MCTD Introduction - The Great Overlap
- MCTD: A distinct systemic autoimmune rheumatic disease, often termed an "overlap syndrome."
- Key characteristic: Combines clinical features typically seen in:
- Systemic Lupus Erythematosus (SLE)
- Systemic Sclerosis (SSc)
- Polymyositis (PM) and/or Dermatomyositis (DM)
- Initial presentation can be as Undifferentiated Connective Tissue Disease (UCTD).
- Disease course: May remain stable MCTD or evolve into a more defined CTD over time.
- Serological hallmark: Presence of high titers of antibodies to U1 ribonucleoprotein (anti-U1 RNP).
⭐ MCTD is characterized by high titers of anti-U1 RNP antibodies. oka
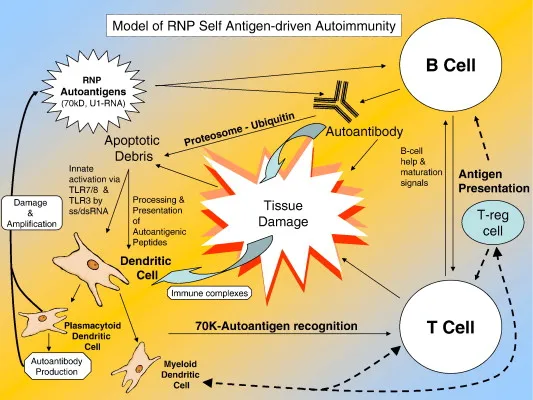
MCTD Pathophysiology - Immune System Mix-up
- Immune Dysregulation: Central defect; involves hyperactive T-cells & B-cells, leading to loss of self-tolerance.
- Autoantibody Production: Key feature is high-titer anti-U1-RNP antibodies.
- These antibodies recognize specific proteins (70kD, A, C) on U1 small nuclear ribonucleoprotein (snRNP) particles, crucial for mRNA splicing.
- Mechanism of Damage: Not fully elucidated but involves:
- Immune complex deposition.
- Complement activation.
- Endothelial cell injury & T-cell mediated cytotoxicity.
- Result: Inflammation & damage in various connective tissues.
⭐ Anti-U1-RNP antibodies target the 70-kD, A, and C proteins of the U1 small nuclear ribonucleoprotein particle.
MCTD Clinical Features - A Symptom Medley
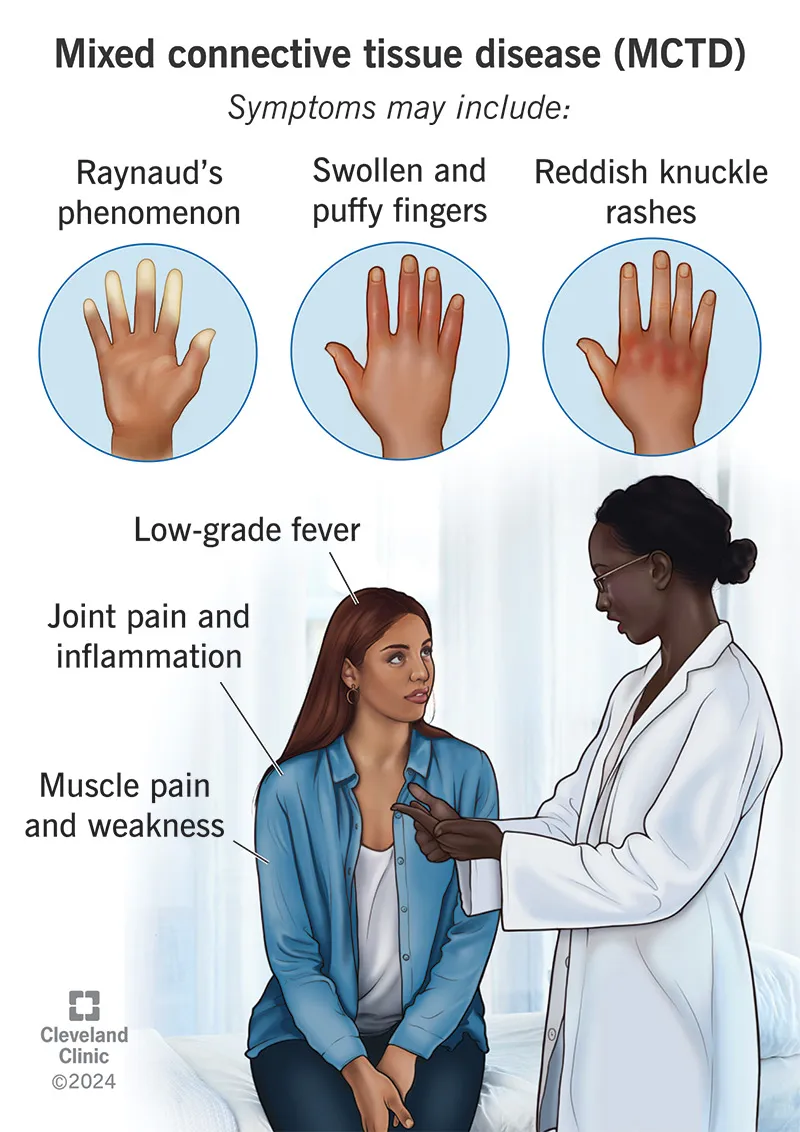
- Hallmarks (Often Initial):
- Raynaud's phenomenon: Vasospasm of digits; nearly 100% prevalence.
- Swollen hands/Puffy fingers: Diffuse swelling ("sausage digits"), may evolve to sclerodactyly.
- Musculoskeletal:
- Arthralgia/Polyarthritis: Symmetric, non-erosive; Jaccoud's arthropathy (deforming but reducible) possible.
- Inflammatory Myositis: Proximal muscle weakness, tenderness; elevated CK.
- Systemic Manifestations:
- Esophageal dysmotility: Dysphagia for solids/liquids, reflux.
- Pulmonary: Interstitial Lung Disease (ILD), Pulmonary Arterial Hypertension (PAH) - significant morbidity/mortality.
- Cardiac: Pericarditis most common; myocarditis, conduction defects.
- Renal: Mild glomerulonephritis (membranous nephropathy commonest).
- Neurologic: Trigeminal neuropathy is the most frequent CNS finding.
- Skin (Overlap Features):
- SLE-like: Malar rash, photosensitivity.
- SSc-like: Sclerodactyly, calcinosis cutis.
- DM-like: Gottron's papules (less common).
⭐ Raynaud's phenomenon is an almost universal presenting feature in MCTD.
MCTD Diagnosis - Pinpointing the Puzzle
- Diagnosis combines clinical criteria and specific serology.
- Commonly used criteria: Alarcon-Segovia, Kasukawa, Sharp.
- Clinical Presentation:
- Requires ≥2 CTD features (SLE, SSc, PM/DM).
- Key manifestations: Raynaud's phenomenon, swollen hands/puffy fingers, arthralgia/arthritis, myositis, esophageal dysmotility, acrosclerosis.
- Serological Hallmark:
- Essential: High-titer anti-U1 RNP antibodies (specifically U1 small nuclear ribonucleoprotein).
- ANA: Typically high-titer, speckled pattern.
⭐ High-titer anti-U1 RNP is essential for diagnosis, often in the absence of other specific autoantibodies like anti-dsDNA or anti-Scl-70.
- Supportive Serology:
- Other disease-specific autoantibodies (e.g., anti-dsDNA, anti-Sm, anti-Scl-70, anti-centromere, anti-Jo-1) typically absent or in low titers.
MCTD Management - Taming the Tempest
- Goal: Symptom control & organ protection.
- Mild disease (arthralgia, myalgia, rash):
- NSAIDs, Hydroxychloroquine (HCQ)
- Low-dose corticosteroids
- Moderate-Severe disease (organ involvement):
- High-dose corticosteroids
- Immunosuppressants (Methotrexate, Azathioprine, Mycophenolate mofetil)
- Biologics (e.g., Rituximab) for refractory cases.
- Raynaud's: Calcium channel blockers, lifestyle changes.
- Pulmonary Hypertension: Vasodilators (PDE5-inhibitors, ERAs, prostanoids).
⭐ Pulmonary hypertension is a major cause of mortality in MCTD.
- Regular follow-up is crucial for monitoring disease activity and complications.
High‑Yield Points - ⚡ Biggest Takeaways
- MCTD is a distinct overlap syndrome with features of SLE, systemic sclerosis, and polymyositis/dermatomyositis.
- Serological hallmark: Presence of high-titer anti-U1 RNP antibodies.
- Frequent early manifestations: Raynaud's phenomenon, swollen hands or puffy fingers, and arthralgias.
- Pulmonary hypertension is a critical complication and a leading cause of mortality.
- Other significant involvements include arthritis, myositis, esophageal dysmotility, and interstitial lung disease.
- Often referred to as Sharp's syndrome.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

