Oropharyngeal Carcinoma - Defining the Danger
- Epidemiology:
- Incidence varies globally; ↑ in regions with high HPV prevalence or tobacco/alcohol use.
- Typically affects males > females (3:1).
- Peak incidence: 50-70 years.
- Etiology:
- Human Papillomavirus (HPV): Major cause, esp. HPV-16. Primarily tonsils & base of tongue.
- Tobacco: Smoking, chewing. Synergistic with alcohol.
- Alcohol: Heavy consumption.
- Other: Poor oral hygiene, immunosuppression, genetic predisposition.
⭐ HPV-positive oropharyngeal cancers, particularly those involving the tonsils and base of tongue, generally have a better prognosis than HPV-negative cancers.
Oropharyngeal Carcinoma - Hotspots & Symptoms
- Anatomical Hotspots:
- Tonsil (palatine): Most common, strong HPV association.
- Base of Tongue (BOT): Often presents late.
- Soft Palate & Uvula.
- Posterior Pharyngeal Wall.
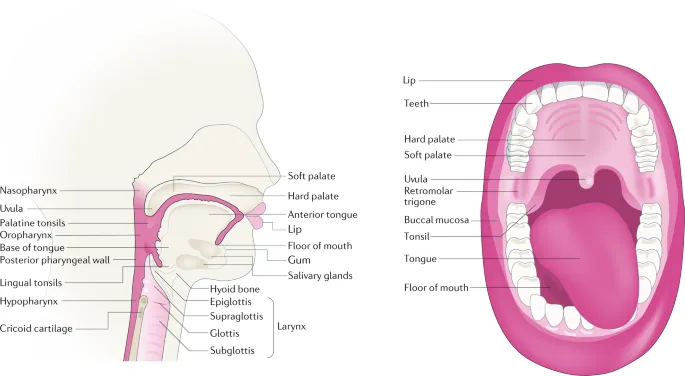
- Presenting Symptoms:
- Persistent unilateral sore throat.
- Dysphagia (difficulty swallowing) & Odynophagia (painful).
- Referred otalgia (ear pain via CN IX, X).
- Neck lump (lymph node metastasis).
- Trismus (difficulty opening mouth).
- Unexplained weight loss.
- Voice change (e.g., "hot potato voice").
⭐ Persistent unilateral sore throat, especially with referred otalgia (cranial nerve IX, X involvement), in an adult smoker/drinker should raise high suspicion for oropharyngeal carcinoma.
Oropharyngeal Carcinoma - Detective Work & Staging
- Clinical & Endoscopic Exam:
- Inspect & palpate oropharynx (tongue base, tonsils, soft palate).
- Direct visualization to assess tumor extent.
- Biopsy:
- Incisional/punch biopsy from primary site: GOLD STANDARD.
- FNAC for suspicious neck nodes.
- Imaging:
- CT Neck (contrast): Primary tumor, nodes, bone.
- MRI: Soft tissue, perineural invasion.
- PET-CT: Distant metastases, occult primaries.
- Chest imaging: Lung metastases.

- Staging (AJCC 8th Ed.):
- p16 testing (HPV surrogate) MANDATORY.
- Separate TNM for p16+ (better prognosis) & p16- tumors.
⭐ As per AJCC 8th edition, p16 testing is mandatory for oropharyngeal squamous cell carcinoma staging; HPV (p16)-positive tumors have a distinct TNM staging system, especially for N categories.
Oropharyngeal Carcinoma - Treatment Tactics & Fate
- Treatment Modalities: Multimodal approach is common.
- Surgery: Transoral Robotic Surgery (TORS), open resection.
- Radiotherapy (RT): External Beam RT (EBRT), Intensity Modulated RT (IMRT).
- Chemotherapy (CT): Cisplatin-based, often concurrent with RT (CCRT).
- Immunotherapy: Pembrolizumab, Nivolumab (PD-1 inhibitors) for recurrent/metastatic disease.
- Targeted Therapy: Cetuximab (EGFR inhibitor).
- HPV+ vs HPV-:
- HPV+ tumors: Better prognosis, often respond well to de-escalated RT/TORS.
- HPV- tumors: More aggressive, standard CCRT often needed.
⭐ Transoral Robotic Surgery (TORS) offers a minimally invasive approach for selected early-stage oropharyngeal cancers, potentially reducing treatment-related morbidity and allowing for de-escalation of adjuvant therapy in HPV-positive cases.
- Prognosis (Fate):
- Better for HPV+, early stage, non-smokers.
- Worse for HPV-, advanced stage, smokers, perineural invasion.
- Overall 5-year survival: HPV+ ~75-80%; HPV- ~40-50%.

High‑Yield Points - ⚡ Biggest Takeaways
- Primary sites: Tonsil and base of tongue are most common.
- Histopathology: Over 90% are Squamous Cell Carcinoma (SCC).
- Etiology: Strongly linked to HPV (p16 positive), tobacco, and alcohol.
- HPV-positive tumors: Better prognosis, affect younger patients, respond well to treatment.
- HPV-negative tumors: Associated with smoking/alcohol, carry a poorer prognosis.
- Clinical features: Persistent sore throat, dysphagia, odynophagia, often a neck mass.
- Diagnostic standard: Biopsy with histopathological examination is crucial.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

