Overview & Types - Skin Tight Saga
Scleroderma ("hard skin"): Diseases causing skin/connective tissue hardening. Morphea: Localized scleroderma; affects skin, can involve deeper tissues.
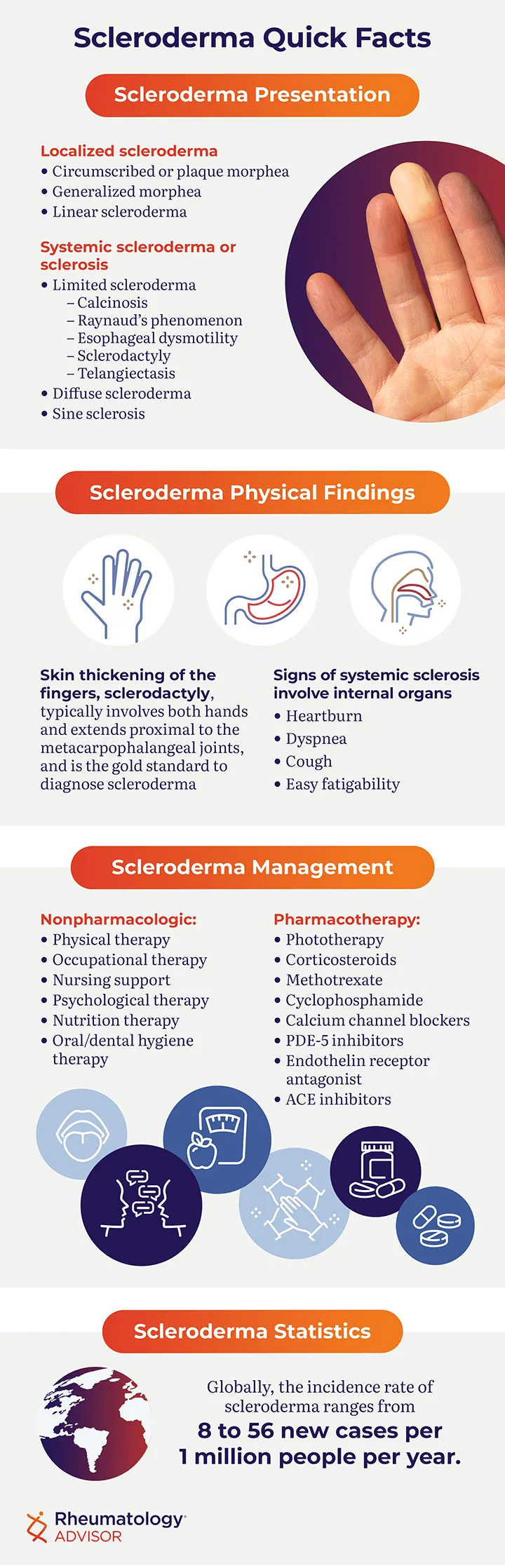
- Systemic Sclerosis (SSc):
- Limited (lcSSc): Skin thickening distal to elbows/knees, face/neck. 📌 CREST.
- Diffuse (dcSSc): Widespread skin thickening (proximal, trunk); early organ risk.
- Morphea (Localized):
- Types: Plaque, Linear (en coup de sabre), Generalized, Pansclerotic.
⭐ CREST syndrome (Calcinosis, Raynaud's, Esophageal dysmotility, Sclerodactyly, Telangiectasias) is a key presentation of limited SSc.
Pathophysiology - Fibrosis Frenzy
- Vascular Injury: Endothelial dysfunction triggers release of vasoactive mediators like Endothelin-1 (ET-1).
- Immune Activation: T-cells and B-cells orchestrate inflammation.
- Key cytokines: TGF-β, IL-6.
- Autoantibodies: ANA, Anti-Scl-70 (topoisomerase I), Anti-centromere (ACA), Anti-RNA polymerase III.
- Fibroblast Dysregulation: Leads to excessive collagen and ECM deposition, causing fibrosis.

⭐ Anti-Scl-70 (anti-topoisomerase I) antibodies are strongly associated with diffuse systemic sclerosis and increased risk of interstitial lung disease.
Morphea (Localized Scleroderma) - Patchy Problems
- Localized skin fibrosis; distinct from systemic sclerosis.
- Types:
- Circumscribed (plaque): Common; oval, indurated plaques.

- Linear: Bands on limbs, trunk, face/scalp ('en coup de sabre', Parry-Romberg syndrome).
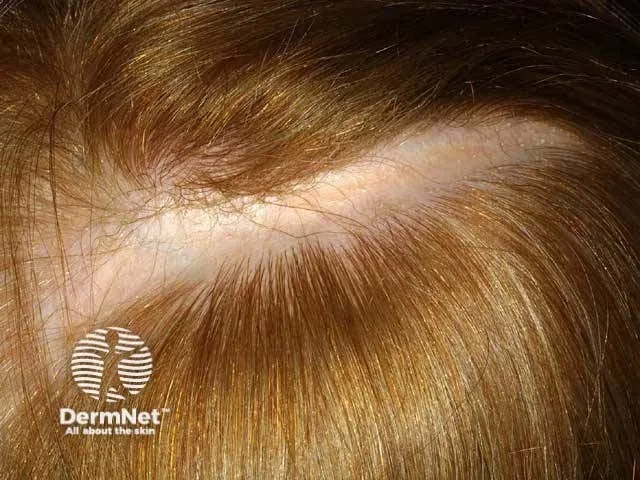
- Generalized: ≥4 large plaques, >2 body sites.
- Pansclerotic: Involves dermis, fat, fascia, muscle, bone.
- Mixed.
- Circumscribed (plaque): Common; oval, indurated plaques.
- Clinical: Erythema → induration, waxy texture, pigment changes, atrophy.
- Extracutaneous (rare): Arthralgia (especially with linear type), malaise.
⭐ 'En coup de sabre,' linear morphea of frontoparietal scalp/forehead, may link to CNS issues.
Systemic Sclerosis (SSc) - Systemic Siege
Core: Chronic autoimmune; fibrosis (skin, organs), vasculopathy.
Flowchart: SSc Subtype Differentiation
Table: Antibody Associations & Key Features
| Feature | lcSSc (CREST) | dcSSc |
|---|---|---|
| Antibodies | Anti-Centromere (ACA) | Anti-Scl-70, Anti-RNA Pol III |
| Skin Score | Lower mRSS | Higher mRSS, rapid ↑ |
| Main Risks | PAH (late) | ILD, Renal Crisis (early) |
- Common: Raynaud's (often initial), digital ulcers.
- GI: Esophageal dysmotility (most common), GAVE.
- Cardiac: Fibrosis, pericarditis (esp. dcSSc).
⭐ Scleroderma renal crisis (SRC): medical emergency (malignant HTN, AKI). More in dcSSc, anti-RNA Pol III+, high-dose steroid use.
Diagnosis & Management - Tackling Tightness
Diagnosis:
- ACR/EULAR 2013 criteria for SSc (score > 9).
- Skin Biopsy: ↑Collagen, perivascular inflammation.
- Autoantibodies: ANA (high titre); SSc-specific (Anti-Scl-70, Anti-centromere).
- Nailfold Capillaroscopy: Megacapillaries, avascular areas.
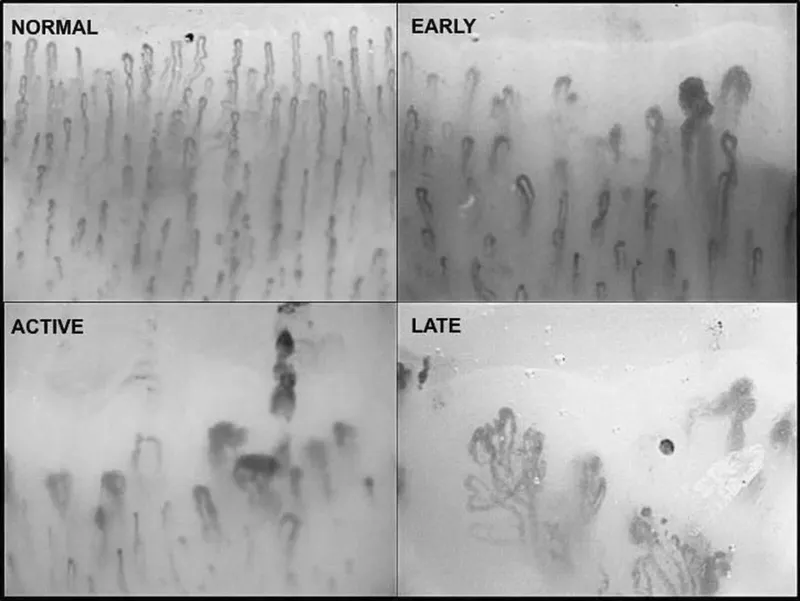
⭐ Nailfold capillaroscopy is a crucial non-invasive tool for early SSc diagnosis, distinguishing primary Raynaud's from secondary, and has prognostic value.
Management: Organ-based therapy; no cure.
- Morphea: Topical/intralesional steroids, phototherapy, MTX (severe).
- SSc (Systemic Sclerosis):
- ILD: Immunosuppressants (MMF, CYC; consider Nintedanib/Tocilizumab).
- Raynaud's/PAH: Vasodilators (CCBs, PDE5i).
- Renal Crisis: ACE inhibitors (STAT).
- GERD: PPIs.
- Physiotherapy essential.
High‑Yield Points - ⚡ Biggest Takeaways
- Scleroderma (Systemic Sclerosis): Multi-system disorder with skin fibrosis & internal organ (lungs, kidney) involvement.
- Morphea: Localized scleroderma; affects skin/subcutaneous tissue only, no systemic SSc features.
- CREST syndrome (lcSSc): Calcinosis, Raynaud's, Esophageal dysmotility, Sclerodactyly, Telangiectasias; associated with Anti-centromere antibodies.
- Diffuse SSc (dcSSc): Widespread skin thickening, rapid onset, early organ damage; linked to Anti-Scl-70 (topoisomerase I) antibodies.
- Anti-Scl-70 antibodies in dcSSc predict an increased risk of pulmonary fibrosis.
- Linear morphea can cause joint contractures and facial/scalp lesions ("en coup de sabre").
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

