SCI Pathophys & Initial Care - Spine SOS!
- Primary Injury: Initial, irreversible mechanical damage.
- Secondary Injury: Delayed cascade (ischemia, inflammation, excitotoxicity); potentially modifiable.
- Spinal Shock: Temporary loss of reflexes, flaccid paralysis below injury. Bulbocavernosus reflex return signals end.
- Neurogenic Shock (Injury ≥T6): Sympathetic disruption. Triad: Hypotension, Bradycardia, Poikilothermia.
⭐ Neurogenic shock: hypotension with bradycardia/normal HR, unlike hypovolemic shock (tachycardia).
- Initial Care (ATLS & 📌 Spine SOS!):
- Airway: Jaw thrust, C-spine control.
- Breathing: Monitor C3-C5 (phrenic n.) for respiratory failure.
- Circulation: MAP >85-90 mmHg (vasopressors; cautious fluids).
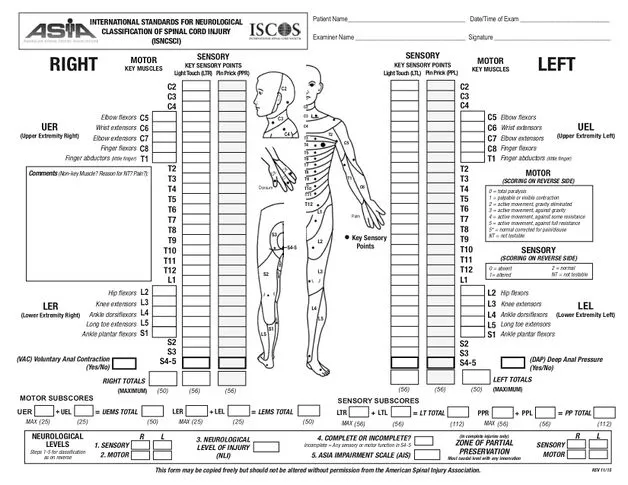
- Disability: ASIA scale.
- Immobilization: Rigid collar, log-roll.
SCI Airway & Induction - Neck's on the Line!
technique for cervical spine protection during intubation)
- C-Spine Protection:
- Absolute priority: Manual In-Line Stabilization (MILS) by a trained assistant.
- Remove rigid collars for intubation (may hinder view/access); maintain MILS.
- Airway Management Algorithm:
- Induction Agents:
- Goal: Maintain Mean Arterial Pressure (MAP) for spinal cord perfusion.
- Ketamine: Often preferred (maintains BP, bronchodilation).
- Etomidate: Hemodynamically stable (consider adrenal suppression).
- Propofol/Thiopentone: Use with caution (risk of hypotension ↓).
- Muscle Relaxants:
- Succinylcholine (SCh):
- Permissible only within first 24 hours post-SCI.
- ⚠️ Strictly AVOID after 24-48 hours (risk of severe hyperkalemia $K^+$↑).
- Rocuronium: Preferred non-depolarizing agent; Sugammadex available.
- Succinylcholine (SCh):
⭐ In acute SCI, succinylcholine is safe for RSI only within the first 24 hours. After 24-48 hours, it can cause life-threatening hyperkalemia due to upregulation of extrajunctional acetylcholine receptors (nAChRs).
SCI Intraop Hemodynamics - Pressure Points!
-
MAP Goal: 85-90 mmHg (first 5-7 days); SBP >90 mmHg to optimize SCPP.
-
Neurogenic Shock (>T6):
- Triad: Hypotension, Bradycardia, Poikilothermia (📌 HBP).
- Mgt: IV fluids (cautious), Norepinephrine (preferred), Atropine for significant bradycardia.
-
Autonomic Dysreflexia (AD) (>T6):
- Trigger: Stimuli below injury (surgery, bladder).
- Sx: Severe HTN, pounding Headache, Brady/Tachycardia, profuse Sweating/Flushing (above lesion).
- Mgt:
-
Monitoring: Invasive A-line (mandatory), continuous core temperature.
-
Temperature: Poikilothermia common → hypothermia risk. Active warming essential.
⭐ Crucial: Maintain MAP 85-90 mmHg for at least 7 days post-acute SCI to optimize spinal cord perfusion and limit secondary injury.
SCI Post-Op & Complications - Recovery Roadblocks
- Ventilatory Support: Prolonged ventilation, especially cervical lesions (C3-C5). Early tracheostomy may be needed. Weaning challenges.
- DVT Prophylaxis: Crucial. LMWH, sequential compression devices (SCDs), early mobilization if possible.
- Pain Management: Multimodal. Neuropathic pain (gabapentinoids, TCAs). Opioid-sparing techniques.
- Pressure Sores: Prevention is key. Regular turning (q2h), specialized surfaces, nutritional support.
- Autonomic Dysreflexia (AD): Persistent risk. Identify & manage triggers (bladder, bowel, skin).
⭐ AD is a medical emergency in patients with SCI at or above T6, characterized by paroxysmal hypertension.
- Spasticity: Develops later. Baclofen, tizanidine, physiotherapy.
- Heterotopic Ossification: Ectopic bone formation around joints, limiting mobility.
- Psychological Support: Essential for coping, rehabilitation, and quality of life adjustment post-SCI.
High‑Yield Points - ⚡ Biggest Takeaways
- Prioritize C-spine immobilization during intubation; AFOI or VL often preferred.
- Expect neurogenic shock (↓BP, ↓HR) with injuries above T6; treat with vasopressors.
- Succinylcholine is contraindicated 24h to 6-12 months post-SCI due to severe hyperkalemia risk.
- Autonomic dysreflexia (lesions >T6): sudden severe HTN, bradycardia; remove trigger, deepen anesthesia.
- Actively manage temperature due to poikilothermia.
- High cervical lesions (C3-C5) can cause respiratory failure.
- Judicious IV fluids to avoid pulmonary edema_
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

