Basic Ultrasound Physics - Wave Wisdom
- US waves: Mechanical, longitudinal. Medical range: 2-20 MHz.
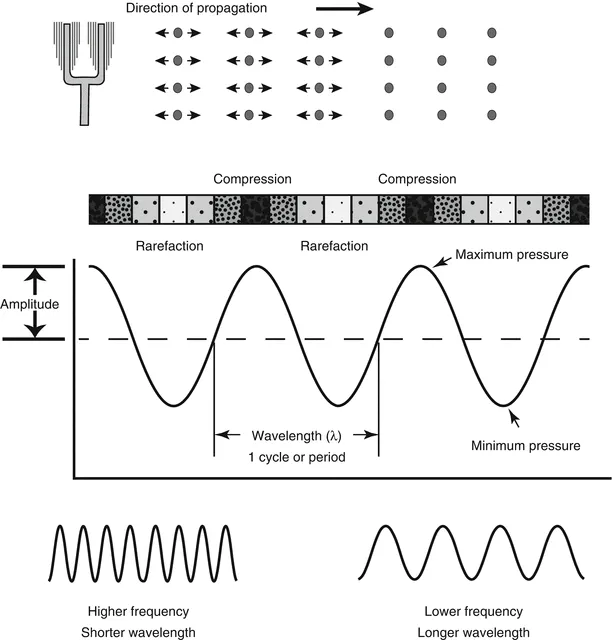
- Frequency (f): Determines resolution & penetration. ↑f = ↑resolution, ↓penetration.
- Wavelength (λ): $λ = c/f$. Inversely related to f.
- Propagation Speed (c): $c = f \times λ$. Constant in a medium. Avg. soft tissue: 1540 m/s. (📌 Cats Find Love)
- Acoustic Impedance (Z): $Z = \rho \times c$. Tissue resistance. Z-mismatches cause reflections (echoes). (📌 Zebras Prefer Carrots)
- Attenuation: Energy loss (absorption, scatter, reflection). ↑ with ↑f.
⭐ The propagation speed of ultrasound is highest in bone (~4080 m/s) and lowest in air/lung (~330 m/s).
Basic Ultrasound Physics - Probe Portraits
- Transducers (Probes): Convert electrical to ultrasound energy & vice-versa.
- Piezoelectric Effect: Crystals (e.g., PZT) deform with current (transmit); echoes deform crystals (receive).
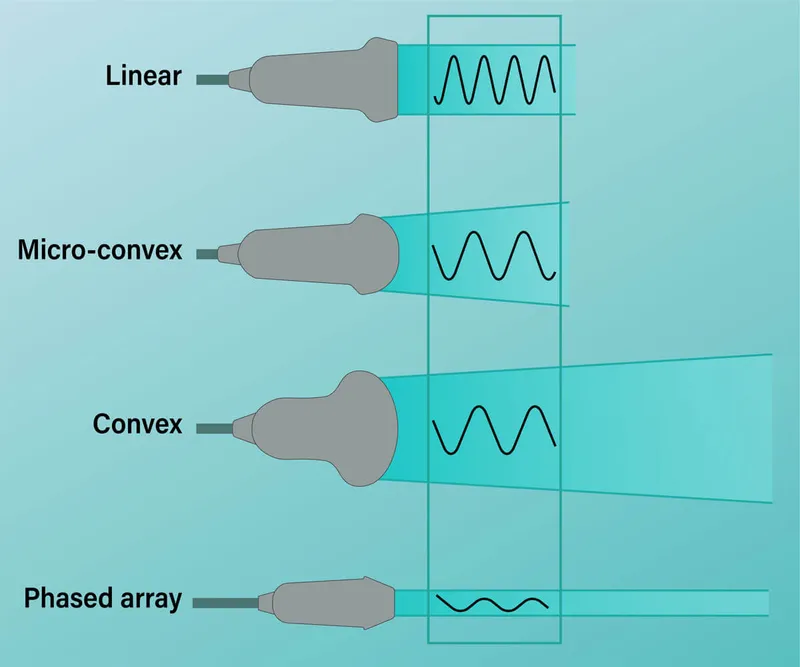
- Probe Types & Frequencies (📌 LCP: Linear-Lines, Convex-Cavities, Phased-Pumper):
- Linear: 6-13 MHz. Superficial (vascular, nerves). Rectangular image. ↑ Axial resolution.
- Curvilinear (Convex): 2-5 MHz. Deep (abdomen, FAST). Fan-shaped. ↑ Penetration.
- Phased Array (Sector): 1-5 MHz. Cardiac, intercostal. Pie-shaped. Small footprint.
- Key Components:
- Matching layer: Improves energy transmission.
- Damping material: Shortens pulse, ↑ axial resolution.
⭐ Higher frequency probes offer better image resolution but have shallower penetration depth.
Basic Ultrasound Physics - Echo Enigmas
- Fundamentals:
- Piezoelectric effect: Crystals generate/detect ultrasound.
- Wave speed ($v = f\lambda$): Avg. 1540 m/s in soft tissue.
- Acoustic Impedance ($Z = \rho c$): Mismatch at interfaces causes reflection (echoes).
- Attenuation: Signal loss with depth; ↑frequency = ↑attenuation, ↓penetration.
- Common Artifacts - Echo Enigmas:
- Acoustic Shadowing: Signal void posterior to high attenuators (e.g., bone, calculi).
- Posterior Acoustic Enhancement: Increased echo intensity posterior to low attenuators (e.g., cysts).
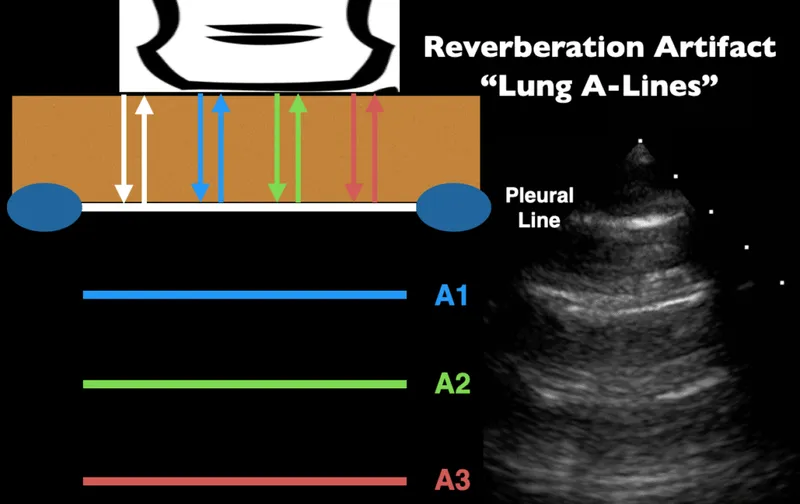
- Reverberation: Multiple, equally spaced linear echoes (e.g., A-lines).
- Mirror Image: Artifactual structure deep to a strong, curved reflector (e.g., diaphragm).
- Anisotropy: Echogenicity of tissues (e.g., tendons) varies with insonation angle. 📌 Angle matters!
⭐ The greater the acoustic impedance mismatch between two tissues, the stronger the reflected echo, forming brighter areas on the ultrasound image.
Basic Ultrasound Physics - Flow Frontiers
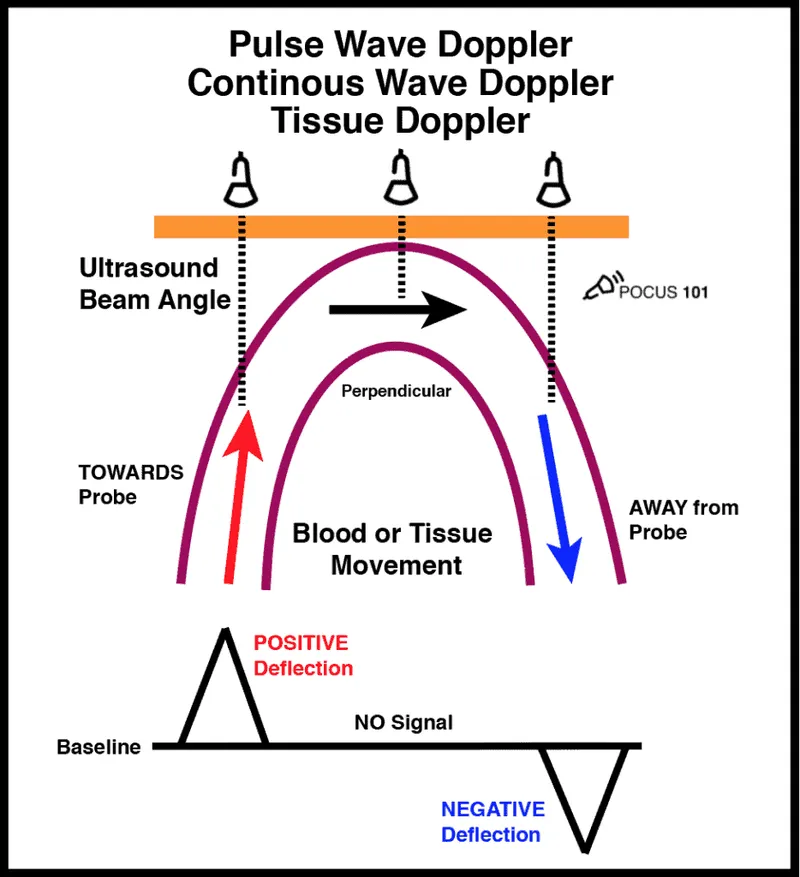
- Doppler Effect: Frequency shift of ultrasound waves reflected from moving structures (e.g., RBCs).
- Doppler Equation: $f_D = \frac{2 \cdot f_t \cdot v \cdot \cos\theta}{c}$
- $f_D$: Doppler shift, $f_t$: transmitted frequency, $v$: velocity, $\theta$: angle, $c$: sound speed.
- Modes:
- Continuous Wave (CW): No aliasing, range ambiguity.
- Pulsed Wave (PW): Range specific, aliasing (Nyquist limit).
- Color Doppler: Mean velocity map. 📌 BART: Blue Away, Red Towards.
- Power Doppler: Sensitive to slow flow, no direction.
⭐ Nyquist Limit: In PW Doppler, aliasing occurs if Doppler shift > PRF/2 (Pulse Repetition Frequency divided by 2).
High‑Yield Points - ⚡ Biggest Takeaways
- Piezoelectric effect is fundamental for ultrasound transducers.
- Acoustic impedance (Z) mismatch (Z = ρc) is crucial for image formation via reflection.
- Higher frequency offers superior axial resolution but has ↓ penetration.
- Lower frequency provides ↑ penetration but has inferior axial resolution.
- Attenuation (energy loss) is directly proportional to frequency and depth.
- The Doppler effect enables assessment of blood flow velocity and direction.
- Key modes include B-mode (2D imaging), M-mode (motion), and Doppler (flow).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

