Immunobullous Overview - Blister Blueprint
- Definition: Group of autoimmune diseases where autoantibodies target adhesion molecules in skin/mucosa, causing blisters.
- Pathophysiology: Autoantibodies (IgG, IgA) bind to target antigens (e.g., desmogleins, BPAG1, BPAG2), activating complement & inflammatory cells, leading to blister formation.
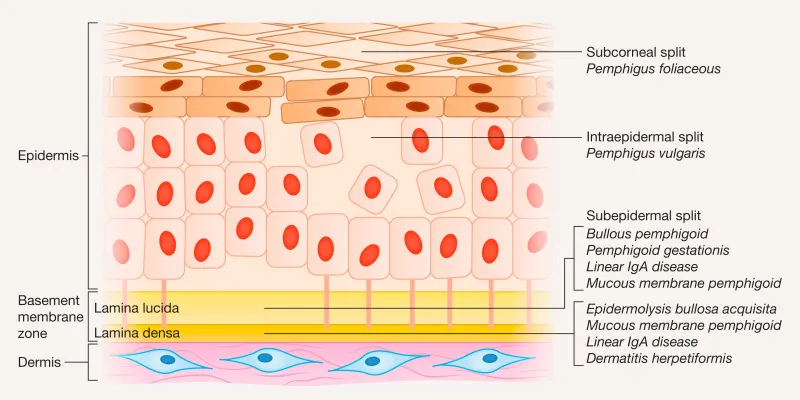
- Classification (Level of Split):
- Intraepidermal: Blisters within the epidermis (e.g., Pemphigus group).
- Subepidermal: Blisters below the epidermis, at dermoepidermal junction (e.g., Pemphigoid group, Dermatitis Herpetiformis).
- Key Diagnostic Tests:
- Skin Biopsy (H&E): Shows level of split, inflammatory infiltrate.
- Direct Immunofluorescence (DIF): Detects autoantibodies in perilesional skin (📌 DIF = Deposits in skin).
- Indirect Immunofluorescence (IIF): Detects circulating autoantibodies in serum (📌 IIF = In serum).
- ELISA: Identifies specific autoantibodies (e.g., anti-Dsg1, anti-Dsg3, anti-BP180, anti-BP230).
⭐ Nikolsky's sign: Elicited by applying tangential pressure to perilesional skin; positive (epidermis dislodges) in conditions with acantholysis like Pemphigus Vulgaris due to loss of keratinocyte adhesion.
Pemphigus Disorders - Intraepidermal Agony
- Pemphigus Vulgaris (PV):
- 📌 'Vulgaris is Vicious and Deep': Targets Desmoglein 3 (Dsg3) > Desmoglein 1 (Dsg1).
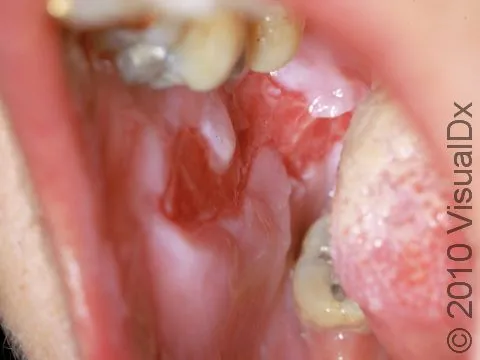
- Clinical: Flaccid blisters, common oral erosions, +Nikolsky sign.
- Histology: Intraepidermal, suprabasal acantholysis, Tzanck cells.
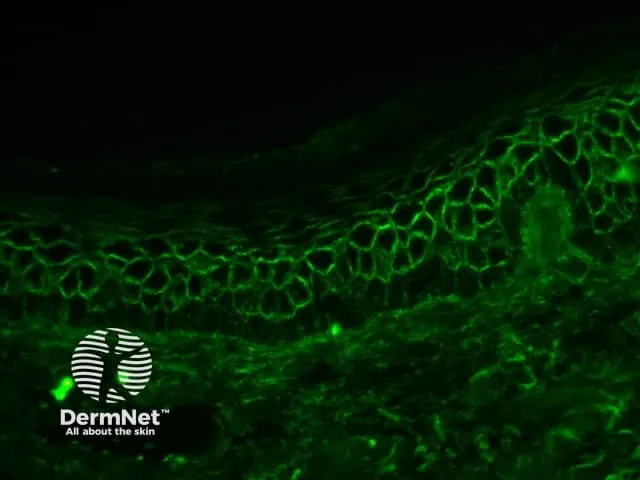
- DIF: Intercellular IgG/C3 ('chicken-wire' or 'fishnet' pattern).
- Pemphigus Foliaceus (PF):
- Targets Desmoglein 1 (Dsg1).
- Clinical: Superficial blisters, crusted/scaly lesions, rare/no oral involvement, +Nikolsky sign.
- Histology: Superficial acantholysis (granular layer).
- Paraneoplastic Pemphigus: Severe, malignancy-associated (often lymphoproliferative); polymorphic lesions.
| Feature | Pemphigus Vulgaris (PV) | Pemphigus Foliaceus (PF) |
|---|---|---|
| Target(s) | Dsg3 > Dsg1 | Dsg1 |
| Oral Lesions | Common, initial | Rare/No |
| Blister Level | Suprabasal | Subcorneal/Granular |
| Severity | More severe | Milder |
Pemphigoid Group - Subepidermal Siege
- Subepidermal autoimmune blistering diseases. Common Direct Immunofluorescence (DIF): linear IgG/C3 deposition at the Basement Membrane Zone (BMZ).
| Feature | Bullous Pemphigoid (BP) | Mucous Membrane Pemphigoid (MMP) | Pemphigoid Gestationis (PG) |
|---|---|---|---|
| Population | Elderly | Adults | Pregnancy/Postpartum |
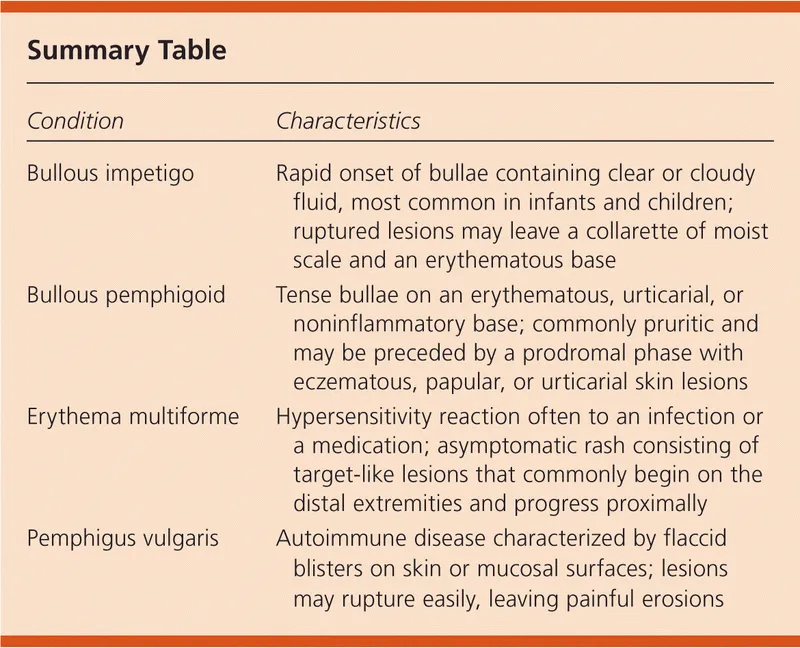
| Clinical | Tense blisters, urticarial plaques, intense pruritus, eosinophils (histology). 📌 BP = Big, Plump Blisters. Nikolsky sign usually negative. | Mucosal dominant, often with scarring (e.g., ocular, oral). | Pruritic papules/plaques progressing to blisters. |
| Target Ag(s) | BPAG1 (BP230), BPAG2 (BP180/Type XVII collagen) | BP180, Laminin 332 | BPAG2 (BP180) |
DH, LABD & EBA - Diverse Blister Battles
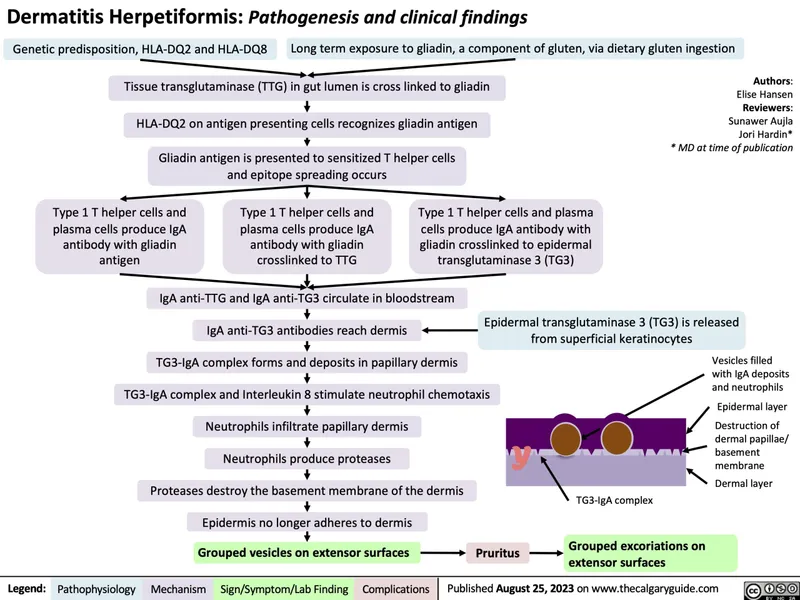
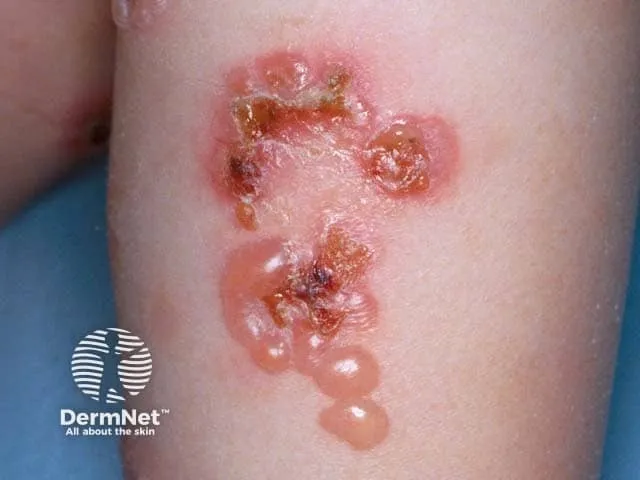
- Dermatitis Herpetiformis (DH)
- Intense pruritus; grouped (herpetiform) vesicles on extensors (elbows, knees, buttocks).
- Strong celiac disease/gluten sensitivity link. Histology: subepidermal, neutrophil microabscesses in dermal papillae. DIF: granular IgA deposits in dermal papillae.
- 📌 DH = Diet & Dapsone Help. Treatment: Dapsone, gluten-free diet.
-
⭐ Dermatitis Herpetiformis is considered a cutaneous manifestation of celiac disease, and a gluten-free diet is a cornerstone of management.
- Linear IgA Bullous Dermatosis (LABD)
- Heterogeneous presentation. Key: Linear IgA deposition at Basement Membrane Zone (BMZ).
- Clinical: vesicles/bullae, often annular; classic 'string of pearls' sign.
- Epidermolysis Bullosa Acquisita (EBA)
- Autoantibodies against Type VII collagen (anchoring fibrils in BMZ).
- Presents with trauma-induced blisters, increased skin fragility, scarring, and milia formation. Often resistant to standard treatments.
High‑Yield Points - ⚡ Biggest Takeaways
- Pemphigus Vulgaris: Intraepidermal (acantholysis), Nikolsky +ve, targets Desmoglein 3 (&1).
- Bullous Pemphigoid: Subepidermal, Nikolsky -ve, targets BPAG1/2, tense bullae, eosinophils.
- Dermatitis Herpetiformis: Subepidermal, IgA deposits (papillae), strong celiac disease link.
- Direct Immunofluorescence (DIF): Crucial for diagnosis, shows antibody location/type.
- Linear IgA Bullous Dermatosis: Linear IgA at BMZ; vancomycin common trigger.
- Pemphigus Foliaceus: Superficial, targets Desmoglein 1 only.
- Epidermolysis Bullosa Acquisita: Targets Type VII collagen.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

