Diagnostic Methods: Clinical & Biopsy - Spotting & Snipping
- Clinical Approach ("Spotting"):
- History: Onset, duration, triggers (drugs, UV), family Hx.
- Examination: Lesion type (macule, papule, vesicle, bulla), distribution. Special signs (Nikolsky's, Asboe-Hansen).
- Skin Biopsy ("Snipping"): Crucial for diagnosis.
- Techniques: Punch (common, 3-4 mm inflammatory), shave (superficial), incisional, excisional.
- Site Selection (Critical!):
- H&E: Edge of active, untreated lesion. Medium: 10% formalin.
- DIF: Perilesional skin (bullous, 1-2 cm away); lesional (vasculitis, <48h). Medium: Michel's.
- H&E Key Patterns: Acantholysis, spongiosis, interface dermatitis, infiltrates.
⭐ For Direct Immunofluorescence (DIF) in bullous disorders, biopsy perilesional (normal-appearing) skin, ideally within 1-2 cm of a blister.
Diagnostic Methods: Immunofluorescence - Antibody Spotlighting
Immunofluorescence (IF) is a key technique to detect autoantibodies in tissue (Direct IF) or serum (Indirect IF).
- Direct Immunofluorescence (DIF)
- Principle: Detects in vivo bound autoantibodies directly on patient's perilesional skin/mucosal biopsy.
- Sample: Fresh tissue, transported in Michel's medium or normal saline (on ice).
- Procedure: Biopsy incubated with fluorescein-labeled anti-human antibodies (IgG, IgA, IgM, C3).
- Detects: Tissue-bound autoantibodies & complement.
- Common Findings:
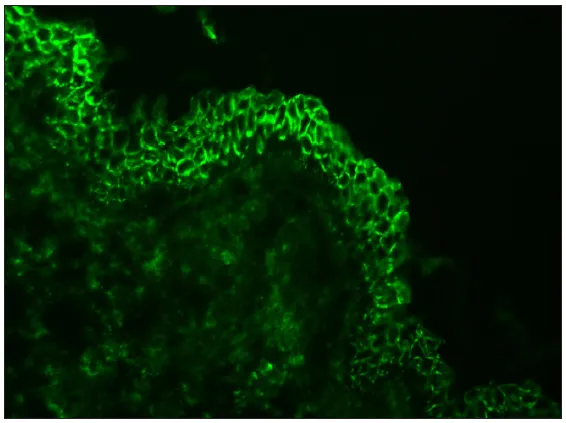
- Pemphigus vulgaris: Intercellular IgG/C3 in epidermis ("chicken-wire" pattern).
- Bullous pemphigoid: Linear IgG/C3 at dermoepidermal junction (DEJ).
- Dermatitis herpetiformis: Granular IgA at DEJ in dermal papillae.
- Lupus erythematosus: Linear/granular IgG, IgM, C3 at DEJ (Lupus Band Test).
- Indirect Immunofluorescence (IIF)
- Principle: Detects circulating autoantibodies in patient's serum.
- Sample: Patient's serum.
- Procedure: Serum incubated with substrate (e.g., monkey esophagus, rat bladder, salt-split skin), then fluorescein-labeled anti-human antibodies.
- Detects: Circulating autoantibodies; titre indicates antibody level.
- Common Substrates & Findings:
- Monkey esophagus: Pemphigus (intercellular), Pemphigoid (BMZ).
- Salt-split skin: Differentiates epidermolysis bullosa acquisita (dermal side) from bullous pemphigoid (epidermal side or both sides).
- HEp-2 cells: ANA patterns in connective tissue diseases.
⭐ Salt-split skin IIF is crucial for differentiating subepidermal blistering diseases. Antibodies binding to the epidermal side (roof) of the split suggest bullous pemphigoid, while binding to the dermal side (floor) suggests epidermolysis bullosa acquisita. Pemphigoid gestationis can show binding to the roof or both roof and floor.
📌 Mnemonic: DIF = Directly In Flesh (tissue biopsy). IIF = In In-vitro Fluid (serum).
Diagnostic Methods: Serology & Special Tests - Blood Tells Tales
- Serology: Detects serum autoantibodies; key for diagnosis, monitoring.
- Indirect Immunofluorescence (IIF):
- Screens: ANA (patterns), anti-dsDNA (Crithidia), ANCA.
- Substrate: HEp-2 (ANA).

- ELISA (Enzyme-Linked Immunosorbent Assay):
- Quantifies: anti-Dsg1/3 (Pemphigus), anti-BP180/230 (Pemphigoid).
- High sensitivity & specificity.
- Western Blot (Immunoblot):
- Confirmatory for specific protein antigens (e.g., anti-Mi-2 in Dermatomyositis).
- Immunoprecipitation (IP): Detects antibodies to soluble nuclear/cytoplasmic Ags (e.g., Ro, La).
- Indirect Immunofluorescence (IIF):
- ANCA (Anti-Neutrophil Cytoplasmic Antibodies):
- c-ANCA (anti-PR3): GPA. 📌 Cytoplasmic for GPA.
- p-ANCA (anti-MPO): Microscopic Polyangiitis, EGPA. 📌 Perinuclear.
⭐ Anti-Dsg1 and anti-Dsg3 antibody titres (ELISA) often correlate with disease activity in Pemphigus Foliaceus and Pemphigus Vulgaris respectively, guiding therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- DIF (Direct Immunofluorescence): Gold standard for bullous diseases; detects tissue-bound autoantibodies (IgG, C3) in perilesional skin.
- IIF (Indirect Immunofluorescence): Detects circulating autoantibodies; Salt-Split Skin substrate differentiates roof (BP) vs floor (EBA) patterns.
- ELISA: Quantifies specific autoantibodies like anti-Dsg1/3 (Pemphigus) and anti-BP180/230 (Bullous Pemphigoid).
- Skin Biopsy (H&E): Crucial for histopathology, showing level of blister and inflammatory cell type.
- Tzanck Smear: Rapid test for acantholytic cells (Pemphigus).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

