Genodermatoses: Basics - Gene Skin Deep
- Genetically determined skin disorders; often present at birth or early childhood.
- Inheritance Patterns:
- Autosomal Dominant (AD): Vertical transmission; 50% offspring risk. E.g., Neurofibromatosis 1, Tuberous Sclerosis.
- Autosomal Recessive (AR): Horizontal transmission; 25% offspring risk. E.g., Xeroderma Pigmentosum, Albinism.
- X-linked Recessive (XLR): Affects males primarily. E.g., Anhidrotic Ectodermal Dysplasia.
- X-linked Dominant (XLD): Often lethal in males. E.g., Incontinentia Pigmenti.
- Key Concepts: Penetrance (all-or-none expression), Expressivity (variable severity).

⭐ Lyonisation (X-inactivation) explains mosaic patterns in X-linked dominant disorders like Incontinentia Pigmenti.
Ichthyoses & PPK - Scaly Skin Tales
- Ichthyosis Vulgaris (IV): AD, FLG gene. Fine scales, spares flexures. Assoc. atopy.
- X-linked Ichthyosis (XLI): XR, STS deficiency. Dark scales (neck). Cryptorchidism, corneal opacities. 📌 "Dirty neck".
- Lamellar Ichthyosis (LI): AR, TGM1 gene. Collodion baby. Large plate-like scales, ectropion.
- Epidermolytic Hyperkeratosis (EHK): AD, KRT1/KRT10 genes. Birth: blisters. Later: verrucous scales (flexures).
- PPK - Diffuse (Unna-Thost/Vorner): AD, KRT9/KRT1 genes. Uniform thickening. Vorner type: epidermolytic.
- PPK - Focal (Richner-Hanhart): AR, TAT gene. Painful plaques (pressure areas). Tyrosinemia type II (corneal lesions).
- PPK - Punctate: Small "raindrop" keratoses.
⭐ X-linked Ichthyosis: Maternal STS gene deletion can lead to prolonged labor due to placental sulfatase deficiency impacting steroid metabolism during pregnancy.
Epidermolysis Bullosa - Bubble Trouble Tales
Group of inherited mechanobullous disorders. Characterized by skin fragility and blister formation upon minor trauma. Classified by the ultrastructural level of blister cleavage within or below the dermo-epidermal junction.
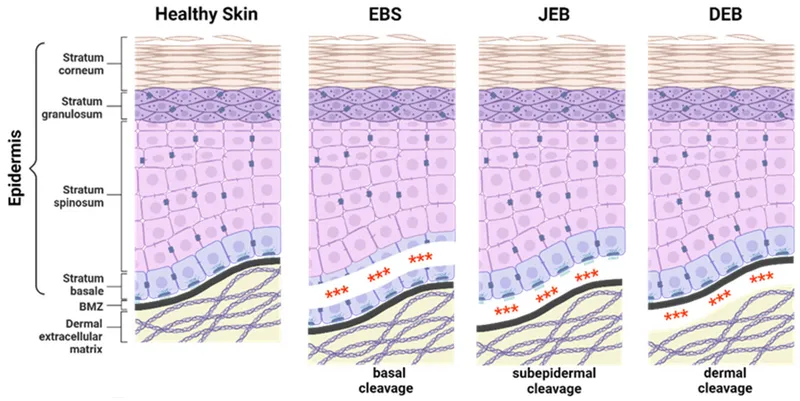
| Type | Cleavage Level | Protein(s) Affected | Inheritance | Clinical Hallmarks |
|---|---|---|---|---|
| EBS | Intraepidermal (basal cells) | Keratin 5, 14 | AD (most) | Blisters (often non-scarring), palmoplantar, Dowling-Meara |
| JEB | Lamina Lucida | Laminin-332, COL17A1, Integrin α6β4 | AR | Severe, granulation tissue, enamel defects, high mortality |
| DEB | Sublamina Densa (upper dermis) | Collagen VII (COL7A1) | AD/AR | Scarring, "mitten" hands (pseudosyndactyly), strictures, ↑SCC |
| Kindler | Variable (mixed planes) | Kindlin-1 (FERMT1) | AR | Neonatal blisters, photosensitivity, poikiloderma, atrophy |
Neurocutaneous Syndromes - Nerve & Nevi Notes
| Syndrome | Gene(s) | Key Skin Features | Key Neuro Features | Key Systemic |
|---|---|---|---|---|
| NF1 | NF1 (Chr 17) | ≥6 CALMs, axillary/inguinal freckling, neurofibromas, Lisch nodules | Optic glioma, learning disability | Bone (sphenoid dysplasia) |
| NF2 | NF2 (Chr 22) | Bilateral vestibular schwannomas (BVS), schwannomas, meningiomas | BVS (hearing loss, tinnitus), spinal tumors | Juvenile cataracts |
| TSC | TSC1/TSC2 | Ash-leaf spots (≥3), angiofibromas, shagreen patch, ungual fibromas (Koenen) | Cortical tubers, SEGA, infantile spasms, seizures | Renal AML, cardiac rhabdomyoma |
| SWS | Somatic GNAQ | Port-wine stain (V1/V2) | Leptomeningeal angioma, seizures, developmental delay | Ocular (glaucoma), hemiparesis |
⭐ Lisch nodules (iris hamartomas) are highly specific for NF1, seen in >90% of adult patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Ichthyosis vulgaris: Filaggrin gene mutation, fine white scales, spares flexures.
- Epidermolysis bullosa: Blistering from minor trauma; defects in keratins, laminin, or collagen VII.
- Neurofibromatosis Type 1 (NF1): Café-au-lait macules, neurofibromas, Lisch nodules; NF1 gene (Chr 17).
- Tuberous Sclerosis Complex (TSC): Ash-leaf spots, adenoma sebaceum (facial angiofibromas), shagreen patch; TSC1/TSC2 genes.
- Incontinentia Pigmenti: X-linked dominant; vesicular, verrucous, swirled hyperpigmentation, then atrophic stages.
- Xeroderma Pigmentosum (XP): Defective DNA nucleotide excision repair, extreme photosensitivity, high skin cancer risk.
- Oculocutaneous Albinism: Defective melanin synthesis (often tyrosinase); hypopigmentation, nystagmus, photophobia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

