Overview of Membrane Pathologies - Membrane Mayhem
Cell membrane dysfunction, or "Membrane Mayhem," underlies diverse diseases. Key mechanisms:
- Genetic: Mutations affecting membrane proteins.
- Channelopathies (e.g., Cystic Fibrosis - CFTR defect).
- Transportopathies (e.g., Cystinuria - amino acid transporter defect).
- Receptor defects (e.g., Familial Hypercholesterolemia - LDLR).
- Structural defects (e.g., Hereditary Spherocytosis - spectrin/ankyrin).
- Autoimmune: Antibodies target membrane components (e.g., Myasthenia Gravis - AChR).
- Toxin-induced: Pathogen toxins or drugs disrupt membrane (e.g., Diphtheria toxin).
- Other: Oxidative stress, lipid peroxidation, nutritional deficiencies (e.g., Vitamin E).
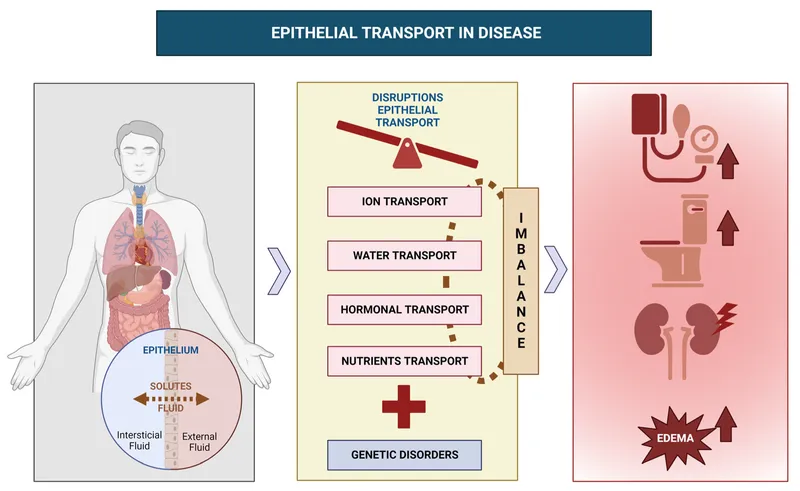
⭐ In Cystic Fibrosis, mutations in the CFTR gene lead to defective chloride ion transport, causing thick, sticky mucus in lungs and pancreas.
Channelopathies & Transporter Defects - Gated Grief & Cargo Chaos
Dysfunctional ion channels or transporters cause inherited/acquired diseases.
-
Channelopathies (Gated Grief): Defective ion channels.
- Cystic Fibrosis (CF): AR. CFTR (Cl⁻ channel) defect. 📌 Chloride Flow Trouble Results. Affects lungs, pancreas.
⭐ Most common CF mutation: ΔF508 in CFTR (misfolding, degradation).
- Long QT Syndromes (LQTS): K⁺/Na⁺ channel gene defects. Prolonged QT, risk of Torsades de Pointes, sudden death.
- Cystic Fibrosis (CF): AR. CFTR (Cl⁻ channel) defect. 📌 Chloride Flow Trouble Results. Affects lungs, pancreas.
-
Transporter Defects (Cargo Chaos): Impaired solute carriers.
- Glucose-Galactose Malabsorption: AR. SGLT1 (Na⁺-glucose cotransporter) defect. Severe neonatal diarrhea.
- Hartnup Disease: AR. Neutral amino acid transporter (SLC6A19) defect. Pellagra-like symptoms (dermatitis, diarrhea, ataxia); ↓ tryptophan absorption → ↓ niacin.
Receptor & Structural Protein Disorders - Signal Sickness & Framework Flaws
-
Receptor Disorders (Signal Sickness):
- Familial Hypercholesterolemia (FH):
- Defect: LDL Receptor (LDLR); AD.
- Patho: ↓Hepatic LDL uptake → ↑Plasma LDL/Cholesterol → Atherosclerosis, tendon xanthomas.
- Myasthenia Gravis (MG):
- Defect: Autoantibodies vs. postsynaptic ACh Receptors (AChR) at NMJ.
- Patho: ↓ACh binding → Fatigable muscle weakness (ocular, bulbar).
- ⭐ > ~75% of MG patients show thymic abnormalities (hyperplasia/thymoma).
- Familial Hypercholesterolemia (FH):
-
Structural Protein Disorders (Framework Flaws):
- Hereditary Spherocytosis (HS):
- Defect: Ankyrin, Spectrin; AD common.
- Patho: RBC membrane instability → Spherocytes → Splenic sequestration, hemolysis, ↑MCHC, ↑Osmotic Fragility.
- Duchenne Muscular Dystrophy (DMD):
- Defect: Dystrophin (DMD gene); X-linked Recessive.
- Patho: Absent dystrophin → Muscle fiber necrosis, progressive proximal weakness, Gower's sign, calf pseudohypertrophy, ↑CK. 📌 Duchenne = Dystrophin Deficient.
- Hereditary Spherocytosis (HS):
Membrane‑Targeting Toxins & Infections - Pathogen Pillage
Pathogens strategically exploit host cell membranes for entry, replication, nutrient acquisition, and immune evasion.
- Bacterial Toxins:
- Pore-Forming Toxins: Disrupt membrane integrity.
- Streptolysin O, Pneumolysin: Cholesterol-dependent cytolysins.
- Staph. aureus α-toxin: Forms β-barrel pores.
- Enzymatic (A-B) Toxins: B-subunit binds; A-subunit (active) enters.
- Diphtheria Toxin: ADP-ribosylates $eEF-2$ $\rightarrow$ halts protein synthesis.
- Cholera Toxin: ADP-ribosylates $G_s\alpha$ $\rightarrow$ $\uparrow\text{cAMP}$.
- Pore-Forming Toxins: Disrupt membrane integrity.
- Viral Membrane Interactions:
- Enveloped Viruses (HIV, Influenza): Membrane fusion via viral glycoproteins.
- Non-enveloped Viruses: Utilize endocytosis or direct membrane penetration.
⭐ Cholera toxin's A subunit ADP-ribosylates the Gs alpha subunit of G-protein, causing persistent cAMP elevation and severe secretory diarrhea.
High‑Yield Points - ⚡ Biggest Takeaways
- Cystic Fibrosis: CFTR gene mutation (common ΔF508), defective Cl- channel transport, ↑ sweat Cl-.
- Hereditary Spherocytosis: Spectrin/Ankyrin defects impair RBC membrane; spherocytes, ↑ osmotic fragility.
- PNH: Acquired PIGA mutation causes GPI anchor deficiency (loss of CD55/CD59), intravascular hemolysis.
- Familial Hypercholesterolemia: LDL receptor gene defect, significantly ↑ plasma LDL-C, xanthomas, early CAD.
- Renal Tubulopathies: Gitelman (NCC defect) and Bartter (NKCC2 defect) syndromes cause hypokalemia, metabolic alkalosis.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

