Adenoids 101 - Nasopharyngeal Guardians

- A.k.a. Pharyngeal tonsils or Luschka's tonsil.
- Location: Midline, posterosuperior wall of the nasopharynx.
- Composition: Lymphoid tissue, part of Waldeyer's tonsillar ring.
- Lining Epithelium: Ciliated pseudostratified columnar epithelium.
- Blood Supply: Key branches from ascending pharyngeal, maxillary, facial arteries.
- Physiology: Active immune role in early childhood; typically begin to atrophy around age 8-10, regress by puberty (~15 years).
⭐ Adenoids (pharyngeal tonsils) are lymphoid tissue located in the posterosuperior wall of the nasopharynx.
Hypertrophy Hub - Why They Swell
- Primary Causes:
- Repeated infections: Viral (adenovirus, rhinovirus) or bacterial (Streptococcus, Haemophilus).
- Allergic rhinitis: Chronic inflammation triggers lymphoid tissue reaction.
- Physiological: Natural immune system development in children.
- Pathophysiology: Persistent antigenic stimulation leads to an increase in the size (hyperplasia) of the adenoid lymphoid tissue.
⭐ Physiological hypertrophy is most prominent between 3-7 years of age. It usually undergoes spontaneous regression by puberty.
Symptom Spotlight - Signs & Snores
- Nasal & Respiratory:
- Mouth breathing (persistent)
- Snoring (loud, apneic pauses → OSA)
- Rhinorrhea (nasal discharge)
- Hyponasal speech (Rhinolalia clausa)
- Otological (Eustachian Tube Dysfunction):
- Recurrent AOM
- OME ("Glue ear") → conductive hearing loss
- Adenoid Facies (Chronic Obstruction):
- Elongated face, open mouth, dull look
- Pinched nares, high-arched palate
- Dental malocclusion
- 📌 FACES Mnemonic:
- Flat midface
- Allergic shiners
- Chronic mouth breathing
- Elongated face
- Short upper lip / High arched palate

- General:
- Restless sleep, night cough
- Feeding difficulty (infants)
⭐ 'Adenoid facies' is a characteristic constellation of facial features due to chronic nasal obstruction from adenoid hypertrophy.
Diagnostic Drilldown - Peeking & Probing
- Clinical Suspicion: Based on hallmark symptoms (persistent nasal obstruction, mouth breathing, snoring, hyponasal speech).
- Examination:
- Posterior Rhinoscopy: May reveal adenoid mass; difficult in young children.
- Nasal Endoscopy: Gold standard for direct visualization and grading.
- Imaging:
- X-ray Soft Tissue Lateral Neck View: Assesses adenoid size relative to nasopharyngeal airway. Narrowed airway; >50% obstruction significant. Calculates Adenoid-Nasopharyngeal (A/N) ratio.
- Confirmation & Grading: From endoscopic/radiological findings.
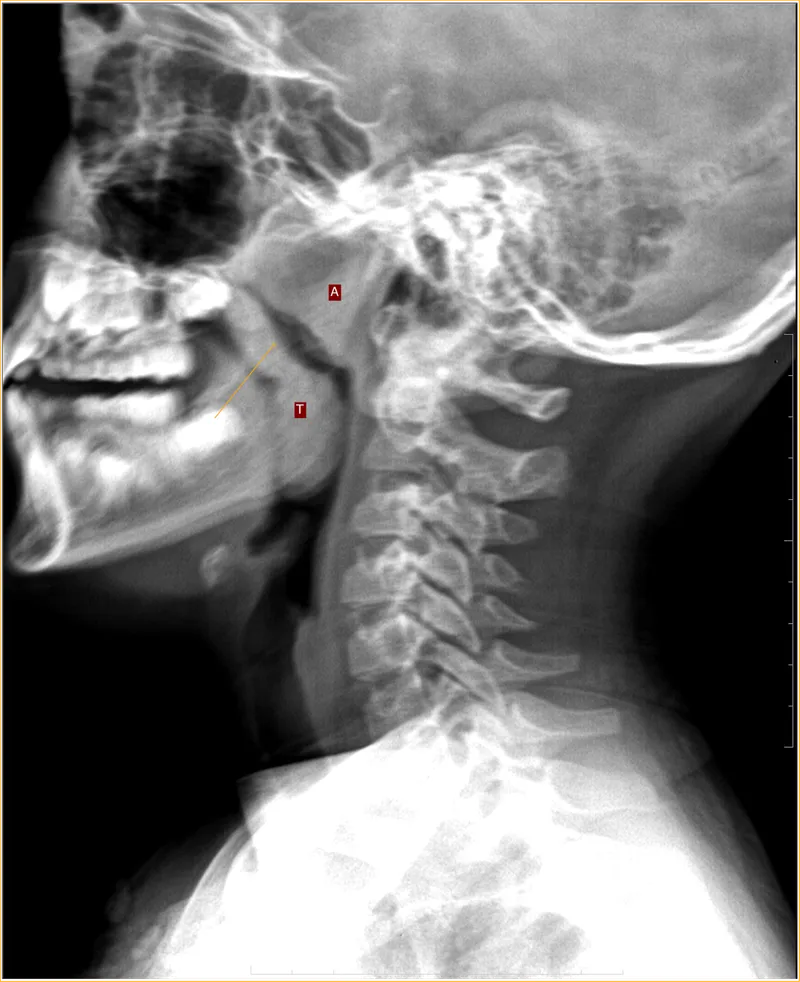
⭐ Nasal endoscopy is the gold standard for diagnosis, but X-ray soft tissue lateral view of nasopharynx is a common, non-invasive investigation.
Treatment Toolkit - Shrink or Snip?
Management hinges on symptom severity and associated complications.
- Medical Management (Shrink):
- Nasal corticosteroids (e.g., fluticasone, mometasone) are first-line.
- Saline nasal irrigation.
- Antihistamines if an allergic component is present.
- Surgical Management (Snip) - Adenoidectomy:
-
Typically considered for children aged >3 years unless severe obstruction or complications arise earlier.
-
Key Indications for Adenoidectomy:
Indication Core Criteria Obstructive Sleep Apnea (OSA) Significant airway obstruction during sleep Recurrent Acute Otitis Media ≥3 episodes in 6 months / ≥4 in 12 months Chronic Suppurative Otitis Media Persistent discharge despite medical Rx Chronic Rhinosinusitis Symptoms refractory to medical therapy Craniofacial Growth Abnormality E.g., "Adenoid facies", dental malocclusion Failure of Conservative Rx Persistent, significant symptoms
-
⭐ Exam Crux: Adenoidectomy is contraindicated in patients with an overt or submucous cleft palate (uncorrected) without prior comprehensive velopharyngeal insufficiency (VPI) assessment, due to risk of post-operative hypernasal speech.
High-Yield Points - ⚡ Biggest Takeaways
- Adenoid facies (open mouth, dull expression, elongated face) is a classic sign.
- Commonly causes nasal obstruction, mouth breathing, and snoring.
- Associated with otitis media with effusion (OME) due to Eustachian tube dysfunction.
- Diagnosis often clinical; X-ray lateral neck view (soft tissue) can confirm.
- Adenoidectomy is the definitive treatment for symptomatic hypertrophy.
- Peak incidence: 3-7 years of age.
- May lead to obstructive sleep apnea (OSA) in severe cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

