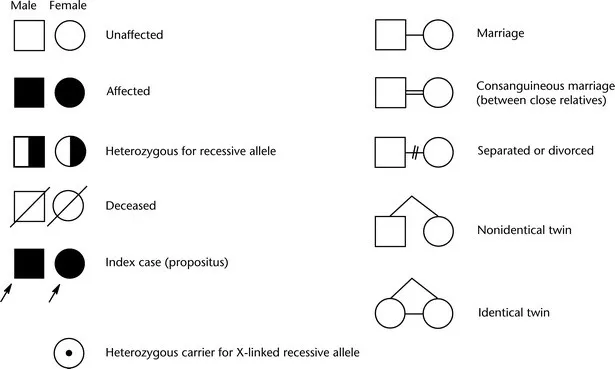
Inheritance Patterns - Gene Game Rules
- Autosomal Dominant (AD):
- One mutant allele. Vertical transmission.
- Male-to-male transmission.
- Risk: 50% (one affected parent).
- Autosomal Recessive (AR):
- Two mutant alleles. Horizontal transmission (skips generations).
- Consanguinity ↑ risk.
- Risk: 25% (both parents carriers).
- X-linked Recessive (XR):
- Males > females. No male-to-male.
- Affected father → all daughters carriers.
- Carrier mother → 50% sons affected.
- X-linked Dominant (XD):
- No male-to-male.
- Affected father → ALL daughters affected, NO sons.
- Affected mother (hetero) → 50% offspring affected.
- Mitochondrial:
- Maternal inheritance ONLY.
- Affected mother → ALL offspring affected.
- Affected father → NO offspring.
⭐ Penetrance: % of individuals with genotype expressing phenotype. Expressivity: Variation in phenotypic severity for a given genotype.
Amino Acidopathies - Protein Problems
- Inherited enzyme defects in amino acid (AA) metabolism, leading to AA or toxic byproduct accumulation.
- Phenylketonuria (PKU):
- Defect: Phenylalanine hydroxylase (PAH).
- Features: Mousy/musty odor, intellectual disability (ID), eczema, fair skin/hair.
- Screening: Guthrie test (↑Phe).
- Alkaptonuria (Ochronosis):
- Defect: Homogentisate oxidase.
- Features: Dark urine on standing, ochronotic pigment (cartilage, sclera), arthritis.
- Maple Syrup Urine Disease (MSUD):
- Defect: Branched-chain α-ketoacid dehydrogenase complex.
- Features: Maple syrup/burnt sugar odor (urine, sweat), neurotoxicity, poor feeding.
- 📌 "I Love Vermont" (Isoleucine, Leucine, Valine affected).
- Homocystinuria:
- Defect: Cystathionine β-synthase (commonest).
- Features: Marfanoid habitus, ectopia lentis (downward & inward), thromboembolism, ID.
- Tyrosinemia Type I:
- Defect: Fumarylacetoacetate hydrolase.
- Features: Cabbage-like odor, liver failure, renal tubular acidosis (Fanconi syndrome).
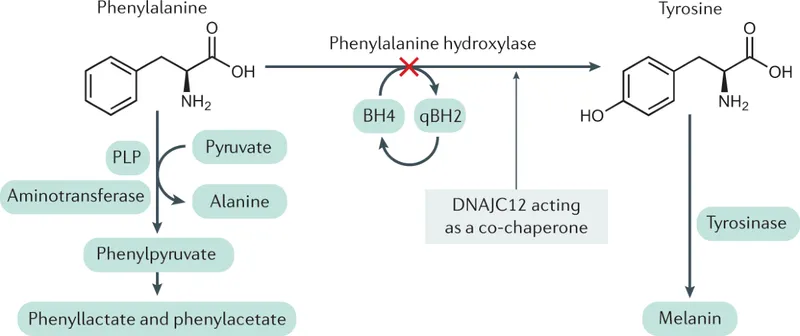
⭐ PKU: Autosomal recessive. Early dietary phenylalanine restriction is key to prevent irreversible intellectual disability. Maternal PKU requires strict control before/during pregnancy to prevent fetal damage (microcephaly, ID).
Carbohydrate Metabolism Disorders - Sweet Sicknesses
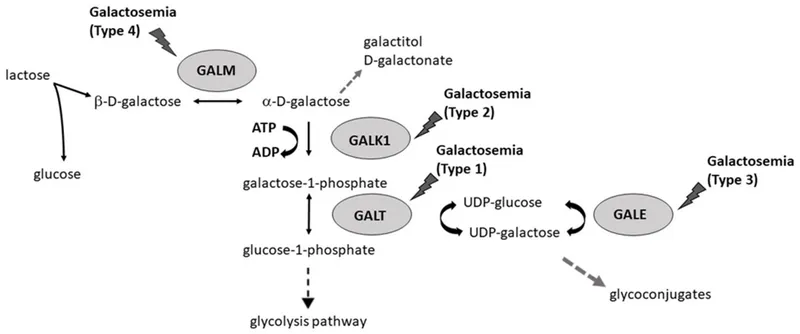
- Galactosemia (Classic): GALT def. → ↑Gal-1-P, galactitol.
- Neonatal jaundice, hepatomegaly, cataracts, E. coli sepsis. Urine: reducing substances.
- Tx: Galactose-free diet.
- Hereditary Fructose Intolerance (HFI): Aldolase B def. → ↑Fructose-1-P.
- Hypoglycemia, vomiting, jaundice post fructose/sucrose. Aversion to sweets.
- Tx: Avoid fructose, sucrose, sorbitol.
- Essential Fructosuria: Fructokinase def. Benign. Fructosuria.
- Glycogen Storage Diseases (GSDs):
- Type I (Von Gierke): Glucose-6-Phosphatase def. Severe fasting hypoglycemia, ↑lactate, hepatomegaly.
- Type II (Pompe): Lysosomal α-1,4-glucosidase (Acid Maltase) def. Cardiomegaly, muscle weakness. 📌 Pompe Pumps (Heart).
- Type V (McArdle): Muscle Glycogen Phosphorylase def. Exercise intolerance, cramps, myoglobinuria.
⭐ Classic galactosemia presents with failure to thrive, liver damage, and cataracts if milk feeding is continued; E. coli sepsis is a common neonatal complication.
Lysosomal Storage & Porphyrias - Cellular Clutter
Error generating content for this concept group: No object generated: the tool was not called.
High‑Yield Points - ⚡ Biggest Takeaways
- Autosomal dominant (AD): Vertical transmission, 50% risk to offspring; e.g., Marfan syndrome, Huntington disease.
- Autosomal recessive (AR): Horizontal transmission, 25% risk, often enzyme deficiencies; e.g., Cystic fibrosis, PKU.
- X-linked recessive (XLR): Affects mainly males, carrier females, no male-to-male transmission; e.g., DMD, Hemophilia A.
- X-linked dominant (XLD): Affected fathers transmit to all daughters; e.g., Rett syndrome, Alport syndrome (classic XLD form).
- Mitochondrial inheritance: Maternal transmission to all offspring; e.g., LHON, MELAS.
- Variable expressivity and incomplete penetrance modify Mendelian patterns.
- New mutations are common in severe AD disorders like Achondroplasia or Osteogenesis Imperfecta type II.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

