LUS Basics - Echoes & Airwaves
- Echoes (Tissue Appearance):
- Anechoic (Black): Simple fluid (e.g., pleural effusion).
- Hypoechoic (Grey): Consolidated lung, complex fluid.
- Hyperechoic (White): Pleura, bone, air artifacts (A/B-lines).
- Key Structures & Artifacts:
- Pleural Line: Bright, hyperechoic line; visceral-parietal pleural interface.
- Lung Sliding: Shimmering/gliding movement at the pleural line. Absence suggests pneumothorax (or adhesions, mainstem intubation, apnea).
- A-lines: Horizontal, repetitive, hyperechoic artifacts arising from pleural line; indicate normal aerated lung.
- B-lines: Vertical, hyperechoic, laser-like artifacts from pleural line to screen edge; erase A-lines, move with lung sliding. Indicate interstitial syndrome (e.g., edema, inflammation, fibrosis).
- Pathological: ≥3 B-lines in one intercostal space.
⭐ Diffuse, bilateral B-lines (often called "lung rockets") are a key sign of cardiogenic pulmonary edema.
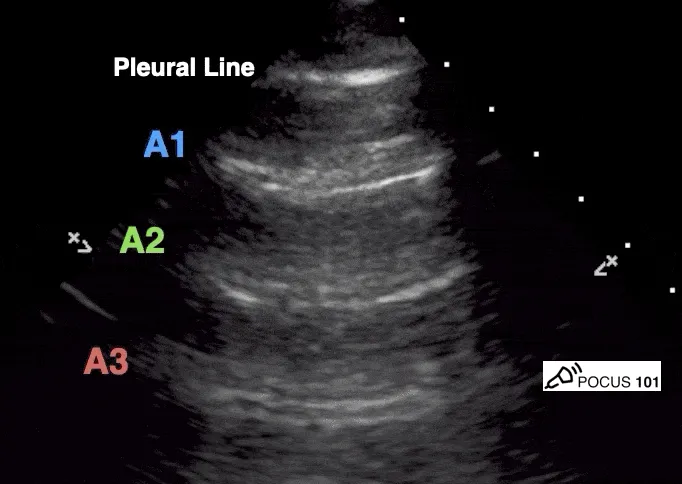
Normal Lungscape - Sliding & Shining
- Pleural Line ("Shining"): Bright, hyperechoic, smooth, horizontal line.
- Represents visceral-parietal pleural interface.
- "Bat Sign": Key landmark; two ribs (wings) sandwiching pleural line (body).
- Lung Sliding: Dynamic "to-and-fro" shimmering or twinkling at the pleural line.
- Synchronous with respiration.
- Indicates visceral pleura sliding against parietal pleura.
- A-lines: Horizontal, hyperechoic reverberation artifacts below pleural line.
- Equidistant, parallel to pleural line.
- Signify air; normal in aerated lung with sliding.
- M-mode: "Seashore Sign" confirms normal sliding.
- Chest wall: Static lines ("waves").
- Lung: Granular pattern ("sandy beach") below pleural line.

⭐ The presence of lung sliding effectively rules out pneumothorax at the specific intercostal space being examined with high negative predictive value.
Pathology Patterns - Spotting Trouble

- Pneumothorax (PTX):
- Key signs: Absent lung sliding, absent B-lines, exclusive A-lines.
- M-mode: "Stratosphere"/"Barcode" sign (vs. "Seashore").
⭐ The Lung Point sign (sliding/non-sliding interface) is pathognomonic, 100% specific for pneumothorax.
- Pleural Effusion:
- Anechoic/hypoechoic space between pleurae.
- Signs: "Quad sign", "Sinusoid sign" (inspiratory lung movement).
- "Jellyfish sign": Atelectatic lung floating.
- Pulmonary Edema (Interstitial Syndrome):
- Multiple (≥3), bilateral, diffuse B-lines ("lung rockets").
- Erase A-lines, move with sliding.
- Thickened, irregular pleural line.
- Consolidation:
- Subpleural, tissue-like pattern ("hepatization").
- "Shred"/"Fractal sign" (irregular border).
- Dynamic air bronchograms (pneumonia-specific).
- Atelectasis:
- Similar to consolidation; loss of aeration.
- Static/absent air bronchograms.
- Volume loss signs (e.g., raised hemidiaphragm).
PeriOp POCUS Plays - Guiding Care
- Preoperative Assessment:
- Identify occult pathology: pleural effusions, B-lines (interstitial syndrome), consolidations.
- Risk stratify for Postoperative Pulmonary Complications (PPCs); informs anesthetic plan.
- Intraoperative Guidance:
- Fluid management: Titrate fluids by monitoring B-lines (target <3 per zone) to prevent overload.
- Diagnose acute respiratory distress:
- Pneumothorax: Absent lung sliding, "lung point" sign (pathognomonic).
- Atelectasis: "Lung pulse" with absent sliding, tissue-like pattern.
- Pulmonary edema: Diffuse, bilateral B-lines (≥3 per zone).
- Endobronchial intubation: Unilateral absent sliding.
- Confirm ETT placement: Bilateral lung sliding, diaphragmatic movement.
- Postoperative Care:
- Early detection & monitoring of PPCs: atelectasis, pneumonia, effusions.
- Guide ventilator weaning: Assess lung aeration (LUS score), predict extubation success.
- 📌 BLUE protocol for acute dyspnea.
⭐ Lung ultrasound (LUS) rapidly diagnoses causes of perioperative respiratory failure, often outperforming CXR and guiding immediate intervention.
High‑Yield Points - ⚡ Biggest Takeaways
- A-lines: Horizontal artifacts; normal lung or pneumothorax if no lung sliding.
- B-lines (≥3 per zone): Vertical artifacts; indicate pulmonary edema or interstitial syndromes.
- Lung sliding absence: Key sign of pneumothorax ("stratosphere sign" on M-mode).
- Lung point: Highly specific for pneumothorax; transition from sliding to no sliding.
- Pleural effusion: Anechoic fluid in dependent areas; "sinusoid sign" may be present.
- Consolidation: Tissue-like pattern ("hepatization") with characteristic air bronchograms.
- BLUE protocol: Systematically diagnoses causes of acute respiratory failure using LUS (Lung Ultrasound).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

