Pediatric PK/PD - Tiny Bodies, Big Changes
- Absorption (A):
- Neonates: Gastric pH ↑, GI transit variable, IM absorption erratic, skin permeability ↑.
- Distribution (D):
- Total Body Water (TBW) ↑ (70-80% vs. 60% adult) & Extracellular Fluid (ECF) ↑ → ↑ Volume of Distribution (Vd) for water-soluble drugs.
- Fat content ↓ → ↓ Vd for lipid-soluble drugs.
- Protein binding ↓ (e.g., albumin) → ↑ free drug fraction.
- Metabolism (M):
- CYP450 enzyme system immature; Phase I reactions (e.g., oxidation) slower.
- Phase II glucuronidation ↓ significantly in neonates. 📌 Neonates Generally Lack UDPGT (UDP-glucuronosyltransferase).
- Excretion (E):
- Glomerular Filtration Rate (GFR) ↓ in neonates/infants (reaches adult values by 6-12 months).
- Pharmacodynamics (PD):
- Receptor density & affinity may differ.
- Paradoxical drug responses (e.g., benzodiazepines causing agitation).
⭐ Minimum Alveolar Concentration (MAC) values for volatile anesthetics are highest in infants (peak at 1-6 months), often ~1.5x adult values (e.g., Sevoflurane).
oka
Inhalational Agents - Sweet Dreams, Safe Air
- MAC (Minimum Alveolar Concentration): Peaks at ~6 months (Sevoflurane/Isoflurane); lower in neonates & older children vs. infants.
- Kinetics: Faster induction/emergence (↑ $V_A$/FRC, ↑ CO to VRG, ↓ blood:gas solubility effect).
- Agents:
- Sevoflurane: Choice for induction; non-pungent.
- Desflurane: Airway irritant; rapid recovery. Not for induction.
- Halothane: Historical; halothane hepatitis risk.
- Nitrous Oxide ($N_2O$): Diffusion hypoxia risk (administer 100% O₂ post-use).
⭐ Sevoflurane is preferred for pediatric inhalational induction due to low pungency and rapid onset.
oka
IV Anesthetics & Opioids - Vein Voyage, Pain Vanquishers
- Propofol:
- Induction/maintenance. Neonates: ↑ Vd, ↑ dose (2.5-3.5 mg/kg).
- ⚠️ Risk: Propofol Infusion Syndrome (PRIS).
- Ketamine:
- Dissociative anesthesia, potent analgesia, bronchodilation.
- Dose (IV): Induction 1-2 mg/kg; Analgesia 0.25-0.5 mg/kg.
- ⚠️ Emergence delirium; ↓ with benzodiazepines.
- Opioids:
- Morphine: Neonates: ↓ clearance, prolonged effect. Dose: 0.05-0.1 mg/kg.
- Fentanyl: Neonates: ↑ sensitivity. Dose: 1-2 mcg/kg. ⚠️ Chest wall rigidity with high doses/rapid injection.
- Remifentanil: Ultra-short acting; plasma esterase metabolism. Ideal for TIVA.
- Dexmedetomidine:
- α2-agonist: sedative, analgesic. Minimal respiratory depression.
- Loading dose: 0.5-1 mcg/kg over 10 min; Maintenance: 0.2-0.7 mcg/kg/hr.
⭐ Fentanyl is approximately 100 times more potent than morphine.
Muscle Relaxants & Reversal - Still Muscles, Swift Wake-up
- Succinylcholine (SCh): 1-2 mg/kg IV. Risks: MH, hyperkalemia, masseter spasm; atropine for bradycardia.
- Non-depolarizers (NDMRs):
- Rocuronium: 0.6-1.2 mg/kg. Reversal: Sugammadex.
- Atracurium/Cisatracurium: Hoffman/ester hydrolysis.
- Pediatric Considerations:
- Neonates: ↑ sensitivity to NDMRs, ↓ plasma cholinesterase.
- Reversal:
- Neostigmine (0.05-0.07 mg/kg) + Glycopyrrolate (0.01-0.02 mg/kg).
- Sugammadex (for Rocuronium).
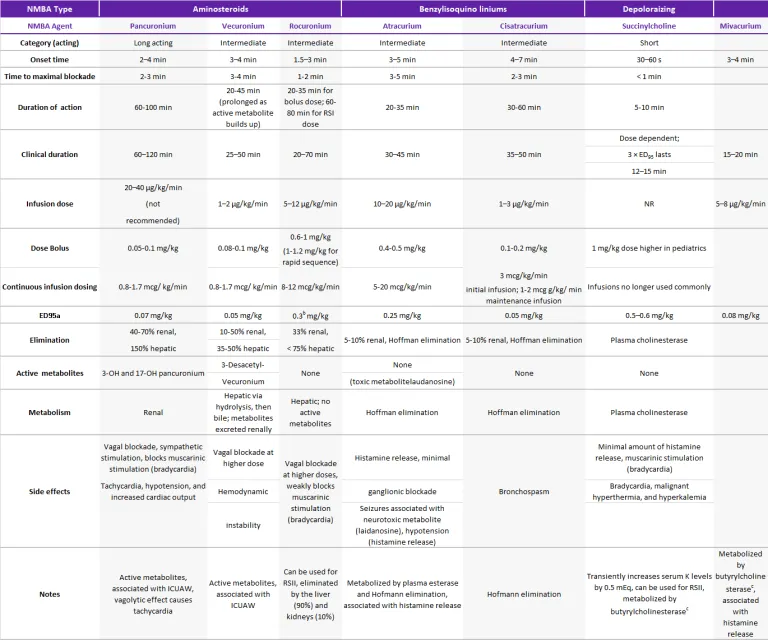
⭐ Neonates: ↑ NDMR sensitivity, ↓ plasma cholinesterase (prolongs SCh).
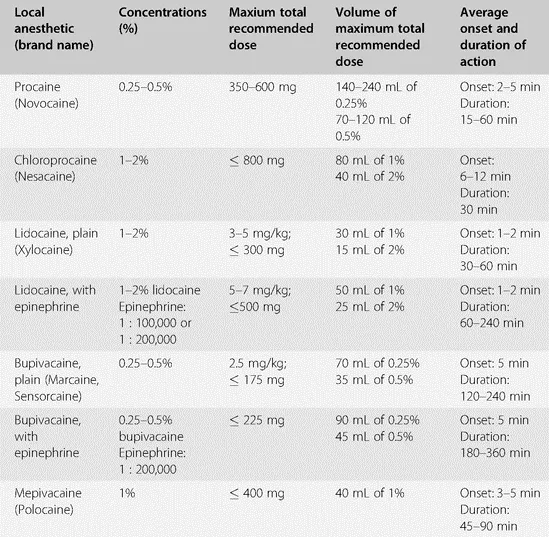
Local Anesthetics & Dosing - Numb & Numbered Right
- Max Doses (mg/kg):
- Lidocaine: Plain 3-5; With Epi 5-7
- Bupivacaine: Plain ~2
- Ropivacaine: Plain ~2-3
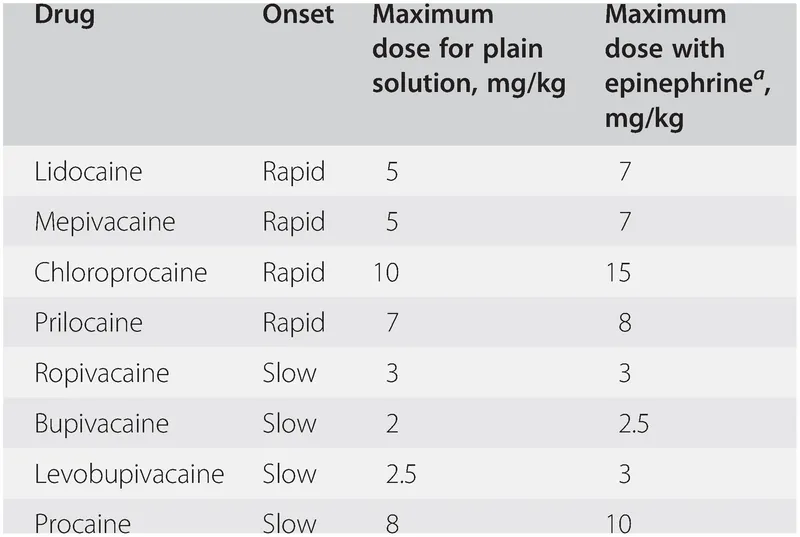
- Neonates: ↓ protein binding (↑ free fraction), ↓ metabolism.
- LAST (Local Anesthetic Systemic Toxicity):
- Signs: CNS (tinnitus, seizures) → CVS (arrhythmias, collapse).
- Management: Intralipid 20%.
- Common Applications: Caudal blocks, EMLA cream.
⭐ For LAST, Intralipid 20% initial bolus is 1.5 mL/kg (ideal body weight) over 1 min; may repeat bolus 1-2 times for persistent asystole/CV collapse.
High‑Yield Points - ⚡ Biggest Takeaways
- Neonates/Infants: ↑ Vd for water-soluble drugs (e.g., succinylcholine) means higher mg/kg doses.
- Immature hepatic metabolism (glucuronidation) prolongs effects of opioids (morphine) & benzodiazepines.
- Reduced GFR in neonates slows renal drug excretion (e.g., aminoglycosides).
- MAC values are higher in infants (peak ~6 months); sevoflurane highest in neonates.
- Marked sensitivity to respiratory depression from opioids and sedatives.
- Rapid inhalational induction/emergence due to ↑ alveolar ventilation/FRC ratio.
- Propofol: Higher induction doses (mg/kg) due to larger Vd & faster clearance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

