigation and exclusion of other causes:
-
External Findings
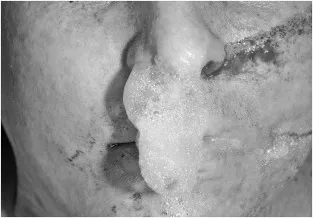
- Fine white foam at nose/mouth: Present in 50-70%, pathognomonic when present
- Washerwoman hands: Palmar/plantar skin wrinkling (after 2-3 hours immersion)
- Cutis anserina ("goose flesh"): Piloerection from cadaveric spasm (30%)
- Adipocere formation: In prolonged immersion >2-3 weeks
- Postmortem injuries: From aquatic animals, boats, rocks (40% show injuries)
-
Internal Findings (Diagnostic Constellation)
- Foam in airways: White/pink foam in trachea/bronchi (70-85%)
- Pulmonary edema: Heavy, wet lungs (combined weight >1,000 g)
- Emphysema aquosum: Overdistended lungs overlapping heart (60%)
- Hemorrhages: Subpleural petechiae (Paltauf spots) in 40%
- Stomach contents: Water in stomach (60-70%), duodenum (30%)
-
Diagnostic Laboratory Tests
- Diatom test: Diatoms in bone marrow/organs suggest antemortem drowning
- Sensitivity: 60-70% (many false negatives)
- Specificity: 85-90% (contamination causes false positives)
- Requires >20 diatoms/sample for significance
- Strontium analysis: Sr⁺² in blood >0.25 mg/L suggests seawater drowning
- Chloride comparison: Left vs right heart Cl⁻ difference >25 mEq/L (unreliable)
- Specific gravity: Left vs right heart difference >0.001 (historical, not validated)
- Diatom test: Diatoms in bone marrow/organs suggest antemortem drowning
⭐ Clinical Pearl: The "dry drowning" autopsy shows minimal lung findings despite witnessed drowning-laryngospasm prevented aspiration but caused fatal hypoxia. These cases (10-15% of drownings) show absence of foam, minimal edema, and no diatoms, making diagnosis dependent on scene investigation and witness statements. Internal findings may resemble suffocation or cardiac death.
| Finding | Drowning | Postmortem Submersion | Diagnostic Value |
|---|---|---|---|
| Foam in Airways | 70-85% | <5% | High specificity |
| Lung Weight | >1,000 g | Normal (600-800 g) | Moderate |
| Diatoms in Organs | 60-70% | Absent | High when positive |
| Stomach Water | 60-70% | May be present | Low specificity |
| Hemorrhages | 40-60% | <10% | Moderate |
| Washerwoman Hands | Present | Present | No value |
Explore the unique diagnostic challenges when drowning occurs in special populations through , where bathtub drownings and inflicted submersion require careful distinction from natural infant death and accidental immersion.
🏥 Drowning: The Aquatic Asphyxia
🔍 Chemical & Positional Asphyxia: The Hidden Killers
Chemical asphyxiants kill through systemic mechanisms-disrupting oxygen transport or cellular utilization-rather than mechanical airway obstruction. These toxins produce >15,000 deaths annually worldwide, with carbon monoxide alone accounting for >50% of poisoning fatalities. Positional asphyxia represents mechanical restriction of breathing from body position, causing >1,000 custody-related deaths over the past two decades and generating significant medicolegal controversy.

Carbon Monoxide: The Silent Epidemic
Carbon monoxide (CO) represents the most common fatal chemical asphyxiant, producing death through competitive oxygen displacement and cytochrome inhibition:
-
Mechanism of Toxicity
- Hemoglobin binding: CO affinity 240× greater than oxygen
- Carboxyhemoglobin (COHb): Shifts O₂-Hb dissociation curve left
- Cytochrome oxidase inhibition: Blocks cellular respiration directly
- Myoglobin binding: Cardiac and skeletal muscle dysfunction
- Lipid peroxidation: Free radical damage to brain tissue
-
COHb Levels and Clinical Effects
- <10%: Normal (smokers baseline 5-8%)
- 10-20%: Headache, mild confusion (threshold for symptoms)
- 20-40%: Severe headache, nausea, weakness, visual disturbance
- 40-60%: Confusion, syncope, tachycardia (>100 bpm), chest
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more
Have doubts about this lesson?
Ask Rezzy, your AI Study Mate, to explain anything you didn't understand
Everything you need for NEET-PG prep
Get full Oncourse access with lessons, practice questions, flashcards and AI study tools.
Scan to download app














