Introduction & Anatomy - Nosebleed Nuances
- Epistaxis: Bleeding from the nose.
- Nasal Septum Vascular Supply:
- Little's Area (Kiesselbach's Plexus): Anterosuperior septum. Arteries: 📌 Superior labial, Anterior ethmoidal, Greater palatine, Sphenopalatine (SAGS).
- Woodruff's Plexus: Posteroinferior, primarily sphenopalatine artery.
- Lateral Wall Supply: Sphenopalatine, ant/post ethmoidals, facial & greater palatine artery branches.
⭐ Kiesselbach's plexus in Little's area is the most common site (~90%) for anterior epistaxis.
Etiology - The Bleed Breakdown
| Local Causes | Systemic Causes |
|---|---|
| * Trauma: nose picking, fractures, foreign bodies | * Hypertension (prolongs bleeding) |
| * Inflammatory: sinusitis, rhinitis, allergies, granulomatous diseases (TB, Wegener's) | * Bleeding disorders: hemophilia, vWD, ITP, leukemia |
| * Neoplastic: JNA, SCC, inverted papilloma | * Medications: aspirin, warfarin, clopidogrel, NSAIDs |
| * Structural: Septal deviation, perforation | * Hereditary Hemorrhagic Telangiectasia (HHT) |
| * Iatrogenic: post-surgical, NG tube | * Others: liver disease, kidney disease, alcohol abuse, vitamin K deficiency |
| * Idiopathic |
Clinical Evaluation - Source Sleuthing
- History: Onset (spontaneous/traumatic), duration, frequency, severity, laterality, site clues (anterior/posterior), provoking factors. Medical Hx (HTN, coagulopathy), Drug Hx (anticoagulants, nasal sprays).
- Examination:
- Assess hemodynamic stability (pulse, BP).
- Anterior rhinoscopy: remove clots, identify bleeding point.
- Nasal endoscopy: if site unclear or posterior bleed suspected.
- Differentiating Anterior vs. Posterior Epistaxis:
- Investigations:
- CBC (assess blood loss).
- Coagulation profile (PT, aPTT, INR): if recurrent/severe/systemic cause suspected/on anticoagulants.
- CT/MRI: for suspected tumors/sinus pathology or refractory epistaxis.
⭐ Posterior epistaxis typically involves bleeding from branches of the sphenopalatine artery (Woodruff's plexus) and often presents with blood trickling down the pharynx.
Management - Flow Stoppers
-
Initial: ABCs. Trotter's method (pinch soft nose, lean forward, mouth breathe 10-20 mins). Ice pack (nasal bridge).
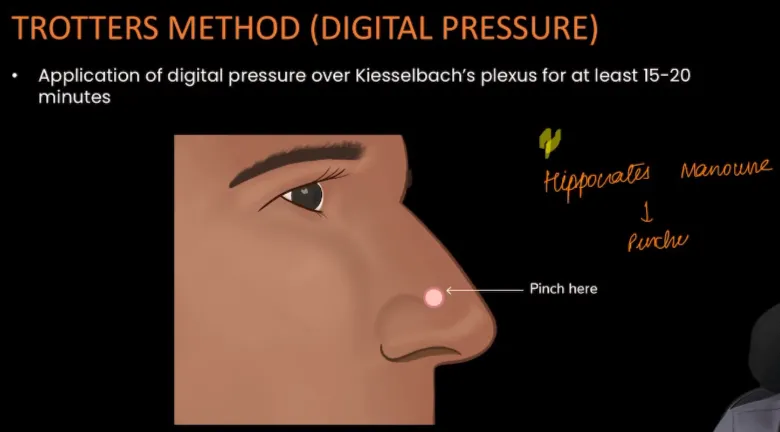
-
Medical/Cautery (if bleeding point visible):
- Topical vasoconstrictors: Oxymetazoline, Adrenaline 1:1000.
- Cauterization: Chemical ($AgNO_3$ - avoid bilateral septal), Electrocautery.
-
Nasal Packing (24-72 hrs):
- Anterior: Absorbable (Surgicel, Gelfoam); Non-absorbable (Merocel, BIPP - add prophylactic antibiotics).
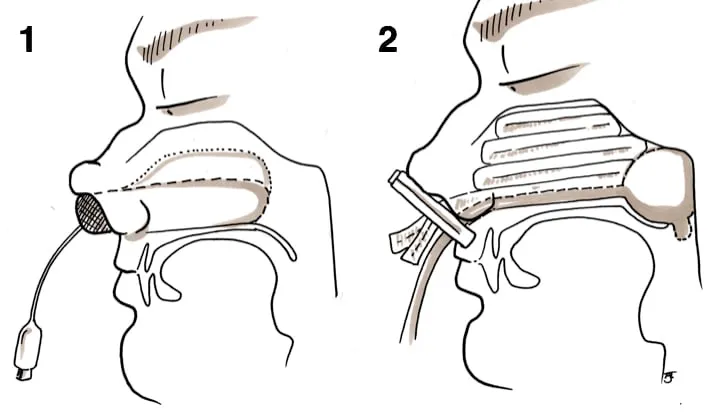
- Posterior: Foley's catheter (10-14 Fr), Epistat/Brighton balloon.
- Anterior: Absorbable (Surgicel, Gelfoam); Non-absorbable (Merocel, BIPP - add prophylactic antibiotics).
-
Surgical/Interventional (refractory/severe posterior):
- ESPAL (Endoscopic Sphenopalatine Artery Ligation) - Treatment of Choice.
- A/P Ethmoidal Artery Ligation. Maxillary Artery Ligation.
- Arterial Embolization (Interventional Radiology).
⭐ ESPAL has >90% success for intractable posterior epistaxis, preferred over older methods.
Complications & Special Cases - Red Alert Risks
- Epistaxis Complications: Anemia, hypovolemic shock, aspiration, sinusitis.
- Management Complications:
- Nasal Packing: Pain, infection, sinusitis, Toxic Shock Syndrome (TSS) (📌 Staph. aureus), septal perforation, alar necrosis.
- Cautery: Crusting, septal perforation, synechiae.
- Surgery/Embolization: Anesthesia risks, blindness, stroke.
- Special Cases:
- Children: Usually anterior; consider foreign body, JNA (adolescent males).
- Anticoagulated: ↑risk; manage anticoagulation.
- HHT: Recurrent; laser, septodermoplasty, Avastin.
⭐ Toxic Shock Syndrome (TSS), with fever, rash, hypotension, is a rare but life-threatening risk of prolonged nasal packing.
High‑Yield Points - ⚡ Biggest Takeaways
- Little's area (Kiesselbach's plexus) is the most common site for anterior epistaxis.
- Posterior epistaxis often arises from Woodruff's plexus (sphenopalatine artery branches), common in elderly/hypertensives.
- Initial management: ABCs, Trotter's method (direct pressure), anterior/posterior nasal packing, then cautery.
- Sphenopalatine Artery Ligation (SPAL) is a key surgical option for refractory posterior epistaxis.
- Suspect Juvenile Nasopharyngeal Angiofibroma (JNA) with recurrent, profuse epistaxis in adolescent males.
- Hereditary Hemorrhagic Telangiectasia (HHT) presents with recurrent epistaxis and multiple telangiectasias.
- Uncontrolled hypertension is a major risk factor, especially for severe or posterior bleeds.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

