Peritonsillar Abscess - Quinsy's Fiery Throat

- Collection of pus between tonsillar capsule & superior constrictor muscle.
- Usually unilateral, complication of acute tonsillitis.
- Presents with severe sore throat, dysphagia, odynophagia, trismus, muffled "hot potato" voice, drooling.
- Uvula deviated to contralateral side.
⭐ Peritonsillar abscess is the most common deep neck infection in adults.
Etiopathogenesis - Bugs & Barricades
- Bugs (Causative Organisms):
- Polymicrobial: Streptococcus pyogenes (Group A Strep) most common. Also Staphylococcus aureus.
- Anaerobes: F. necrophorum, Prevotella, Porphyromonas, Peptostreptococcus spp.
- Pathogenesis (Progression):
- Complication of acute exudative tonsillitis.
- Infection from tonsillar crypts invades peritonsillar space, often superiorly.
⭐ Involvement of Weber's glands (minor salivary glands in the supratonsillar fossa) is key in the pathogenesis, as their ducts can become obstructed.
Clinical Picture - Symptoms & Signs
- Symptoms:
- Severe, progressive unilateral sore throat.
- Odynophagia (painful swallowing) & dysphagia (difficulty swallowing).
- Fever, chills, malaise.
- Ipsilateral otalgia (referred ear pain).
- Drooling, halitosis.
- Key Signs: 📌 TUV Mnemonic for classic triad:
- Trismus (difficulty opening mouth).
- Uvular deviation to contralateral (unaffected) side.
- Voice change:
⭐ The 'hot potato voice' (muffled voice, as if speaking with a hot potato in the mouth) is a classic pathognomonic sign.
- Oropharyngeal Exam Findings:
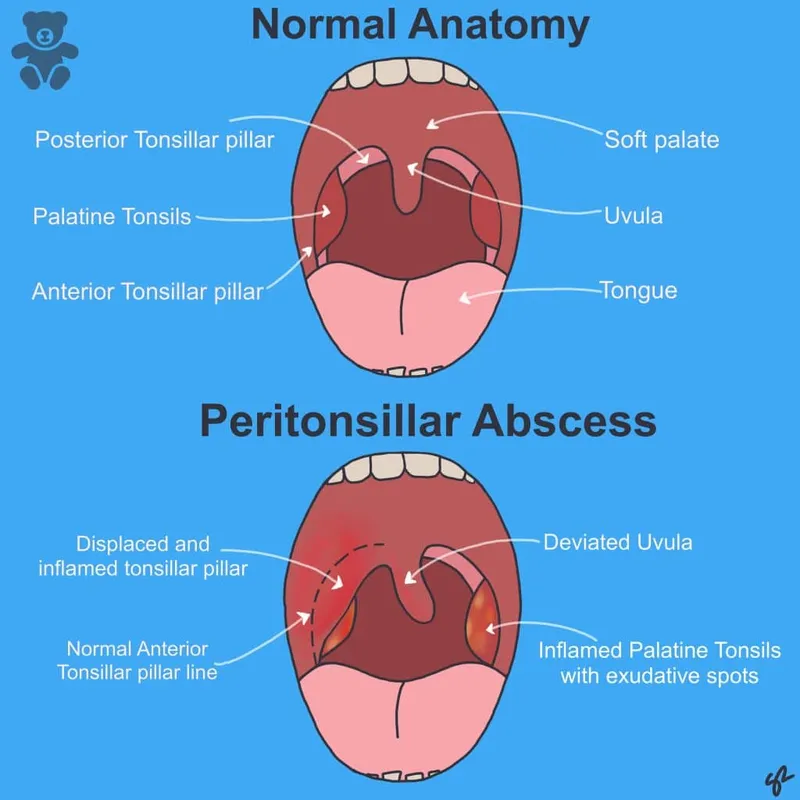
- Unilateral peritonsillar swelling & erythema; bulging soft palate.
- Affected tonsil displaced medially and inferiorly.
- Tender cervical lymphadenopathy.
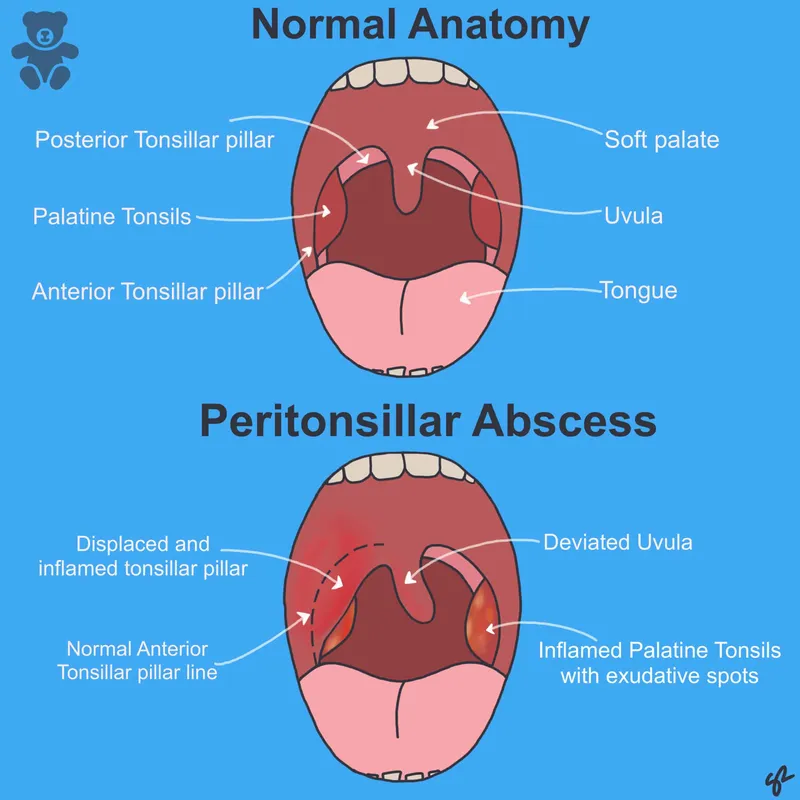
Diagnosis & DDx - Spotting the Pus
- Clinical Diagnosis: Key signs: trismus, muffled voice, uvular deviation.
- Needle Aspiration:
- Confirms pus.
- Often therapeutic.
- Site: Superior tonsillar pole.
- Imaging:
- CT with contrast: For unclear diagnosis/deep neck spread. Shows collection.
- Intraoral ultrasound: Alternative to CT.
⭐ Needle aspiration is both diagnostic (confirms presence of pus) and often therapeutic.
Differential Diagnosis:
| Condition | Differentiating Features |
|---|---|
| Peritonsillar Cellulitis | No pus; diffuse inflammation |
| Severe Tonsillitis | Bilateral; no trismus/uvular shift |
| Parapharyngeal Abscess | Medial pharyngeal bulge; neck swelling |
| Dental Infection | Primary dental pathology |
Management - Drain & Tame
- Initial Steps:
- Airway assessment; secure if compromised.
- IV fluids, potent analgesia.
- Empirical IV antibiotics (e.g., Amoxicillin-Clavulanate or Clindamycin; Penicillin G + Metronidazole).
- Drainage (Crucial):
- Needle Aspiration: Often first-line; diagnostic & therapeutic.
- Incision & Drainage (I&D): For larger abscesses or failed aspiration.
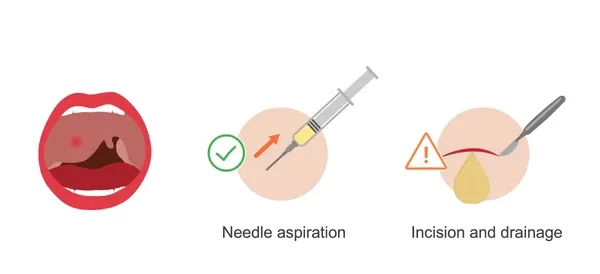
- Tonsillectomy Considerations:
- Interval tonsillectomy: 4-6 weeks post-resolution for recurrent PTA.
- Quinsy (Hot) tonsillectomy: During acute phase for specific indications.
⭐ Key indications for 'quinsy tonsillectomy' (tonsillectomy à chaud, during acute infection) include recurrent peritonsillar abscess, failure of adequate drainage, or presence of complications.
Complications - When Quinsy Spreads
- Spread to adjacent spaces:
- Parapharyngeal abscess
- Retropharyngeal abscess
- Ludwig's angina
- Airway compromise:
- Laryngeal edema, obstruction
- Systemic/Vascular:
- Sepsis, septic shock
- Aspiration pneumonia
- Mediastinitis
⭐ Lemierre's syndrome: Septic thrombophlebitis of IJV (Internal Jugular Vein), often Fusobacterium necrophorum. Rare, life-threatening.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common deep neck infection in adults, typically a complication of acute tonsillitis.
- Presents with severe unilateral sore throat, odynophagia, trismus, and characteristic "hot potato" voice.
- Key signs: Uvular deviation to the contralateral side and bulging of the soft palate.
- Caused by polymicrobial infection, commonly Strep. pyogenes and anaerobes.
- Management: Incision and Drainage (I&D) is crucial, along with systemic antibiotics.
- Interval tonsillectomy is often recommended after one episode to prevent recurrence.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

